Radial head fractures are among the most common elbow injuries encountered in clinical practice. Proper diagnosis and management are essential to restore function, maintain joint stability, and prevent long-term complications.
Epidemiology
Radial head fractures account for 1.7% to 5.4% of all fractures and approximately one-third of all elbow fractures. Notably, about one-third of patients present with associated injuries, including fractures or ligamentous damage involving the shoulder, humerus, forearm, wrist, or hand.
Anatomy and Biomechanics
The radial head plays a critical role in elbow and forearm function:
- The radial head and capitellum are reciprocally curved, enabling smooth articulation.
- Force transmission across the radiocapitellar joint occurs throughout elbow motion and is greatest in full extension.
- Accurate positioning of the radial head within the lesser sigmoid notch is essential for full forearm rotation.
- The radial head contributes to:
- Valgus stability (secondary restraint)
- Load sharing across the elbow
- Longitudinal forearm stability in conjunction with the interosseous membrane
Loss of radial head integrity—especially when combined with ligament injury—can result in instability and proximal migration of the radius.
See Also: Elbow Anatomy
Mechanism of Injury
Most radial head fractures occur due to:
- Fall onto an outstretched hand (FOOSH)
- Higher-energy trauma such as:
- Falls from height
- Sports injuries
Biomechanical patterns:
- Axial loading with the elbow between 0–80° flexion → radial head fracture
- Combined forces (axial + rotational) may lead to:
- Posterolateral rotatory injuries
- Fracture-dislocations (e.g., Monteggia or olecranon fracture-dislocations)
These injuries are frequently associated with ligamentous damage and, less commonly, capitellar fractures.
Clinical Evaluation
Symptoms:
- Elbow pain
- Limited range of motion (especially rotation)
- Pain with passive forearm rotation
Signs:
- Localized tenderness over the radial head
- Elbow effusion
- Reduced flexion-extension and pronation-supination
Important Assessments:
- Examine wrist and distal radioulnar joint (DRUJ)
→ Wrist pain may indicate an Essex-Lopresti lesion - Evaluate medial collateral ligament (MCL) stability
- Joint aspiration with local anesthetic may:
- Reduce pain
- Help detect mechanical block to motion
Radiographic Evaluation
Standard Imaging:
- Anteroposterior (AP) and lateral elbow X-rays
Special Views:
- Greenspan (radiocapitellar) view improves visualization of the radial head
Key Findings:
- Fat pad sign (especially posterior) suggests occult fracture
- Subtle fractures may not be immediately visible
Advanced Imaging:
- CT scan for:
- Comminution
- Surgical planning
- MRI if soft tissue injury or occult fracture is suspected
See Also: Elbow X-ray Views
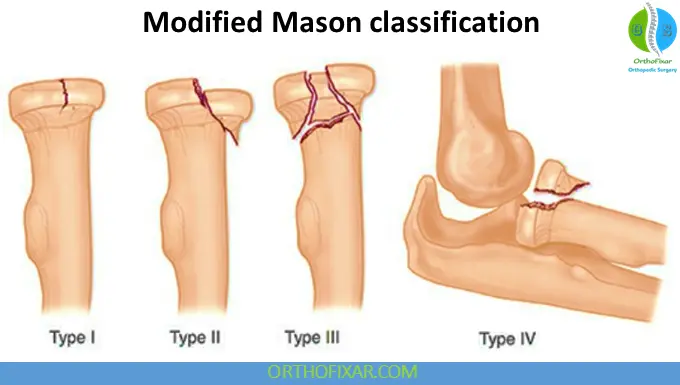
Classification (Modified Mason Classification)
- Type I: Nondisplaced fractures
- Type II: Displaced marginal fractures
- Type III: Comminuted fractures of the entire head
- Type IV: Radial head fracture with elbow dislocation
Treatment
Treatment Goals
- Restore forearm rotation
- Achieve early mobilization
- Maintain elbow and forearm stability
- Prevent long-term complications such as arthrosis
Nonoperative Treatment
Indications:
- Nondisplaced fractures (Type I)
- Displaced fractures without mechanical block
Approach:
- Sling for comfort
- Early mobilization within 24–48 hours
- Optional joint aspiration for pain relief
Operative Treatment
1. Open Reduction and Internal Fixation (ORIF)
Indications:
- Type II fractures with mechanical block to motion
- Large displaced fragments (>2 mm or >25% of head)
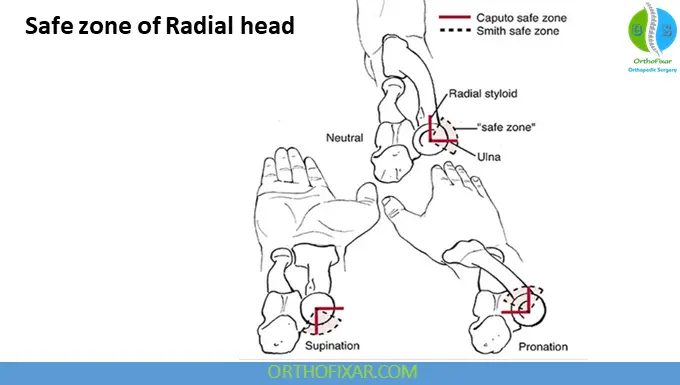
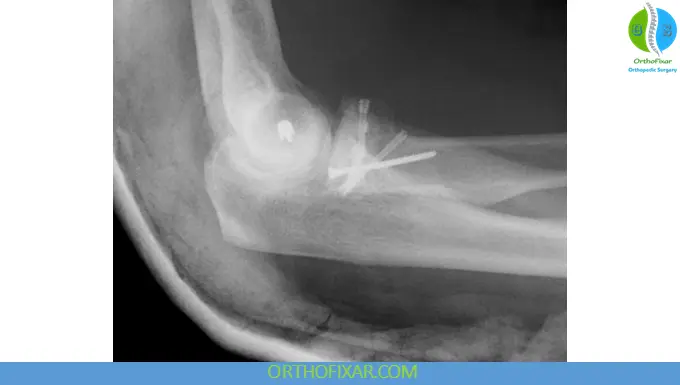
Technique highlights:
- Lateral approach (Kocher or Kaplan)
- Fixation with screws or plates in the safe zone
2. Radial Head Replacement
Indications:
- Comminuted fractures (Type III)
- Unstable elbow or forearm injuries
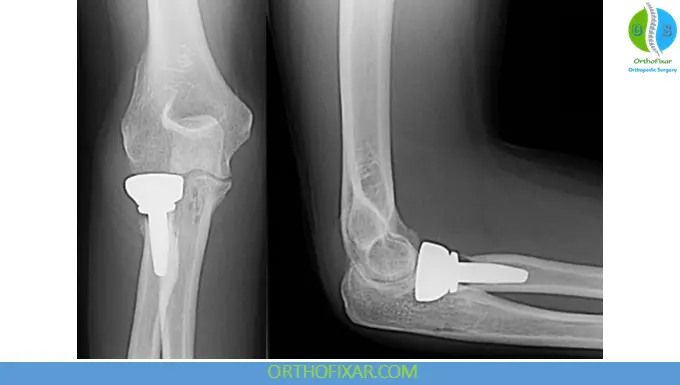
Notes:
- Metallic prostheses (titanium/vitallium) preferred
- Avoid oversizing, which can impair joint mechanics
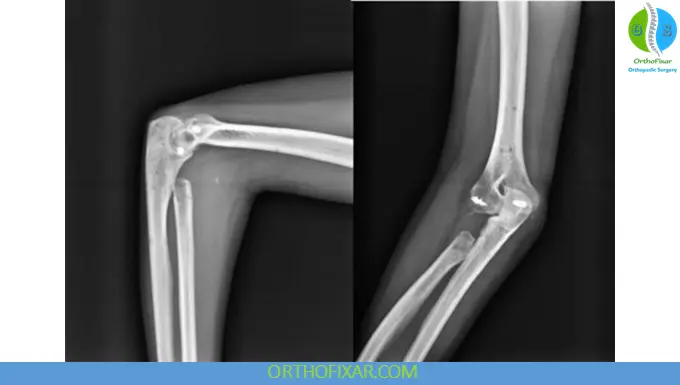
3. Radial Head Excision
- Rarely used in acute settings
- Contraindicated in unstable injuries
- May be considered in chronic cases with good outcomes
Essex-Lopresti Lesion
A complex injury involving:
- Radial head fracture
- Interosseous membrane disruption
- DRUJ instability
Key point:
- Do NOT excise the radial head
→ leads to proximal radial migration
Management:
- Radial head repair or replacement
- Stabilization of DRUJ
See Also: Essex-Lopresti Injury
Postoperative Care
- Early mobilization is critical:
- Begin active or assisted motion within 5–7 days
- Avoid prolonged immobilization
Complications
- Elbow stiffness (contracture)
- Heterotopic ossification
- Chronic wrist pain (missed ligament injury)
- Proximal migration of radius
- Posttraumatic osteoarthritis
- Complex regional pain syndrome (CRPS)
- Chronic instability (rare, often due to missed injuries)
Key Clinical Insights
- Always assess the entire upper limb, not just the elbow
- Wrist pain in radial head fractures is a red flag for Essex-Lopresti injury
- Early motion is essential to prevent stiffness
- Preservation or replacement of the radial head is critical in unstable injuries
References & More
- Pappas N, Bernstein J. Fractures in brief: radial head fractures. Clin Orthop Relat Res. 2010 Mar;468(3):914-6. doi: 10.1007/s11999-009-1183-1. PMID: 19967474; PMCID: PMC2816766. Pubmed
- Patiño JM, Saenz VP. Radial Head Fractures. [Updated 2023 Jun 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Al-Tawil K, Arya A. Radial head fractures. J Clin Orthop Trauma. 2021 Jul 8;20:101497. doi: 10.1016/j.jcot.2021.101497. PMID: 34307018; PMCID: PMC8283329. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Campbel’s Operative Orthopaedics 12th edition Book.