Movement impairment syndromes (MIS) are defined as localized painful conditions arising from irritation of myofascial, periarticular, or articular tissues.
It was described by Shirley Sahrmann in her book “Diagnosis and Treatment of Movement Impairment Syndromes” in 2001.
The repeated movements and sustained postures alter tissue characteristics, which eventually change the pattern of movement and ,if less than ideal, can cause impairment. If movements are faulty or strength and flexibility are compromised, negative changes occur in soft tissues and in bony structures. The eventual result of injury to these tissues is musculoskeletal pain or a movement impairment syndrome.
The intrinsic factors, such as characteristics of the patient, and extrinsic factors, such as work type and fitness can contribute to the tissue changes.
See Also: Thomas Test
Hip Movement Impairment Syndromes
Movement Impairment Syndromes of the Hip include the following:
| Syndrome | Accessory Movement | Associated Diagnoses |
|---|---|---|
| Femoral anterior glide | Without rotation | Iliopsoas tendinopathy; bursitis |
| With medial rotation | Iliopsoas tendinopathy; bursitis | |
| With lateral rotation | Adductor strain; iliopsoas tendinopathy; groin pull | |
| Hip adduction | Without rotation | Gluteus medius strain; trochanteric bursitis |
| With medial rotation | Lengthened piriformis syndrome; iliotibial band fascitis | |
| Hip extension | With knee extension | Hamstring strain as a result of insufficient gluteus maximus or quadriceps participation |
| With hip medial rotation | Hamstring strain as a result of insufficient intrinsic lateral rotator muscle participation | |
| Femoral accessory | Early degenerative hip joint disease | |
| Hypermobility | Labral tears | |
| Femoral hypomobility | With superior glide | Degenerative hip joint disease |
| Hip lateral rotation | Shortened piriformis syndrome | |
| Femoral lateral glide | Short axis distraction | Hip pain; popping hip; subluxation |
The intervention for these syndromes focuses on the correction of muscle imbalances. The adaptively shortened structures are stretched and the weak muscles are strengthened.
Femoral Anterior Glide Syndrome:
The characteristic findings for Femoral Anterior Glide Syndrome result from an insufficient posterior glide of the femoral head during hip flexion.
This syndrome is often diagnosed as iliopsoas tendonitis because of the pressure exerted by the femoral head against the anterior joint structures, which occurs when the postural alignment of the hip is hyperextension. This pressure combined with the diminished posterior glide of the femur during hip flexion causes the femur to impinge on the anterior tissues of the joint capsule.
Typically, the patient complains of groin pain, particularly during hip flexion, gait, and running.
The consequences of this syndrome are:
- stretching of the anterior joint capsule and tightening of the posterior structures resulting in excessive hip extension ROM;
- an increase or decrease in the length of the hip external rotators;
- a decreased posterior glide of the femoral head;
- a decrease in length of the TFL on the involved side;
- weakness and lengthening of the iliopsoas on the involved side;
- dominance of hamstring activity over gluteus maximus activity, both of which are shortened.
See Also: Hip ROM

Hip Extension with Knee Extension Syndrome:
The characteristic findings for Hip Extension with Knee Extension Syndrome result from an insufficient participation of the gluteus maximus during hip extension or the quadriceps during knee extension.
Typically, the patient complains of pain at the hamstring insertion site on the ischial tuberosity and along the muscle belly, particularly during resisted hip extension, knee flexion, or both.
The consequences of this syndrome are:
- a decrease in hip flexion because of the hypertrophy of the hamstrings;
- dominance of hamstring activity over gluteus maximus activity;
- weakness of the gluteus maximus and hip external rotators;
- a decrease in the length of the hamstrings;
- an increase in the frequency of hamstring strains.
Femoral Accessory Motion Hypermobility:
The characteristic findings for Femoral Accessory Motion Hypermobility result from early degenerative changes and increased compression at the hip joint because of stretching forces on the rectus femoris and hamstrings.
Typically, the patient complains of pain deep in the hip joint and anterior groin that may extend along the medial and the anterior thigh, particularly during gait.
The consequences of this syndrome are:
- A slight antalgic gait,
- internal rotation of the hip during single-leg stance,
- external rotation of the hip with passive knee flexion in prone,
- medial rotation of the femur with knee extension in sitting,
- stiffer rectus femoris and hamstrings as compared to the iliopsoas and intrinsic hip internal rotators,
- anterior hip joint pain with FABER test.
Lumbar Movement Impairment Syndromes
Sahrmann categorizes a number of movement impairment syndromes that can present in the lumbar spine as a result of an imbalance of flexibility and strength.
The intervention for each of the syndromes involves a correction of these imbalances:
Flexion syndrome: This syndrome is characterized by lumbar flexion motions that are more flexible than hip flexion motions. The syndrome is typically found in the 8–45 year old age range and results in pain with positions or motions associated with lumbar flexion, because of adaptive shortening of the gluteus maximus, hamstrings, or rectus abdominis.
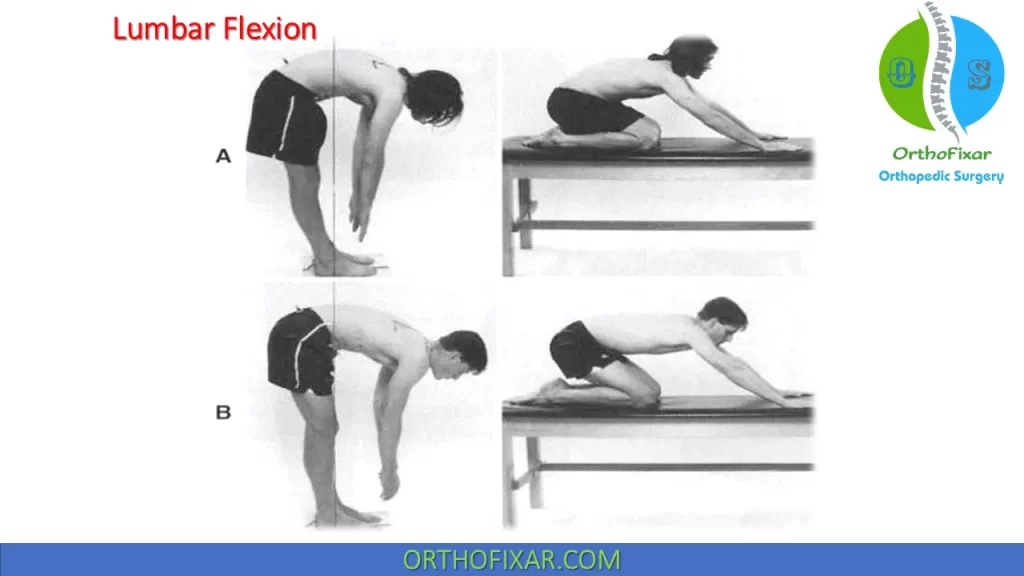
Extension syndrome: This syndrome is characterized by lumbar extension motions that are more flexible than hip extension motions. Patients with this syndrome are usually older than 55 years of age, and the symptoms are increased with positions or motions associated with an increase in lumbar lordosis, because of adaptive shortening of the hip flexors and lumbar paraspinals and weakness of the external
oblique muscles.
Lumbar rotation: This syndrome is characterized by pain that is unilateral or greater on one side and is increased with rotation to one side. No attempt is made to equate the side of rotation with the side of the symptoms. It is theorized that this syndrome is produced when one segment of the lumbar spine rotates, side bends, glides, or translates more easily than the segment above or below it. This syndrome is associated with spinal instability and can result from habitual motions or positions that involve rotation to one side, a leg-length discrepancy , or a muscle imbalance between the oblique abdominal muscles.
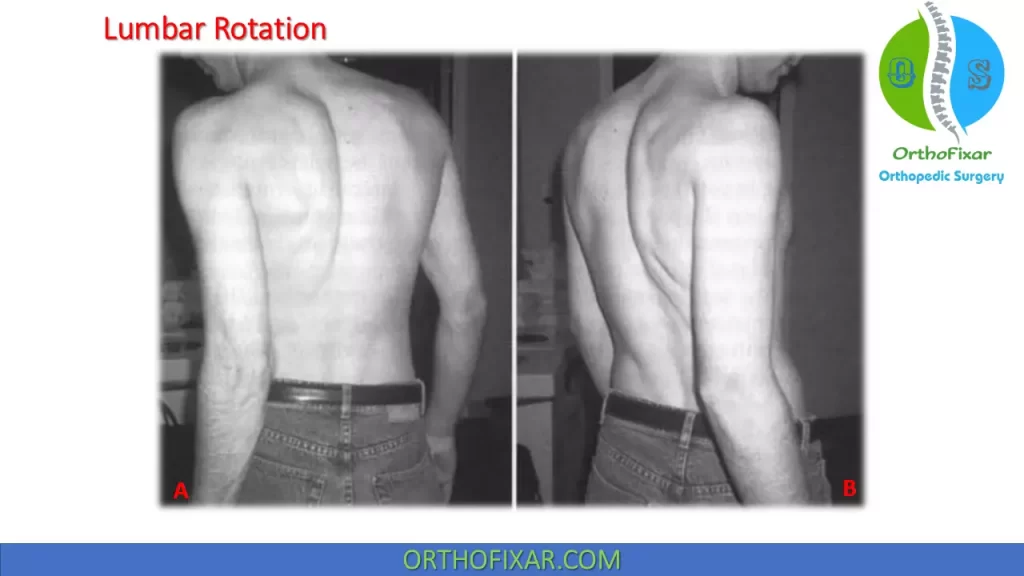
Lumbar flexion with rotation: This syndrome is characterized by pain that is unilateral or greater on one side and is increased with the combined motion of lumbar flexion and rotation. Many of the characteristics of the lumbar flexion and lumbar rotation syndromes can be applied to this syndrome.
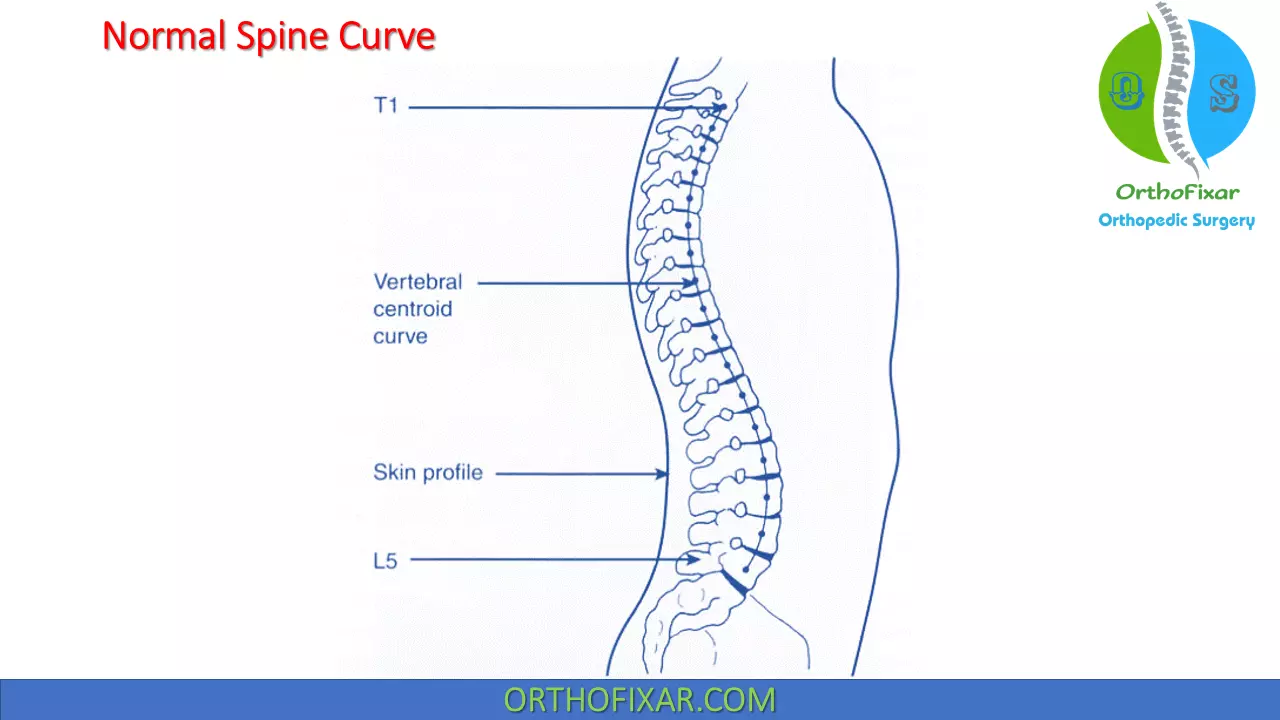
Lumbar extension with rotation: This syndrome is characterized by pain that is unilateral or greater on one side and is increased with the combined motion of lumbar extension and rotation. Many of the characteristics of the lumbar extension and lumbar rotation syndromes can be applied to this syndrome.

References
- Sahrmann S, Azevedo DC, Dillen LV. Diagnosis and treatment of movement system impairment syndromes. Braz J Phys Ther. 2017 Nov-Dec;21(6):391-399. doi: 10.1016/j.bjpt.2017.08.001. Epub 2017 Sep 27. PMID: 29097026; PMCID: PMC5693453.
- Sahrmann SA: Movement impairment syndromes of the hip. In: Sahrmann SA, ed. Movement Impairment Syndromes. St Louis, MO: Mosby, 2001:121–191.
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
