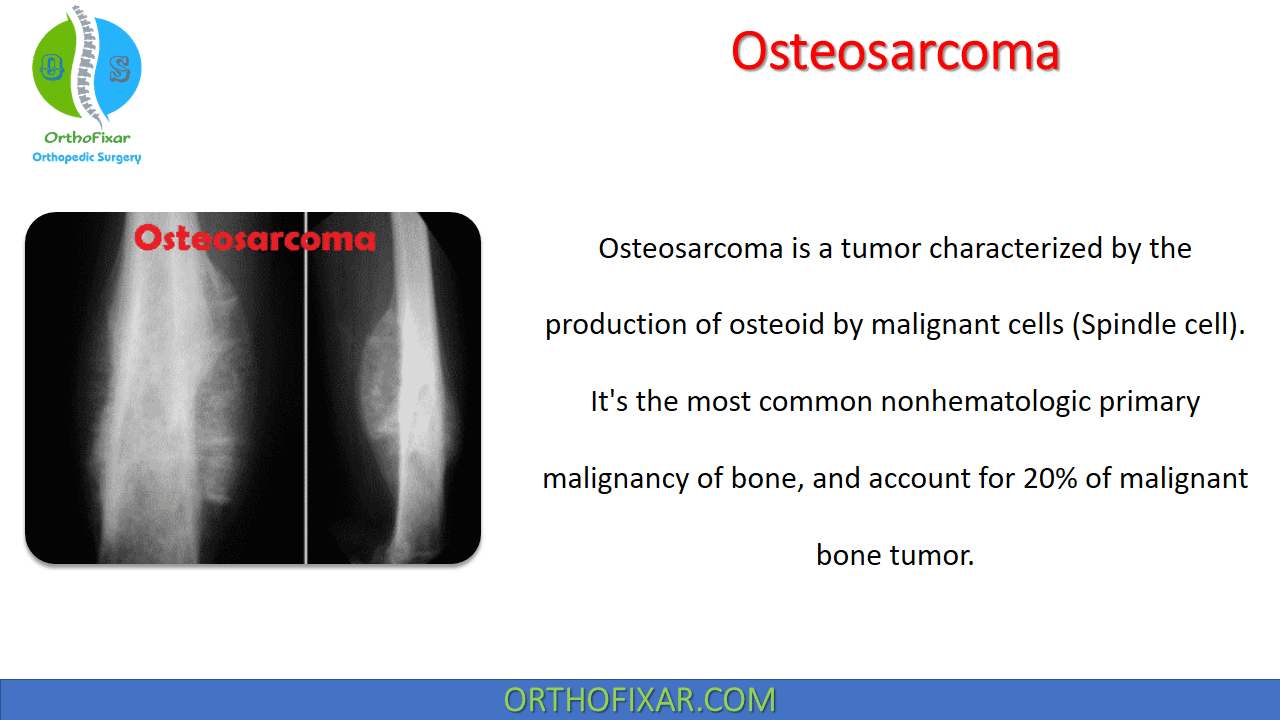
Osteosarcoma is a tumor characterized by the production of osteoid by malignant cells (Spindle cell). It’s the most common nonhematologic primary malignancy of bone, and account for 20% of malignant bone tumor.
It occurs most commonly in the second decade of life.
The most important prognostic factor at the time of diagnosis is the tumor stage.
See Also: Differential Diagnosis for Bone Lesions
Types of Osteosarcomas
Primary Types
Primary types include:
- Intramedullary osteosarcoma.
- Parosteal osteosarcoma.
- Periosteal osteosarcoma.
Secondary Types
Secondary types occur at the site of another disease process. They rarely occur in young patients but constitute almost half of the osteosarcomas in patients older than age 50 years.
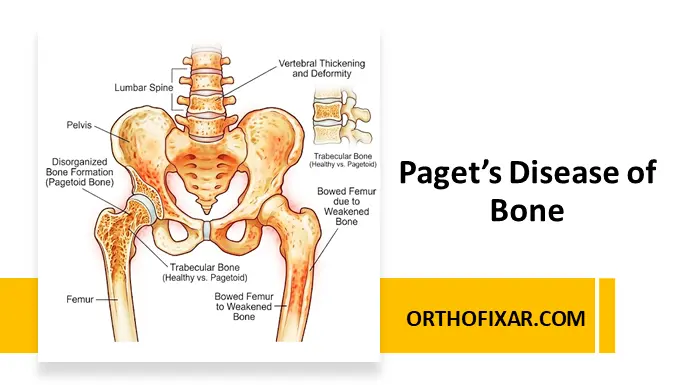
These types may occur with Paget disease or after irradiation.
Telangiectatic Osteosarcoma
It is a purely lytic lesion. On a radiograph, it can have an invasive appearance, or it can have a ballooned appearance similar to that of an aneurysmal bone cyst.
Intramedullary Osteosarcoma
It is the most common type, usually occurs in children and young adults (mostly second decade of life).
Most common location is the distal femur and proximal tibia, it can also occurs in proximal humerus, proximal femur, and pelvis.
More than 90% of intramedullary osteosarcomas are high grade and penetrate the cortex early to form a soft tissue mass (stage IIB lesion).
10% to 20% of affected patients have pulmonary metastases at presentation.
Lungs are the most common site for metastasis whereas bone is the second most common site.
Osteosarcoma symptoms include pain, fever and swelling and may feel a mass in the site of tumor.
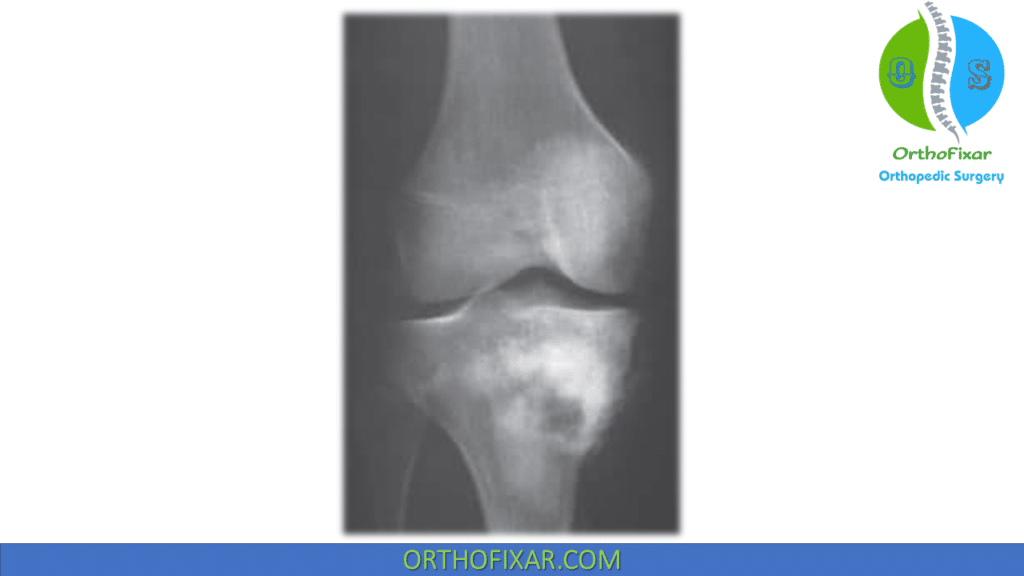
Radiology:
A purely sclerotic or lytic lesion in which there is bone destruction and bone formation and a periosteal reaction (Codman’s triangle).
MRI is useful for defining the anatomy of the lesion with regard to intramedullary extension, involvement of neurovascular structures, and muscle invasion.
Bone scan: shows a hot spot, useful to evaluate extent of local disease and presence of bone metastases.
Chest CT is required to evaluate for pulmonary metastases.
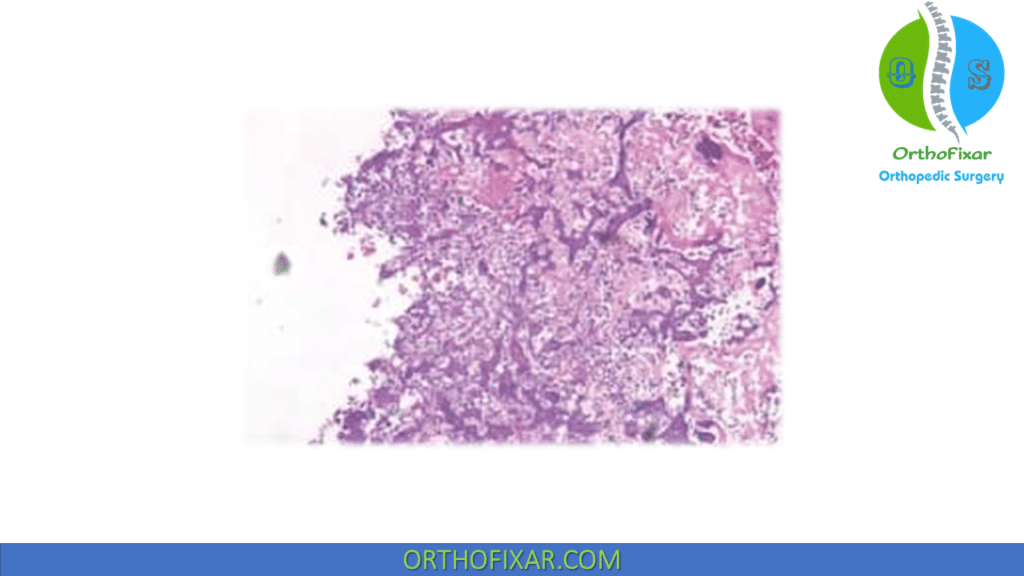
Histology
Diagnosis depends on two histologic criteria: tumor cells produce osteoid and stromal cells are frankly malignant.
Tumor cells show significant atypia and produce osteoid. Giant cells may be present in giant cell rich osteosarcoma.
Differentials Diagnosis
- Ewing’s sarcoma.
- Leukemia
- Lymphoma
- Eosinophilic granuloma
- Osteomyelitis
- Desmoplastic fibroma
- Fibrosarcoma
- Dedifferentiated chondrosarcoma
- Secondary sarcoma
- Rhabdomyosarcoma
Treatment of Intramedullary Osteosarcoma
Treatment includes:
Preoperative chemotherapy for 8-12 weeks followed by wide-margin surgical resection (limb salvage).
Maintenance chemotherapy for 6-12 months after surgical resection.
Limb amputation indications:
- Pathologic fracture
- Encasing neurovascular bundle
- Enlarging during preop chemo AND adjacent to neurovascular bundle.
Parosteal Osteosarcoma
Parosteal osteosarcoma is a rare, low grade sarcoma. It arises on the surface of the bone and invades the medullary cavity only at a late stage.
Women > Men and mostly occurs at the age of 30-40 years old.
Most common sites are the posterior aspect of the distal femur, proximal tibia, and proximal humerus.
Patients often present with a painless mass.
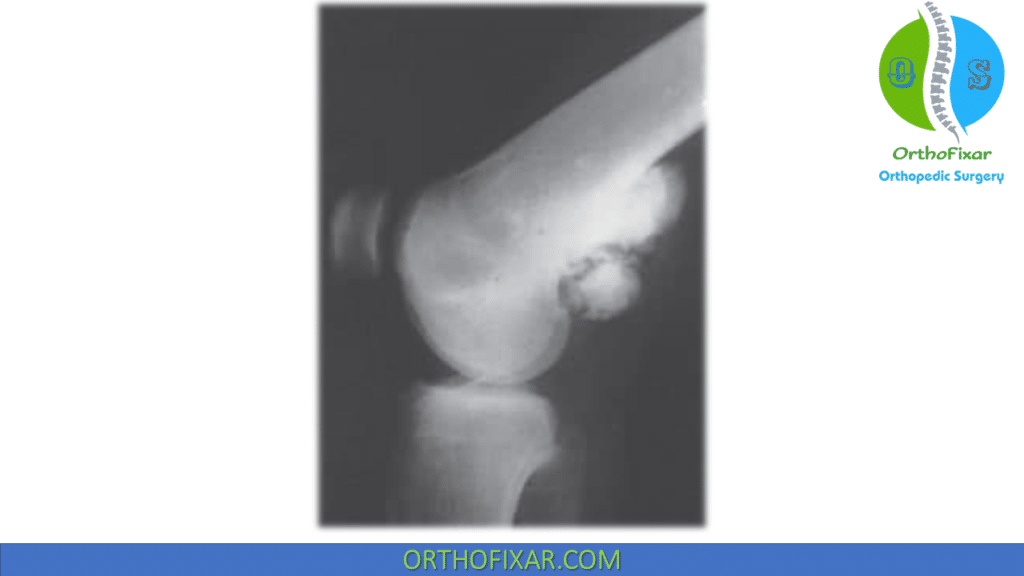
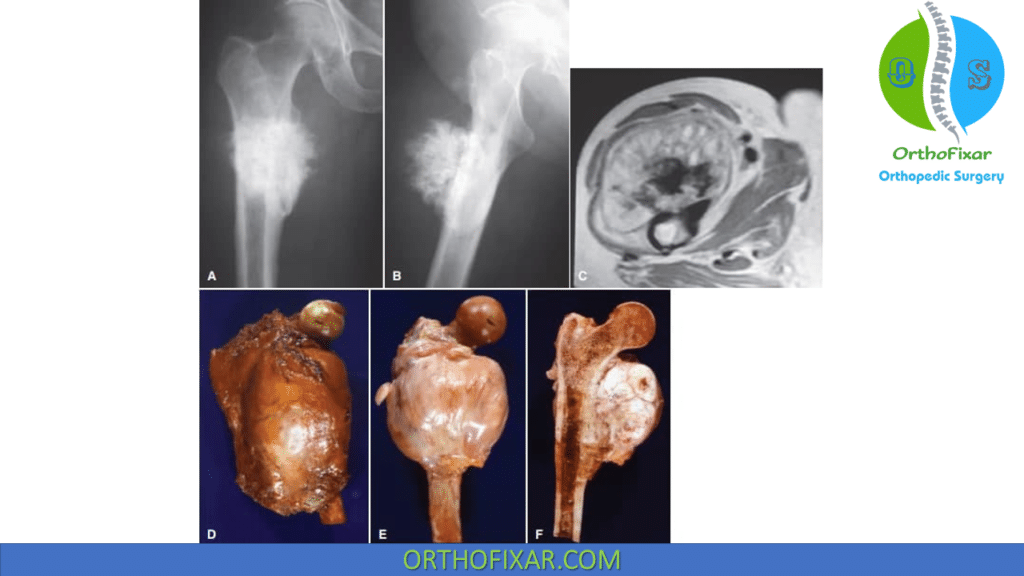
Imaging Evaluation:
Characteristic radiographic appearance: a heavily ossified, often lobulated mass arising from the cortex (mostly the posterior aspect of the distal femur).
CT may be helpful in differentiating this subtype of osteosarcoma from myositis ossificans or an osteochondroma. The ossification in myositis ossificans is more mature at the periphery of the lesion, whereas the center of a parosteal osteosarcoma is more heavily ossified.
MRI: Helps determine soft tissue / marrow involvement and skip lesions.
Bone scan: Shows a hot spot.
Histology
Parosteal Osteosarcoma histology is look like a low-grade intramedullary osteosarcoma. It consists of slightly atypical spindle cells seen between regularly arranged osseous trabeculae.
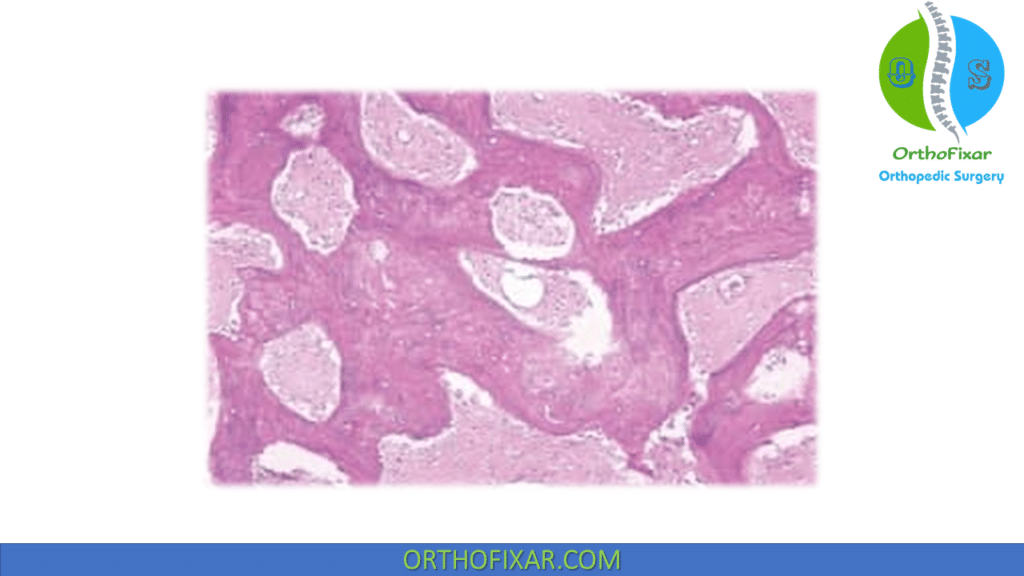
Differentials Diagnosis
- Fibrous dysplasia
- Myositis Ossificans
- Osteochondral exostosis
- Developmental defect at insertion of adductor magnus
Parosteal Osteosarcoma Treatment
Surgical resection with a wide margin.
Chemotherapy is not required except in high grade tumor.
Periosteal Osteosarcoma
Periosteal Osteosarcoma is a rare surface form (intermediate grade). Mostly occurs in the diaphysis of long bones (typically femur or tibia).
Imaging Evaluation
It has a sunburst-type lesion rests on a saucerized cortical depression. There is no involvement of the medullary canal.
Bone scan: Shows a hot spot.
CT scan: required for staging and evaluation the presence of pulmonary metastasis
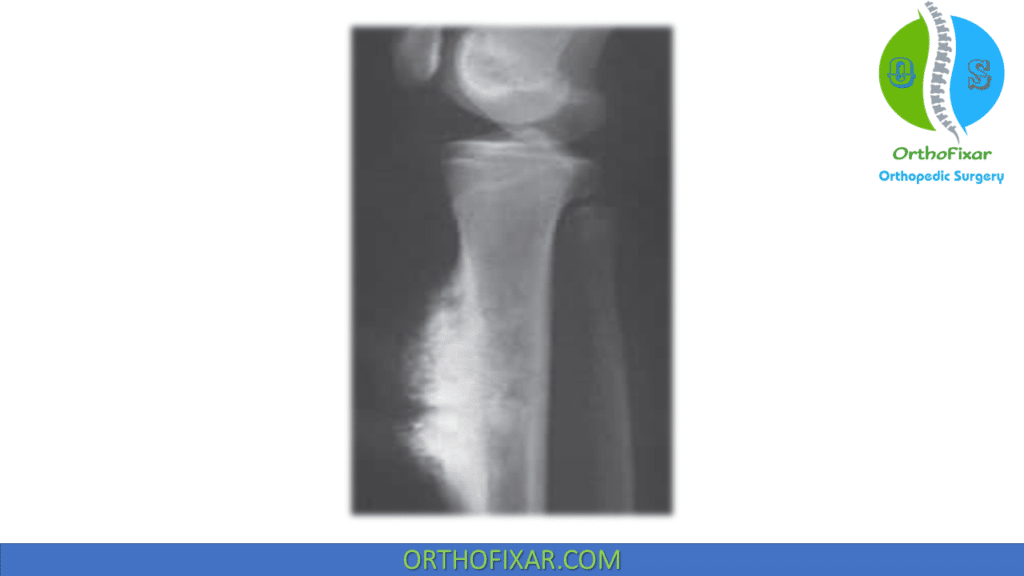
Histology
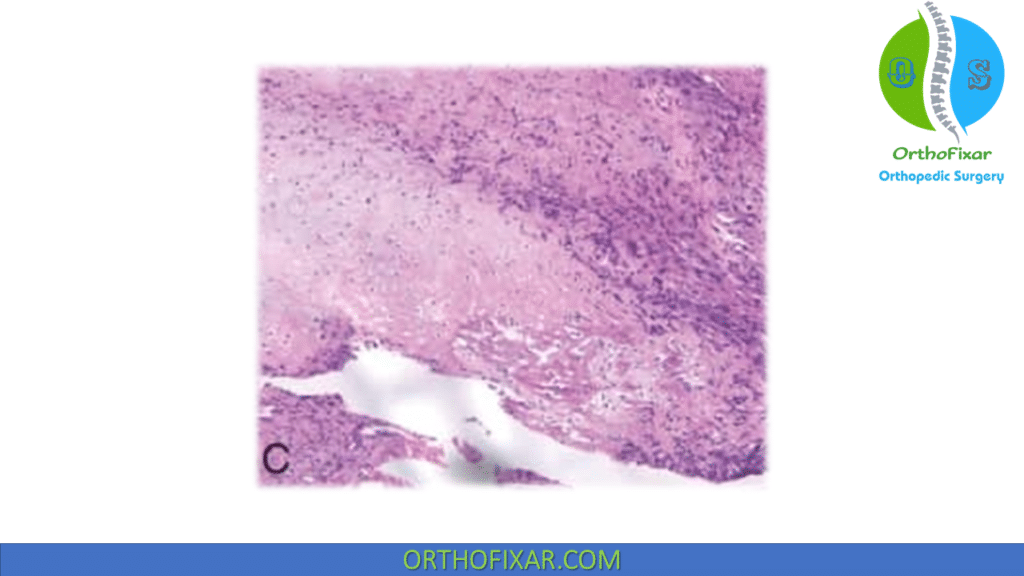
Lobular and cartilaginous appearance.
Histology reveals areas of chondroblastic matrix although the tumor produces osteoid. If histology shows no osteoid production, tumor would be classified as a chondrosarcoma.
Periosteal Osteosarcoma Treatment
Preoperative chemotherapy for 8-12 weeks followed by wide-margin surgical resection (limb salvage).
Maintenance chemotherapy for 6-12 months after surgical resection.
High-grade surface osteosarcoma
This type is extremely a rare form of surface osteosarcomas.
Imaging is a mixed lytic sclerotic aggressive surface lesion in the metaphysis or diaphysis.
Treatment and prognosis are the same as conventional osteosarcoma.
Telangiectatic osteosarcoma
Tissue of the lesion can be described as a bag of blood with few cellular elements. It occurs in the same locations as aneurysmal bone cysts; radiographic appearances of both can be confused.
Radiographic features are those of a destructive, lytic, expansile lesion.
References & More
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.
- Lindsey BA, Markel JE, Kleinerman ES. Osteosarcoma Overview. Rheumatol Ther. 2017 Jun;4(1):25-43. doi: 10.1007/s40744-016-0050-2. Epub 2016 Dec 8. PMID: 27933467; PMCID: PMC5443719.
- Prater S, McKeon B. Osteosarcoma. [Updated 2022 May 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK549868/