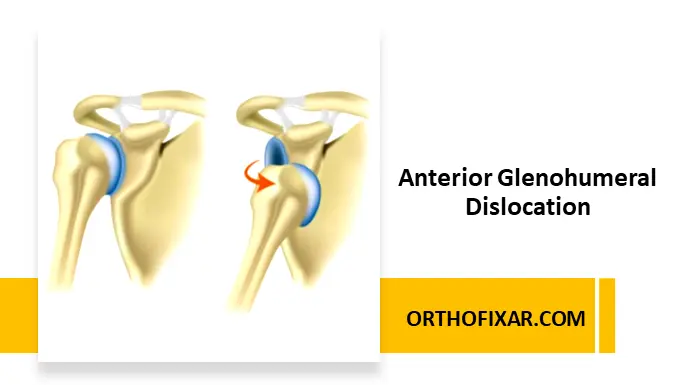
Anterior glenohumeral dislocation is the most common type of shoulder dislocation, accounting for approximately 96% of all cases. It involves displacement of the humeral head from the glenoid cavity in an anterior direction, typically resulting from traumatic mechanisms or underlying joint instability.
The Anterior Glenohumeral Dislocation is frequently encountered in emergency and orthopedic settings and requires prompt recognition, reduction, and appropriate follow-up to minimize complications.
Incidence
- Anterior Glenohumeral Dislocation Represents ~96% of shoulder dislocations
- It’s Common in young, active individuals, particularly athletes
- It’s also seen in older adults, often associated with falls and rotator cuff pathology
Mechanism of Injury
1. Indirect Trauma (Most Common)
- Anterior Glenohumeral Dislocation occurs with the shoulder in:
- Abduction
- Extension
- External rotation
- Typical in sports injuries (e.g., throwing, tackling)
2. Direct Trauma
- Posteriorly directed force to the shoulder
- Pushes the humeral head anteriorly
3. Other Causes
- Convulsions or electrical shock (less common for anterior dislocation)
- Recurrent instability due to:
- Congenital laxity
- Capsular insufficiency
- Prior dislocations
See Also: Glenohumeral Joint Anatomy
Clinical Evaluation
History
- Mechanism and timing of injury
- Prior dislocations or instability episodes
- Presence of ligamentous laxity
- Contralateral shoulder involvement
Physical Examination
Typical Presentation
- In Anterior shoulder dislocation, the arm is held in:
- Slight abduction
- External rotation
- Severe pain and muscle spasm
Inspection and Palpation
- “Squared-off” shoulder appearance
- Prominent acromion
- Palpable mass anteriorly (displaced humeral head)
- Hollow beneath posterior acromion
Neurovascular Assessment (Critical)
- Axillary nerve:
- Sensation over lateral deltoid
- Motor: deltoid contraction (often limited acutely)
- Musculocutaneous nerve:
- Sensation over anterolateral forearm
⚠️ Deltoid weakness may be due to pain—not always nerve injury.
Special Test
Apprehension Test
- Performed in abduction + external rotation
- Positive if patient experiences:
- Pain
- Sense of instability
See Also: Shoulder Apprehension Test
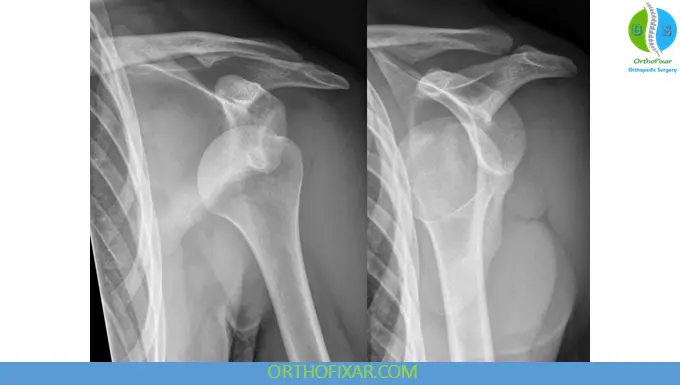
Radiographic Evaluation
Standard Trauma Series
- Anteroposterior (AP) view
- Scapular-Y view
- Axillary view
When to Obtain Pre-reduction X-rays
- First-time dislocation
- Age > 40 years
- High-energy trauma
Alternative View
- Velpeau axillary view
- Used when patient cannot abduct due to pain
Special Imaging Views
- West Point view: evaluates anterior glenoid rim
- Hill-Sachs view: detects posterolateral humeral head defects
- Stryker notch view: identifies humeral head lesions
Advanced Imaging
- CT scan:
- Bony defects
- Glenoid fractures (bony Bankart lesions)
- MRI:
- Labral tears (Bankart lesion)
- Rotator cuff injuries
- Capsular damage
See Also: Shoulder X-ray Views
Classification
Based on Stability
- Dislocation vs. subluxation
Based on Chronology
- Acute
- Chronic
- Recurrent
Based on Etiology
- Traumatic Anterior Glenohumeral Dislocation: single major injury, often labral tear
- Atraumatic Anterior Glenohumeral Dislocation: ligamentous laxity, minimal trauma
Based on Direction
- Subcoracoid (most common)
- Subglenoid
- Intrathoracic (rare)
Based on Patient Control
- Voluntary
- Involuntary
Anterior Glenohumeral Dislocation Treatment
Closed Reduction
Performed after:
- Adequate analgesia
- Sedation or intra-articular anesthesia
Common Reduction Techniques
- Traction–countertraction
- Stimson technique (gravity-assisted)
- Scapular manipulation
- Milch technique
⚠️ Kocher maneuver is not recommended due to fracture risk.
See Also: Shoulder Reduction Techniques
Post-reduction Care
- Immobilization:
- 2–5 weeks
- Shorter duration in older adults
- Sling or immobilizer (Velpeau dressing offers no clear advantage)
Rehabilitation
- Gradual progression:
- External rotation
- Flexion and abduction
- Early motion:
- Hand, wrist, and elbow
Operative Management
Indications
- First-time dislocation in young active patients
- Irreducible Anterior Glenohumeral Dislocation
- Associated injuries:
- Greater tuberosity fracture (>5 mm displacement)
- Glenoid rim fracture (>5 mm)
- Soft tissue interposition
Surgical Options
- Arthroscopic Bankart repair (most common)
- Capsular shift / capsulorrhaphy
- Tendon or bony transfer procedures (refractory cases)
Postoperative Care
- Immobilization duration varies by age:
- <30 years: up to 3 weeks
- 30–40 years: ~2 weeks
- 50 years: 1–2 weeks
- Early controlled range-of-motion exercises
- Progressive strengthening
Complications
1. Recurrent Instability (Most Common)
- Strongly age-dependent:
- Age 20: 80–92%
- Age 30: ~60%
- Age 40: 10–15%
- Most occur within 2 years
- More common in males and athletes
2. Osseous Injuries
- Hill-Sachs lesion
- Bony Bankart lesion
- Greater tuberosity fracture
- Acromion or coracoid fractures
3. Soft Tissue Injuries
- Rotator cuff tears (especially in older patients)
- Capsular and tendon injuries
4. Neurovascular Injuries
- Axillary nerve (most common)
- Musculocutaneous nerve
- Usually neurapraxia → recovery expected
- Persistent deficits >3 months require further evaluation
5. Vascular Injury
- Rare, but serious
- Typically involves axillary artery
- More common in elderly patients
6. Degenerative Changes
- Posttraumatic osteoarthritis may develop over time
Key Takeaways
- Anterior shoulder dislocation is the most frequent type of shoulder instability
- Prompt clinical and radiographic evaluation is essential
- Closed reduction is the mainstay of initial management
- Recurrent instability is the most common complication, especially in younger patients
- Surgical stabilization is indicated in selected high-risk or recurrent cases
References & More
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Pak T, Kim AM. Anterior Glenohumeral Joint Dislocation. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed

[…] See Also: Anterior Glenohumeral Dislocation […]