Acetabulum Fractures generally are caused by high energy trauma, and associated injuries are frequent. These fractures demand greater attention and expertise due to their complex anatomy, potential long-term consequences, and the impact they can have on a patient’s quality of life.
Related Anatomy
The acetabulum, a key structure in the hip joint, consists of an incomplete hemispherical socket surrounded by an inverted horseshoe-shaped articular surface.
The supporting structures of the acetabulum can be illustrated by Letournel’s column concept. He described it as being held by an inverted Y made up of the anterior and posterior columns of bone.
Acetabulum is supported by two bone columns:
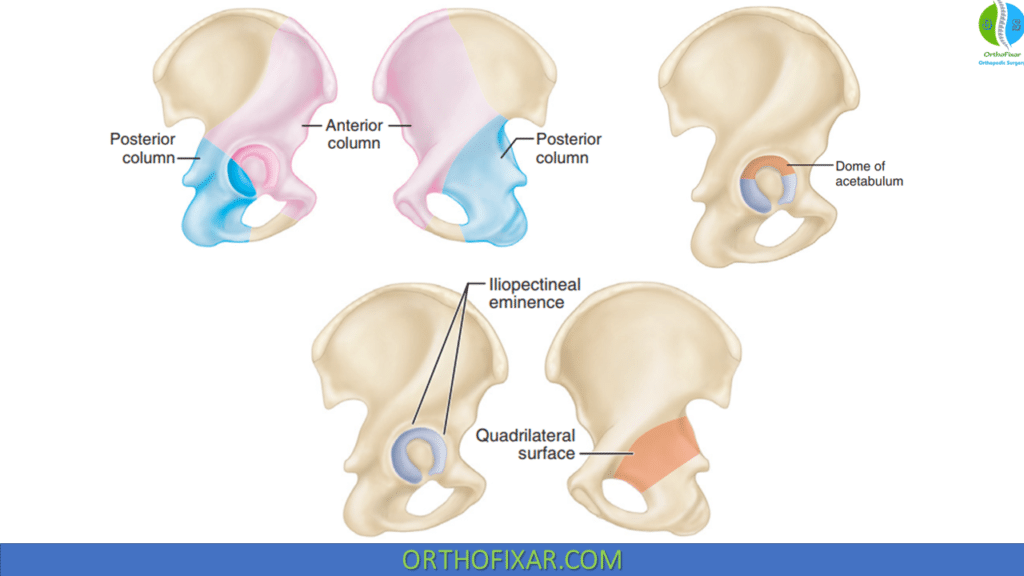
- The anterior column, which includes the iliac crest, spines, anterior acetabulum, and pubis.
- The posterior column, which includes the ischium, ischial spine, posterior acetabulum, and sciatic notch.
The dome, or roof, of the acetabulum is the weightbearing portion of the articular surface that supports the femoral head. Anatomical restoration of the dome with concentric reduction of the femoral head beneath this dome is the goal of both operative and nonoperative treatment.
The quadrilateral surface is the flat plate of bone forming the lateral border of the true pelvic cavity and thus lying adjacent to the medial wall of the acetabulum. The iliopectineal eminence is the prominence in the anterior column that lies directly over the femoral head. Both the quadrilateral surface and the iliopectineal eminence are thin and adjacent to the femoral head, limiting the types of fixation that can be used in these regions.
See Also: Hip joint Anatomy
See Also: Hip Muscles Anatomy
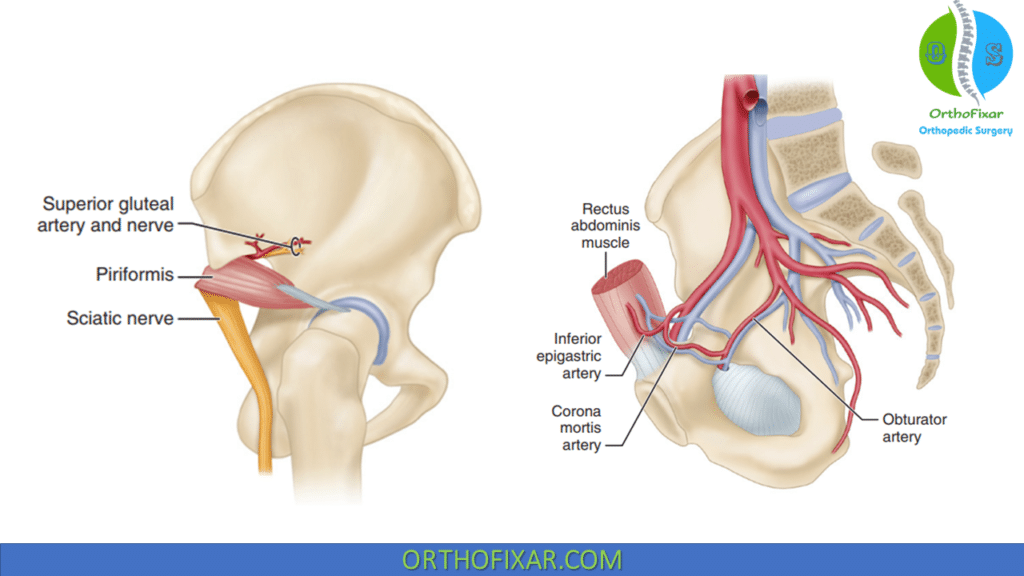
The sciatic nerve exiting the greater sciatic notch inferior to the piriformis muscle frequently is injured with posterior fracture-dislocations of the hip and fractures with posterior displacement. The sciatic nerve has frequent variation in its relationship to the piriformis muscle as it exits the sciatic notch, with common separation of tibial and peroneal branches at this level.
The superior gluteal artery and nerve exit the greater sciatic notch at its most superior aspect and can be tethered to the bone at this level by variable fascial attachments. Fractures that enter the superior portion of the greater sciatic notch can be associated with significant hemorrhage, possibly requiring angiography with embolization of the superior gluteal artery.
See Also: Pelvic Anatomy
Mechanisms of Injury
Acetabulum fractures are commonly caused by the impact of the femoral head on the acetabular articular surface. This force can be exerted through the greater trochanter, along the axis of the femoral neck, or along the long axis of the femoral shaft.
The resulting acetabulum fracture pattern depends on the hip’s position at the time of impact and the location and direction of the force applied:
- When the force is applied along the axis of the femoral neck, external hip rotation leads to an anterior fracture type,
- While internal rotation results in a posterior fracture.

Generally, a force applied along the femur’s axis, when the hip is flexed, drives the femoral head against the posterior articular surface of the acetabulum. However, the femoral head may dislocate without causing a fracture when adduction is added.
Regardless of hip position or the force’s location, the extent of fracture displacement, comminution (fragmentation), and articular impaction are influenced by the force magnitude and the strength of the underlying bone.
Even with relatively low-energy injuries, individuals with osteopenic bone often sustain severely comminuted fractures with articular impaction. In older osteopenic patients, a simple fall on the greater trochanter can lead to an acetabulum fracture. Therefore, it’s not surprising that anterior column and/or wall fractures, resulting from a fall on the greater trochanter, are the most common types of fractures in the elderly. These low-energy injuries typically cause isolated fractures, whereas high-energy injuries are often associated with additional skeletal or systemic trauma.
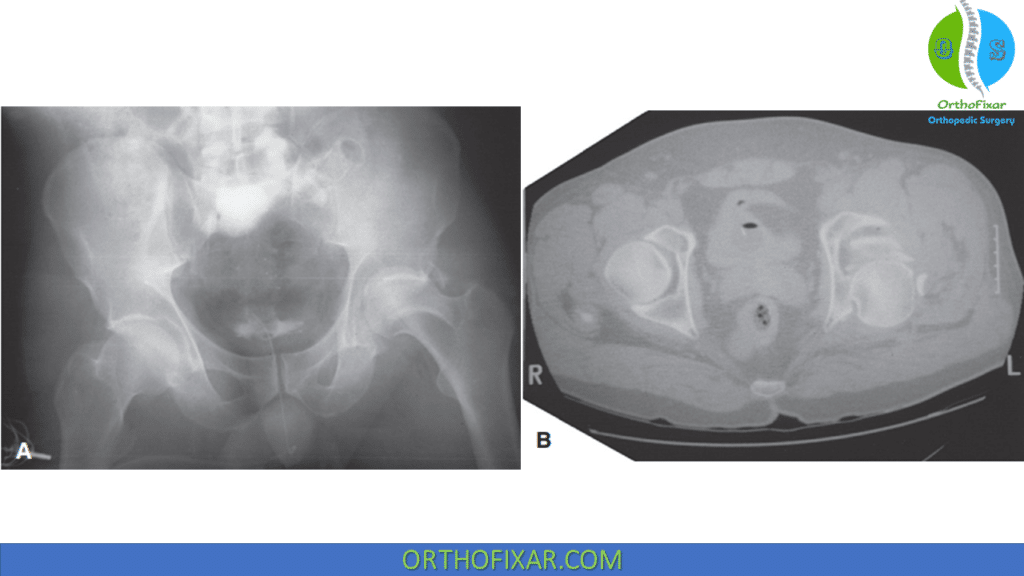
Associated Injuries with Acetabulum Fractures
Acetabulum fractures are often accompanied by other injuries affecting the musculoskeletal system and internal organs. Studies have shown that over 50% of patients with acetabulum fractures experience associated injuries. These injuries can vary widely and may involve the extremities, head, chest, nerves, abdomen, genitourinary system, or spine. Among the associated injuries, lower extremity fractures are the most common. It is crucial for orthopedic doctors to be aware of these associated injuries, as they can be life-threatening or limb-threatening.
The Advanced Trauma Life Support (ATLS) evaluation sequence should be followed to prioritize the treatment of life-threatening conditions. It is important to note that even apparently isolated fractures of the acetabulum can require blood replacement in a significant number of cases.
Signs and Symptoms
Physical examination of any patient who has sustained a high-energy injury should follow standard ATLS protocol. In general, a complete examination of the musculoskeletal system is required, especially evaluation of the peripheral nerves.
Patient history, such as the mechanism of injury (e.g., motor vehicle accident, fall from a height), can provide clues about the fracture type and associated musculoskeletal injuries. It is important to evaluate the knee as well, as it can be the first indication of an injury (e.g., patellar fractures, chondral injuries, ligamentous injuries).
In cases of lower-energy trauma, such as sports-related injuries or simple falls, a complete evaluation of the hip joint is necessary. Physical examination following standard protocol is crucial, including evaluation of the musculoskeletal system and peripheral nerves.
Injuries involving the posterior hip dislocation and fracture displacement of the posterior wall or column often result in sciatic nerve injury, which can present as sensory deficits, weakness, or loss of movement in specific muscles. Sciatic nerve injury is often incomplete, most often involving the peroneal division.
A patient who presents with a flexed, adducted, and internally rotated hip often will have either a relatively small posterior wall fracture fragment or a pure posterior dislocation. Absence of this abnormal limb positioning does not preclude the presence of a posterior wall fracture and, in fact, may be associated with a large posterior wall fracture fragment.
Imaging Study
Radiographic Imaging
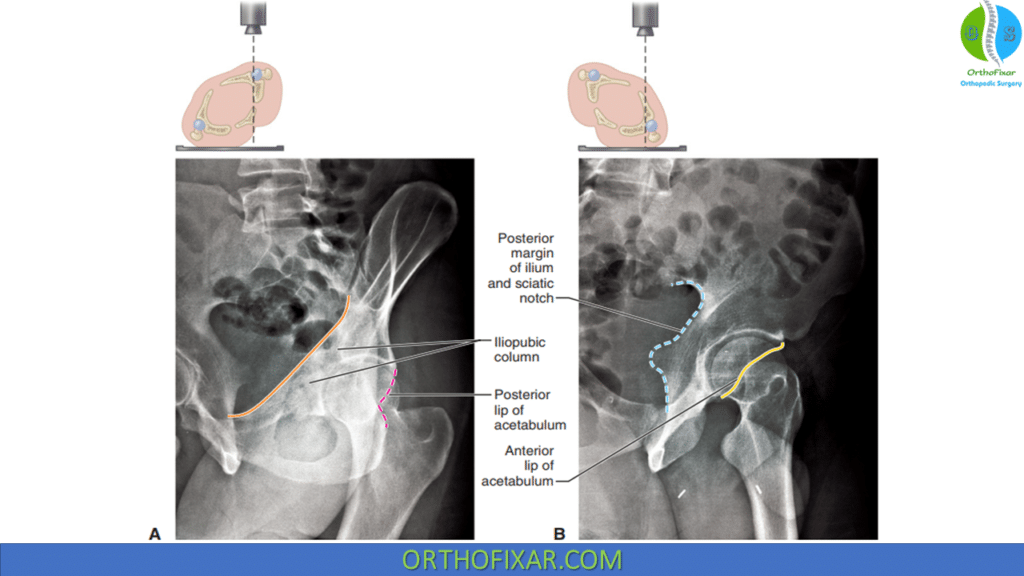
Recommended views include anteroposterior pelvic view as well as with the 45-degree oblique
views of the pelvis (Judet views). In the iliac oblique view, the radiographic beam is roughly perpendicular to the iliac wing. In the obturator oblique view, the radiographic beam is roughly perpendicular to the obturator foramen.
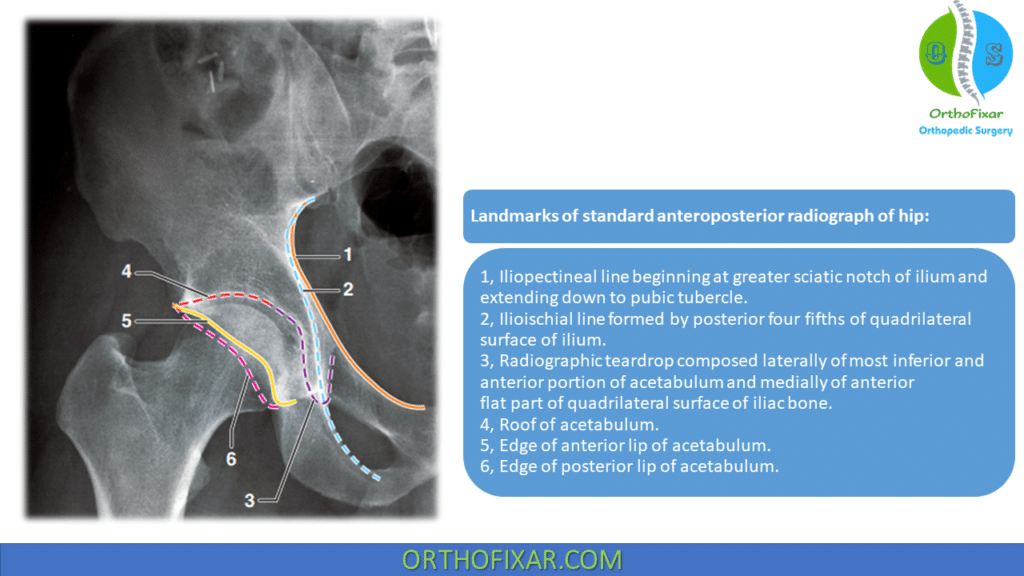
The medial clear space between the femoral head and the radiographic teardrop in the injured and uninjured hips should be compared on the anteroposterior view as an indication of femoral head subluxation.
Fractures that traverse the anterior column disrupt the iliopectineal line, whereas fractures that traverse the posterior column disrupt the ilioischial line.
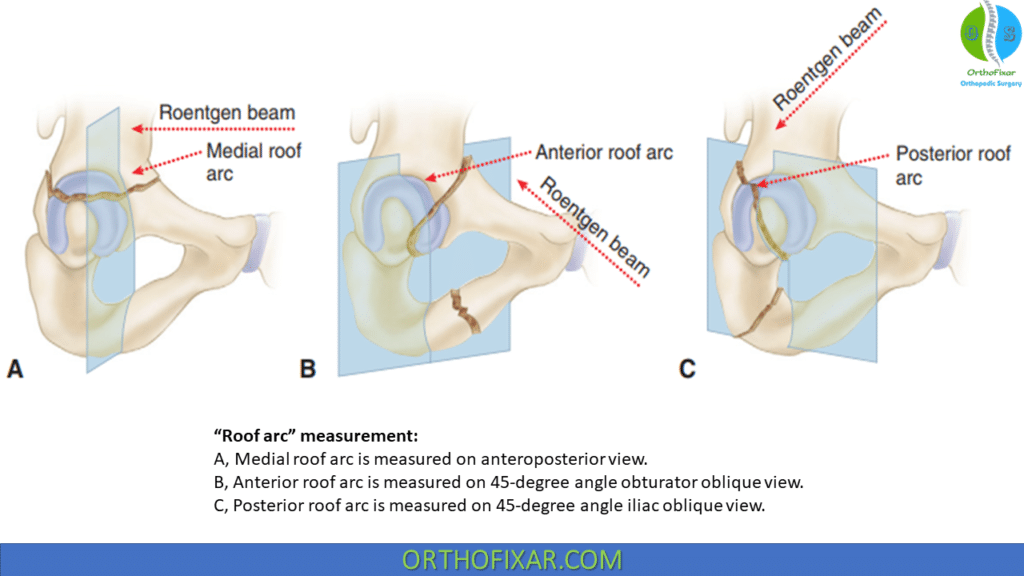
Roof arc measurements
Roof arc measurements involve determination of how much of the roof remains intact on each of the three standard radiographic views: anteroposterior, obturator oblique, and iliac oblique. The medial roof arc is measured on the anteroposterior view by drawing a vertical line through the roof of the acetabulum to its geometric center. A second line is then drawn through the point where the fracture line intersects the roof of the acetabulum and again to the geometric center of the acetabulum. The angle thus formed represents the medial roof arc. The anterior and posterior roof arcs are similarly determined on the obturator oblique and iliac oblique views, respectively.
Roof arc measurements are useful in the assessment of fractures of the posterior or anterior column, transverse fractures, T-type fractures, and associated anterior column and posterior hemitransverse fractures; they have limited usefulness for evaluation of both-column fractures and fractures involving the posterior wall. If any of the roof arc measurements in a displaced fracture are less than 45 degrees, operative treatment should be considered.
CT Imaging
CT is invaluable in the treatment of acetabulum fractures. Axial cuts should be taken with thin (3-mm) intervals and corresponding slice thicknesses.
the transverse fracture lines and fractures of the anterior and posterior walls are in the sagittal plane, paralleling the quadrilateral surface when they are viewed on axial CT images. Anterior and posterior column fractures usually extend through the quadrilateral surface and into the obturator foramen with a more coronal orientation; variant fracture types, however, may not follow these generalities.
High-resolution coronal and sagittal reconstructions of the fracture are helpful in the preoperative evaluation of complex fractures by delineating fractures that lie directly in the plane of a given axial CT image.
CT scans can give the same information about the acetabular dome as the roof arc measurements on the anteroposterior and oblique radiographs. Axial CT scans showing the superior 10 mm of the acetabular roof to be intact have been shown to correspond to radiographic roof arc measurements of 45 degrees.
Three-dimensional CT reconstructions of a fracture have become sophisticated and can be projected in many different views with subtraction of the femoral head that show unique features of the various fracture patterns.
Acetabulum Fracture Classification
The classification of acetabular fractures described by Letournel and Judet is the commonly used classification system.
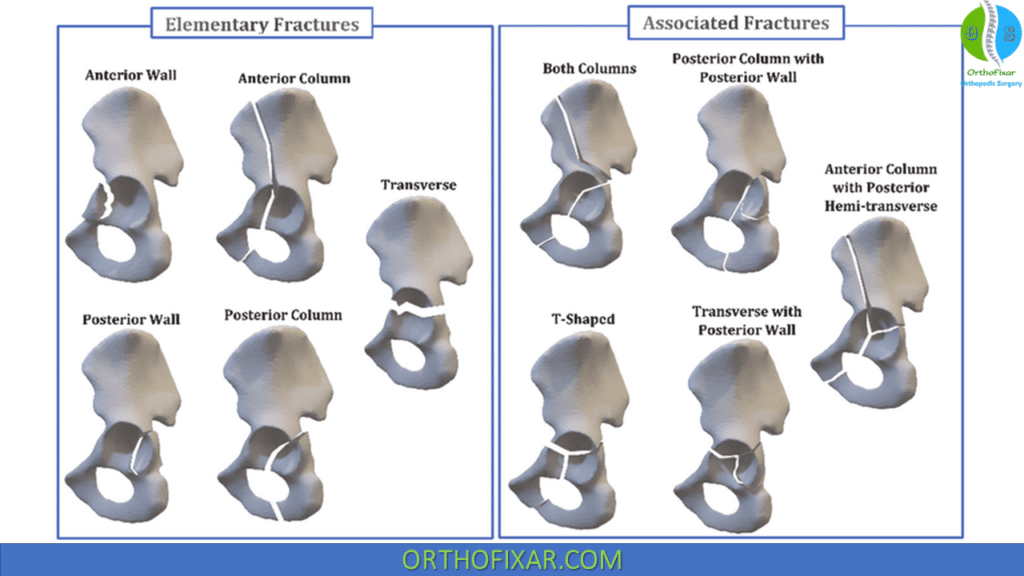
Elementary Fracture Patterns:
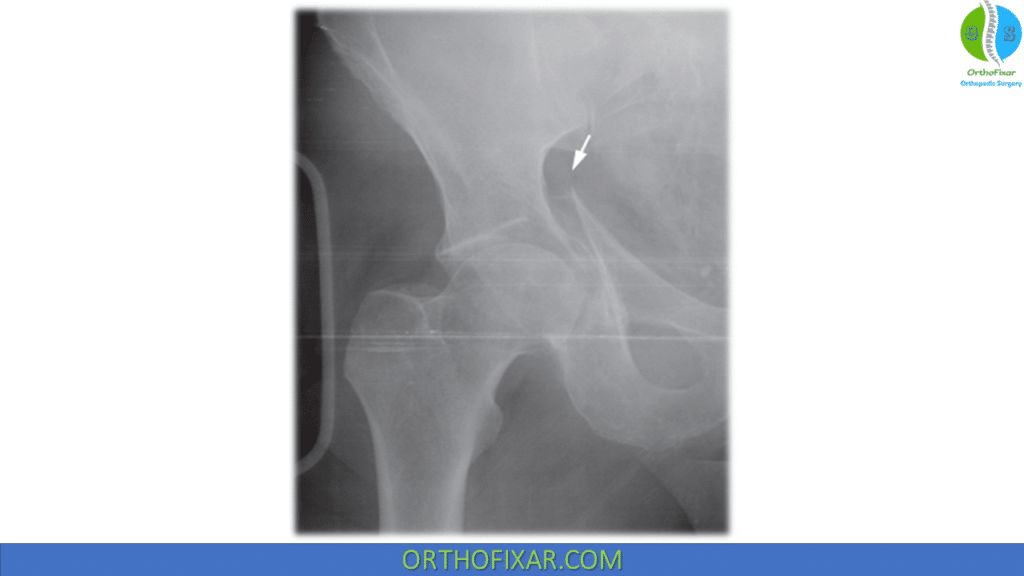
| Posterior wall | • Most common • “gull sign” on obturator oblique view |
| Posterior column | • check for injury to superior gluteal NV bundle |
| Anterior wall | • Very rare |
| Anterior column | • More common in elderly patients with fall from standing (most common in elderly is “anterior column + medial wall”) |
| Transverse | • Axial CT shows anterior to posterior fracture line • Only elementary fracture to involve both columns |
Associated Fracture Patterns:
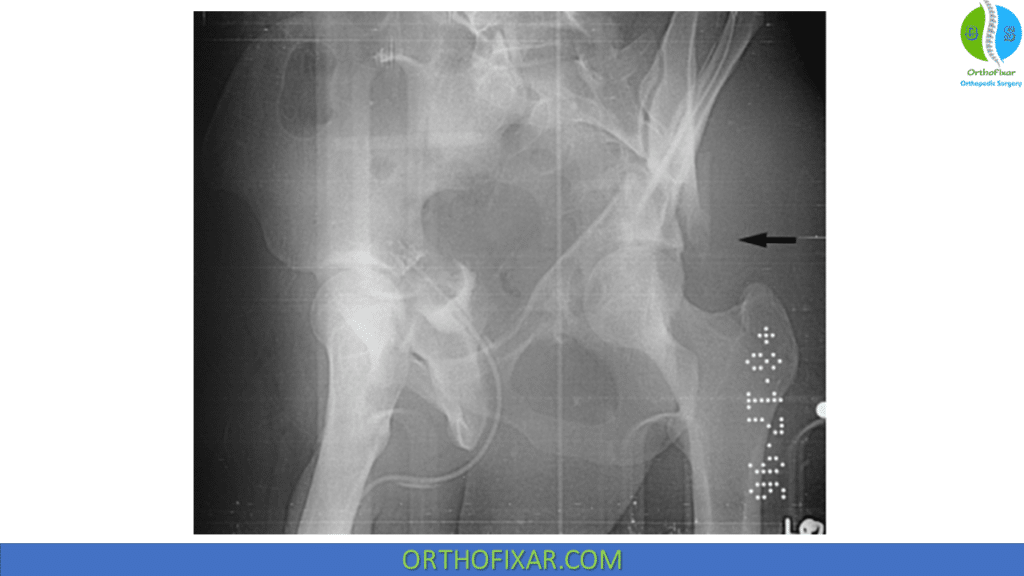
| Associated Both Column | • Characterized by dissociation of the articular surface from the inonimate bone • will see “spur sign” on obturator oblique |
| Transverse + Posterior Wall | • Most common associated fracture |
| T Shaped | • May need combined approach |
| Anterior column or wall + Posterior hemitransverse | • Common in elderly patients |
| Post. column + Posterior wall | • Only associated fracture that does not involve both columns |
Acetabulum Fracture Treatment
It is now evident that fractures involving even minor residual misalignments in the crucial part of the acetabulum are more likely to result in long-term arthritis compared to similar fractures with better anatomical realignments.
Indications for non-operative treatment
Nonoperative acetabular fracture treatment can be considered for certain cases in the management of acetabular fractures. These indications include:
- Non displaced acetabular fracture treatment with non-weight bearing for a period of 6 to 12 weeks, with regular radiographic monitoring to ensure that no further displacement occurs.
- Fractures with significant displacement but involving a non-critical joint region: Fractures that exhibit significant displacement but are not in a critical joint region may be treated nonoperatively. However, displaced fractures through the weight-bearing dome should still be treated with surgical fixation.
- Secondary congruence in displaced both-column fractures: In certain cases of both-column fractures, where the articular fragments can assume a position of secondary congruence around the femoral head, closed treatment may yield satisfactory results.
- Medical contraindications to surgery: Patients with multiple trauma or medical conditions that make surgery difficult or risky may be managed nonoperatively. Skeletal traction can be used to protect the hip joint during delays in operative intervention.
- Local soft tissue problems: Open wounds in the surgical field, systemic infections, and soft tissue lesions from blunt trauma are contraindications to surgery. In some cases, fractures can be approached from different angles to avoid the affected area.
- Elderly patients with osteoporotic bone: In elderly patients with osteoporosis, open reduction may not be feasible or may have poor outcomes. Alternative options include mobilization without fixation, percutaneous fixation with mobilization, or primary total hip arthroplasty.
Indications for nonoperative treatment may vary depending on the specific fracture and patient factors. The decision to pursue nonoperative treatment should be made in consultation with a healthcare professional, considering the individual circumstances and risks involved.
Indications for operative treatment
The following are the main indications acetabulum fracture surgery treatment:
- Fracture Characteristics: Operative treatment is indicated for acetabular fractures with 2 mm or more of displacement in the dome of the acetabulum, as determined by roof arc measurements of less than 45 degrees. Additionally, any subluxation of the femoral head resulting from a displaced acetabular fracture seen on radiographic views warrants surgical intervention. Posterior wall fractures with more than 50% involvement of the articular surface or clinical instability with hip flexion to 90 degrees also require operative treatment. Posterior wall fractures involving less than 50% of the wall may be unstable and are assessed clinically and with stress testing under anesthesia.
- Incarcerated Fragments in the Acetabulum after Closed Reduction of a Hip Dislocation: Small avulsed fragments of the ligamentum teres that remain sequestered in the cotyloid fossa and do not affect hip congruency do not need excision. However, fragments located between the articular surfaces of the femoral head and the acetabulum, as confirmed by CT imaging, should be excised.
- Prevention of Nonunion and Retention of Sufficient Bone Stock for Later Reconstructive Surgery: This indication is considered outdated and should be applied only in cases of extreme deformity. Total hip arthroplasty after failed operative fixation of an acetabular fracture can be more challenging than hip arthroplasty after nonoperative management due to scarring, hardware, and heterotopic bone. Percutaneous fixation may be used in older patients with comminuted fractures to prevent gross displacement and facilitate mobilization. Conversion to total hip arthroplasty can be considered if needed after fracture healing. Primary total hip arthroplasty has been advocated in older patients with fractures having a poor prognosis, provided adequate stabilization of the acetabular shell can be achieved.
In summary, operative treatment for acetabular fractures is indicated for specific fracture characteristics, incarcerated fragments affecting hip congruency, and in certain cases to prevent nonunion and preserve bone stock for later reconstructive surgery.
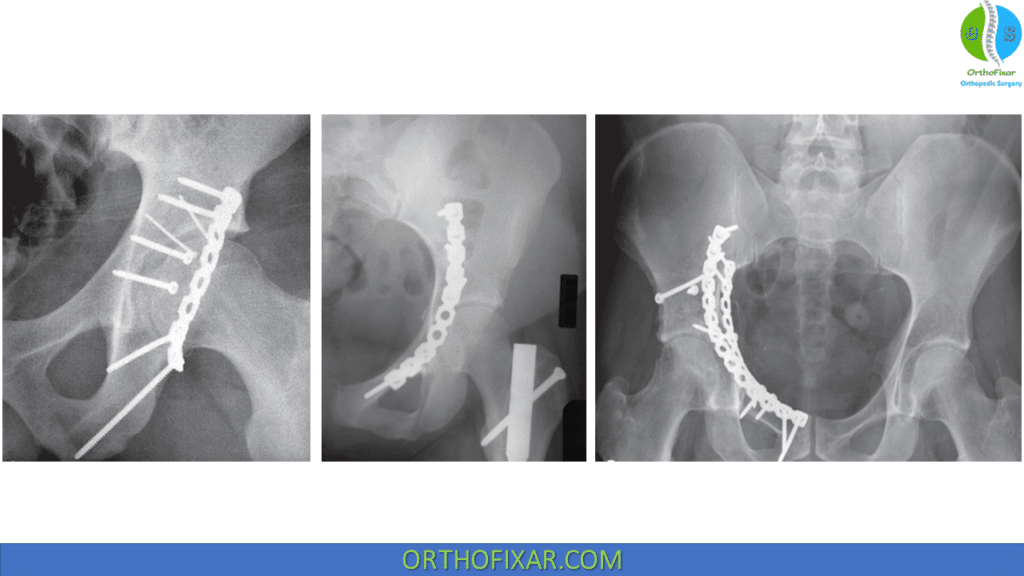
Acetabular fractures that are associated with certain complications, such as irreducible hip dislocation, open fracture, vascular compromise, or worsening neurologic deficit, require immediate surgical intervention. However, in most cases, acetabular fracture surgery should be performed after the patient’s medical condition has been optimized, and the surgeon has thoroughly examined the fracture and conducted adequate preoperative planning. It is also important to assemble an experienced surgical team.
Ideally, open reduction and internal fixation (ORIF) of acetabular fractures should be performed within 5 to 7 days of the injury. Beyond this timeframe, achieving anatomical reduction becomes more challenging due to factors such as hematoma organization, soft tissue contracture, and early callus formation. These factors can hinder the process of fracture reduction, particularly if more limited exposures are used during surgery.
References
- Hoge S, Chauvin BJ. Acetabular Fractures. [Updated 2022 Mar 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK544315/
- Letournel E. Acetabulum fractures: classification and management. Clin Orthop Relat Res. 1980 Sep;(151):81-106. PMID: 7418327.
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Rockwood and Green’s Fractures in Adults 8th Edition book.