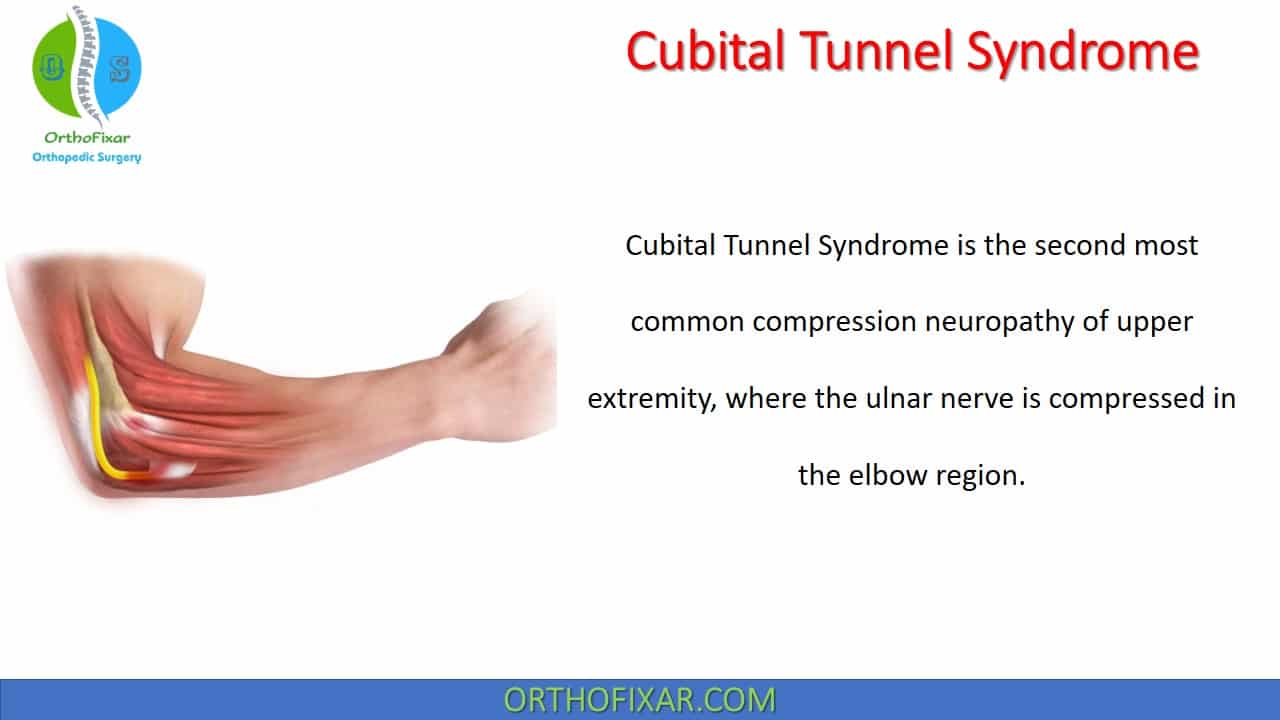
Cubital Tunnel Syndrome is the second most common compression neuropathy of upper extremity, where the ulnar nerve is compressed in the elbow region.
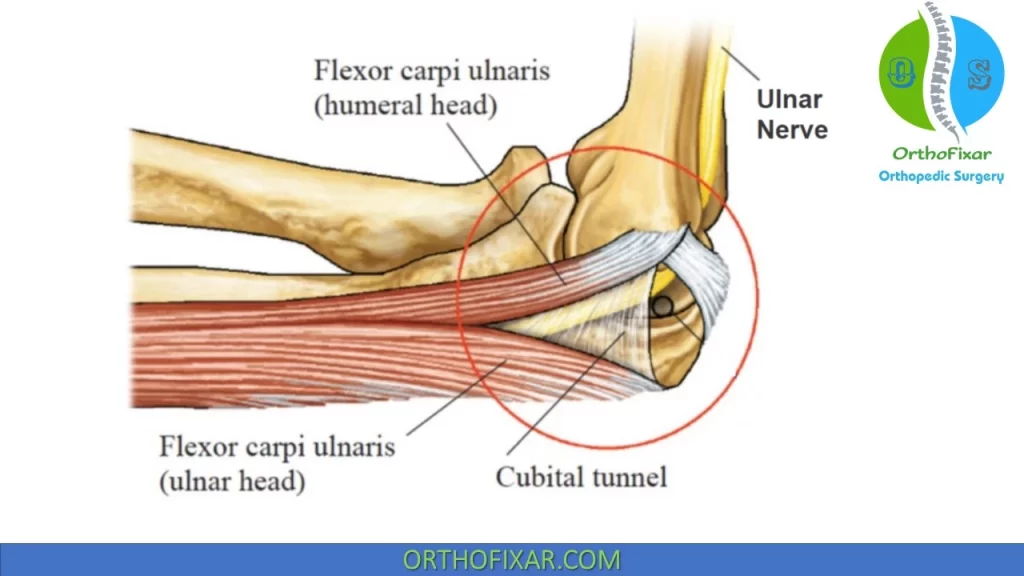
Cubital Tunnel Anatomy
Nirschl has divided the medial epicondylar groove into three zones:
- Zone I: proximal to the medial epicondyle;
- Zone II: the level of the medial epicondyle (retrocondylar groove);
- Zone III: distal to the medial epicondyle (cubital tunnel).
Definition of the cubital tunnel:
- Deep (floor): medial collateral ligament (MCL) and elbow joint capsule.
- Walls of the tunnel: medial epicondyle and olecranon.
- Roof: FCU fascia and arcuate ligament of Osborne (fibrous band that traverses cubital tunnel from medial epicondyle to olecranon).
See Also: Carpal Tunnel Syndrome
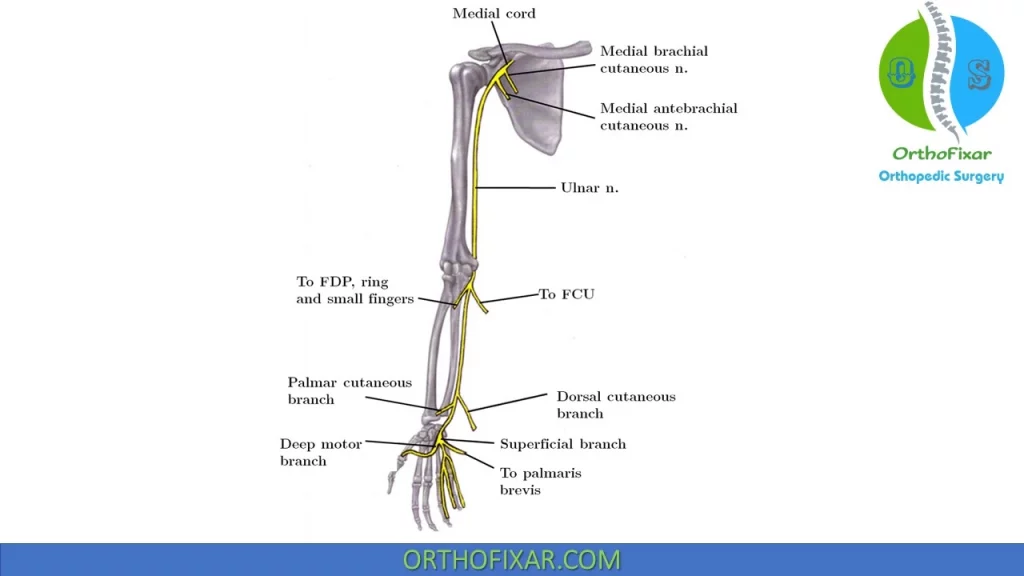
Ulnar Nerve Anatomy
Ulnar nerve arises from the medial cord (C8, T1) of the brachial plexus. It lies posteromedial to brachial artery in upper arm and then passes posterior to the medial intermuscular septum at the arcade of Struthers (8-10 cm from medial epicondyle).
There is No branches in arm, but it supplies articular branch to elbow joint.
Ulnar nerve enters the forearm between the two heads of the FCU (humeral and ulnar), runs between the FCU and FDP, innervating the ulnar half of this muscle (FDP to ring and small fingers).
It runs radial to FCU at distal forearm and wrist.
Dorsal cutaneous nerve branches approximately 7 cm proximal to ulnar styloid and provides sensation to dorsoulnar forearm and wrist.
Ulnar nerve enters hand superficial to transverse carpal ligament through Guyon canal, and divides into a superficial sensory branch (palmaris brevis and skin) and a deep motor branch:
- Deep branch travels around the hook of the hamate between the abductor digiti minimi and flexor digiti minimi brevis, providing motor to intrinsic muscles of hand.
- Sensory branch supplies ulnar half of the ring and the small finger.
See Also: Elbow Anatomy
The muscles innervated by the ulnar nerve include:
Flexor carpi ulnaris, flexor digitorum profundus (third and fourth), pollicis brevis, abductor digiti minimi, opponens digiti minimi, flexor digiti minimi, third and fourth lumbrical muscles, interossei, adductor pollicis, deep head of flexor pollicis brevis.
Cubital Tunnel Syndrome Causes
The causes of Cubital Tunnel Syndrome based on the medial epicondylar groove:
- Repetitive overuse can result in compression of the ulnar nerve in zone III by a tight FCU muscle.
- Entrapment can also be precipitated in zones II and III by a subluxating ulnar nerve,
- Elbow synovitis in zone II.
- Cubitus valgus deformity in zone I or II.
- Medial intermuscular septum in zone I , which slopes from a thick wide base at the medial epicondyle, to a weak and thin edge more proximal on the humeral shaft.
It has been suggested that because of the superficial location of the ulnar nerve, repetitive motion may initiate a cycle of inflammation and edema that inhibits the normal gliding of the nerve.
Additional injury occurs when traction forces caused by elbow flexion produce an additional compressive force on the internal architecture of the nerve.
The anconeus has also been reported as a cause of cubital tunnel syndrome and has been found to occur in 3–28% of human anatomic specimen elbows, and in as many as 9% of patients undergoing surgical treatment for cubital tunnel syndrome.
Sites of compression:
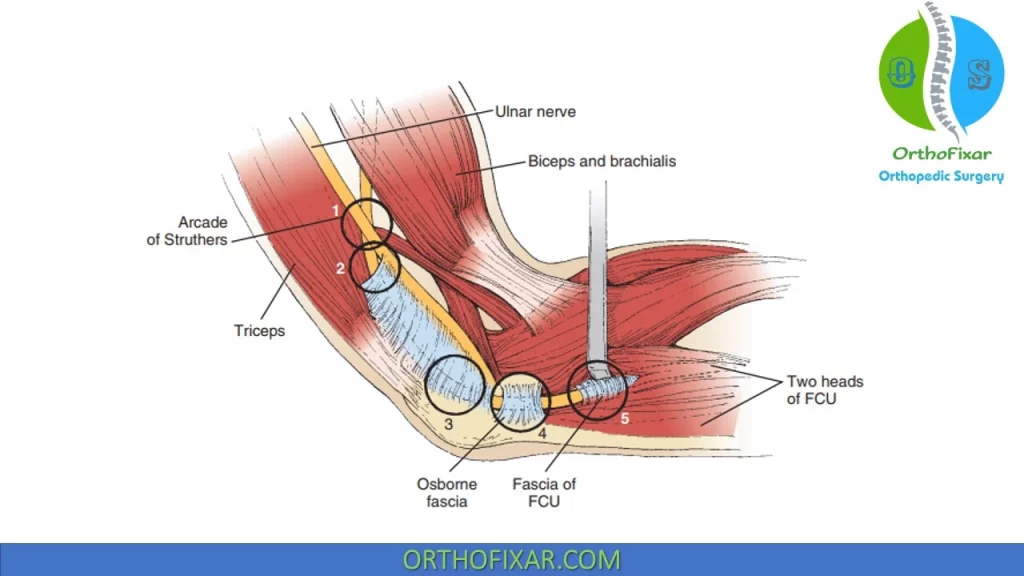
Sites of compression of ulnar nerve in Cubital Tunnel Syndrome include:
- Arcade of Struthers (fascial thickening at hiatus of medial intermuscular septum as the ulnar nerve passes from anterior to posterior compartment 8 cm proximal to the medial epicondyle).
- Medial head of triceps.
- Medial intermuscular septum.
- Osborne ligament.
- Anconeus epitrochlearis (anomalous muscle originating from medial olecranon and inserting on medial epicondyle).
- Between two heads of FCU muscle/aponeurosis.
- Aponeurosis of proximal edge of FDS.
Other potential external sources of compression:
- tumors,
- ganglions,
- osteophytes,
- heterotopic ossification,
- medial epicondyle nonunion.
Symptoms & Signs
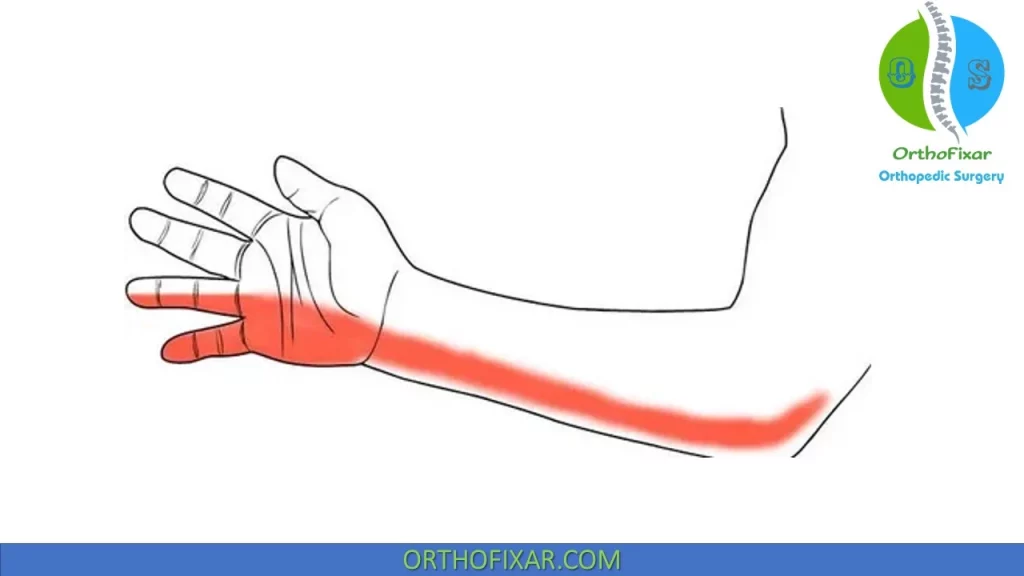
The clinical findings for an ulnar nerve syndrome depend on the location of the lesion and may include:
- activity-related pain or paresthesias involving the fourth and fifth digits, accompanied by pain that may extend proximally or distally in the medial aspect of the elbow;
- pain or paresthesias worse at night;
- decreased sensation in the ulnar distribution of the hand;
- progressive inability to separate the fingers;
- loss of grip power and dexterity;
- atrophy or weakness of the ulnar intrinsic muscles of the hand (late sign);
- clawing contracture of the ring and little fingers (late sign);
- positive elbow flexion and pressure-provocative test;
- positive Wartenberg’s sign, Froment’s sign and Jeanne sign.
- positive Tinel’s sign at the elbow.
Check for subluxation of ulnar nerve over medial epicondyle during elbow flexion-extension arc.
Conduction velocity of less than 50 m/sec across elbow typical threshold for diagnosis; larger decreases in conduction velocity signal worse disease.
Cubital Tunnel Syndrome Treatment
Conservative treatment is recommended for patients with intermittent symptoms and without changes in two point discrimination or muscle atrophy.
Non-operative treatment of cubital tunnel syndrome include:
- Activity modification with protection over the cubital tunnel with an elbow pad placed on the medial-posterior aspect,
- limiting repetitive extreme elbow flexion,
- night splinting at 40–60 degrees may be helpful. In severe cases, the splint is worn during the day, or the elbow is cast at about 45 degrees.
- Exercises must not reproduce the distal nerve symptoms and may, therefore, initially need to be performed in limited arcs of motion.
Surgical treatment indications include:
- For those patients who fail to respond to conservative management after 3–4 months,
- Patients who have muscle atrophy,
- persistent sensory changes,
- persistent symptoms.
Cubital tunnel syndrome surgery include surgical decompression, or an anterior transposition of the ulnar nerve is available.
Recent meta-analyses of techniques fail to show statistically significant difference in outcome between simple decompression and transposition of ulnar nerve.
Persistent postoperative medial/posterior elbow pain may be secondary to neuroma formation from iatrogenic injury to branches of the medial antebrachial cutaneous nerve.
References
- Nirschl RP. Soft-tissue injuries about the elbow. Clin Sports Med. 1986 Oct;5(4):637-52. PMID: 3768969. Pubmed
- Lundborg G. Surgical treatment for ulnar nerve entrapment at the elbow. J Hand Surg Br. 1992 Jun;17(3):245-7. doi: 10.1016/0266-7681(92)90106-c. PMID: 1624851. Pubmed
- Dellon AL. Musculotendinous variations about the medial humeral epicondyle. J Hand Surg Br. 1986 Jun;11(2):175-81. doi: 10.1016/0266-7681(86)90254-8. PMID: 3734552. Pubmed
- Preston D, Shapiro B: Electromyography and Neuromuscular Disorders. Clinical Electrophysiologic Correlations. Boston, MA: Butterworth-Heinemann, 1998.
- O’Connor FG, Wilder RP, Sobel JR: Overuse injuries of the elbow. J Back Musculoskel Rehabil 4:17–30, 1994.
- Idler RS. General principles of patient evaluation and nonoperative management of cubital syndrome. Hand Clin. 1996 May;12(2):397-403. PMID: 8724591.
- Bozentka DJ. Cubital tunnel syndrome pathophysiology. Clin Orthop Relat Res. 1998 Jun;(351):90-4. PMID: 9646751.
- Andrews K, Rowland A, Pranjal A, Ebraheim N. Cubital tunnel syndrome: Anatomy, clinical presentation, and management. J Orthop. 2018 Aug 16;15(3):832-836. doi: 10.1016/j.jor.2018.08.010. Erratum in: J Orthop. 2020 Dec 14;23:275. PMID: 30140129; PMCID: PMC6104141.