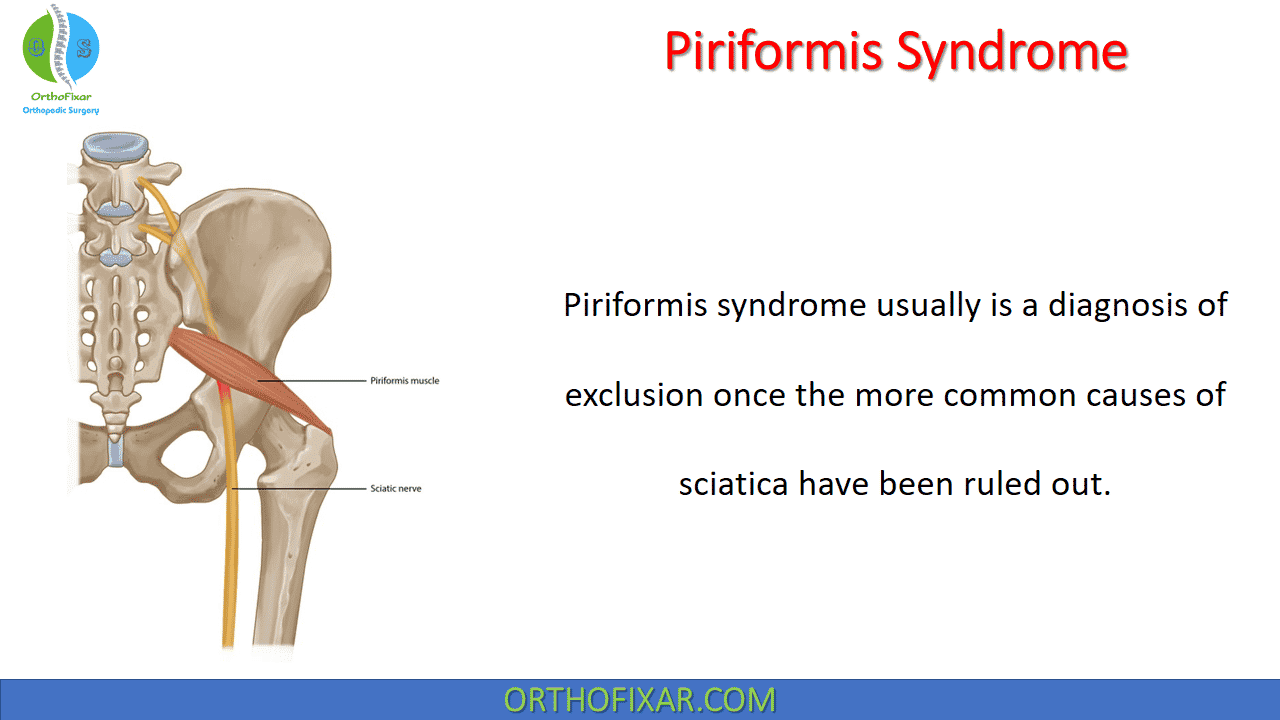
Piriformis syndrome usually is a diagnosis of exclusion once the more common causes of sciatica have been ruled out. It may also be described as a sensation in which the hamstring muscles feel “tight” or are “about to tear”.
Piriformis syndrome is more common in women than in men.
See Also: Hip Muscles Anatomy
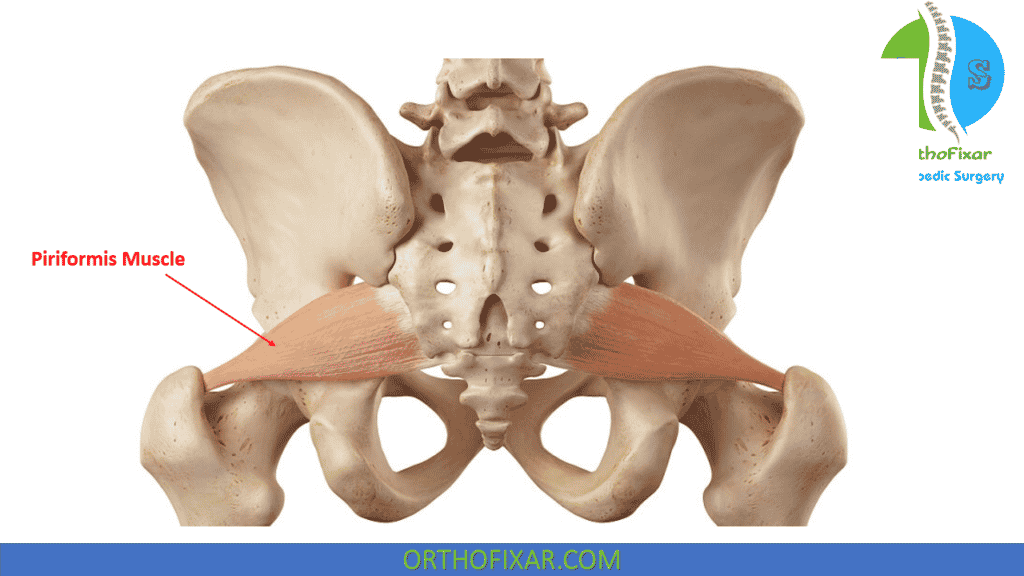
Piriformis Syndrome Causes
Multiple Causes have been proposed to explain the compression or irritation of the sciatic nerve that occurs with the piriformis syndrome:
- Hypertrophy of the piriformis muscle.
- Overuse of the piriformis muscle: Although there is disagreement, overuse seems to be the most common cause of piriformis syndrome. This suggests that patients must be effectively cautioned about returning too quickly to the type of activity that bought about the piriformis syndrome once recovered.
- Trauma: Trauma, direct or indirect, to the sacroiliac or gluteal region can lead to piriformis syndrome and is a result of hematoma formation and subsequent scarring between the sciatic nerve and the short external rotators.
- Hip flexion contracture: A flexion contracture at the hip has been associated with piriformis syndrome. This flexion contracture increases the lumbar lordosis, which increases the tension in the pelvic–femoral muscles, as these muscles try to stabilize the pelvis and spine in the new position. This increased tension causes the involved muscles to hypertrophy with no corresponding increase in the size of the bony foramina, resulting in neurological signs of sciatic compression.
- Gender: Females are more commonly affected by piriformis syndrome, with as much as a 6:1 female-to-male incidence.
- Ischial bursitis.
- Pseudoaneurysm of the inferior gluteal artery.
- Excessive exercise to the hamstring muscles.
- Inflammation and piriformis spasm: This is often in association with trauma, infection, and anatomical variations of the muscle.
- Anatomical anomalies: In 1938, anomalies of the piriformis muscle, with a subsequent alteration in the relationship between the piriformis muscle and the sciatic nerve, were implicated in sciatica. Local anatomical anomalies may contribute to the likelihood that symptoms will develop. Patients with this condition report radicular pain that is much like the nerve-root pain associated with lumbar disk disease with movement of the hip. These patients typically present with a history of gluteal trauma, symptoms of pain in the buttock and intolerance to sitting, tenderness to palpation of the greater sciatic notch, and pain with flexion, adduction, and internal rotation of the hip.
See Also: Piriformis Muscle Anatomy
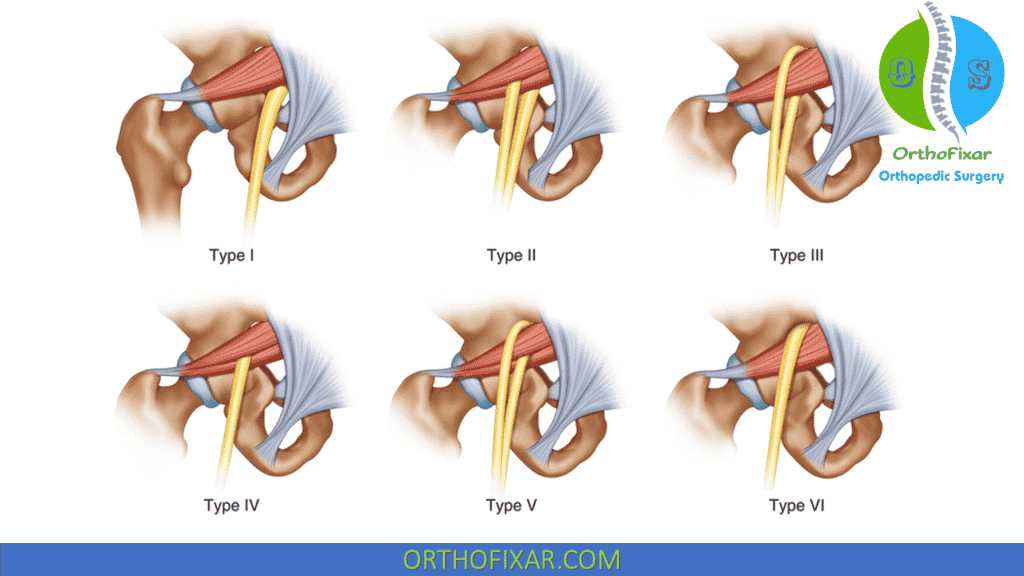
The sciatic nerve usually travels below the piriformis. In approximately 15% of the population, however, either the tibial part of the sciatic nerve passes through the belly of the piriformis muscle or the piriformis has two muscle bellies and the nerve passes between the two bellies.
Spasm or hypertrophy of the piriformis places pressure on the sciatic nerve, mimicking the signs and symptoms of lumbar nerve root compression or sciatica in the buttock and posterior leg.
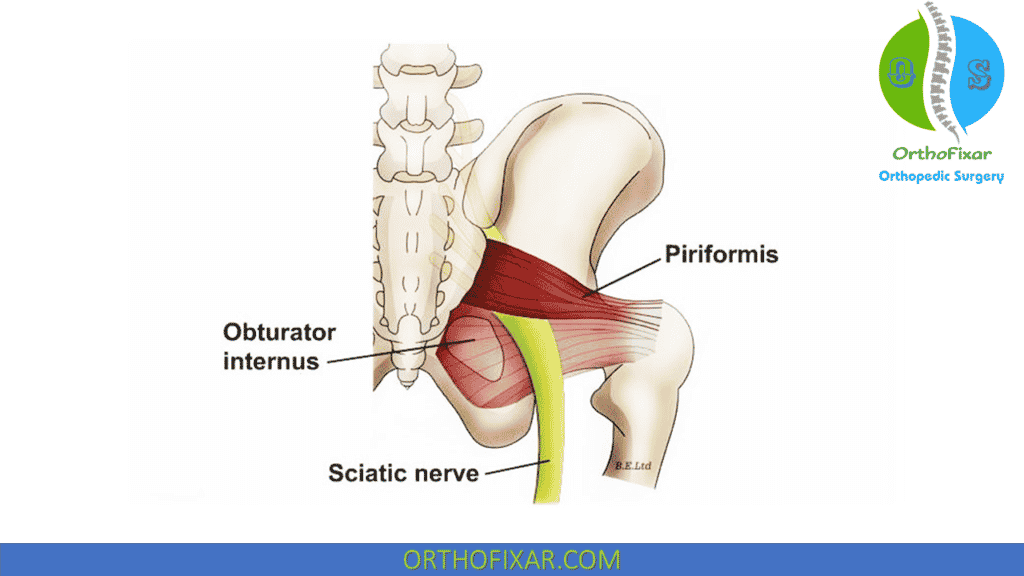
Piriformis Syndrome Symptoms
Robinson listed six cardinal features of piriformis syndrome:
- a history of trauma to the sacroiliac and gluteal regions;
- pain in the region of the sacroiliac joint, greater sciatic notch, and piriformis muscle, extending down the lower limb and causing difficulty in walking;
- acute exacerbation of the symptoms by lifting or stooping;
- a palpable, sausage-shaped mass over the piriformis muscle, during an exacerbation of symptoms, which is markedly tender to pressure (this feature is pathognomonic of the syndrome);
- a positive result on the SLR test;
- gluteal atrophy, depending on the duration of symptoms.
Improved diagnostic tests for lumbar nerve root impingement and intervertebral disk disease have decreased the frequency with which piriformis syndrome is diagnosed.
Although the signs and symptoms of piriformis syndrome are similar to those caused by other lumbopelvic conditions, piriformis syndrome remains relatively undefined and confusing. Complaints include burning, pain, numbness, or paresthesia that are increased with contraction of the piriformis or during palpation or prolonged sitting.
Symptoms may be heightened by the straight leg raise test on the involved side, passive hip internal rotation (Freiberg sign), and resisted external rotation with the patient seated. Resisted hip abduction with the patient seated may also increase the symptoms.
Local muscle spasm usually is palpable in the obturator internus or, less commonly, in the piriformis muscle. The neurologic examination is usually normal. An examination of the hip and lower leg usually demonstrates restricted internal rotation of the hip and lumbosacral muscle tightness.
These symptoms may also be caused by entrapment of the sciatic nerve by the hamstring muscles, termed hamstring syndrome.
See Also: Piriformis Syndrome Test
See Also: Lasegue Test

Imaging
Radiographs is Radiographs.
Lumbar MRI helpful to rule out spine as cause of compression of sciatic nerve.
Electrodiagnostic studies o can document functional impairment of sciatic nerve.
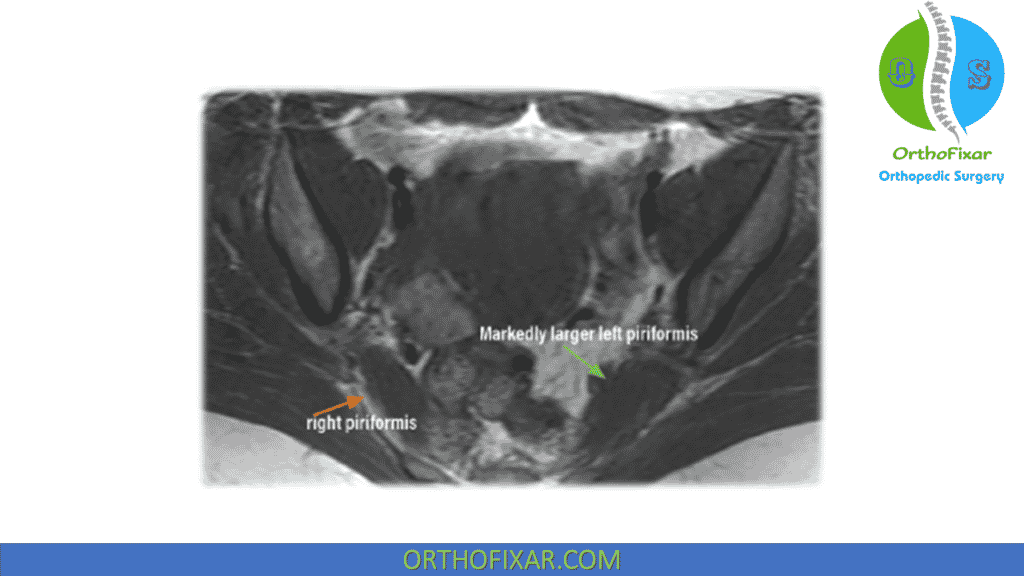
Piriformis Syndrome Treatment
The Piriformis Syndrome Treatment depends on the suspected pathology:
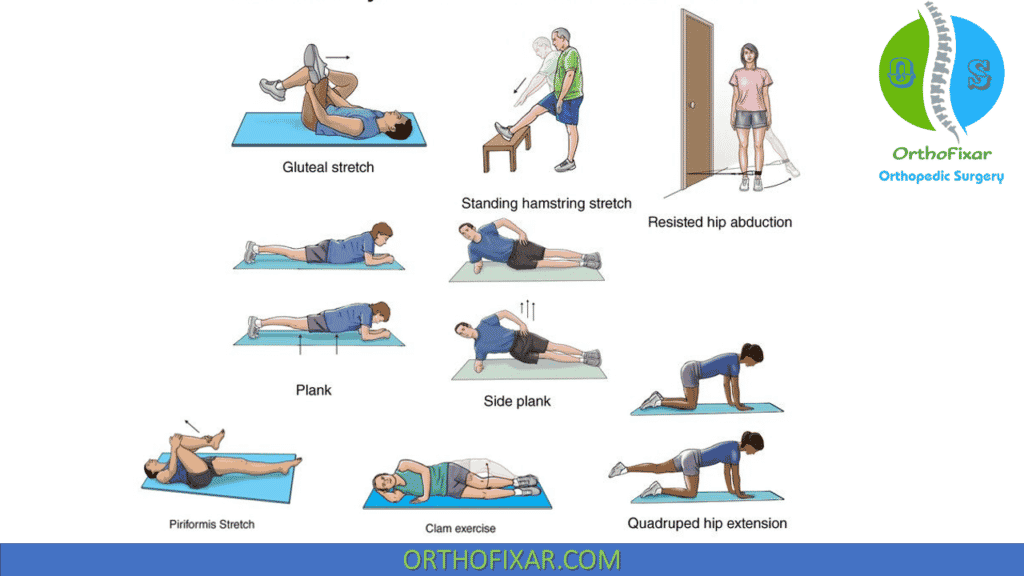
- If muscular spasm and tightness is the suspected etiology, then an aggressive piriformis muscle stretch and massage should be instituted.
- If this conservative approach fails, a local anesthetic block to the muscle should be considered.
- Botulinum neurotoxins have been successfully used in clinical practice to reduce the strength of idiopathic muscular spasm and muscle tightness caused by overuse, trauma, or occupation in the piriformis muscle. One study showed that this form of injection followed by physical therapy significantly shortens recovery time, thereby reducing both the patient’s pain and treatment time.
Surgical release of the piriformis muscle may be indicated in cases that do not respond to conservative care.
References
- Vandertop WP, Bosma NJ. The piriformis syndrome. A case report. J Bone Joint Surg Am. 1991 Aug;73(7):1095-7. PMID: 1874775.
- Robinson DR: Pyriformis syndrome in relation to sciatic pain. Am J Surg 73:355–358, 1947.
- McCrory P: The piriformis syndrome –myth or reality? Br J Sports Med 35:209–210, 2001.
- Beauchesne RP, Schutzer SF: Myositis ossificans of the piriformis muscle: an unusual cause of piriformis syndrome. A case report. J Bone Joint Surg Am 79:906–910, 1997.
- Jankiewicz JJ, Hennrikus WL, Houkom JA: The appearance of the piriformis muscle syndrome in computed tomography and magnetic resonance imaging. A case report and review of the literature. Clin Orthop 262:205–209, 1991.
- Palliyath S, Buday J: Sciatic nerve compression: diagnostic value of electromyography and computerized tomography. Electromyog Clin Neurophysiol 29:9–11, 1989.
- Fishman LM, Dombi GW, Michaelsen C, et al.: Piriformis syndrome: diagnosis, treatment, and outcome – a 10-year study. Arch Phys Med Rehabil 83:295–301., 2002.
- Papadopoulos SM, McGillicuddy JE, Albers JW: Unusual cause of piriformis muscle syndrome. Arch Neurol 47:1144–1146, 1990.
- Tesio L, Bassi L, Galardi G: Transient palsy of hip abductors after a fall on the buttocks. Arch Orthop and Trauma Surg 109:164–165, 1990.
- Pace JB, Nagle D: Piriformis syndrome. Western J Med 124:435–439, 1976.
- Pecina M: Contribution to the etiological explanation of the piriformis syndrome. Acta Anat Nippon 105:181–187, 1979.
- Boyd KT, Pierce NS, Batt ME: Common hip injuries in sport. Sports Med 24:273–288, 1997.
- Durrani Z, Winnie AP: Piriformis muscle syndrome: an underdiagnosed cause of sciatica. J Pain Symptom Manage 6:374–379, 1991.
- Solheim LF, Siewers P, Paus B: The piriformis muscle syndrome. Sciatic nerve entrapment treated with section of the piriformis muscle. Acta Orthop Scand 52:73–75, 1981.
- Steiner C, Staubs C, Ganon M, et al.: Piriformis syndrome: pathogenesis, diagnosis, and treatment. J Am Osteopath Assn 87:318–323, 1987.
- Julsrud ME: Piriformis syndrome. J Am Podiat Med Assn 79:128–131, 1989.
- Pfeifer T, Fitz WFK: Das Piriformis-Syndrom. Zeitschr Orthop 127:691– 694, 1989.
- Beaton LE, Anson BJ: The sciatic nerve and the piriformis muscle: their interrelation a possible cause of coccygodynia. J Bone Joint Surg 20:686– 688, 1938.
- Hughes SS, Goldstein MN, Hicks DG, et al.: Extrapelvic compression of the sciatic nerve. An unusual cause of pain about the hip: report of five cases. J Bone Joint Surg 74-A:1553–1559, 1992.
- Benson ER, Schutzer SF: Posttraumatic piriformis syndrome: diagnosis and results of operative treatment. J Bone Joint Surg 81A:941–949, 1999.
- Freiberg AH: Sciatic pain and its relief by operations on muscle and fascia. Arch Surg 34:337–350, 1937.
- Lang AM: Botulinum toxin type B in piriformis syndrome. Am J Phys Med Rehabil 83:198–202, 2004.
- Childers MK, Wilson DJ, Gnatz SM, et al.: Botulinum toxin type A use in piriformis muscle syndrome: a pilot study. Am J Phys Med Rehabil 81:751–759, 2002.
- Fishman LM, Konnoth C, Rozner B: Botulinum neurotoxin type B and physical therapy in the treatment of piriformis syndrome: a dose-finding study. Am J Phys Med Rehabil 83:42–50; quiz 51–53, 2004.