Piriformis Syndrome Test is used in the assessment of a contracture of the piriformis muscle or to detect compression of the sciatic nerve by the piriformis.
The piriformis Muscle is an external rotator of the hip at less than 60 degrees of hip flexion. At 90 degrees of hip flexion, the piriformis muscle reverses its muscle action, becoming an internal rotator and abductor of the hip.
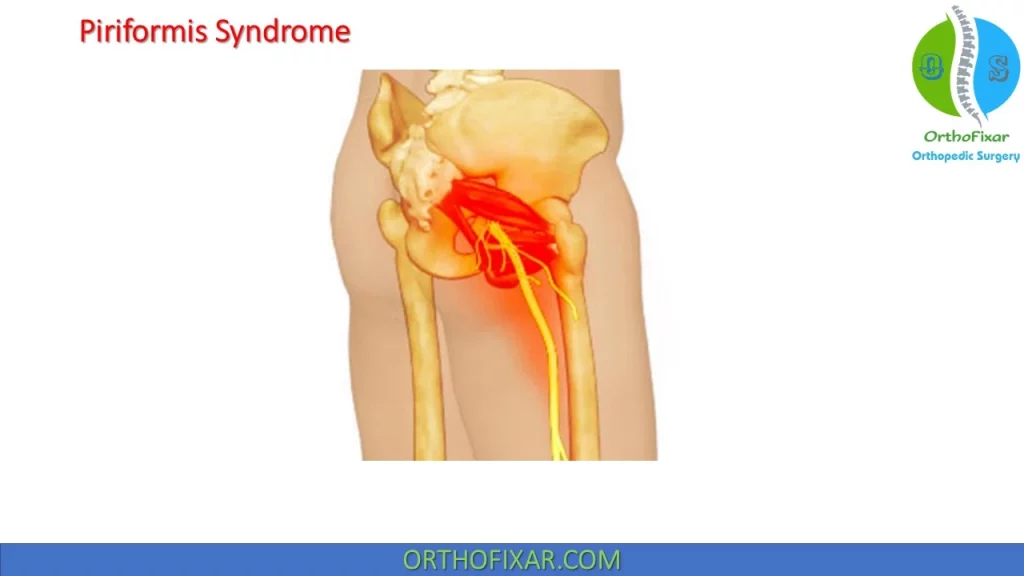
Piriformis syndrome is the result of entrapment of the sciatic nerve by the piriformis muscle, as it passes through the sciatic notch.
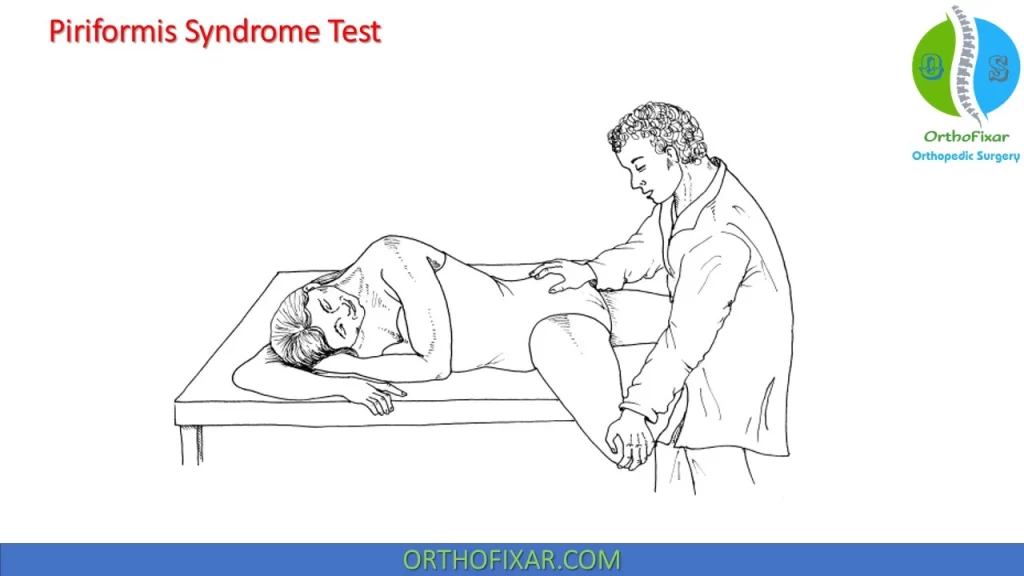
How do you perform the Piriformis Syndrome Test?
The patient lies in the lateral position with the test leg uppermost. The patient flexes the hip of that leg to 60° with the knee flexed. The examiner stabilizes the hip with one hand and applies downward pressure to the knee.
What does a positive Piriformis Syndrome Test mean?
If the piriform is tight, pain is elicited in the muscle. If the piriformis is pinching the sciatic nerve, pain results in the buttock and the patient may experience sciatica.
See Also: Piriformis Muscle Anatomy
See Also: Thomas Test of the Hip

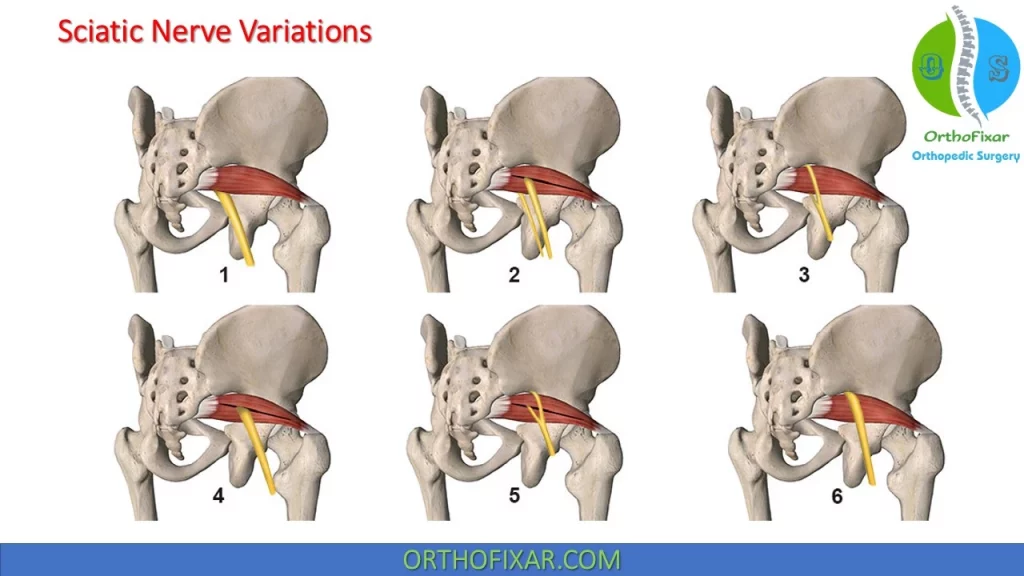
In around 80% of cases, the sciatic nerve travels below the piriformis muscle. While in 17% of people, the piriformis muscle is pierced by parts or all of the sciatic nerve.
References
- Fishman LM, Dombi GW, Michaelsen C, Ringel S, Rozbruch J, Rosner B, Weber C. Piriformis syndrome: diagnosis, treatment, and outcome–a 10-year study. Arch Phys Med Rehabil. 2002 Mar;83(3):295-301. doi: 10.1053/apmr.2002.30622. PMID: 11887107.
- Smolders JJ: Myofascial pain and dysfunction syndromes. In: Hammer WI, ed. Functional Soft Tissue Examination and Treatment by Manual Methods – The Extremities. Gaithersburg, MD: Aspen, 1991:215–234
- Roy S, Irvin R: Sports Medicine – Prevention, Evaluation, Management, and Rehabilitation. Englewood Cliffs, NJ: Prentice-Hall, 1983.
- Pecina M: Contribution to the etiological explanation of the piriformis syndrome. Acta Anat Nippon 105:181–187, 1979.
- Robinson DR: Pyriformis syndrome in relation to sciatic pain. Am J Surg 73:355–358, 1947.
- Solheim LF, Siewers P, Paus B: The piriformis muscle syndrome. Sciatic nerve entrapment treated with section of the piriformis muscle. Acta Orthop Scand 52:73–75, 1981.