Navicular stress fracture is a high-risk overuse injury of the midfoot that commonly affects athletes involved in running, jumping, sprinting, and cutting activities. Delayed diagnosis is common because symptoms may initially mimic a simple foot sprain or tendinopathy. Early recognition and appropriate management are critical to prevent nonunion, chronic pain, and prolonged disability.
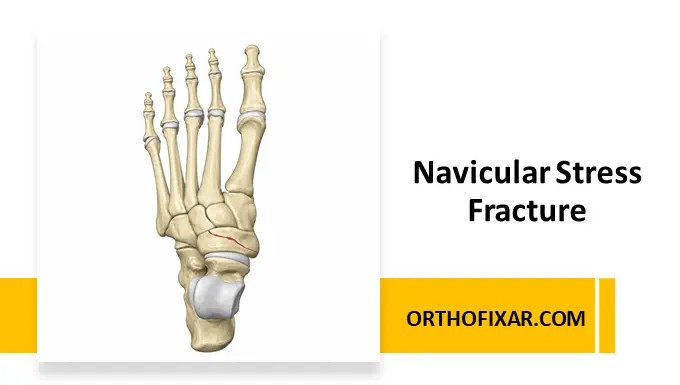
A navicular stress fracture is a fatigue fracture involving the tarsal navicular bone of the foot. It develops due to repetitive mechanical loading that exceeds the bone’s ability to remodel and heal.
The navicular bone plays a central role in maintaining the medial longitudinal arch and transferring forces across the midfoot during gait and athletic activity. Because the central portion of the navicular has relatively limited vascularity, healing may be delayed compared with other stress fractures.
Epidemiology
Navicular stress fractures are relatively uncommon in the general population but are frequently seen in competitive athletes and military recruits.
Sports commonly associated with navicular stress fractures include:
- Track and field
- Basketball
- Soccer
- Tennis
- Rugby
- Gymnastics
- Football
Young male athletes are particularly affected, although female athletes are also at risk, especially in the presence of low bone mineral density or energy deficiency. Navicular stress fractures represent a substantial proportion of high-risk stress fractures in athletes.
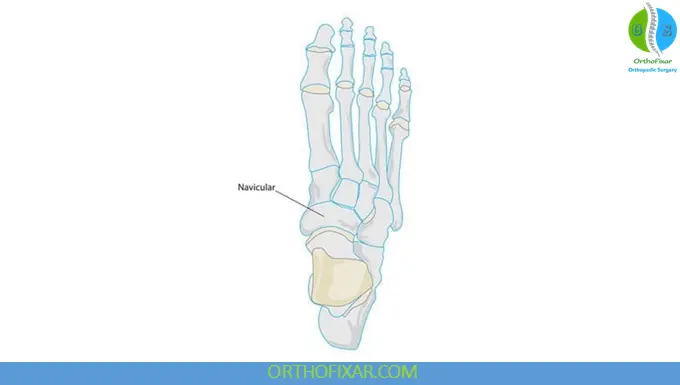
The navicular is located in the medial midfoot between the talus proximally and the cuneiforms distally.
Important biomechanical features include:
- Central role in force transmission
- Contribution to foot arch stability
- High compressive and shear loads during push-off
- Relative hypovascularity in the central third
These characteristics explain why navicular stress fractures are considered high-risk injuries.
See Also: Ankle Anatomy
Causes and Risk Factors
Navicular stress fractures result from repetitive cyclic loading rather than acute trauma.
Intrinsic Risk Factors
- Limited ankle dorsiflexion
- Cavus foot
- Pes planus
- Biomechanical malalignment
- Previous stress fracture
- Poor bone health
- Vitamin D deficiency
- Female athlete triad / RED-S
Extrinsic Risk Factors
- Sudden increase in training intensity
- Hard training surfaces
- Inadequate footwear
- Overtraining
- Insufficient recovery time
Repetitive forefoot loading during sprinting and jumping is particularly implicated in the pathogenesis.
Pathophysiology
Repeated loading creates microdamage within the navicular bone. When bone remodeling cannot keep pace with stress accumulation, a stress reaction develops and may progress to a cortical fracture.
The central avascular region of the navicular contributes to:
- Delayed healing
- Nonunion
- Recurrent stress injury
This is why navicular stress fractures require aggressive management compared with many other stress fractures.
Common Symptoms
Patients usually report:
- Gradual onset dorsal midfoot pain
- Pain during running or jumping
- Pain relieved by rest initially
- Progressive pain with activity
- Reduced athletic performance
Pain often localizes to the dorsal central navicular region, known as the “N spot.”
Physical Examination Findings
Clinical findings may include:
- Tenderness over the dorsal navicular
- Pain with hopping
- Pain during toe walking
- Antalgic gait
- Midfoot swelling (occasionally)
Examination findings can be subtle, contributing to delayed diagnosis.
See Also: Ankle Fractures: Classification, Diagnosis & Treatment
Delayed diagnosis is common, with some studies reporting delays of several months after symptom onset.
Imaging Evaluation
Plain Radiographs
Initial X-rays are often normal in early stress fractures.
Radiographs may eventually demonstrate:
- Cortical lucency
- Sclerosis
- Fracture line
However, radiographs have limited sensitivity.
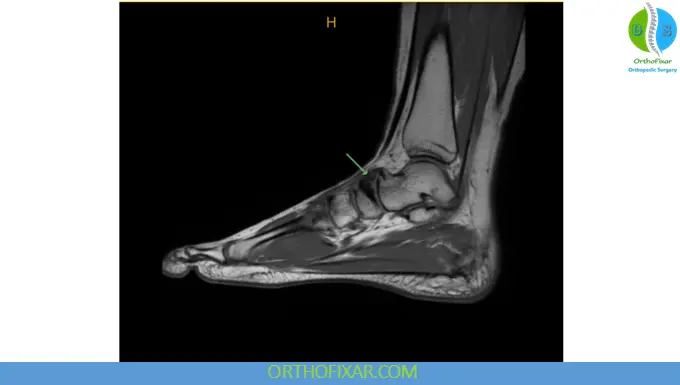
MRI
MRI is highly sensitive for early stress injury detection.
MRI findings include:
- Bone marrow edema
- Stress reaction
- Fracture line
- Associated soft tissue injury
MRI is useful for early diagnosis before cortical fracture progression.
CT Scan
CT is considered the gold standard for defining fracture morphology and assessing healing.
CT helps classify fractures and determine:
- Fracture extent
- Cortical involvement
- Sclerosis
- Delayed union
- Nonunion
See Also: Ankle X-Ray Imaging
Saxena Classification
- Type I: Dorsal cortical fracture only.
- Type II: Fracture extends into the navicular body.
- Type III: Complete fracture through both cortices.
Higher-grade injuries are associated with longer recovery times and increased risk of complications.
Differential Diagnosis
Conditions that may mimic navicular stress fracture include:
- Tibialis posterior tendinopathy
- Midfoot sprain
- Lisfranc injury
- Extensor tendinitis
- Osteoarthritis
- Stress reaction without fracture
- Tarsal coalition
Treatment depends on fracture severity, displacement, athlete demands, and chronicity.
Nonoperative Treatment
Conservative treatment is generally reserved for:
- Incomplete fractures
- Nondisplaced fractures
- Low-demand patients
Standard Conservative Protocol
- Non-weight-bearing cast immobilization
- Immobilization for 6–8 weeks
- Gradual rehabilitation
- Progressive return to sport
Healing rates can be favorable with strict adherence to non-weight-bearing protocols.
Surgical Treatment
Surgery is commonly recommended for:
- Complete fractures
- Displaced fractures
- Elite athletes
- Delayed union
- Nonunion
- Failed conservative treatment
Surgical Techniques
Procedures may include:
- Open reduction and internal fixation (ORIF)
- Screw fixation
- Bone grafting
- Biologic augmentation
Surgical treatment may allow earlier return to sport in selected athletes.
Rehabilitation progresses through phases:
Phase 1: Protection
- Non-weight-bearing
- Pain control
- Immobilization
Phase 2: Early Mobilization
- Gradual weight-bearing
- Range-of-motion exercises
- Intrinsic foot strengthening
Phase 3: Strength and Conditioning
- Calf strengthening
- Proprioception training
- Gait retraining
Phase 4: Return to Sport
- Sport-specific drills
- Running progression
- Plyometric training
Return to sport should occur only after clinical and radiographic healing.
Return to Sport Timeline
Return-to-play timing varies according to fracture severity and treatment method.
Average return to sport may range from:
- 4–6 months after surgery
- 5–8 months with conservative treatment
Elite athletes may require longer rehabilitation depending on imaging findings and symptoms.
Complications
Potential complications include:
- Delayed union
- Nonunion
- Refracture
- Chronic midfoot pain
- Osteoarthritis
- Persistent functional limitation
Delayed diagnosis significantly increases complication risk.
Prevention Strategies
Preventive measures include:
- Gradual training progression
- Adequate recovery periods
- Proper footwear
- Correction of biomechanical abnormalities
- Vitamin D optimization
- Nutritional support
- Cross-training programs
Prognosis
Early diagnosis and proper management generally produce favorable outcomes.
However, navicular stress fractures remain challenging injuries because of:
- Limited vascularity
- High biomechanical stress
- Risk of recurrent injury
Prompt imaging and strict treatment adherence improve long-term outcomes and athletic return rates.
Key Points
- Navicular stress fracture is a high-risk midfoot stress injury.
- Athletes involved in running and jumping sports are most commonly affected.
- MRI and CT are essential imaging modalities.
- Delayed diagnosis is common and worsens prognosis.
- Non-weight-bearing immobilization is the cornerstone of conservative treatment.
- Surgical fixation is frequently used in elite athletes and complete fractures.
- Early diagnosis improves healing and return-to-sport outcomes.
Is navicular stress fracture serious?
Yes. It is considered a high-risk stress fracture because healing may be delayed and complications such as nonunion can occur.
Can you walk with a navicular stress fracture?
Some patients can walk initially, but continued weight-bearing may worsen the fracture and delay healing.
What imaging is best for navicular stress fracture?
MRI is highly sensitive for early diagnosis, while CT is best for fracture characterization and healing assessment.
How long does recovery take?
Recovery commonly requires several months, especially in competitive athletes.
References & More
- Patel KA, Christopher ZK, Drakos MC, O’Malley M. Navicular Stress Fractures. J Am Acad Orthop Surg. 2021. PubMed
- Shakked RJ, Walters EE, O’Malley MJ. Tarsal navicular stress fractures. Curr Rev Musculoskelet Med. 2017. PMC
- Attia AK, Mahmoud K, Bariteau J, et al. Return to sport following navicular stress fracture: systematic review and meta-analysis. Int Orthop. 2021. PubMed
- Burne SG, Mahoney CM, Forster BB, et al. Tarsal navicular stress injury: long-term outcome and clinicoradiological correlation. Am J Sports Med. 2005. PubMed
- Gheewala R, Arain A, Rosenbaum AJ. Tarsal Navicular Fractures. StatPearls. 2023. NCBI