PCL injury results from knee hyperextension or a blow to the anterior tibia as occurs when plantarflexed. A fall onto the ground with a plantar-flexed foot is also a mechanism of injury for PCL tears.
PCL Anatomy
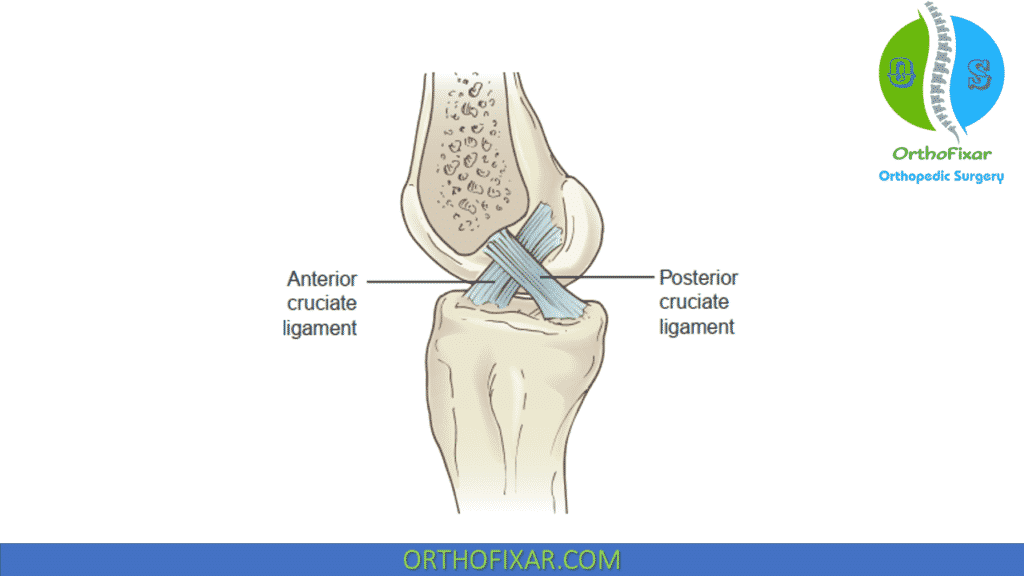
The PCL arises from the posterior aspect of the tibia and takes a superior and anterior course, passing medially to the ACL, to attach on the lateral portion of the femur’s medial condyle.
The PCL, stronger and 120% to 150% wider than the ACL, is a primary stabilizer of the knee.
The PCL has two distinct components the anterolateral and posteromedial bundles, bands named relative to their tibial insertions, although three and four bundles have been described in the PCL. The anterolateral bundle is taut when the knee is flexed and loosens when the knee is extended; the posteromedial bundle is relatively lax when the knee is flexed and tightens when the knee is extended.
The PCL is the primary restraint against posterior displacement of the tibia on the femur and a secondary restraint against external tibial rotation.
The PCL receives its limited blood supply from the middle geniculate artery.
See Also: Anterior Cruciate Ligament Injury
Mechanism of Injury
If the foot is dorsiflexed when falling on the knee, much of the force is directed toward the patellofemoral joint, thereby sparing the PCL. However, if the foot is plantarflexed, the resulting force is delivered to the PCL when the tibial tuberosity makes contact with the ground or another stationary object.
PCL Tear Grading
- Grade I injury: an isolated PCL injury in which the tibia remains anterior to the femoral condyles, 1-5 mm posterior tibial translation.
- Grade II injury: an isolated complete PCL injury in which the anterior tibia becomes flush with the femoral condyles, 6-10 mm posterior tibial translation.
- Grade III injury: an injury in which the tibia is posterior to the femoral condyles; usually indicative of associated ACL or PLC injuries or both, >10 mm posterior tibial translation.
PCL Injury Symptoms
Immediately after the onset of injury, the patient may be relatively asymptomatic or may display the signs and symptoms of a tear of the medial head of the gastrocnemius or a sprain of the posterior capsule. Unlike ACL tears, the patient may not report feeling a “pop” at the time of injury. Also the effusion may not be present initially but may develop over time.
Tenderness may be elicited in the popliteal fossa if the sprain involves the posterior capsular structures or
popliteus muscle; otherwise, no pain or abnormalities are usually noted.
Over time, symptoms such as pain in the posterior knee, weakness of the hamstring and quadriceps muscle groups, and reduced ROM during flexion and extension become evident.
Initially, knee ROM may be equal to that of the opposite limb if there is an isolated PCL sprain, but noticeable deficits will be evident if multiple structures are damaged.
The posterior drawer test and posterior sag sign are highly specific in identifying the presence of chronic PCL sprains. The quadriceps active test can identify grade II and III PCL tears.
Isolated PCL trauma results in greater posterior instability as the knee is flexed from 0 to 90 degrees. The LCL, posterolateral corner, and MCL are secondary restraints to posterior tibial displacement of the tibia on the femur, especially in the presence of a PCL-deficient knee.
Isolated PCL sprains increase the amount of posterior tibial translation but do not increase the varus rotation or external tibial rotation. Instability is greatest when there is concurrent damage to both the PCL and the knee’s posterolateral structures. PCL sprains must also be evaluated for posterolateral corner deficiencies.
See Also:
Imaging
Plain radiographs should be obtained to evaluate for avulsion injuries (acute) and arthrosis of the medial and patellofemoral compartments (chronic).
Stress radiographs are becoming the standard for evaluation and grading of PCL injuries; side-to-side differences of more than 12 mm on stress radiographs are suggestive of a combined PCL and PLC injury.
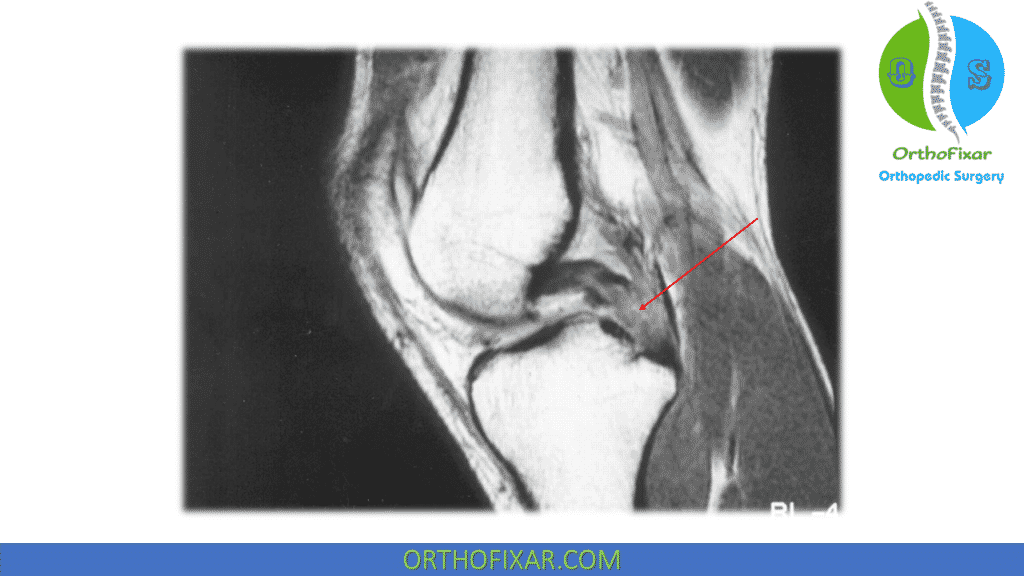
MRI is a confirmatory study, the presence of a complete or partial PCL tear can be identified via MRI.
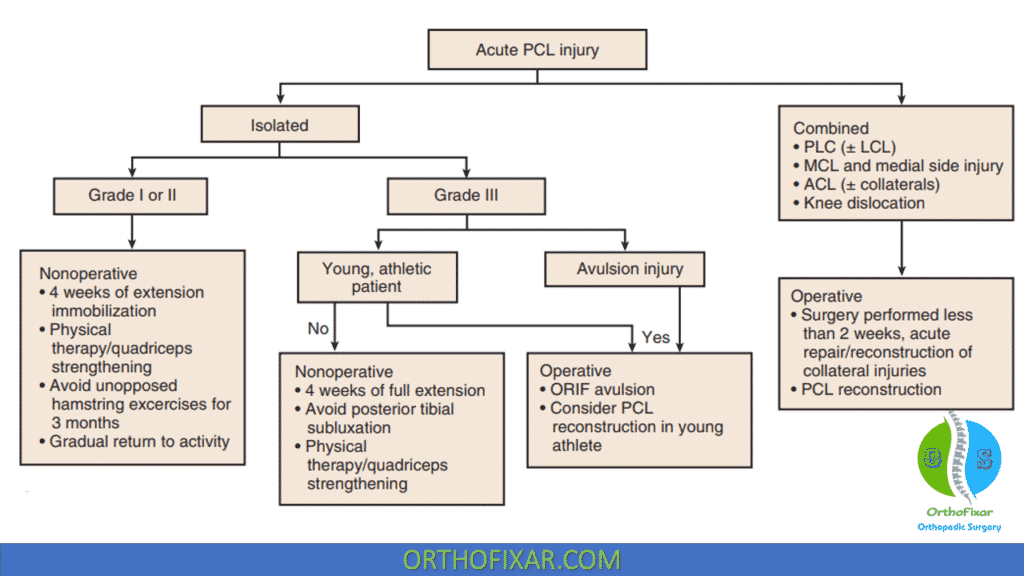
PCL Injury Treatment
posterior cruciate ligament injury treatment is nonoperative for most grade I and II (isolated) PCL injuries, these include:
- Protected weight bearing,
- Rehabilitation: PCL tear physical therapy should focus on strengthening the knee extensors. Patients treated nonoperatively can regain full function and independence and may often return to athletic competition unhindered by the ligamentous deficit.
PCL tear physical therapy include:
- Quadriceps strengthening and open-chain knee extension exercises protect the graft by resulting in an anterior-directed force.
- Open-chain knee flexion caused by hamstring contraction should be avoided because it causes posterior-directed force across the graft.
Grade III injuries are indicative of a combined injury, usually to the posterolateral corner. Bony avulsion fractures can be repaired primarily with good results, although primary repair of midsubstance PCL (and ACL) injuries has not been successful.
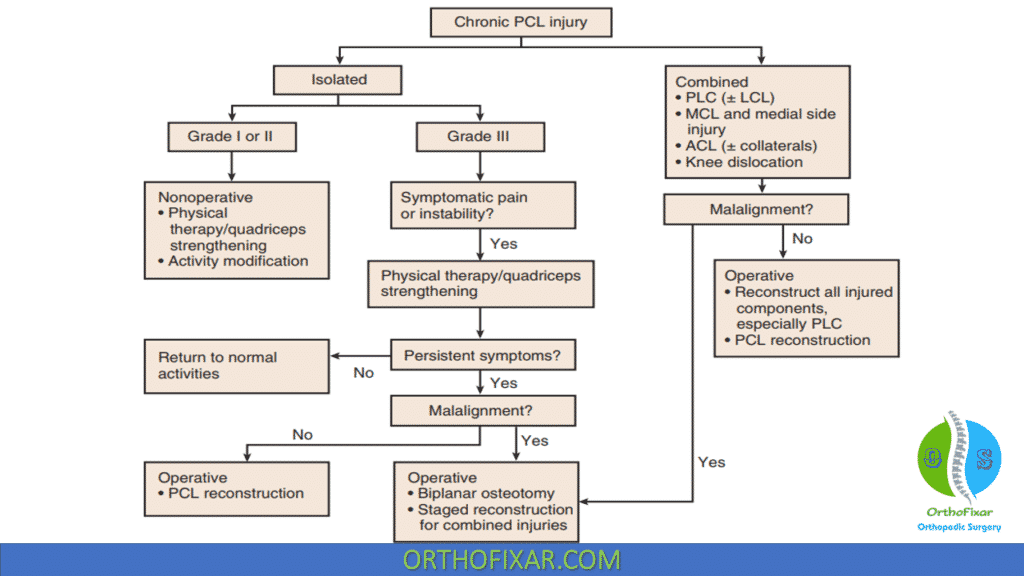
Chronic PCL deficiency can result in late chondrosis of the patellofemoral compartment or medial femoral condyle, or both.
PCL reconstruction is recommended for functionally unstable or combined injuries. In general, the results of PCL reconstruction are not as good as those of ACL reconstruction, and some residual posterior laxity often remains. For successful reconstruction, concomitant ligament injuries must be addressed.
A biplanar high tibial osteotomy can be used to treat combined malalignment and PCL insufficiency.
The strength of the quadriceps muscle group soon returns after a PCL sprain to assist the popliteus in providing muscular compensation against posterior tibial displacement. Actual posterior laxity does not always result in knee dysfunction.
Complications
If the PCL deficiency is not identified or not appropriately treated, changes in the structure and function of the ACL, meniscus, and weight-bearing surfaces will occur over time, potentially leading to chronic joint instability, alteration in the gait pattern, muscle activation patterns, and reduced muscle strength. The long-term consequence of these conditions is the early onset of OA and increased joint laxity.
References
- Davies H, Unwin A, Aichroth P. The posterolateral corner of the knee. Anatomy, biomechanics and management of injuries. Injury. 2004 Jan;35(1):68-75. doi: 10.1016/s0020-1383(03)00094-9. PMID: 14728958.
- Harner, CD, et al: The effects of a popliteus muscle load on in situ forces in the posterior cruciate ligament and on knee kinematics: a human cadaveric study. Am J Sports Med, 26:669, 1998.
- Schulz, MS, et al: Epidemiology of posterior cruciate ligament injuries. Arch Orthop Trauma Surg, 234:186, 2003.
- Cosgarea, AJ, and Jay, PR: Posterior cruciate ligament injuries: evaluation and management. J Am Acad Orthop Surg, 9:297, 2001.
- Schulz, MS, et al: Reliability of stress radiography for evaluation of posterior knee laxity. Am J Sports Med, 33:502, 2005.
- Fontboté, CA, et al: Neuromuscular and biomechanical adaptations of patients with isolated deficiency of the posterior cruciate ligament. Am J Sports Med, 33:982, 2005.
- Jonsson, H, and Karrholm, J: Three-dimensional knee kinematics and stability in patients with a posterior cruciate ligament tear. J Orthop Res, 17:185, 1999.
- Shelbourne, KD, Davis, TJ, and Patel, DV: The natural history of acute, isolated, nonoperatively treated posterior cruciate ligament injuries: a prospective study. Am J Sports Med, 27:276, 1999.
- Goyal, K, et al: In vivo analysis of the isolated posterior cruciate ligamentdeficient knee during functional activities. Am J Sports Med, 40:777, 2012.
- Ochi, M, et al: Isolated posterior cruciate ligament insufficiency induces morphological changes of anterior cruciate ligament collagen fibrils. Arthroscopy, 15:292, 1999.