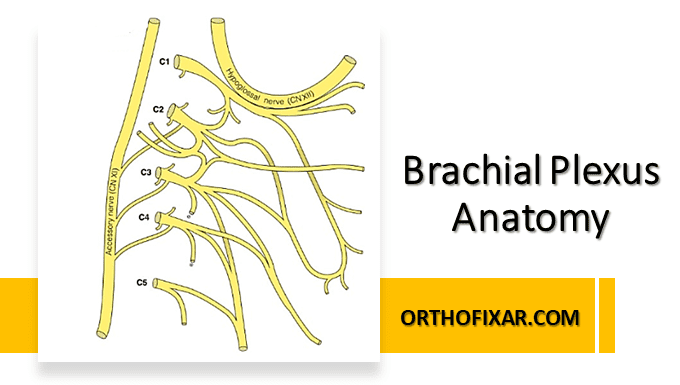
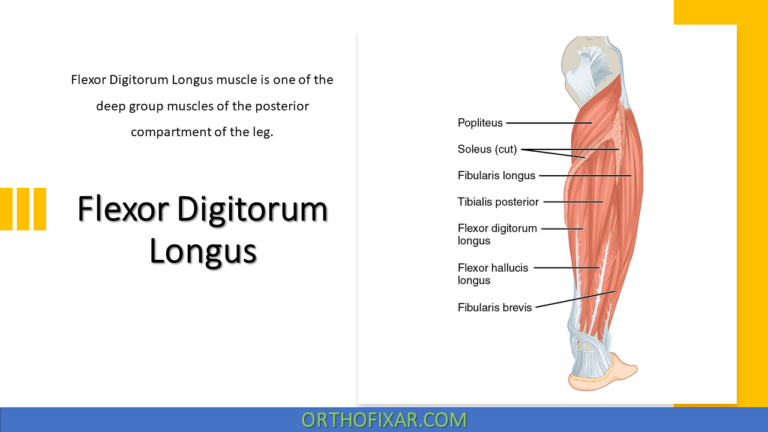
Brachial Plexus Anatomy describes a complex network of peripheral nerves that originates from the anterior rami of the cervical and upper thoracic spinal nerve roots C5, C6, C7, C8, and T1. The brachial plexus typically begins to form distal to the scalene muscles in the neck. Anatomical variations are common, with C5 occasionally receiving fibers from C4 and T1 sometimes receiving contributions from T2.
After exiting the intervertebral foramina, each spinal nerve root receives a sympathetic component via a gray ramus communicans. The cervical nerve roots obtain their sympathetic fibers from the lower cervical sympathetic ganglia, while the T1 nerve root receives its sympathetic supply from the first thoracic sympathetic ganglion, after contributing a white ramus communicans.
Brachial plexus palsy may occur in newborns following difficult or traumatic childbirth (obstetric brachial plexus injury) or in adults as a result of trauma, accidents, or shoulder injuries. Understanding the detailed anatomy of the brachial plexus is essential for accurate diagnosis and management of these nerve injuries.

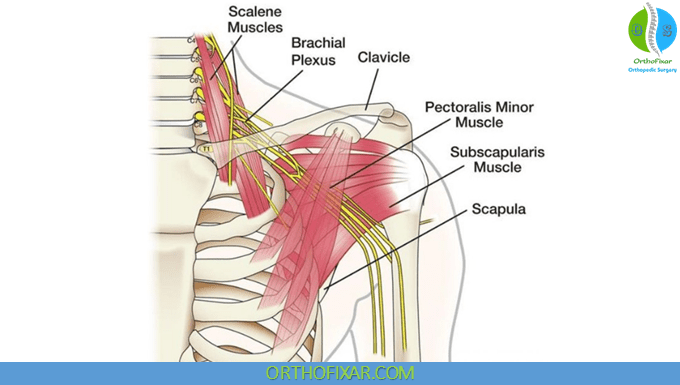
Parts of Brachial Plexus:
The Brachial Plexus consists of ( 5 Roots – 3 Trunks – 6 Divisions – 3 Cords – 5 Terminal Branches) respectively :
- The 5 Roots are the anterior rami of (C5 – C6 – C7 – C8 – T1) as mentioned above.
- The 3 Trunks are ( Upper – Middle – Lower trunk).
- The 6 Divisions are anterior and posterior of each trunks.
- The 3 Cords are ( Lateral – Posterior – Medial).
See Also: Brachial Plexus Palsy
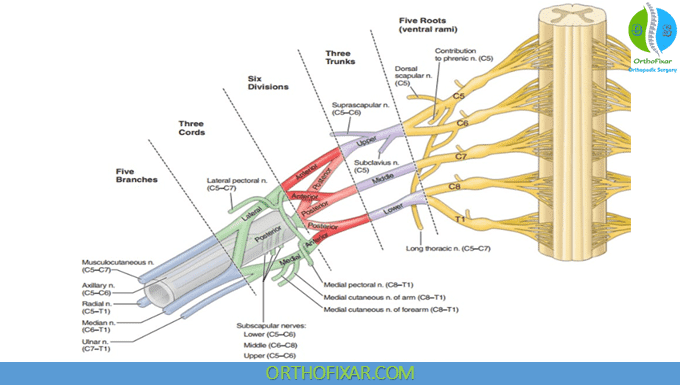
The only nerves that arise from the Brachial Plexus root directly are:
Dorsal scapular nerve:
- Dorsal scapular nerve arises from C5 root, it’s the first important branch seen when the plexus is explored superior to the clavicle.
- It supplies the rhomboids and the levator scapulae muscles.
- Its lesions can result from a forward posture of the head and the neck as this position increases tension in the anterior cervical spine, producing the potential for hypertonicity and hypertrophy of the medial scalene.
- The chief complaint is usually one of scapular pain radiating to the lateral shoulder and arm.
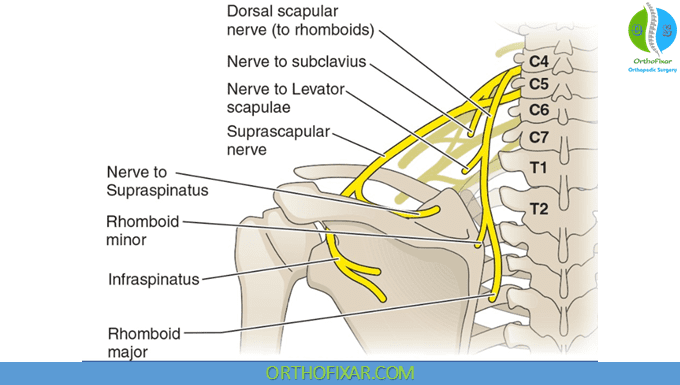
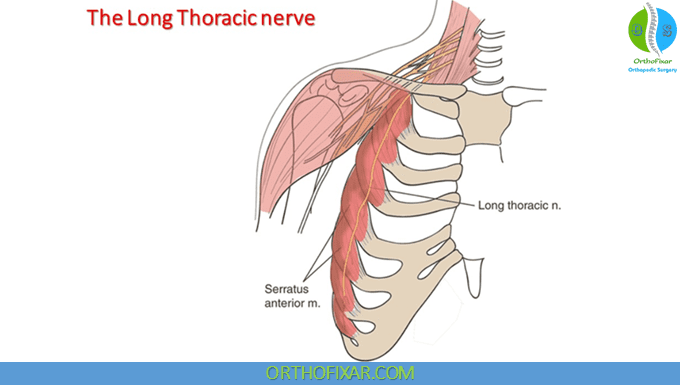
The Long Thoracic nerve:
- The long thoracic nerve (C5–7) is purely a motor nerve that originates from the anterior (ventral) rami of the fifth, the sixth, and the seventh cervical roots.
- It is the sole innervation to the serratus anterior muscle.
- The long thoracic nerve extends as far inferior as the eighth or the ninth rib.
Its long and relatively superficial course makes it susceptible to injury from any of the following causes:
- Entrapment of the fifth and the sixth cervical roots, as they pass through the scalenus medius muscle
- Compression of the nerve during traction to the upper extremity by the undersurface of the scapula, as the nerve crosses over the second rib.
- Compression and traction to the nerve by the inferior angle of the scapula during general anesthesia or with vigorous passive abduction of the arm.
The most common cause of long thoracic nerve injury results from carrying a heavy object on the shoulder. Other causes include:
- postinfection,
- postinjection,
- postpartum,
- postoperative.
The typical clinical presentation includes the following:
- Vague pain in the neck and the scapula region
- An inability to fully elevate the arm overhead
- Shoulder flexion and abduction are weak and limited in AROM due to the loss of the trapezius–serratus anterior force couple.
- The clinician should note winging of the scapula when testing the serratus anterior.
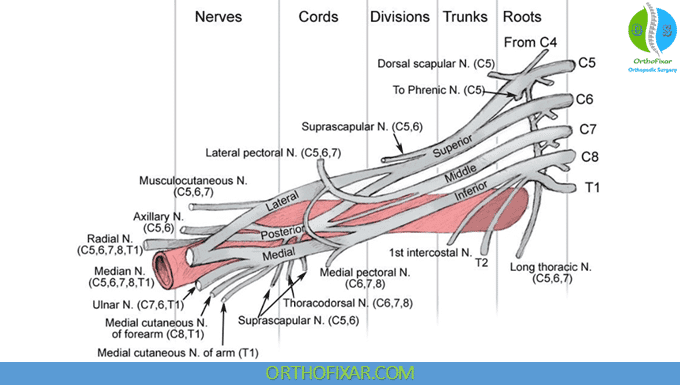
The Trunks:
There are three trunks formed from the united of the roots, they proceed infero-laterally behind the clavicle.
The three trunks are:
- The Upper trunk is formed by the united of C5 & C6 cervical roots.
- The Middle trunks is formed by the C7 cervical root alone.
- The Lower trunk is formed by the united of the C8 & T1.
The upper trunk gives arise to:
- Suprascapular nerve.
- Subclavius nerve.
The subclavius muscle acts mainly on the stability of the sternoclavicular joint, with more or less intensity, according to the degree of the clavicular interaction with the movements of the peripheral parts of the superior limb, and seems to act as a substitute for the ligaments of the sternoclavicular joint.
The Divisions:
Each trunk is divided into two divisions:
- Anterior Division.
- Posterior Division.
No Nerves arise from the divisions.
The Cords:
The Lateral Cord is formed by the united of the anterior divisions of the upper and middle trunks, it gives arise to the:
- Lateral Pectoral Nerve (C5 – C6 – C7).
The Posterior Cord is formed by the united of the three posterior divisions, , it gives arise to the (Respectively from proximal to distal):
- Upper Subscapular Nerve (C5 – C6): supplies the subscapularis muscle
- Thoracodorsal (Middle Subscapular) Nerve (C6 – C7 – C8): This nerve courses along the posterior–lateral chest wall, along the surface of the serratus anterior, and deep to the subscapularis, giving rise to branches that supply the latissimus dorsi.
- Lower Subscapular Nerve (C5 – C6): supplies the teres major and part of the subscapularis muscle.
The Medial Cord is formed by the anterior division of the lower trunk alone, it gives arise to the (Respectively from proximal to distal):
- Medial Pectoral Nerve (C5 – C6 – C7).
- Medial Brachial Cutaneous Nerve (T1).
- Medial Antebrachial Cutaneous Nerve (C8 – T1).
These cords is named based on their relationship with the axillary artery:
- Lateral Cord is located lateral to the axillary artery.
- Posterior Cord is located posterior to the axillary artery.
- Medial Cord is located medial to the axillary artery.
Notice: The lateral pectoral nerve and the medial pectoral nerve communicate by an anastomotic loop.
The medial and lateral pectoral nerves supply the pectoralis major (it has dual innervation) and pectoralis minor muscles.
The lateral pectoral nerve (C5–7) is actually more medial in the muscle, travels with the thoracoacromial vessels, and innervates the clavicular and sternal heads.
The medial pectoral nerve (C8–T1) shares a course with the lateral thoracic vessels and provides innervation to the sternal and costal heads. The main trunk of these nerves can be found near the origin of the vascular supply of the muscle.
Terminal Branches:
- The Musculocutaneous Nerve (C5 – C6 – C7): arises from the lateral cord.
- The Axillary Nerve (C5 – C6): arises from the posterior cord.
- The Radial Nerve (C5 – C6 – C7 – C8 – T1): arises from the posterior cord.
- The Median Nerve (C5 – C6 – C7 – C8 – T1): arises from the lateral & medial cord.
- The Ulnar Nerve (C7 – C8 – T1): arises from the medial cord.
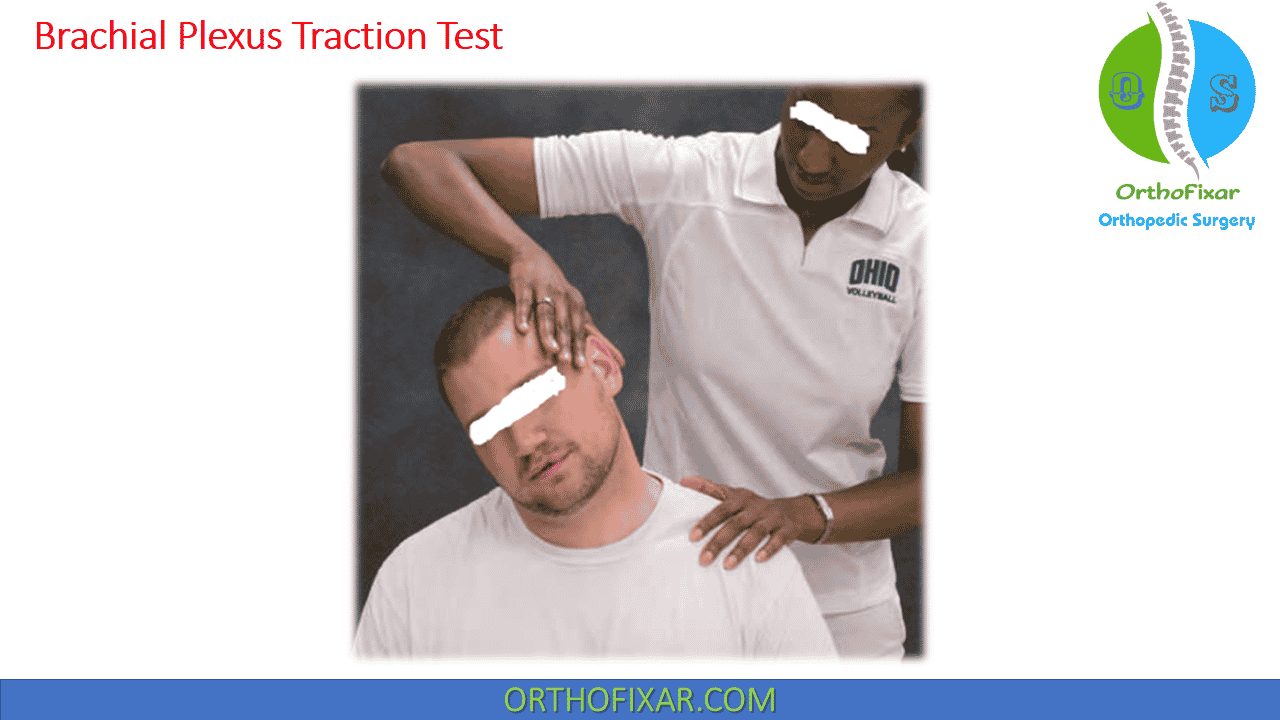
Brachial Plexus Traction Test
The patient seated or standing, with the examiner standing behind the patient. One hand is placed on the side of the patient’s head; the other hand is placed over the AC joint, stabilizing the trunk. The cervical spine is laterally bent and the opposite shoulder depressed.
Positive test if reproduction of pain and/or paresthesia symptoms throughout the involved upper extremity, indicating:
- Brachial plexus neurapraxia.
- Radiating pain on the side opposite the lateral bending: Tension (stretching) of the brachial plexus
- Radiating pain on the side toward the lateral bending: Compression of the cervical nerve roots between two vertebrae.
This test should not be performed until the possibility of a cervical fracture or significant instability has been ruled out.

References
- Polcaro L, Charlick M, Daly DT. Anatomy, Head and Neck, Brachial Plexus. [Updated 2021 Aug 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: Pubmed
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Millers Review of Orthopaedics -7th Edition Book.
- Campbel’s Operative Orthopaedics 12th edition Book.