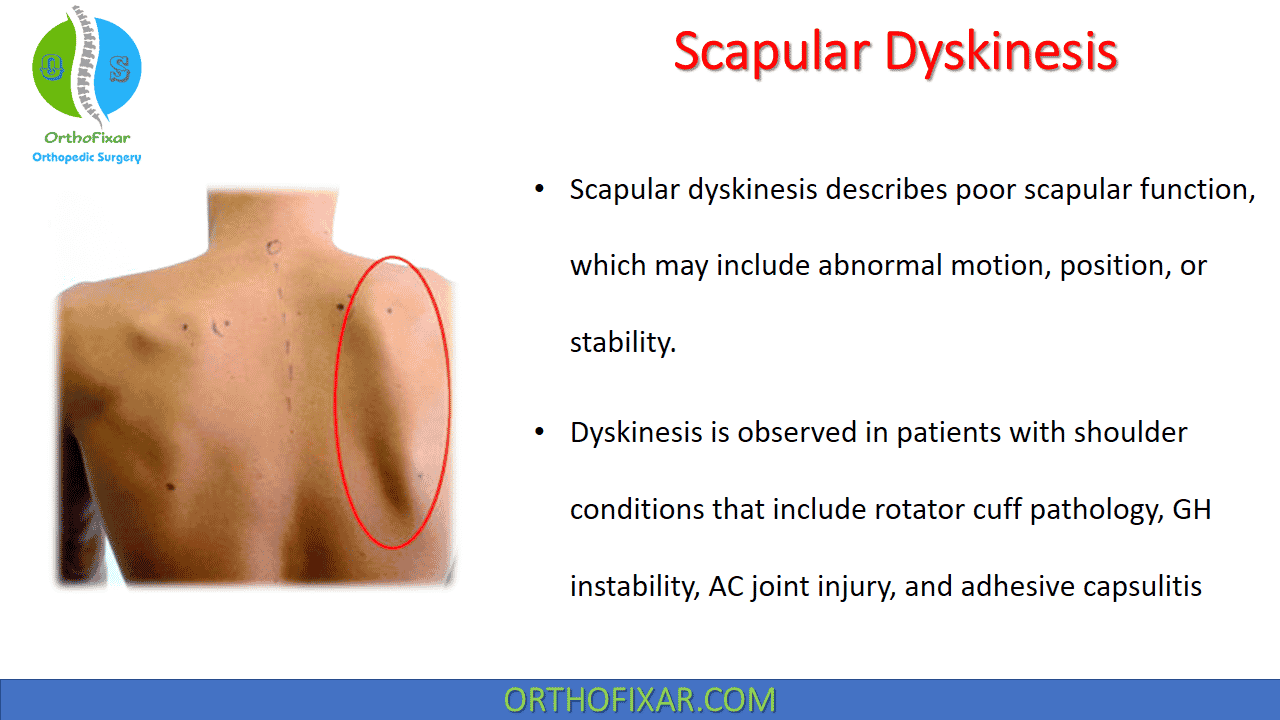
Scapular dyskinesis is an alteration in the normal position or motion of the scapula that occurs during coupled scapulohumeral movements as a response to shoulder dysfunction. It’s also called scapulothoracic dyskinesis. Shoulder dyskinesia occurs most often in overhead athletes (61%) compared with the non-overhead athletes (33%).
It should be suspected in patients with shoulder injury and can be identified and classified by specific physical examination.
Dyskinesis is observed in patients with shoulder conditions that include rotator cuff pathology, GH instability, AC joint injury, and adhesive capsulitis.
See Also: Frozen Shoulder | Adhesive Capsulitis
Related Anatomy
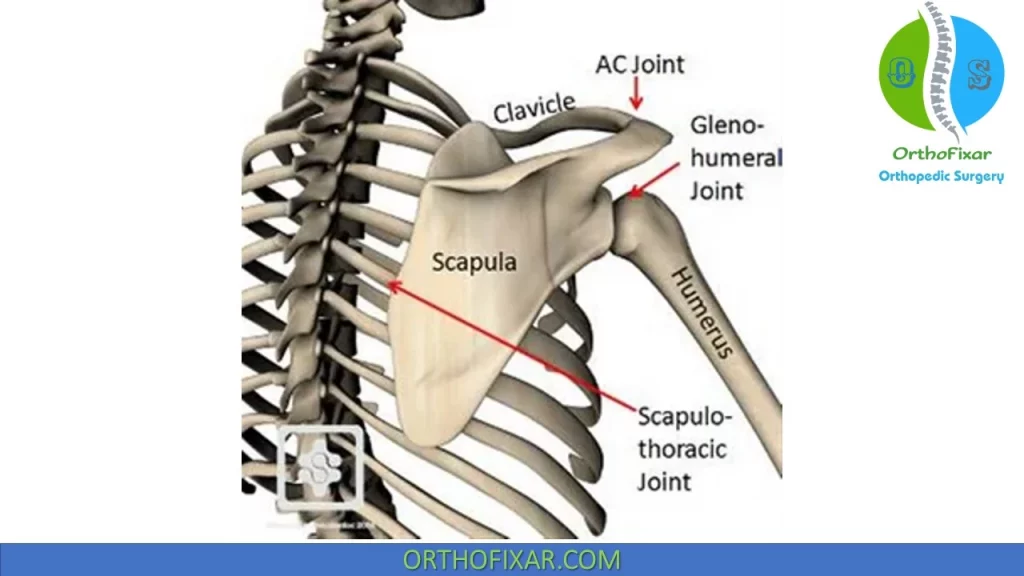
The Scapula Spans from second through seventh ribs and serves as an attachment for 17 muscles. It’s anteverted on chest wall approximately 30 degrees relative to the body.
Although the scapulothoracic joint is not a true joint, it allows scapular movement against the posterior rib cage and contributes to glenohumeral joint positioning and mechanics.
The scapulothoracic joint is fixed primarily by the scapular muscular attachments:
- The muscles connecting the upper limb to the vertebral column are trapezius, latissimus, both rhomboid muscles, and levator scapulae muscle.
- The muscles connecting the upper limb to the thoracic wall are both pectoralis muscles, subclavius, and serratus anterior muscle.
See Also: Scapula Anatomy
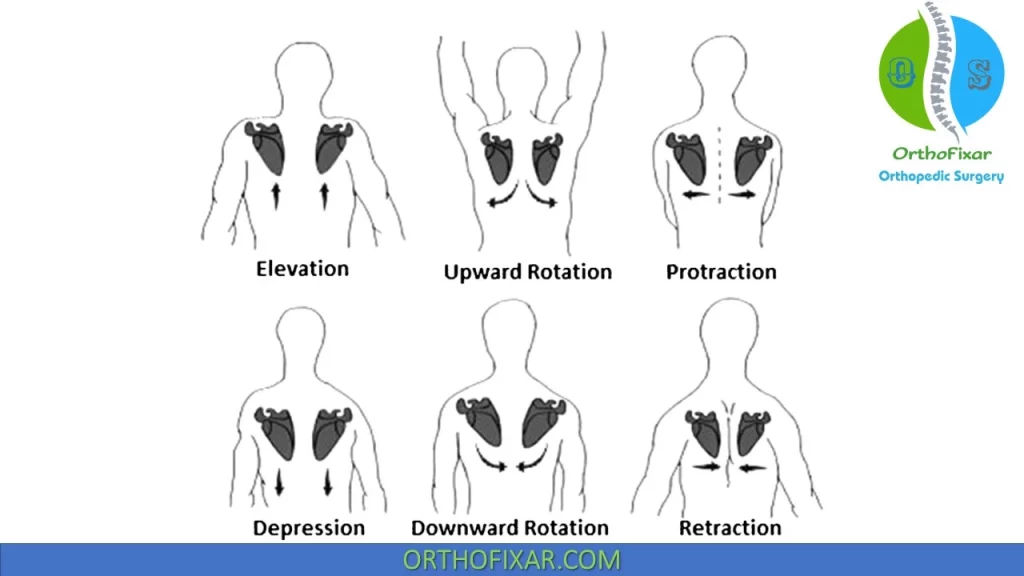
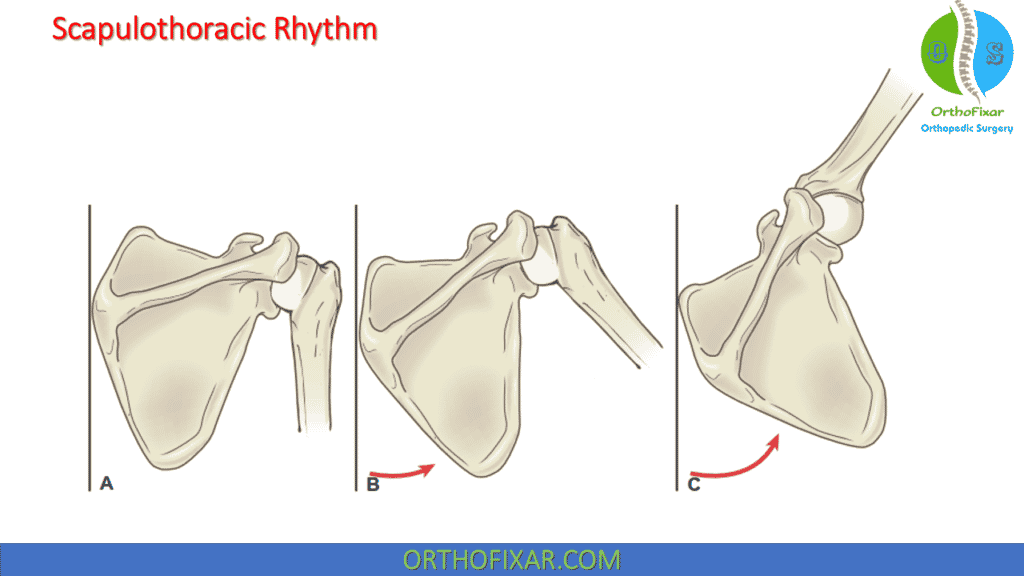
Scapulothoracic Rhythm
For the hand to obtain its maximal arc of motion, the GH and scapulothoracic articulations must combine their available ROMs:
- If the humeral head were rigidly fixated in the glenoid fossa in a manner eliminating GH movement, the humerus could still be elevated to 60 degrees through movement of the scapula via the AC and SC joints.
- For the humerus to be elevated to its maximum ROM of 180 degrees (relative to the thorax), the GH and scapulothoracic articulation must function together. Although a wide range of individual variability exists, an approximate 2:1 ratio is found between GH elevation and upward scapular rotation.
- For 180 degrees of humeral elevation to occur, 120 degrees is from GH movement, and 60 degrees is through upward rotation of the scapula.
The ratio of GH elevation to upward scapular rotation varies throughout humeral motion:
- Approximately the first 30 degrees of elevation is achieved primarily through GH motion, with the scapula setting (fixating) to provide stability for the contracting muscles.
- As humeral elevation reaches 90 degrees, the ratio between the GH joint and the scapula is approximately 1:1.
- Towards full elevation, motion is again achieved primarily through the GH joint. Maintenance of this rhythm is based on the coordination of the prime movers of the humerus and the synergistic contractions of the scapular stabilizers.
Scapular Dyskinesis Causes
Potential Causes of Scapula Dyskinesis include:
Abnormality in bony posture or injury:
Excessive scapular protraction and acromial depression in all stages of motion which increases the risk for impingement Excessive resting kyphosis. Forward head posture creates tightness to the anterior neck musculature, which again in turn facilitates the abnormal scapula position.
Kyphoscoliosis, rib fracture callus or hypertrophic nonunion, shortened clavicle as a result of fracture malunion and enlarging soft- tissue or skeletal masses, among several other potential defects, can produce symptoms such as scapulothoracic crepitation with shoulder motion (caused by any abnormality that results in a decreased scapulothoracic space) or clinical findings such as the gradual appearance of scapular malposition (caused by the presence of an enlarging mass within the scapulothoracic space which can push the scapular body away from the posterior thorax, thus producing the appearance of scapular winging and dyskinesis).
AC joint injuries or instabilities:
Can alter the center of rotation of the scapula, leading to faulty mechanics.
Muscle function alterations:
Alterations involving the serratus anterior and lower trapezius are a common source of dysfunction, especially in cases of secondary impingement Microtrauma due to excessive strain in the muscles, fatigue, and inhibition due to pain.
In at least one study, the amplitude of activation and the contraction strength of the serratus anterior muscle was significantly decreased in patients with subacromial impingement. This produced an abnormal scapular resting position (increased anterior tilt and downward rotation) and subsequent scapular dyskinesis due to the unbalanced opposing force couple between the serratus anterior muscle (weaker muscle) and the trapezius muscle (stronger muscle).
Contractures:
Especially of the anterior musculature that attaches to the coracoid process (pectoralis minor and short biceps head) can create an anterior tilt and forward lean to the scapula, as can tightness to the posterior capsule and latissimus.
Nerve damage:
It’s a rare cause of Scapular Dyskinesis. Neurogenic causes such as cervical radiculopathy and the oft-cited palsies involving the long thoracic nerve (results in prominence of the medial scapular border) and the spinal accessory nerve (results in more subtle scapular winging with difficulty in abduction)
Association of Scapular Dyskinesis with Shoulder Pathologies:
Rotator cuff impingement/tear:
- The patient lacks scapular upward rotation, external rotation, and posterior tilt during arm elevation.
- The scapular assistance test may decrease impingement symptoms.
- Manual scapular retraction may increase strength with the empty can test.
- The relocation test may relieve symptoms of internal (posterior) impingement.
- Those with definite rotator cuff tears display increased upward rotation and lack posterior tilt.
Superior labral lesion:
- The patient lacks scapular external rotation and posterior tilt during arm elevation.
- Manual scapular retraction may decrease symptoms during positive tests for superior labral lesions.
AC sprain:
- Those with Type III-V AC sprains lack retraction at rest and during humeral elevation.
GH Multidirectional Instability:
- The patient lacks scapular external rotation and posterior tilt during arm elevation.53 Manual scapular retraction may increase strength with the empty can test.
The most commonly encountered cascade of events occurs in the following sequence:
- primary or secondary dyskinesis, which leads to
- submaximal supraspinatus contraction, which leads to
- gradual superior humeral head migration, which leads to
- a gradual decrease in subacromial space, which leads to
- subacromial impingement and supraspinatus tears, which lead to
- pain, which leads to
- compensatory, asymmetric muscle firing patterns, which lead to
- worsening of scapular malposition, dyskinesis, superior humeral head migration, and so on.
Scapular Dyskinesis Types
There are three types of scapular dyskinesis:
Type I:
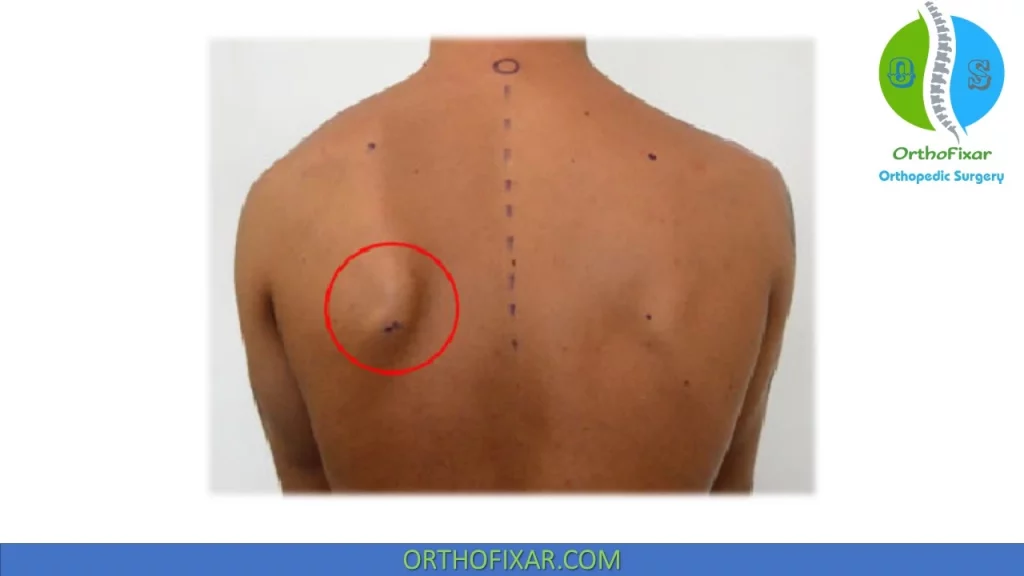
Type I is characterized by prominence of the inferior medial scapular border.
In throwers, this type may be referred to as a SICK scapula (malposition of the Scapula, prominence of the Inferior medial border of the scapula, Coracoid pain and malposition, and scapular dyskinesia).
A thrower with this syndrome presents with an apparent “dropped” scapula in the symptomatic shoulder compared with the contralateral shoulder’s scapular position.
Viewed from behind, the inferior medial scapular border appears very prominent, with the superior medial border and acromion less prominent.
When viewed from the front, this tilting (protraction) of the scapula makes the shoulder appear to be lower than the opposite side.
The pectoralis minor tightens as the coracoid tilts inferiorly and shifts laterally away from the midline, and its insertion at the coracoid becomes very tender.
Type II:
Type II is characterized by protrusion of the entire medial border.
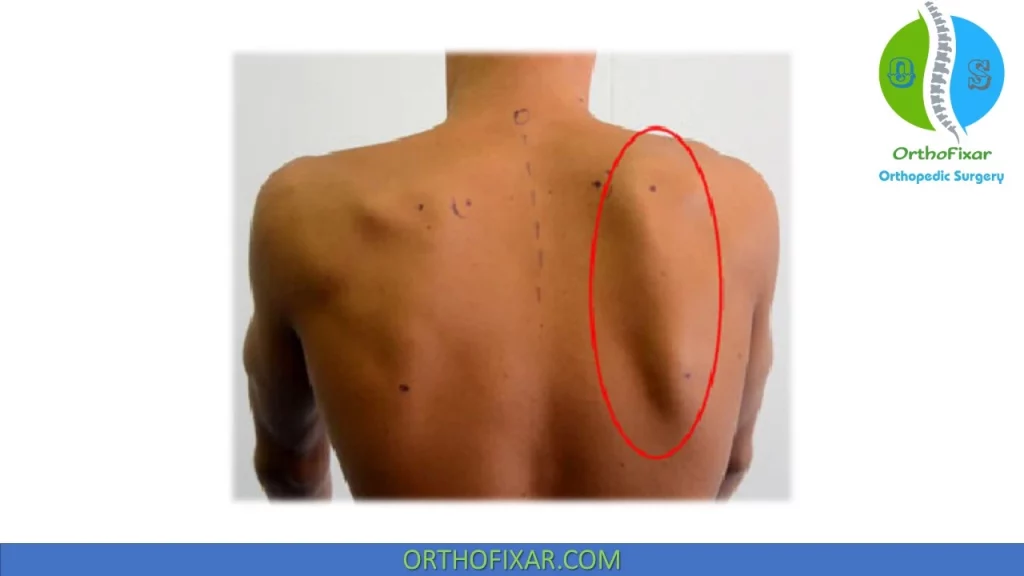
Type III:
Type III involves superior translation of the entire scapula and prominence of the superior medial border.
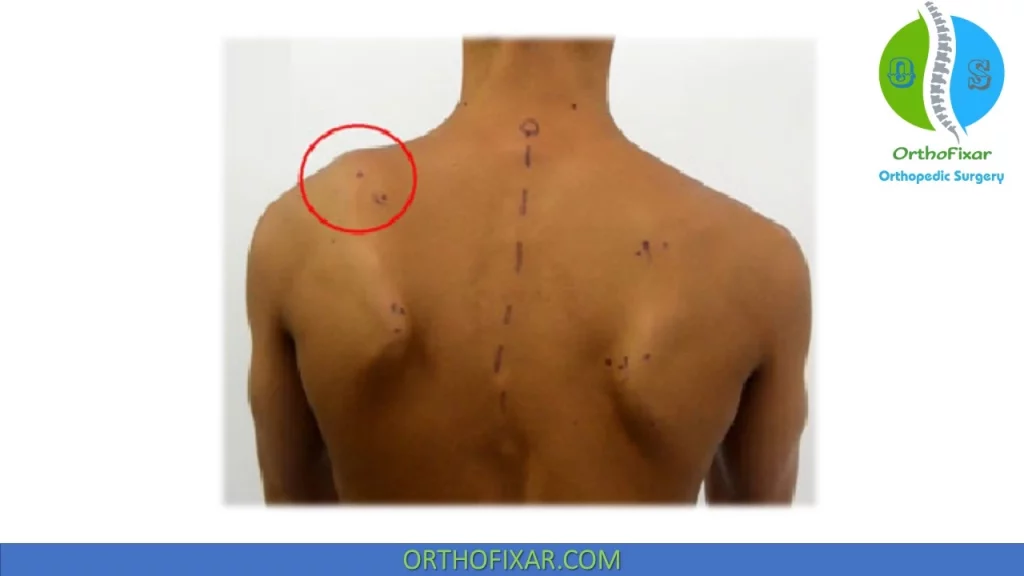
Mechanisms of Scapular Dyskinesia
| Mechanism | Associated Effects |
|---|---|
| Inadequate serratus anterior activation | Lesser scapular upward rotation and posterior tilt |
| Excess upper trapezius activation | Greater clavicular elevation |
| Pectoralis minor tightness | Greater scapular medial rotation and anterior tilt |
| Posterior glenohumeral joint soft-tissue tightness | Greater scapular anterior tilt |
| Thoracic kyphosis or flexed posture | Greater scapular medial rotation and anterior tilt, lesser scapular upward rotation |
Symptoms & Sign
Evaluation of the patient should include the trunk segments, hip and lower extremity function, and scapular position and movement analysis.
Dyskinesis often becomes apparent during an assessment of associated GH or elbow pain. Pain may be localized over the coracoid process, pectoralis minor, superior and medial borders of the scapula, AC joint, posterior-lateral GH joint line, or subacromial space. Muscle spasm is often palpated or reported in the upper trapezius, posterior cervical, and levator scapulae musculature.
There may even be painful scar tissue found in the musculature due to long-standing dyskinesis.
The assessment of scapular function begins with postural observation. Resting position of the scapula should be approximately 5 degrees of upward rotation, 40 degrees of internal rotation, and 15 degrees of anterior tilt. Abnormal position of the scapula often includes an excessively lower, protracted, and anteriorly tilted scapula. The prominence of the vertebral scapular border and inferior angle may be secondary to thoracic kyphosis, cervical lordosis, scoliosis, a tight or shortened pectoralis minor or short head of the biceps, or posterior rotator cuff and capsular tightness.
Strength testing can include the isometric scapular pinch, the Scapular Assistance Test, the scapular retraction test, and the lateral slide test (LST).
Scapular Dyskinesis Treatment
Once all the factors involved in the dysfunction of the shoulder are identified, Scapular Dyskinesis Treatment can begin on restoring normal scapular position and movement. More extensive therapy, including strengthening, should not occur until this step is accomplished; otherwise the shoulder is being worked in a faulty position.
The treatment of scapular dyskinesis is directed at managing underlying causes and restoring normal scapular muscle activation patterns by kinetic chain-based rehabilitation protocols. Patients must avoid aggravating motions or activity during early rehabilitation. Early treatment may include local modalities and manual therapy for pain, inflammation, and any spasms in the upper trapezius, posterior cervical, or levator scapulae musculature.
Leg, back, and trunk flexibility and strength should be normalized, and exercises that emphasize kinetic chain activation of the leg, trunk, and scapula should be instituted.
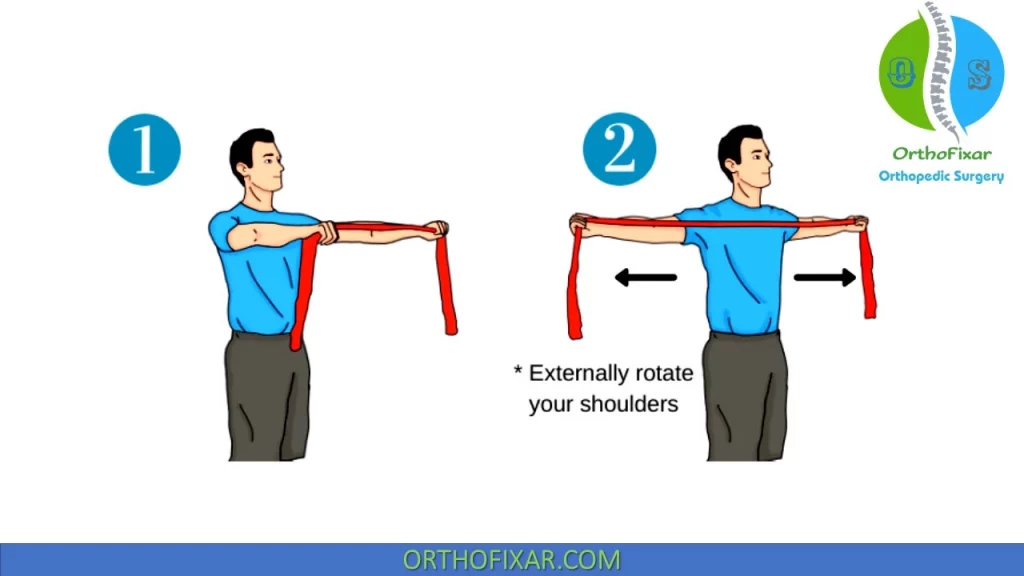
Physical therapy for scapular dyskinesis include:
- trunk extension and scapular retraction,
- trunk rotation and scapular retraction,
- one-legged stance and diagonal trunk rotation and scapular retraction.
All of these exercises facilitate lower trapezius muscle activation.
References
- Burn MB, McCulloch PC, Lintner DM, Liberman SR, Harris JD. Prevalence of Scapular Dyskinesis in Overhead and Nonoverhead Athletes: A Systematic Review. Orthop J Sports Med. 2016 Feb 17;4(2):2325967115627608. doi: 10.1177/2325967115627608. PMID: 26962539; PMCID: PMC4765819. Pubmed
- Kibler WB, McMullen J. Scapular dyskinesis and its relation to shoulder pain. J Am Acad Orthop Surg. 2003 Mar-Apr;11(2):142-51. doi: 10.5435/00124635-200303000-00008. PMID: 12670140. Pubmed
- Burkhart SS, Morgan CD, Kibler WB: The disabled throwing shoulder: spectrum of pathology Part III: The SICK scapula, scapular dyskinesis, the kinetic chain, and rehabilitation. Arthroscopy 19:641–661, 2003. Pubmed
- Doody, SG, and Waterland, JC: Shoulder movements during abduction in the scapular plane. Arch Phys Med Rehabil, 51:595, 1970. Pubmed
- Hebert, LJ, et al: Scapular behavior in shoulder impingement syndrome. Arch Phys Med Rehabil, 83:60, 2002. Pubmed
- McClure, PW, et al: Shoulder function and 3-dimensional scapular kinematics in people with and without shoulder impingement syndrome. Phys Ther, 86:1075, 2006. Pubmed
- Warner, JJP, et al: Scapulothoracic motion in normal shoulders and shoulders with glenohumeral instability and impingement syndrome: a study using Moiré topographic analysis. Clin Orthop Relat Res, 285:191, 1992. Pubmed
- Paletta, GA, et al: Shoulder kinematics with two-plane x-ray evaluation in patients with anterior instability or rotator cuff tearing. J Shoulder Elbow Surg, 6:516, 1997. Pubmed
- von Eisenhart-Rothe, R, et al: Pathomechanics in atraumatic shoulder instability: scapular positioning correlates with humeral head centering. Clin Orthop Relat Res, 433:82, 2005. Pubmed
- Gumina, S, et al: Scapular dyskinesis and sick scapula syndrome in patients with chronic type III acromioclavicular dislocation. Arthroscopy, 25:40, 2009. Pubmed
- Fayad, F, et al: Three-dimensional scapular kinematics and scapulohumeral rhythm in patients with glenohumeral osteoarthritis or frozen shoulder. J Biomech, 41:326, 2008. Pubmed
- Graichen, H, et al: Three-dimensional analysis of shoulder girdle and supraspinatus motion patterns in patients with impingement syndrome. J Orthop Res, 19:1192, 2001. Pubmed
- Kibler, WB, et al: Evaluation of apparent and absolute supraspinatus strength in patients with shoulder injury using the scapular retraction test. Am J Sports Med, 34:1643, 2006. Pubmed
- Kibler, WB, et al: Clinical utility of traditional and new tests in the diagnosis of biceps tendon injuries and superior labrum anterior and posterior lesions in the shoulder. Am J Sports Med, 37:1840, 2009. Pubmed
- Ludewig, PM, and Reynolds, JF: The association of scapular kinematics and glenohumeral joint pathologies. J Orthop Sports Phys Ther, 39:90, 2009. Pubmed
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.