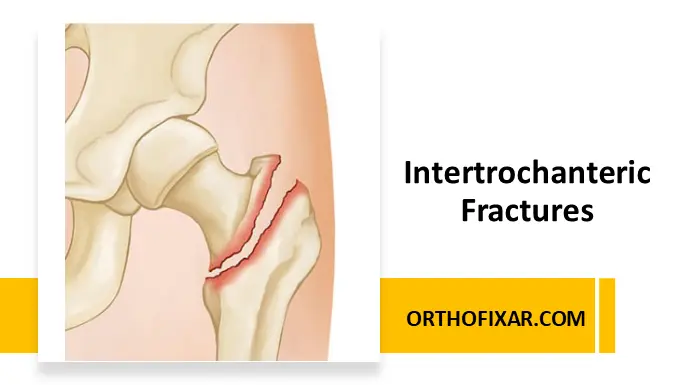
Intertrochanteric fractures are extracapsular fractures of the proximal femur occurring between the greater and lesser trochanters. These injuries are particularly common in elderly patients and represent a major cause of morbidity worldwide.
Epidemiology
Intertrochanteric hip fx account for ~50% of all proximal femur fractures.
- ~150,000 cases annually in the United States
- Incidence:
- 63 per 100,000 in elderly females
- 34 per 100,000 in elderly males
- Female-to-male ratio: 2:1 to 8:1
- Strong association with osteoporosis and postmenopausal bone loss
Key Risk Factors
- Advanced age
- Multiple comorbidities
- Reduced independence in activities of daily living
- History of fragility fractures
Anatomy
Intertrochanteric fractures occur in the cancellous bone-rich region between the trochanters, often extending into the subtrochanteric region.
Important Biomechanics
- Abundant blood supply → low risk of nonunion and osteonecrosis
- Muscle forces deform fracture fragments:
- Abductors → lateral/proximal displacement of greater trochanter
- Iliopsoas → medial/proximal displacement of lesser trochanter
- Hip muscles → proximal migration of distal fragment
Stability Determinant
- Posteromedial cortex integrity
- Intact → Stable fracture
- Comminuted → Unstable fracture
See Also: Hip Joint Anatomy
Mechanism of Injury
Elderly Patients (90%)
- Low-energy trauma
- Typically simple fall onto the greater trochanter
Younger Patients
- High-energy trauma:
- Motor vehicle accidents
- Falls from height
Clinical Presentation
Patients typically present with:
- Severe hip pain
- Inability to bear weight
- Shortened, externally rotated limb
Important Clinical Considerations
Delayed presentation is common, increasing risk of:
- Dehydration
- Malnutrition
- Venous thromboembolism (VTE)
- Pressure ulcers
- Hemodynamic instability (due to blood loss into thigh)
Radiographic Evaluation
Standard Imaging
- AP pelvis
- AP and cross-table lateral hip views
Additional Imaging
- Internal rotation view → better fracture visualization
- MRI → gold standard for occult fractures
- CT/Bone scan → if MRI contraindicated
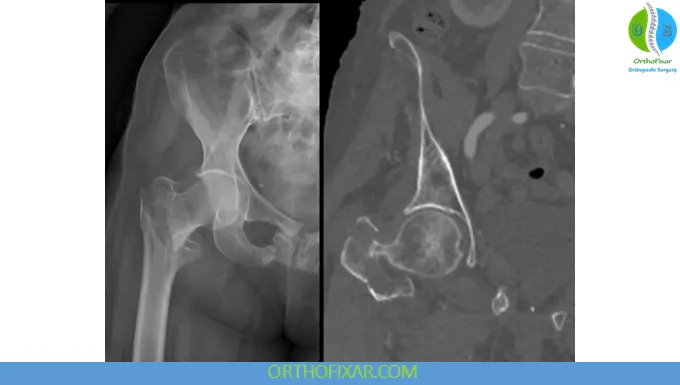
Intertrochanteric Fracture Classification
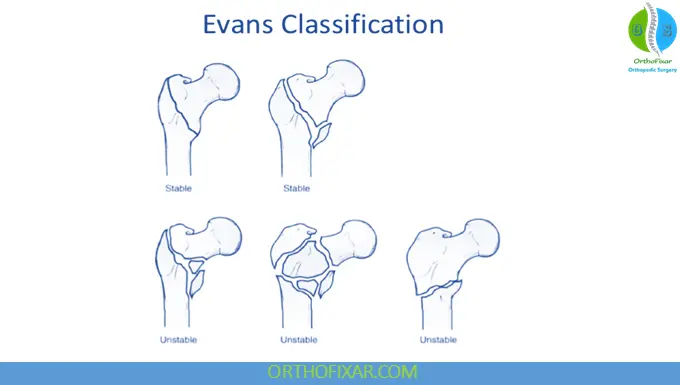
Evans Classification
Based on stability and reducibility:
- Stable fractures
- Intact posteromedial cortex
- Unstable fractures
- Comminution or loss of medial support
- Reverse oblique pattern
AO/OTA Classification
- A1 → Stable
- A2, A3 → Unstable
In practice, many clinicians simplify classification into stable vs unstable Intertrochanteric fracture, which has direct treatment implications.
Special Fracture Patterns
1. Basicervical Fractures
- Located at femoral neck base
- Behave like intertrochanteric fractures
- Higher risk of osteonecrosis
2. Reverse Oblique Fractures
- Oblique fracture line (medial → proximal, lateral → distal)
- Strong tendency for medial shaft displacement
- Treated like subtrochanteric fractures
Treatment of Intertrochanteric Fractures
Nonoperative Management
Reserved for:
- Medically unfit patients
- Non-ambulatory patients with minimal pain
Key principle:
- Early mobilization (bed-to-chair) to prevent complications
Operative Management (Standard of Care)
Goal: Stable fixation allowing early weight-bearing
Timing
- Surgery should be performed as soon as medically stable
Intertrochanteric Fracture Surgery Options
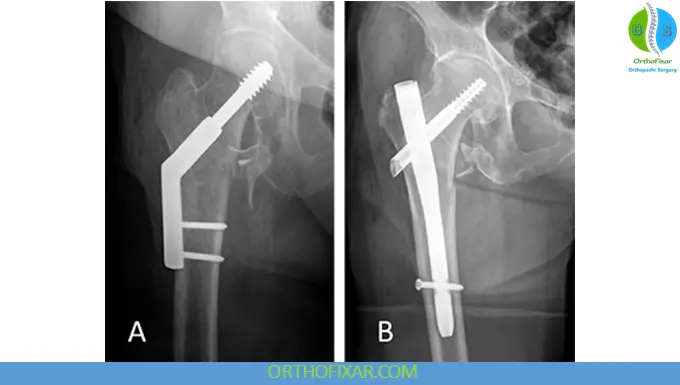
1. Sliding Hip Screw (SHS)
- Traditional gold standard
- Effective for stable fractures
Key Technical Point
- Tip–apex distance < 25 mm reduces risk of screw cutout
Limitations
- Higher failure in unstable fractures
- More collapse and shortening
2. Cephalomedullary Nail (CMN)
- Intramedullary device
- Biomechanically superior in unstable patterns
Advantages
- Less soft tissue damage
- Reduced bending stress
- Better for:
- Reverse oblique fractures
- Subtrochanteric extension
3. Prosthetic Replacement
- Indicated when:
- Fixation fails
- Severe comminution
Considerations
- Higher surgical morbidity
- Risk of dislocation
4. External Fixation
- Rarely used
- Reserved for select cases
- Associated with:
- Pin loosening
- Infection
Rehabilitation
- Early mobilization is critical
- Weight-bearing as tolerated
- Prevent complications:
- Pneumonia
- VTE
- Muscle wasting
Complications
1. Loss of Fixation (Most Common)
- Incidence: up to 20% in unstable fractures
Causes:
- Poor screw positioning
- Varus collapse
- Severe osteoporosis
2. Nonunion (<2%)
- Rare due to good blood supply
- Consider:
- Revision fixation
- Bone grafting
- Arthroplasty in elderly
3. Malrotation
- Causes gait dysfunction
- May require corrective osteotomy
4. Implant-Specific Complications
- Z-effect (dual screw nails)
- Nail tip impingement
- Screw cutout
5. Osteonecrosis
- Rare compared to femoral neck fractures
Key Clinical Pearls
- Stability (posteromedial cortex) determines treatment strategy
- Early surgery improves outcomes
- Tip–apex distance is critical for fixation success
- CMN preferred for unstable fracture patterns
- Early mobilization reduces mortality
References & More
- Attum B, Pilson H. Intertrochanteric Femur Fracture. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Kürüm H, Tosun HB, Aydemir F, Ayas O, Orhan K, Key S. Intertrochanteric Femoral Fractures: A Comparative Analysis of Clinical and Radiographic Outcomes Between Talon Intramedullary Nail and Intertan Nail. Cureus. 2023 Dec 21;15(12):e50877. doi: 10.7759/cureus.50877. PMID: 38259364; PMCID: PMC10801105. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.