Odontoid fractures constitute 8–18% of all cervical fractures, with neurological deficits occurring in 10–20% of cases. High-velocity trauma such as motor vehicle accidents account for most odontoid fractures in young adults, whereas low-velocity injuries, such as falls, account for the injuries in the elderly (osteoporotic fractures) and children.
The mechanism of injury includes avulsion of the apex of the dens by the alar ligament or lateral/oblique forces that cause fracture through the body and base of the dens. Posteriorly displaced fractures are the result of hyperextension whereas anteriorly displaced fractures are due to a hyperflexion force.
The vascular supply of the C2 vertebra is from the apex, via a periapical plexus that is supplied by a branch of the basilar artery, and from the base, via the vertebral artery with a watershed area in the neck of the odontoid. This watershed area of poor vascularity, lack of periosteum and cancellous bone results in high non-union rates of type II odontoid fractures.
See Also: Occipital Condyle Fractures
Odontoid Fracture Diagnosis
Symptoms can be minimal, but severe pain behind the ears and neck stiffness are frequent. Patients often report a feeling of instability at the base of the skull and present holding their head with both hands.
Odontoid fractures are one of the most commonly missed spinal fractures; hence, radiographs should be critically evaluated for odontoid fractures. Subtle signs such as retropharyngeal swelling may alert the physician to the presence of a fracture.
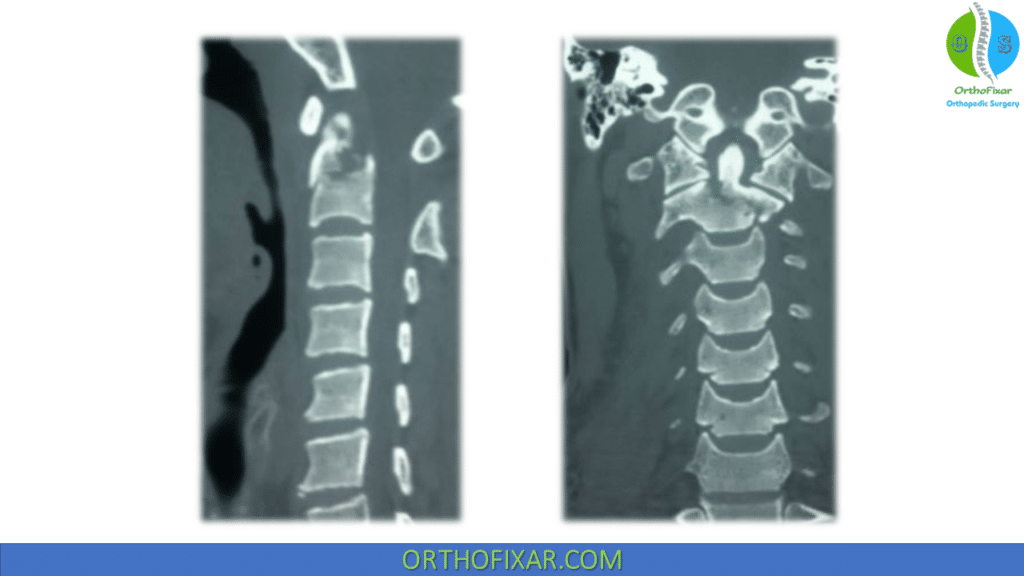
Fine-section CT with sagittal and coronal reformations should be considered if the open-mouth view is obscured, if a high index of suspicion for a fracture exists clinically or on radiographs, or if the patient has altered mental status. A CT should also be obtained to fully characterize the fracture morphology to assist in management decision-making.
See Also: Occipitocervical Dissociation
Odontoid Fracture Classification
Odontoid fractures have been classified by Anderson and D’Alonzo into three types, with Hadley adding a fourth type – type IIA.
| Type I (5%) | Oblique avulsion fracture of the apex | Represents an avulsion of the alar and apical ligaments, Rule out atlanto-occipital dislocation |
| Type II (60%) | Fracture at the junction of the dens with the body of C2 | High non-union rate Rule out associated transverse atlantal ligament injury |
| Type IIA (Hadley) | Comminuted injury extending from the waist of the dens into the body of the axis | Highly unstable |
| Type III (30%) | Fracture extending into the cancellous portion of the body of C2 and possibly involving one or both of the superior articular facets | High likelihood of union owing to the cancellous bed of the fracture site |

Odontoid Fracture Treatment
Type I fractures can be immobilized in an external orthosis for 6–8 weeks once the possibility of an associated occipitocervical dissociation has been excluded.
Type III fractures have been reported to have a sufficiently high healing rate with rigid external immobilization in a halo vest.
Treatment of type II fractures is controversial and depends largely on specific patient and fracture characteristics. Treatment options include halo vest immobilization, anterior odontoid screw stabilization or a posterior C1–2 fusion.

While undisplaced or minimally displaced fractures that are easily reduced may be treated with halo vest immobilization for 6–12 weeks, non-union rates ranging from 10% to 77% have been reported for displaced fractures.
A number of risk factors associated with an increased incidence of non-union for type II odontoid fractures have been identified. These include:
- Initial fracture displacement of >4 mm,
- >10 degrees angulation,
- Posterior displacement,
- Fracture comminution,
- Elderly patients,
- Delayed treatment
- Smoking
- Inability to achieve or maintain a reduction.
Early surgical treatment is an option for patients with any of these risk factors. Elderly patients tolerate halo vest immobilization poorly, demonstrate decreased healing rates and should be considered for early surgical management.
Anterior fixation is indicated for most type II and shallow type III fractures in patients older than 7 years. The procedure is contraindicated in fractures with:
- Oblique pattern,
- Disruption of the atlantal transverse ligament,
- Non-unions,
- Pathological fractures
- Osteoporosis.
- Patients with a short neck, a rigid neck or cervical kyphosis and thoracic kyphosis/barrel chest are not suitable for this procedure as there is a technical difficulty associated with passage of the screw. Posterior C1–2 fusion is then indicated.
Studies comparing one- versus two-screw techniques show that there is no difference between the two in terms of load to failure and hence a single anterior screw is adequate.
References & More
- Mercer’s Textbook of Orthopaedics and Trauma, Tenth edition.
- Tenny S, Munakomi S, Varacallo M. Odontoid Fractures. [Updated 2023 Aug 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441956/
- Deluca A, Wichlas F, Deininger C, Traweger A, Mueller EJ. Reevaluation of a classification system: stable and unstable odontoid fractures in geriatric patients-a radiological outcome measurement. Eur J Trauma Emerg Surg. 2022 Aug;48(4):2967-2976. PubMed