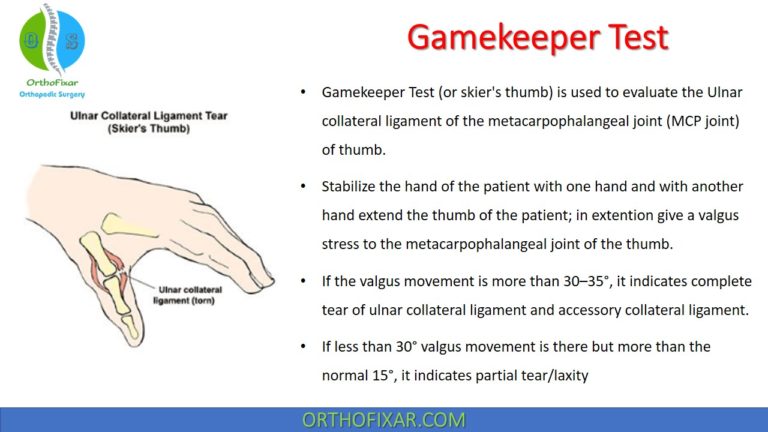
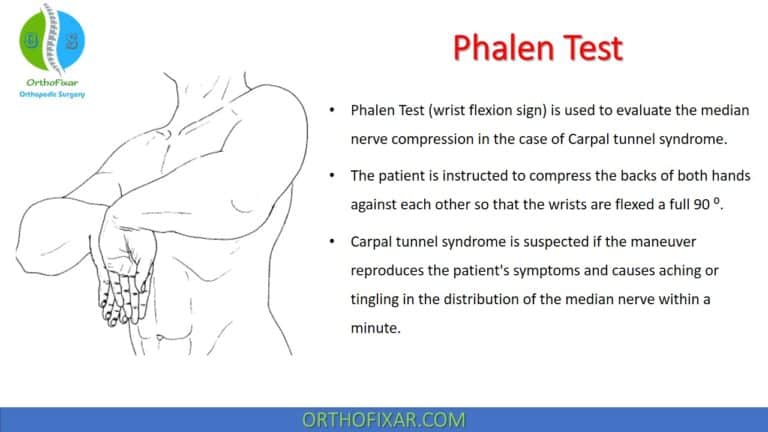
Jeanne Sign is used to test for Ulnar nerve motor weakness. It’s Hyperextension of the thumb metacarpophalangeal joint (MCP) during key pinch.
How do you perform Jeanne Sign ?
The examiner asks the patient to demonstrate a key pinch movement.

Ulnar Nerve Other Tests:
What does a positive Jeanne Sign mean?
The Jeanne Sign is considered positive if patient’s first metacarpophalangeal joint is hyperextended during the maneuver.
Note
- Strong pinch requires both thumb opposition and adduction.
- Opposition is the refined, unique movement that positions the thumb so that its tip can oppose the finger tips throughout their flexion arcs.
- Once the tips are opposed, especially that of the thumb and index finger, thumb adduction force is necessary for performing work activities.
- If the adductor pollicis is paralyzed, as in ulnar nerve palsy, firm index and middle finger pinch is impossible, and the thumb cannot be brought across the palm for pinch with the ring and little fingers.
- The flexor pollicis longus can provide some adduction power when the thumb is held in slight adduction so that the muscle flexes the digit through an arc parallel to the plane of the palm.
- Eventually, the interphalangeal joint of the thumb becomes hyperflexed as the flexor pollicis longus attempts to produce pulp pinch (Froment sign) and the metacarpophalangeal joint becomes hyperextended secondary to unbalanced extensor forces (Jeanne sign).
Ulnar Nerve Palsy
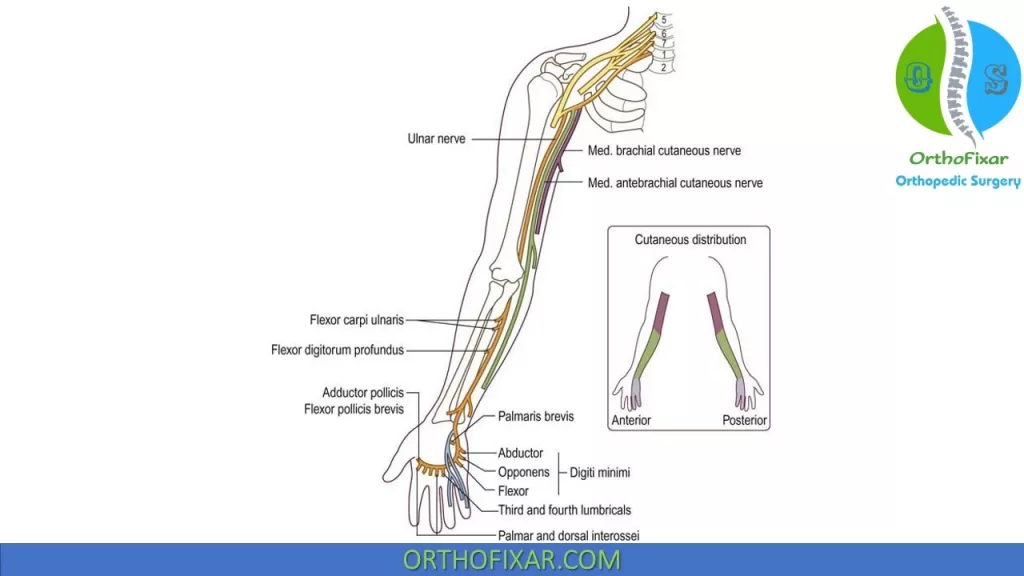
The ulnar nerve is composed of fibers from C8 and T1 coming from the medial cord of the brachial plexus.
It is most commonly compressed at the elbow in the region of the cubital tunnel and less frequently at the wrist in the Guyon canal. With compression of the ulnar nerve, patient complaints will include paresthesia or numbness, or both, in the small or the ring finger, or in both. In more severe cases, ulnar nerve motor dysfunction will lead to weakness, atrophy, and hand clumsiness.
It may be divided at any point along its course by missile wounds or lacerations:
- When it is injured in the upper arm, other nerves or the brachial artery because of their proximity also may be injured.
- In the middle of the arm the ulnar nerve is relatively protected,
- but in the distal arm and at the elbow it often is injured by dislocations of the elbow and supracondylar and condylar fractures.
An ulnar nerve deficit complicating a fracture or dislocation may be caused by the initial trauma, by repeated manipulations of the osseous injury, or by scar formation developing sometime after injury.
The nerve is injured most commonly in the distal forearm and wrist; in these locations it may be injured by gunshot wounds, lacerations, fractures, or dislocations. Traction on the nerve, subluxation or dislocation of the nerve, and entrapment syndromes also can cause ulnar nerve deficits that may require surgical treatment.
Tardy ulnar nerve palsy may develop after malunited fractures of the lateral humeral condyle in children, displaced fractures of the medial humeral epicondyle, dislocations of the elbow, and contusions of the nerve.
In malunion of the lateral humeral condyle, cubitus valgus develops; in this deformity, the ulnar nerve is gradually stretched and can become incompletely paralyzed.
Tardy ulnar nerve palsy also may develop in patients who have a shallow ulnar groove on the posterior aspect of the medial humeral epicondyle, hypoplasia of the humeral trochlea, or an inadequate fibrous arch that normally keeps the nerve in the groove, resulting in recurrent subluxation or dislocation of the nerve.
In most patients, flexion of the elbow aggravated the symptoms of pain and paresthesias.
Cubitus varus deformities also may be associated with tardy ulnar nerve palsy.
Entrapment or compression of the ulnar nerve also may occur at the supracondylar process of the humerus medially (also associated with median nerve compression), at the arcade of Struthers near the medial intermuscular septum, between the heads of origin of the flexor carpi ulnaris, and at the wrist in the Guyon canal.
In other areas, the nerve may be compressed by tight fascia or ligaments, neoplasms, rheumatoid synovitis, aneurysms, vascular thromboses, or anomalous muscles.
Postoperative ulnar nerve palsy may result from direct pressure on the ulnar nerve at the elbow or prolonged flexion of the elbow during surgery.

Reference
- Sarvdeep S. Dhatt, Sharad Prabhakar – Handbook of Clinical Examination in Orthopedics.
- Campbel’s Operative Orthopaedics 12th edition book.
- Drury W, Stern PJ. Froment’s paper sign and Jeanne’s sign– unusual etiology. J Hand Surg Am. 1982 Jul;7(4):404-6. doi: 10.1016/s0363-5023(82)80154-8. PMID: 6288794.