A full understanding of pelvic anatomy is required to treat pelvic fractures, to prevent iatrogenic injuries, and to provide the best results.
Learning Pelvic Anatomy is composed of learning bones, muscles, ligaments, nerves and vascular supply.
Osteology
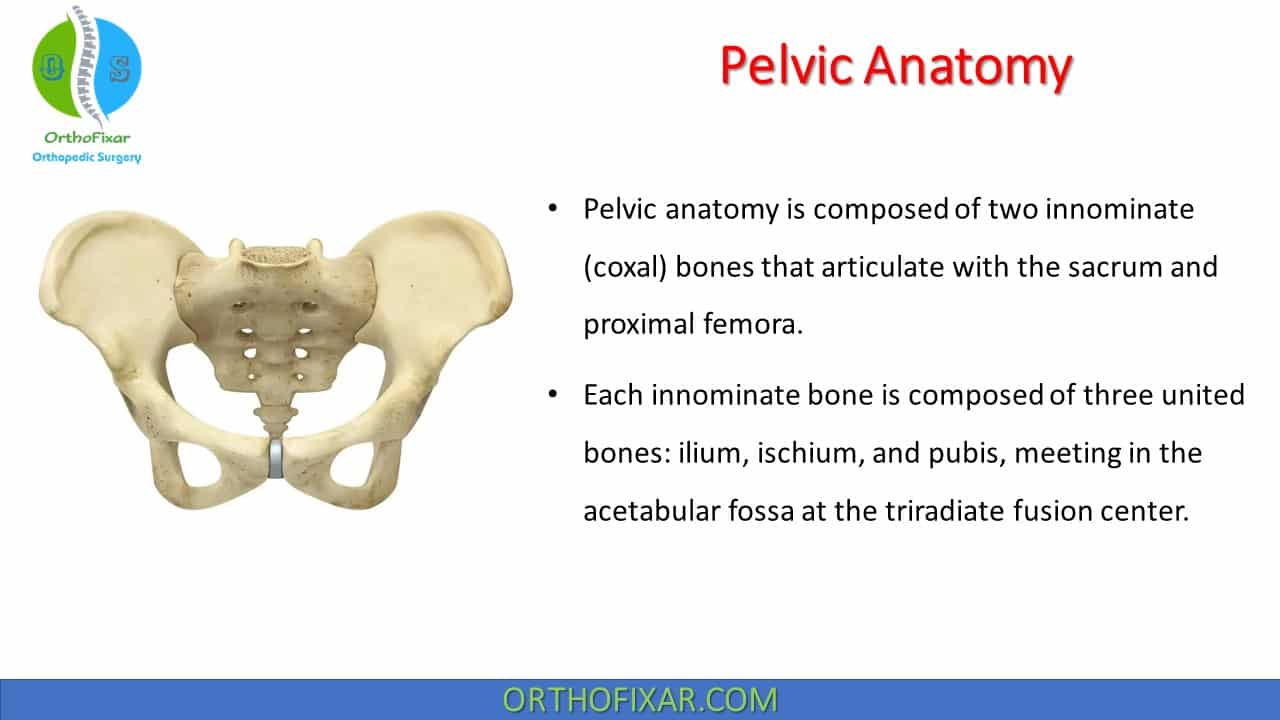
Pelvic anatomy is composed of two innominate (coxal) bones that articulate with the sacrum and proximal femora.
Each innominate bone is composed of three united bones: ilium, ischium, and pubis, meeting in the acetabular fossa at the triradiate fusion center.
See Also: Pelvic Fractures

Ilium Bone:
The ilium is the largest of these three bones. It is composed of a large fan-like wing (ala) and an inferiorly positioned body. The body of the ilium forms the superior two-fifths of the acetabulum.
The wing of the ilium spans superiorly from the posterior superior iliac spine (PSIS) to the anterior superior iliac spine
(ASIS). The wing serves as the insertion for the gluteus minimus, medius, and maximus.
The anterior surface of the ilium forms a fossa and serves as the proximal attachment of the iliacus muscle.
Important landmarks include:
- iliac crest,
- anterior-superior iliac spine (ASIS),
- anterior-inferior iliac spine (AIIS),
- posterior-superior iliac spine (PSIS)
Iliac crest: under-skin palpable rim of ilium, it’s an important site for bone graft harvest (iliac tubercle 5 cm posterior to ASIS).
ASIS: palpable at lateral edge of inguinal ligament; origin of sartorius muscle and transverse and internal abdominal muscles.
AIIS: less prominent; origin of direct head of the rectus femoris and iliofemoral ligament (Y ligament of Bigelow)
PSIS: 4 to 5 cm lateral to S2 spinous process; important landmark for posterior iliac crest bone graft harvest.
See Also: Anterior Approach to the Iliac Crest
The bone in the ilium has two columns, which are extremely thick and strong:
- The first column runs from the ischial tuberosity to the SI joint and allows for force transfer during sitting.
- The second column runs from the dome of the acetabulum to the SI joint and allows for force transfer during standing.

Ischium Bone:
The ischium is composed of a body, which contributes to the acetabulum, and a ramus. The ischium
forms the posterior two-fifths of the acetabulum.
Together, the ischium and the ramus form the ischial tuberosity.
Ischial tuberosity: origin of hamstrings; sacrotuberous ligament (posterolateral sacrum to ischial tuberosity) inferior border of lesser sciatic foramen.
The ischial spine, located on the body of the ischium, serves as the attachment for the sacrospinous ligament
Iliac spine separates greater and lesser sciatic notch; while sacrospinous ligament (anterior sacrum to ischial spine) separates greater and lesser sciatic foramina.
Greater sciatic notch: located posterior and superior to acetabulum.
Muscles that Attach to the Ischial Tuberosity incloude:
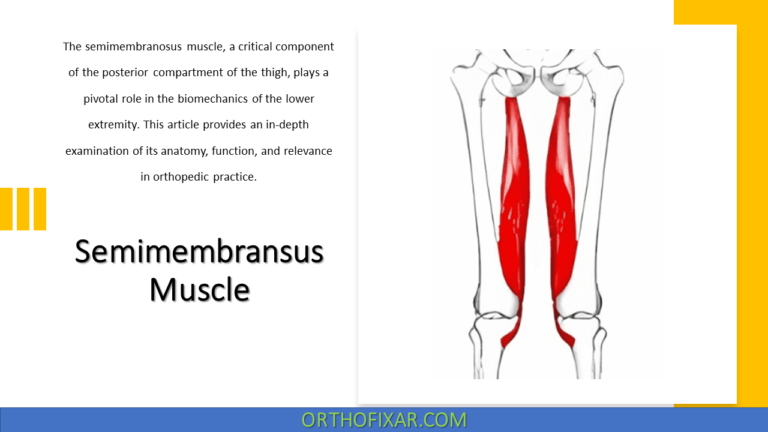
- Semimembranosus
- Semitendinosus
- Long head of the biceps femoris
- Adductor magnus
- Quadratus femoris
- Gemellus inferior
Pubis Bone:
The pubis bone is the smallest of the three bones and consists of a body and inferior and superior rami, it forms the anterior fifth of the acetabulum.
Pubis bone forms the anterior pelvic ring.
Bilateral pubic rami articulate at pubic symphysis anteriorly.
Iliopectineal eminence: anterior pelvic rim prominence at the union of the ilium and pubis.
Acetabulum
The ilium, ischium, and pubis fuse together within the acetabulum and form a deep-seated depression in the lateral
pelvis, which allows for the proximal transmission of weight from the axial skeleton to the lower extremity.
The surface of the acetabulum faces laterally, inferiorly, and anteriorly.
The superior and posterior margins of the acetabulum are reinforced with a compact cortical bone, which extends the peripheral brim of the fossa, enhancing the stability of the joint during weight-bearing from both flexed and extended positions.
While the majority of acetabular development is determined by the age of eight, the depth of the acetabulum increases additionally at puberty, because of the development of three secondary centers of ossification.
Around the periphery of the acetabulum is a thickened collar of fibrocartilage known as the acetabular rim, or labrum that further deepens the concavity and grasps the head of the femur.
The articular surface of the acetabulum is limited to an inverted horseshoe-shaped area covering the anterior, superior, and posterior margins. This relatively small contact area, may contribute to the prevalence of hip degenerative joint disease in humans.
The articular surface is covered by a thickened layer of hyaline cartilage, which thins near the center of the joint, and is absent over the acetabular notch, the area occupied by the ligamentum teres and obturator artery.
The diameter of the acetabulum is slightly less than that of the femoral head and results in an incongruous fit of the joint surfaces. This incongruity unloads the joint during partial weight-bearing (PWB), by allowing the femoral head to sublux laterally out of the cup, while in full weight-bearing, the femoral head is forced into the acetabulum.
In addition, elastic deformation of the acetabulum increases joint congruency of the two-joint surfaces in weight-bearing. Finally, a strong vacuum contributes to the joint coaptation.
The position of maximum articular congruence corresponds to a quadriped position: 90 degrees flexed, slightly abducted, and externally rotated.
The transverse acetabular ligament is a fibrous tissue link spanning the inferior acetabular notch that connects the anteroinferior and posteroinferior horns of the semilunar surface of the acetabulum. The posterior aspect of the ligament attaches to the bone beneath the lunate surface, and the anterior aspect attaches to the labrum. The transverse acetabular ligament contains no cartilage cells. The function of this ligament in the hip is currently unknown.
See Also: Sacral Fractures

Pelvic Ligaments
The three bony structures (ilium, ischium, and pubis) are held together with strong ligaments that are important in understanding pelvic anatomy and biomechanics.
Pelvic floor consists of two ligaments:
- Sacrospinous ligaments: resist external rotation forces.
- Sacrotuberous ligaments: resist shear and flexion forces.
The SI joints are held together with anterior, intra-articular, and posterior sacroiliac ligaments.
Posterior sacroiliac complex
Posterior sacroiliac complex is the strongest ligaments in the body, it consists of 4 ligaments:
- Anterior sacroiliac ligaments: resist external rotation.
- Interosseous sacroiliac ligament: resist anterior-posterior translation of pelvis.
- posterior sacroiliac ligament: resist cephalad-caudad displacement of pelvis.
- Iliolumbar ligament: resist rotation and augment posterior SI ligaments.
The posterior ring structures are responsible for the majority of pelvic ring stability.
The symphyseal ligaments, which hold the pubis together, resist external rotation and account for only 15% of the stability to the entire ring.

Biomechanics of the Pelvis
The forces on the pelvic ring vary according to load, principally, either single-leg or bilateral-leg stance.
- When a person stands on both legs, both the symphysis and inferior SI joints are under tension, whereas the superior aspect of the SI joint is under compression.
- During a single-leg stance, the symphysis actually undergoes compression while the SI joint forces flip, with compression inferiorly and tension superiorly.
Neurovascular Structures
The internal iliac vessels and its major trunks pass anterior to the SI joints and then exit the pelvis through the greater and lesser sciatic notches and the obturator foramen. The superior gluteal vessels exit the greater sciatic notch.
- The L5 nerve root lies on the anterior aspect of the sacral ala and is at risk with pelvic ring fractures or during surgical intervention. The sacral nerve roots exit from each of the five sacral foramina. These coalesce to form part of the lumbosacral and all of the sacral plexus, which innervate the perineal structures and lower extremities.
- The primary named peripheral nerves that exit the pelvis via the greater sciatic notch are the sciatic nerve, the superior and inferior gluteal nerves, and the internal pudendal nerve. The obturator nerve exits the pelvis via the obturator foramen.
A full understanding of pelvic anatomy is required to treat pelvic fractures, to prevent iatrogenic injuries, and to provide the best results.

References
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Millers Review of Orthopaedics -7th Edition Book.
- Rockwood and Green’s Fractures in Adults 8th Edition book.
- Chaudhry SR, Nahian A, Chaudhry K. Anatomy, Abdomen and Pelvis, Pelvic Anatomy. [Updated 2021 Aug 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482258/