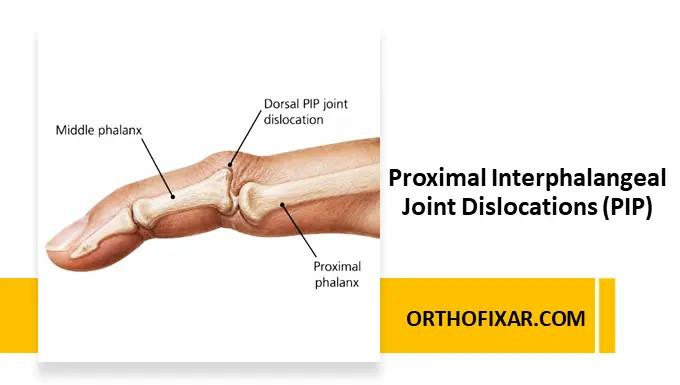
A proximal interphalangeal joint dislocation occurs when the middle joint of a finger is forced out of its normal anatomical alignment. This joint lies between the proximal phalanx and the middle phalanx and plays a crucial role in grip and fine motor function.
PIP dislocations are among the most common finger injuries, particularly in ball-handling sports such as basketball, volleyball, and handball.
See Also: Hand Anatomy
Why PIP Dislocations Are Often Missed
A key clinical concern is that PIP dislocations are frequently misdiagnosed as simple “sprains.”
This leads to delayed treatment and increases the risk of chronic stiffness, deformity, or functional impairment.
According to evidence from peer-reviewed orthopedic literature (including PubMed-indexed studies):
- Many injuries are incomplete ligament disruptions, making them harder to detect.
- Up to 50% of cases involve the long (middle) finger, followed by the ring finger.
- Subtle joint incongruence on lateral X-ray may be the only sign of persistent instability.
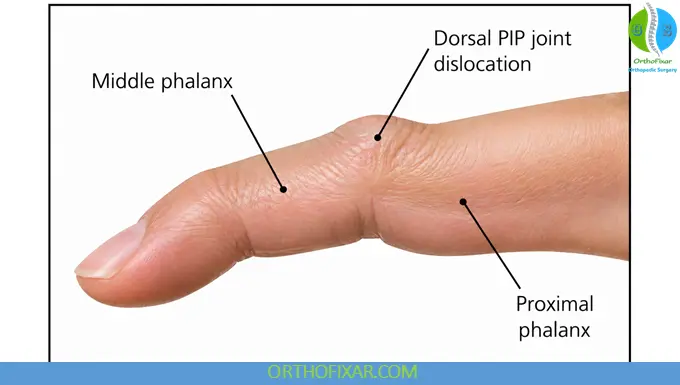
Types of PIP Joint Dislocations
Understanding the injury pattern is critical for proper management.
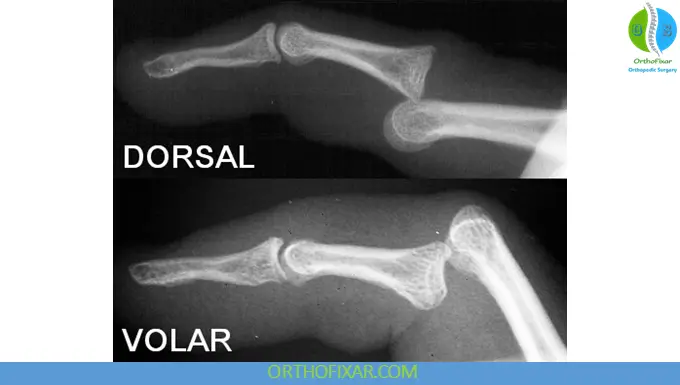
1. Dorsal PIP Dislocation (Most Common)
- The middle phalanx is displaced backward (dorsally)
- Typically involves volar plate injury (often distal avulsion ± small bone fragment)
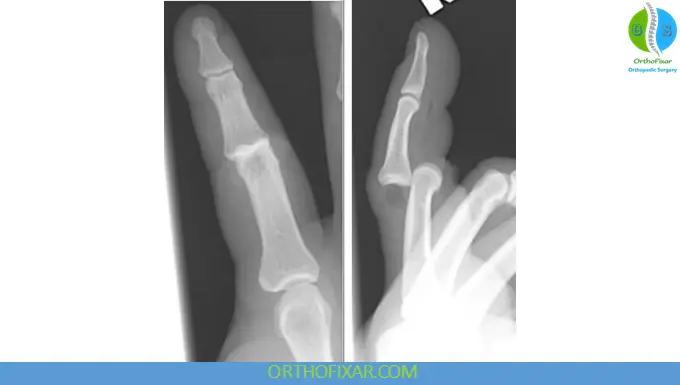
2. Volar PIP Dislocation (Rare but Serious)
- Displacement toward the palm
- Associated with:
- Central slip injury
- At least one collateral ligament rupture
- Volar plate may remain intact
3. Rotatory Volar PIP Dislocation
- Complex injury involving rotational deformity
- Often unstable and may require careful reduction
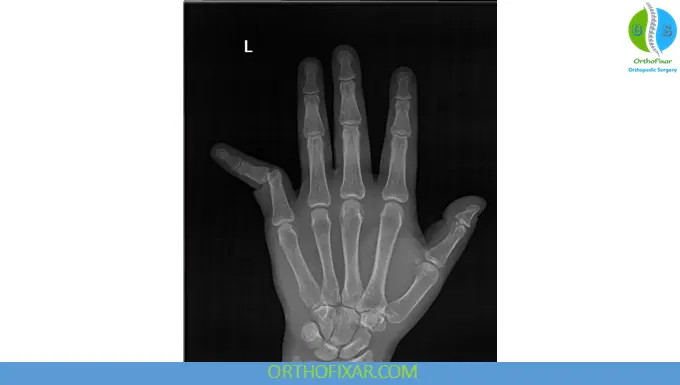
4. Lateral PIP Dislocation
- Caused by collateral ligament disruption
- May lead to joint instability if untreated
Irreducible PIP Dislocations
Some dislocations cannot be reduced closed due to soft tissue interposition:
- The head of the proximal phalanx may become trapped between:
- Central slip
- Lateral bands
This creates a “noose effect”, preventing reduction and requiring surgical (open) reduction.
Key Diagnostic Principle
👉 Joint congruence on lateral radiograph is critical
- Even subtle subluxation indicates instability
- Missed incongruence can lead to:
- Chronic deformity
- Poor functional outcome
Complications
1. Stiffness (Most Common)
- Occurs in nearly all injury patterns if not managed properly
- Primary concern in pure dislocations
2. Instability
- Rare in pure dislocations
- Common in fracture-dislocations
3. Chronic Dislocation
- Requires open surgical reduction
- Almost always results in residual stiffness
Treatment of PIP Joint Dislocations
Management depends on the type and stability of the injury.
✅ 1. Stable Injuries (After Reduction)
Includes:
- Rotatory volar dislocations
- Isolated collateral ligament injuries
- Dorsal dislocations stable in full extension
Treatment:
- Immediate active range of motion (ROM)
- Buddy taping (strapping to adjacent finger)
⚠️ 2. Dorsal Dislocations with Subluxation
- Seen on extension lateral X-ray
Treatment:
- Extension block splinting for several weeks
- Prevents hyperextension while allowing flexion
⚠️ 3. Volar Dislocations with Central Slip Injury
Treatment protocol:
- PIP joint extension splinting: 4–6 weeks
- Followed by:
- Night splinting for 2 additional weeks
- Important:
- DIP joint must remain free
- Encourage active DIP flexion to prevent stiffness
🔴 4. Open Dorsal Dislocations
- Often present with a transverse wound at the flexion crease
Management:
- Urgent wound debridement
- Then joint reduction
- Infection prevention is critical
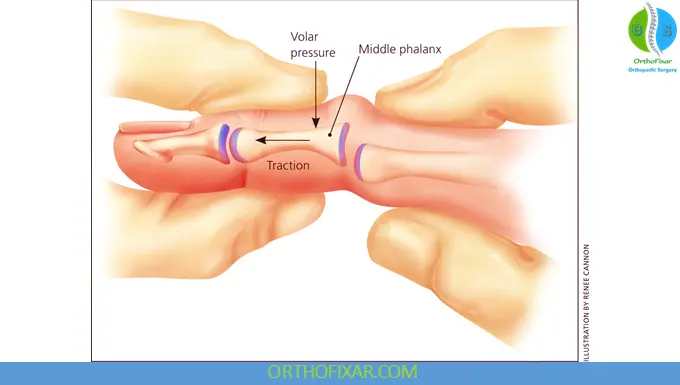
Rehabilitation
Early motion is essential to avoid long-term disability after proximal interphalangeal joint dislocation:
- Begin movement as early as stability allows
- Avoid prolonged immobilization
- Hand therapy may be required in complex cases
Key Takeaways
- PIP dislocations are common but frequently underestimated
- Missed diagnosis = long-term stiffness
- Radiographic alignment is critical
- Treatment depends on injury pattern and stability
- Early motion is the cornerstone of recovery
References & More
- Freiberg A. Management of proximal interphalangeal joint injuries. Can J Plast Surg. 2007 Winter;15(4):199-203. doi: 10.1177/229255030701500407. PMID: 19554177; PMCID: PMC2696003. Pubmed
- Elfar J, Mann T. Fracture-dislocations of the proximal interphalangeal joint. J Am Acad Orthop Surg. 2013 Feb;21(2):88-98. doi: 10.5435/JAAOS-21-02-88. PMID: 23378372; PMCID: PMC5823287. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.