Perilunate dislocations are among the most severe and commonly missed injuries of the wrist. These high-energy injuries disrupt the intricate ligamentous architecture of the carpus, leading to instability, long-term dysfunction, and posttraumatic arthritis if not promptly recognized and treated.
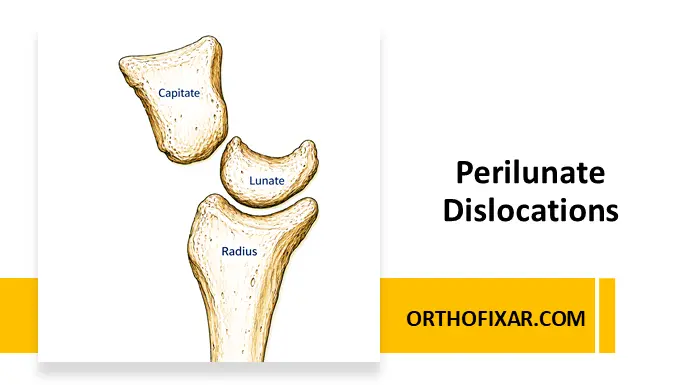
The lunate—often referred to as the “carpal keystone”—plays a central role in maintaining wrist stability due to its strong ligamentous attachments to the distal radius. Disruption of this relationship defines perilunate injuries.
Anatomy and Biomechanics
The carpus is composed of two rows of bones working in harmony to allow complex wrist motion. Stability depends on both bony architecture and ligamentous integrity.
- The lunate acts as the central stabilizer
- Intercarpal ligaments (especially the scapholunate and lunotriquetral ligaments) maintain alignment
- Disruption leads to predictable patterns of instability
Loss of normal carpal kinematics results in progressive collapse and degenerative changes, as well documented in studies indexed in PubMed.
See Also: Wrist Anatomy
Classification of Perilunate Injuries
1. Greater Arc Injuries
These injuries pass through the bones surrounding the lunate:
- scaphoid
- capitate
- triquetrum
- Distal radial styloid
Common patterns:
- Transscaphoid perilunate fracture-dislocation (most common)
- Transcapitate injuries
- Transradial styloid injuries
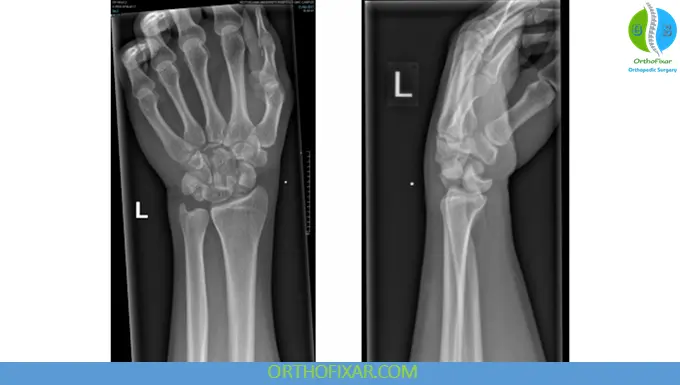
See Also: Scaphoid Fractures
2. Lesser Arc Injuries
These involve purely ligamentous disruption:
- scapholunate ligament
- Midcarpal joint
- lunotriquetral ligament
These injuries result in:
- Perilunate dislocation
- Lunate dislocation (advanced stage)
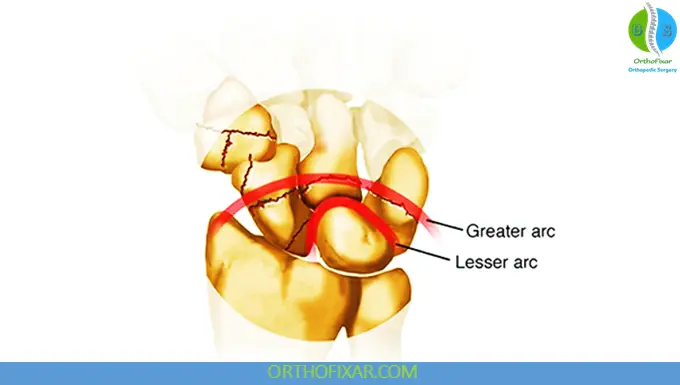
Mechanism of Injury
Perilunate Dislocation injuries typically occur due to:
- Axial load applied to the thenar eminence
- Wrist forced into hyperextension
This mechanism is common in:
- Falls on an outstretched hand (FOOSH)
- High-energy trauma (motor vehicle accidents, sports injuries)
Mayfield Progression of Instability
Perilunate Dislocation injuries follow a predictable pattern described by Mayfield classification:
Stage I – Scapholunate Disruption
- Injury to scapholunate ligament
- Early instability
Stage II – Midcarpal Disruption
- Capitate displaces dorsally
- Radioscaphocapitate ligament injured
Stage III – Lunotriquetral Disruption
- Complete dissociation of proximal row
Stage IV – Lunate Dislocation
- Lunate dislocates volarly into the carpal tunnel
- Capitate occupies lunate fossa
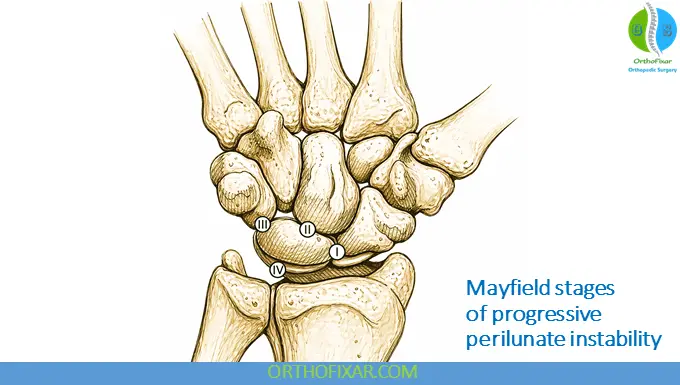
Clinical Presentation
Typical findings include:
- Wrist pain and swelling
- Tenderness distal to Lister’s tubercle
- Decreased range of motion
- Possible median nerve symptoms (numbness, tingling)
In dorsal perilunate dislocation:
- Prominent dorsal wrist deformity may be present
Radiographic Evaluation
Standard Imaging
- PA view
- Lateral view (most important)
- Oblique view
Key Radiologic Signs
PA View:
- Disrupted Gilula lines
- Scapholunate gap > 3 mm (“Terry Thomas sign”)
- Triangular (“piece-of-pie”) lunate appearance
Lateral View:
- Misalignment of capitate and lunate
- “Spilled teacup sign” → indicates volar lunate dislocation
CT Scan:
- Useful for detecting associated fractures and defining injury pattern
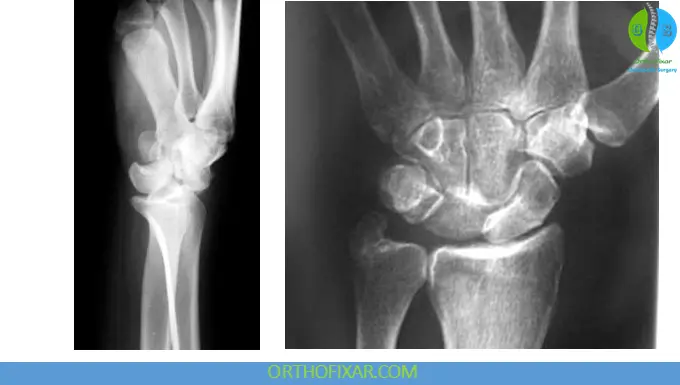
Perilunate Dislocation Treatment
1. Emergency Management
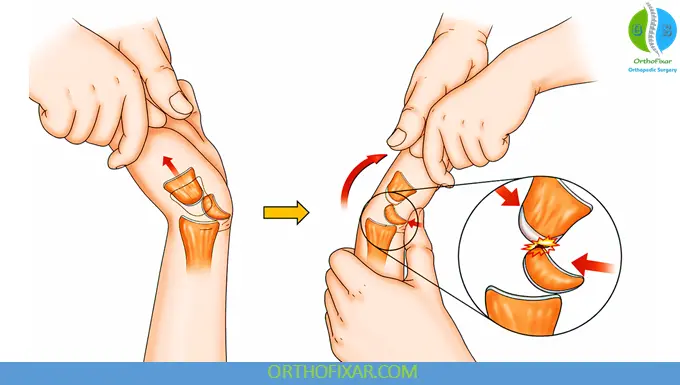
Closed reduction (Tavernier technique):
- Longitudinal traction (5–10 minutes)
- Wrist hyperextension
- Volar pressure on lunate
- Palmar flexion to reduce capitate
⚠️ Note: Closed reduction is often unsuccessful in lunate dislocations.
2. Surgical Management
Preferred treatment in most cases:
- Open reduction and internal fixation (ORIF)
- Repair of ligamentous structures
- Stabilization with K-wires
Special Case: Transscaphoid Injuries
- Fix scaphoid fracture first
- Then restore carpal alignment
3. Indications for Urgent Surgery
- Median nerve compression
- Failed closed reduction
- Severe instability
May require carpal tunnel release.
4. Limited Indications
Closed reduction + pinning:
- For patients unfit for surgery
Complications
1. Median Neuropathy
Compression within the carpal tunnel may necessitate urgent decompression.
2. Posttraumatic Arthritis
- Due to cartilage damage or malalignment
- Common long-term outcome
3. Chronic Perilunate Instability
Occurs with delayed or missed diagnosis:
- Chronic pain
- Weakness
- Carpal collapse
Treatment options:
- Ligament reconstruction (tenodesis, capsulodesis)
- Salvage procedures:
- Proximal row carpectomy
- Radiocarpal fusion
Prognosis
Outcomes depend heavily on:
- Timing of diagnosis
- Accuracy of reduction
- Adequacy of ligament repair
Delayed treatment (>6 weeks) significantly worsens prognosis, often requiring salvage surgery.
Key Takeaways
- Perilunate dislocations are high-energy, frequently missed injuries
- The lunate is the keystone of carpal stability
- Transscaphoid perilunate fracture-dislocation is the most common type
- Diagnosis relies heavily on lateral X-ray findings
- Early surgical management is critical to prevent long-term disability
References & More
- French RJ. Fractures and dislocations of the wrist. In: Brinker MR, ed. Review of Orthopaedic Trauma. 2nd ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2013:323–352.
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Duckworth AD, Strelzow J. Carpal fractures and dislocations. In: Tornetta P III, Ricci WM, Ostrum RF, et al., eds. Rockwood and Green’s Fractures in Adults. Vol 1. 9th ed. Philadelphia: Wolters Kluwer; 2020:1591–1664.
- Frane N, Goldenberg W. Perilunate Dislocation. [Updated 2023 Aug 14]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Jagiella-Lodise O, Sweeney A, Ghareeb P, Zelenski NA. Perilunate Dislocation Reduction Technique and Results. Hand (N Y). 2026 Mar;21(3):372-379. doi: 10.1177/15589447251317236. Epub 2025 Feb 13. PMID: 39949064; PMCID: PMC11826821. Pubmed