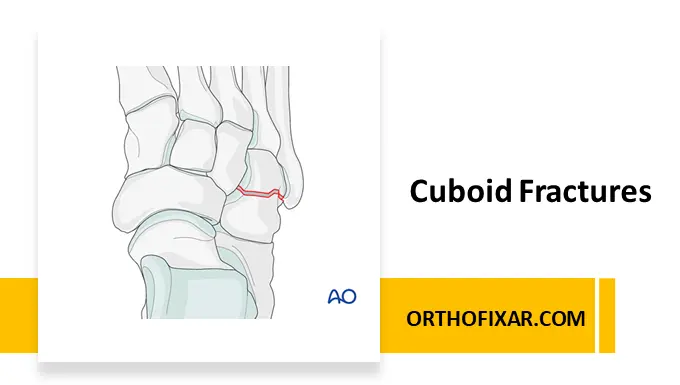
Cuboid fractures are relatively uncommon injuries of the lateral midfoot but can have significant functional consequences if missed or improperly managed. This guide provides an evidence-based overview of cuboid fractures, including epidemiology, anatomy, mechanism of injury, clinical evaluation, imaging, classification, treatment, and potential complications.
Epidemiology
Cuboid fractures may occur in isolation, but more commonly they are associated with injuries to the talonavicular joint, lateral column of the foot, or Lisfranc injuries. They are observed in both athletic populations and trauma patients. According to studies, these fractures account for a small fraction of foot injuries but can significantly impact gait and foot biomechanics if untreated.
Anatomy
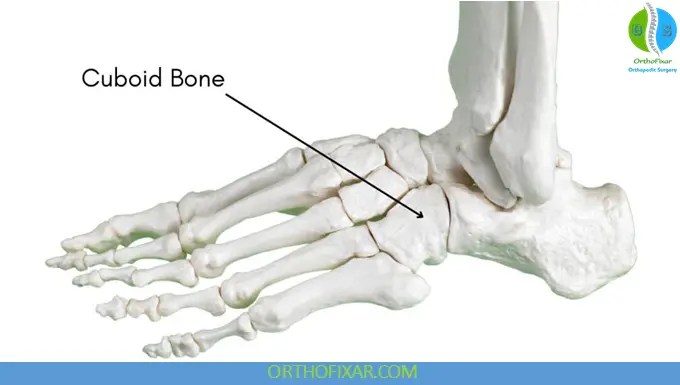
The cuboid bone is a key component of the lateral support column of the foot. Its articulations include:
- Proximal: Calcaneus
- Medial: Navicular and lateral cuneiform
- Distal: Fourth and fifth metatarsals
The cuboid’s plantar aspect forms part of the peroneal groove, which houses the peroneus longus tendon. Irregularity or scarring of this groove following fracture may impair tendon function and lateral foot stability.
See Also: Foot Anatomy
Mechanism of Injury
Cuboid fractures may occur via direct or indirect mechanisms:
Direct Trauma
- Rare
- Usually caused by trauma to the dorsolateral aspect of the foot
Indirect Trauma
- Accounts for most cuboid fractures
- “Nutcracker injury”: Forefoot abduction or torsional stress compresses the cuboid between the calcaneus and lateral metatarsals
- Extreme plantar flexion can lead to calcaneocuboid joint sprains or dislocations (common in high-velocity trauma, dance injuries, or patients with Ehlers-Danlos syndrome)
- Stress fractures: Common in athletes, especially runners or jumpers
See Also: Cuboid Syndrome
Clinical Evaluation
Patients with cuboid fractures often present with:
- Pain, swelling, and tenderness over the dorsolateral midfoot
- Pain on weight-bearing
- Confusion with peroneal tendonitis in stress fractures
A thorough palpation of all foot bones is essential to identify associated injuries.
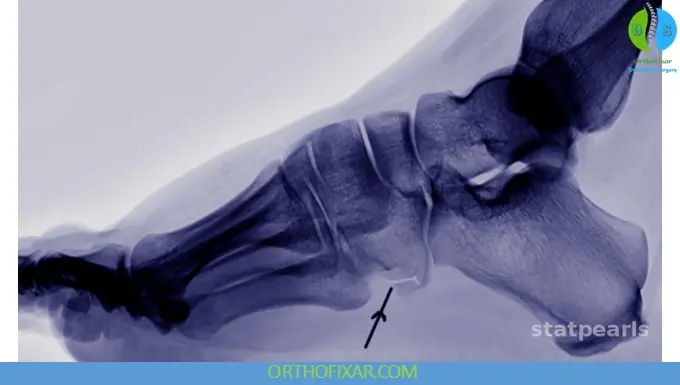
Radiographic Evaluation
- AP, lateral, and oblique foot X-rays are standard.
- Multiple medial oblique views may be required to visualize the calcaneocuboid and cuboid-metatarsal joints.
- Weight-bearing or stress views help detect interosseous instability.
- CT scans: Assess fracture extent and articular involvement.
- MRI or bone scans: Useful for detecting stress fractures.
- Medial or dorsal navicular avulsion fractures may indicate underlying cuboid injury.
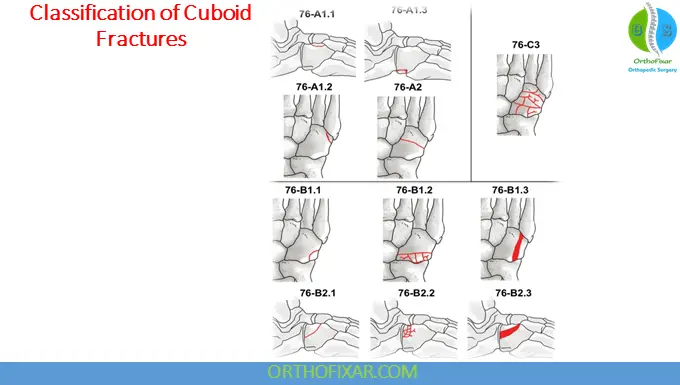
Classification of Cuboid Fractures
In clinical practice, cuboid fractures are most commonly classified according to the anatomic element involved. This often represents an arbitrary classification of a descriptive nature. Cuboid fractures can be described as stable or unstable, simple or comminuted, intraarticular or extraarticular, displaced or undisplaced or crush.
The Orthopedic Trauma Association has proposed a classification system dividing cuboid fractures into 3 main categories. According to this classification, cuboid fractures can be extraarticular (Group A), involving either of the calcaneocuboid or metatarsocuboid joint (Group B) or represent complex injuries involving both major joint surfaces (Group C).
This classification further subdivides these fractures according to their complexity, plane, and the part of the bone involved. Each group is denoted with numbers, and the higher the number, more significant is the nature of the injury. Group C fractures, in particular, represent significant crash injuries of the bone that involve the articular surfaces and can be either undisplaced (Type 1) or displaced (Type 2).
Treatment
Nonoperative Management
- Indicated for isolated fractures without osseous shortening or instability
- Immobilization in cast or removable boot
- Non–weight bearing: 4–6 weeks
Operative Management
- Open reduction and internal fixation (ORIF) is recommended if:
- Joint surface disruption >2 mm
- Evidence of longitudinal compression or displacement
- Calcaneocuboid arthrodesis: Considered in severe comminution or residual articular incongruity to restore lateral column stability
Complications
Potential complications include:
- Osteonecrosis: Especially in severely displaced fractures
- Posttraumatic osteoarthritis: Due to articular incongruity or osteochondral fragments
- Nonunion: Occurs with displacement and inadequate fixation; may require ORIF with bone grafting if symptomatic
Key Takeaways
- Cuboid fractures, though rare, are critical injuries affecting lateral foot stability.
- High suspicion is required in lateral midfoot pain, particularly in athletes and trauma patients.
- Proper imaging, accurate classification, and appropriate management are essential to prevent long-term complications such as chronic pain, deformity, or osteoarthritis.
References & More
- Lau H, Dreyer MA. Cuboid Stress Fractures. [Updated 2023 Aug 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542250/
- Pountos I, Panteli M, Giannoudis PV. Cuboid Injuries. Indian J Orthop. 2018 May-Jun;52(3):297-303. doi: 10.4103/ortho.IJOrtho_610_17. PMID: 29887632; PMCID: PMC5961267. NCBI
- Cotton C, Langston R, Fernicola J, Knight J, Bowman J. Management of a Displaced, Osteoporotic Cuboid Fracture: A Case Report. Cureus. 2025 Aug 28;17(8):e91186. doi: 10.7759/cureus.91186. PMID: 40895664; PMCID: PMC12393304. NCBI
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.