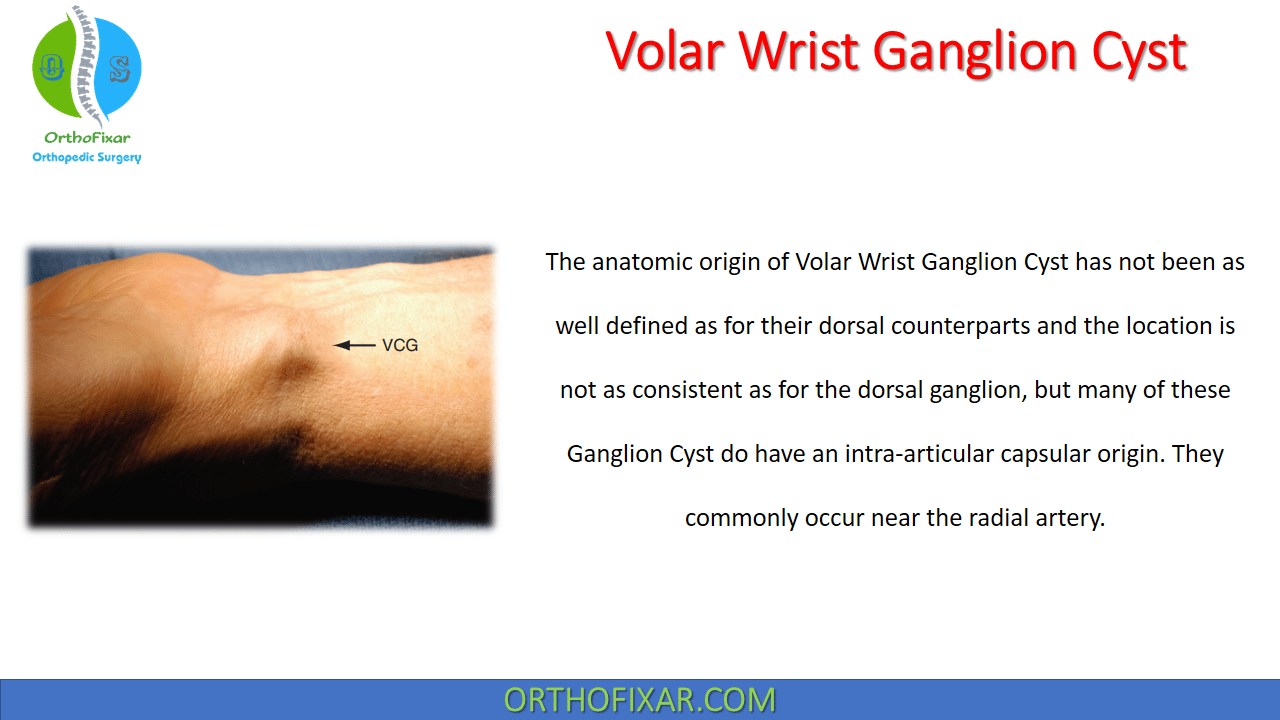
The anatomic origin of volar ganglion cyst in the wrist has not been as well defined as for their dorsal counterparts and the location is not as consistent as for the dorsal ganglion, but many of these Ganglion Cyst do have an intra-articular capsular origin. They commonly occur near the radial artery.
Ganglion cysts are saclike structures that do not have a true cellular lining. They are benign soft tissue tumors that are most commonly found in the wrist but may occur adjacent to or originating from any joint. Approximately 10% of the time, they form from tendon sheaths. They are filled with a viscous fluid that contains glucosamine, albumin, globulin, and hyaluronic acid.
Volar Ganglion Cyst Causes
The origin of most Volar ganglion cysts is idiopathic. Occasionally, a traumatic event precedes the development of a cyst, lending support to a possible traumatic origin of these lesions. These masses are not inflammatory, and they do not arise as simple herniations from the joint capsule.
Other Volar Ganglion Cyst Causes are:
- Capsular rents caused by preexisting joint pathology,
- Synovial fluid leakage with secondary cyst formation,
- Mucoid degeneration or mucin secretion stimulated by joint stress or other degenerative processes.
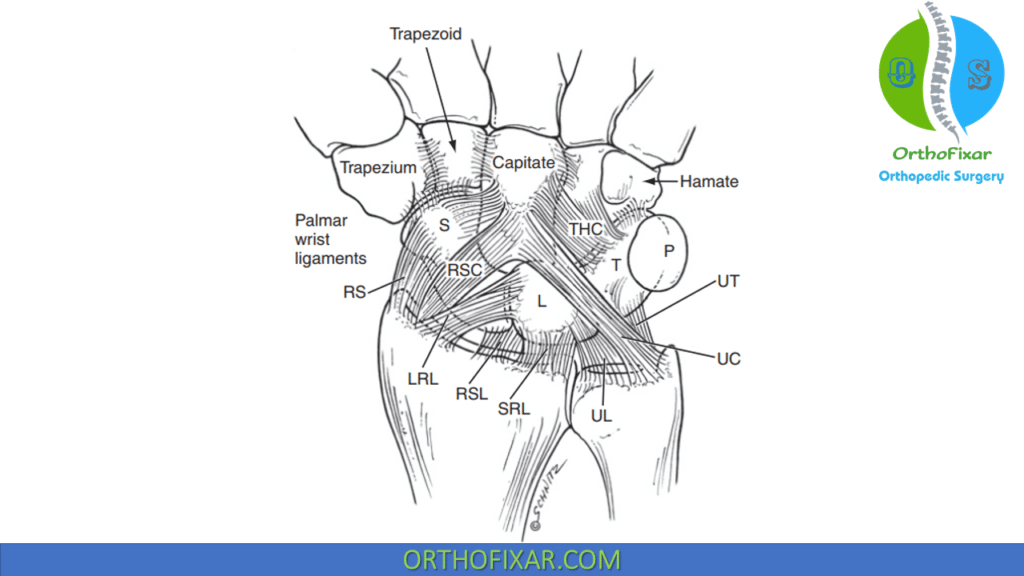
Symptoms may be caused by capsular injury, inflammatory changes, or local pressure. The anatomic origin of the volar ganglion cyst is not as well defined as that of its dorsal counterpart. The literature suggests a radioscaphoid, scaphotrapezial, or trapeziometacarpal (TM) joint origin. Volar cysts may also arise from the flexor carpi radialis (FCR) tendon sheath or other aberrant locations. Most arise from the radiocarpal joint, and when they do, they have a volar capsular origin from the relatively deficient area between the radioscaphocapitate (RSC) and long radiolunate (LRL) ligaments
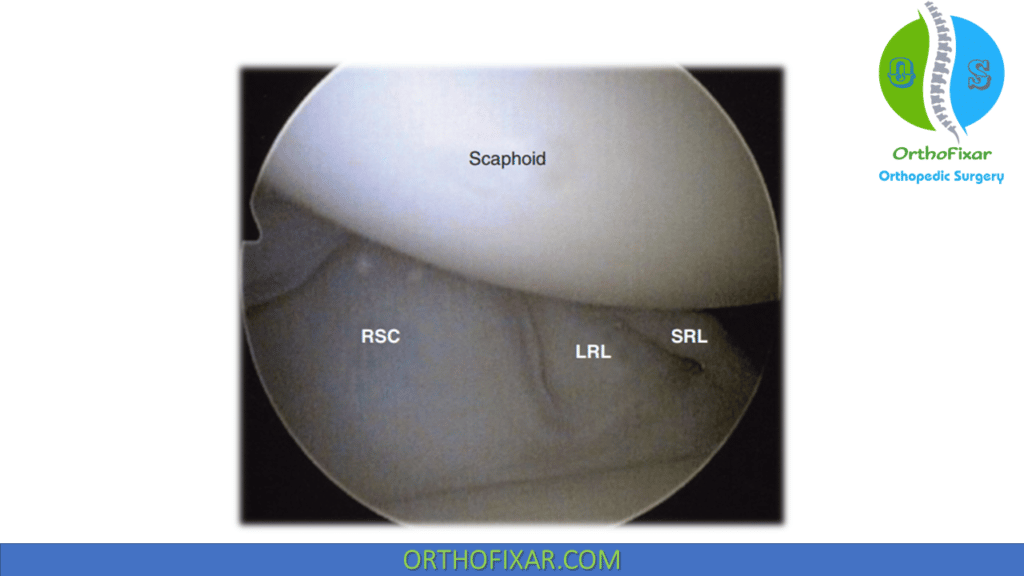
The ligaments represent the volar extrinsic components that work in conjunction with the intrinsic and extrinsic dorsal ligaments and with the interosseous ligaments to provide wrist stability. Starting radially and proceeding in an ulnar direction, they are the RSC, the LRL, and the short radiolunate (SRL) ligaments. When they are visualized arthroscopically, distinct clefts can be seen between these ligaments.
See Also: Wrist Anatomy
Clinical Evaluation
Most volar ganglion cysts occur in women in their second, third, or fourth decade of life. The onset is usually insidious, with a progressive increase in size occurring over many years. The ganglion usually manifests as a visible and palpable mass. Patients may relate a traumatic event, such as a wrist hyperextension injury, that occurred before the cyst appeared; however, most cannot recall an event or activity related to the development or appearance of the mass.
The masses may be painful, and the symptoms usually are described as an aching discomfort in the region of the mass. Cosmetic dissatisfaction and concern that the mass represents a malignancy are associated complaints. A painless mass is the most frequent presenting complaint.
Volar Wrist Ganglion Cyst usually is a 1- to 2-cm, round or ovoid mass usually manifests as a visible fullness in the interval between the FCR tendon and the radial artery. It may be unilobular or multilobular. Palpation reveals a mass that may be slightly tender. The consistency is usually soft and compressible, although chronic lesions may be quite firm. Transillumination with a penlight usually confirms the diagnosis.
The differential diagnosis includes vascular lesions of the radial artery, and it is important to determine whether the mass is pulsatile or the pulsations of the radial artery can be distinguished from the mass itself. Despite the relatively easy diagnosis, it is important to exclude other causes of wrist discomfort, such as radiocarpal arthrosis, STT arthrosis, TM arthrosis, De Quervain’s tendonitis, and FCR tendonitis.
Isolated loading and stress testing of the individual joints should not produce any pain if the joint is not arthritic. The result of a Finkelstein maneuver should be negative, and there should be no tenderness of the first dorsal compartment tendons. Resisted wrist flexion should produce no pain over the FCR tendon. In patients with an occult volar ganglion cyst, the only positive physical finding may be fullness in the FCR–radial artery interval and pain with pressure in the region. Exclusion of other potential causes of volar radial wrist pain is essential.
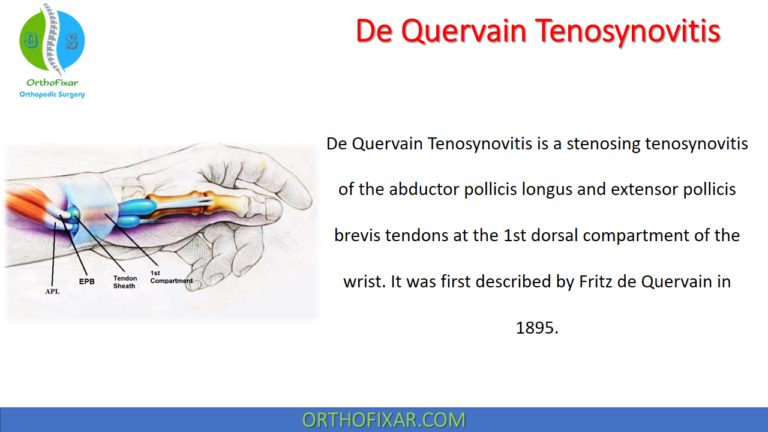
See Also: De Quervain Tenosynovitis
Imaging Study
If the diagnosis is certain and the physical examination presents no confounding findings, imaging is not necessary. When desired, plain radiographs are usually sufficient as an imaging study to exclude arthrosis of the STT or TM joint.
Arthroscopic management of volar ganglion cyst is indicated only for capsular radiocarpal origins; preoperative radiographs that demonstrate arthrosis raise suspicion that the cyst may arise from a location other than the radiocarpal joint. .
If the nature of the mass is unclear, ultrasound or magnetic resonance imaging is useful. Ultrasound is a cost-effective study that demonstrates the mass as a hypoechoic lesion.
Volar Ganglion Cyst Wrist Treatment
Conservative treatment of symptomatic volar ganglion cysts is somewhat limited. Historically, conservative treatment of ganglions has included:
- External pressure with a variety of topical agents and mechanical devices,
- External rubbing or massage,
- Closed rupture with the use of digital pressure or more violent means, such as striking the mass with a heavy book, which accounts for the designation Bible cyst.
These techniques are associated with recurrence rates as high as 64%. Spontaneous resolution of ganglia occurs in approximately 50% of patients but can take many years.
Cysts that have developed acutely or after an identifiable traumatic event should be treated with a period of splint immobilization, because the initial symptoms and the mass may resolve. More frequently, patients present with a cyst of insidious origin with a duration of many months or even years, and splinting is not an effective treatment.
Aspiration of Volar Wrist Ganglion has a success rate of only 30% to 50%. The poorest results for aspiration are associated with volar ganglion cysts, and most surgeons caution against aspiration because of the risk of injury to adjacent neurovascular structures such as the radial artery and the palmar cutaneous branch of the median nerve. Aspiration is offered to patients who desire cyst resolution but want to avoid a more involved surgical procedure. Physicians should be certain that adjacent neurovascular structures are separate from the mass and that there is no possibility that the volar mass represents a lesion of vascular origin. Patients should be warned that the failure rate with aspiration is high and that recurrence is likely.
If conservative management has failed to bring about symptom resolution or elimination of the mass, Volar Ganglion Cyst surgical treatment is recommended.
Indications for Arthroscopic Ganglion excision are relative. Patients desire excision of the ganglion cyst to improve cosmesis, to eliminate pain, and for absolute diagnosis and exclusion of potential malignancy. The procedure is recommended for the typical volar ganglion that manifests in the interval between the FCR and the radial artery and is not located distal to the distal wrist flexion crease.
Arthroscopic removal of volar ganglions is contraindicated for masses that may be coming from locations other than the radiocarpal joint capsule, such as the STT joint or the FCR sheath.
Volar Ganglion Cyst removal with open fashion:
- Wrists that have sustained prior trauma or are excessively stiff and may present difficulty in visualization of the volar extrinsic ligaments.
- Unusual or atypical masses that are likely not ganglions.
- Recurrent ganglion cysts.

References
- Gude W, Morelli V. Ganglion cysts of the wrist: pathophysiology, clinical picture, and management. Curr Rev Musculoskelet Med. 2008 Dec;1(3-4):205-11. doi: 10.1007/s12178-008-9033-4. Epub 2008 Aug 26. PMID: 19468907; PMCID: PMC2682407.
- Roth, JH, Poehling GG, and Whipple TL . Arthroscopic surgery of the wrist. Instr Course Lect. 1988 ; 37 : 183 – 194 .
- Osterman AL, Raphael J . Arthroscopic resection of dorsal ganglion of the wrist. Hand Clin. 1995 ; 11 : 7 – 12.
- Ho PC, Law BK, Hung LK . Arthroscopic volar wrist ganglionectomy. Chir Main. 2006 ; 25 (suppl 1): S221 – S230 .
- Kuhlmann JN, Luboinski J, Baux S, Mimoun M . Ganglions of the wrist: proposals for topographical systematization and natural history . Rev Chir Orthop Reparatrice Appar Mot. 2003 ; 89 : 310 – 319 .
- Wang G, Jacobson JA, Feng FY, et al. Sonography of wrist ganglion cysts: variable and noncystic appearances . J Ultrasound Med. 2007 ; 26 : 1323 – 1328; quiz 1330-1331.
- Mathoulin C, Hoyos A, Pelaez J . Arthroscopic resection of wrist ganglia. Hand Surg. 2004 ; 9 : 159 – 164 .
- Psaila JV, Mansel RE . The surface ultrastructure of ganglia . J Bone Joint Surg Br. 1978 ; 60 : 228 – 233 .
- Greendyke SD, Wilson M, Shepler TR . Anterior wrist ganglia from the scaphotrapezial joint . J Hand Surg Am. 1992 ; 17 : 487 – 490 .
- Aydin A, Kabakas F, Erer M , et al . Surgical treatment of volar wrist ganglia. Acta Orthop Traumatol Turc. 2003 ; 37 : 309 – 312 .
- Ho PC, Lo WN, Hung LK . Arthroscopic resection of volar ganglion of the wrist: a new technique . Arthroscopy. 2003 ; 19 : 218 – 221 .
- Thornburg LE . Ganglions of the hand and wrist . J Am Acad Orthop Surg. 1999 ; 7 : 231 – 238 .
- Westbrook AP, Stephen AB, Oni J, Davis TR . Ganglia: the patient’s perception. J Hand Surg Br. 2000 ; 25 : 566 – 567 .
- Wong AS, Jebson PJ, Murray PM, Trigg SD . The use of routine wrist radiography is not useful in the evaluation of patients with a ganglion cyst of the wrist . Hand (N Y). 2007 ; 2 : 117 – 119 .
- Nelson CL, Sawmiller S, Phalen GS . Ganglions of the wrist and hand. J Bone Joint Surg Am. 1972 ; 54 : 1459 – 1464 .
- Dias J, Buch K . Palmar wrist ganglion: does intervention improve outcome? A prospective study of the natural history and patient-reported treatment outcomes . J Hand Surg Br. 2003 ; 28 : 172 – 176 .
- Nahra ME, Bucchieri JS . Ganglion cysts and other tumor related conditions of the hand and wrist . Hand Clin. 2004 ; 20 : 249 – 260, v.
- Wright TW, Cooney WP, Ilstrup DM . Anterior wrist ganglion . J Hand Surg Am. 1994 ; 19 : 954 – 958 .
- Jacobs LG, Govaers KJ . The volar wrist ganglion: just a simple cyst? J Hand Surg Br. 1990 ; 15 : 342 – 346 .
- Greenberg JA . Arthroscopic treatment of volar carpal ganglion cysts . In: Slutsky DJ, Nagle DJ , eds. Techniques in Hand and Wrist Arthroscopy. Philadelphia, PA : Churchill Livingstone/Elsevier ; 2007 : 188 – 190 .
- Rocchi L, Canal A, Fanfani F, Cantalano F. Articular ganglia of the volar aspect of the wrist: arthroscopic resection compared with open excision. A prospective randomised study . Scand J Plast Reconstr Surg Hand Surg. 2008 ; 42 : 253 – 259 .