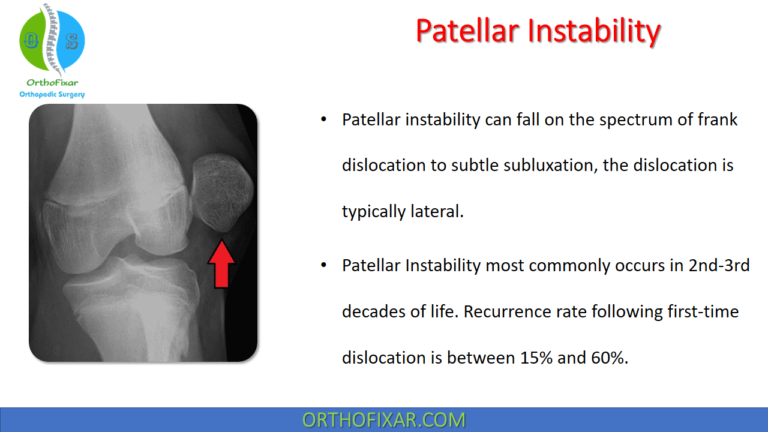
Medial Tibial Stress Syndrome (MTSS), commonly known as shin splints, is one of the most frequent causes of leg pain in athletes. It accounts for nearly 60% of all exercise-related leg injuries. MTSS is an overuse injury characterized by periostitis at the posterior medial border of the tibia, often triggered by repetitive activities such as running or jumping.
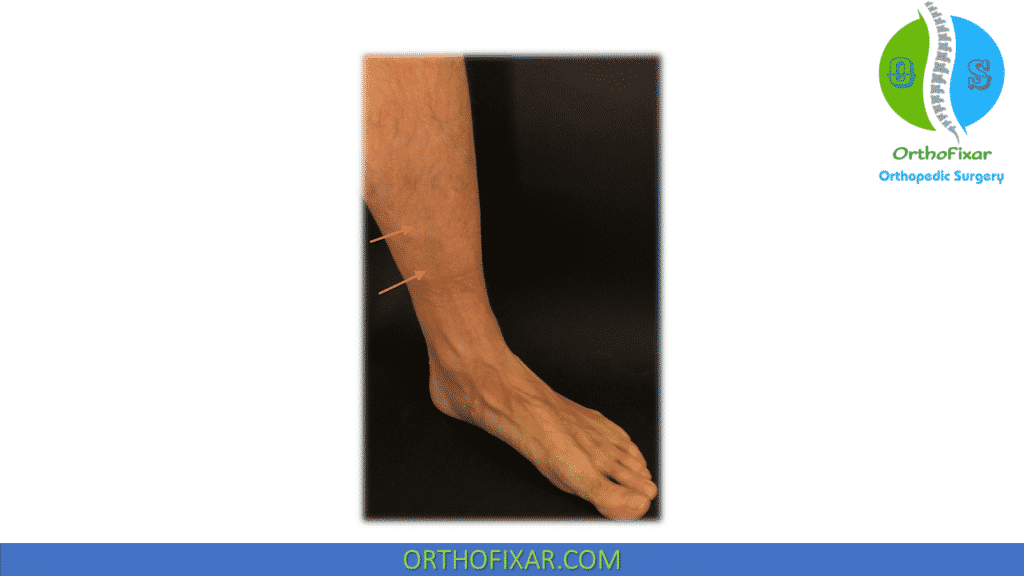
The pain in Medial Tibial Stress Syndrome is usually located along the posteromedial border of the tibia and diffuse and broad (>5 cm) rather than pinpointed (which suggests a stress fracture).
What is Medial Tibial Stress Syndrome?
Medial Tibial Stress Syndrome is an overuse injury of the tibia caused by irritation and inflammation of the periosteum (the connective tissue around the bone).
Other names for MTSS include:
- Periostitis
- Medial tibial syndrome
- Tibial stress syndrome
- Shin splints
- Posterior tibial syndrome
- Soleus syndrome
See Also: Femoral Stress Fracture
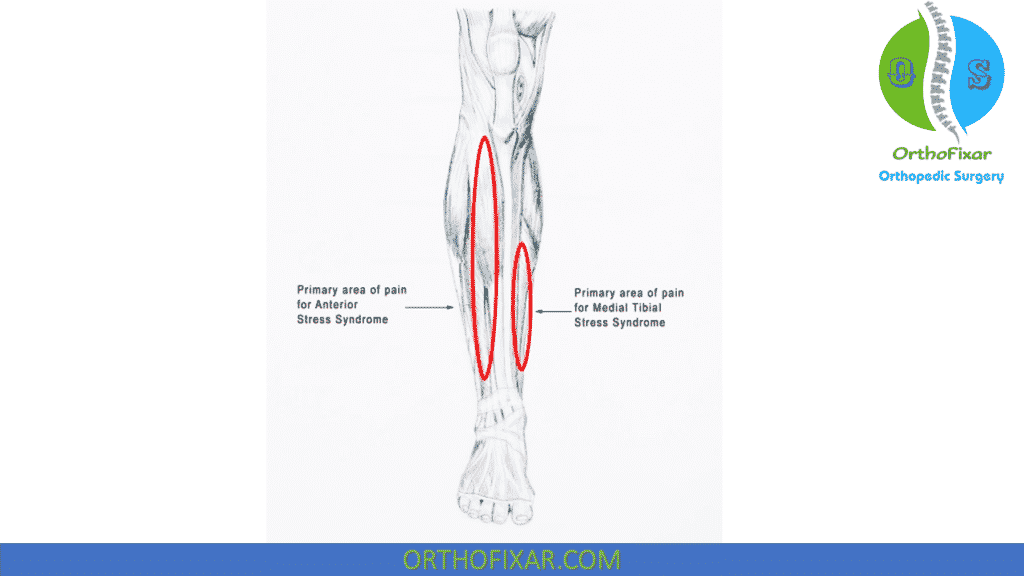
Causes of Medial Tibial Stress Syndrome
MTSS appears to involve periosteal irritation indicated by a diffuse linear uptake on a bone scan along the length of the tibia. The anatomic site of the abnormality has been fairly well localized to the fascial insertion of the medial soleus.
The onset of Medial Tibial Stress Syndrome is attributed to the following causes:
- training errors (training on a hard surface, increasing load too quickly),
- incorrect footwear,
- Overuse or weakness of the tibialis anterior, EDL, or EDB,
- biomechanical abnormalities.
Prolonged pronation, indirectly measured via static observation, an excessive navicular drop or directly using more sophisticated gait measures, is a key feature associated with the development of this condition.
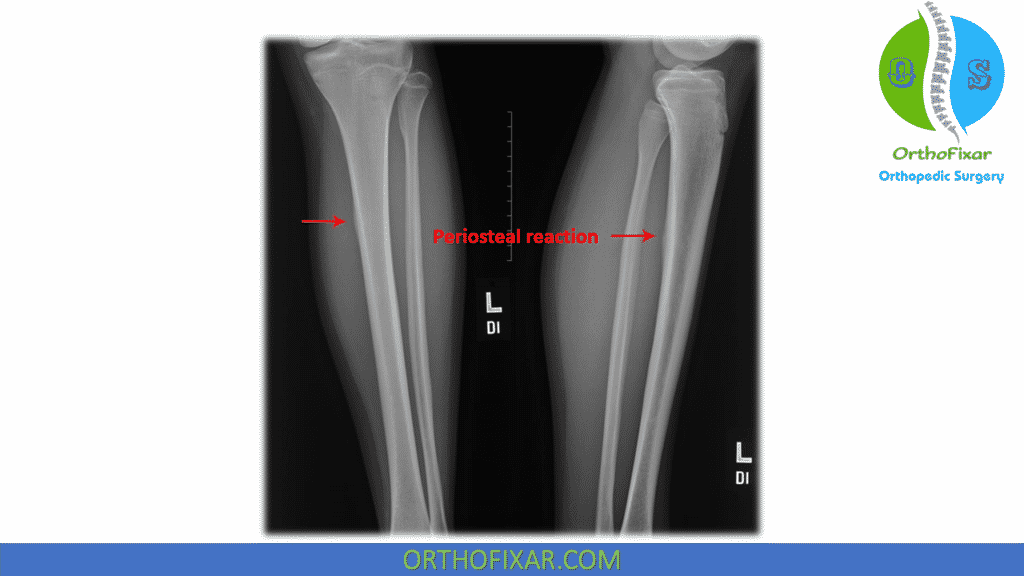
A bone stress reaction, MTSS may be a precursor to stress fractures, and bone scans in individuals with MTSS reveal uptake of the radionucleotide in the involved region
Clinical Evaluation
Patients describe a gradual onset of symptoms, consistent with many overuse injuries.
Early in the progression, patients describe a dull aching pain along the middle or distal posteromedial tibia at the beginning of an exercise session that subsides as activity continues but returns when the activity is over. At this stage, the pain typically subsides quickly with rest. With continued training the pain usually becomes more severe, and persistent, and with increasing chronicity, the pain may be present with ambulation or at rest.
The diffuse pain at the posteromedial tibial border covers a broad span (greater than 5 cm), not the localized tenderness associated with stress fractures.
Palpation at the medial and distal posteromedial border is painful.
Repetitive muscle testing of the long toe flexors, posterior tibialis, or soleus may replicate symptoms that emerge with fatigue of these muscles.
Imaging
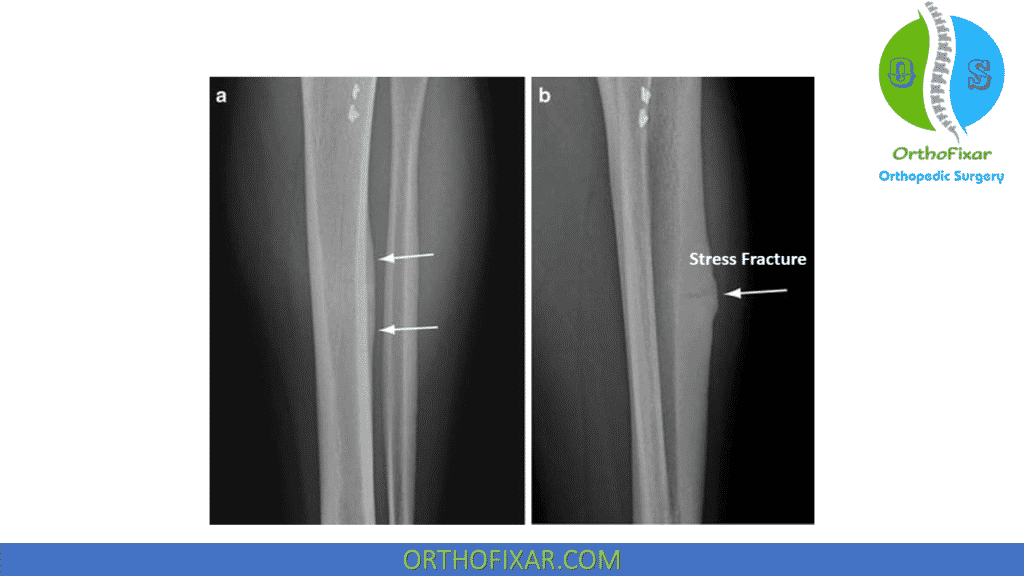
Radiographs and bone scans is required to differentiate from stress fractures.
Differential Diagnosis
Differential Diagnosis of Medial Stress Syndrome include:
- Tibial stress fracture,
- deep posterior exertional compartment syndrome,
- deep vein thrombosis,
- popliteal artery entrapment syndrome
| Finding | Stress Fracture | Medial Tibial Stress Syndrome | Acute Compartment Syndrome | Chronic Exertional Compartment Syndrome |
|---|---|---|---|---|
| Symptom Characteristics | Localized over the involved area of the bone | More diffuse along the posteromedial border of the middle or distal one-third of the tibia | Severe pain in the involved compartment of the leg Numbness on the dorsum of the foot, especially the web space between the 1st and 2nd toes (anterior) Dorsalis pedis pulse may be diminished (anterior) | Pain in the involved compartment of the leg Numbness on the dorsum of the foot, especially the web space between the 1st and 2nd toes Dorsalis pedis pulse diminished |
| Onset | Following changes in footwear or playing surfaces or increases in intensity, duration, or frequency of activity | Following changes in footwear or playing surfaces or increases in intensity, duration, or frequency of activity | Acute following trauma to the anterior leg Acute during exercise but symptoms not decreasing with rest | Symptoms increasing in proportion to exercise, resulting in inability to continue Pain possibly limiting activity after symptoms begin |
| Pain Patterns | Increased with activity and decreased with rest Possibly progressing to constant pain | Initially, pain at the start of activity, possibly diminishing with continued participation; pain possibly increasing again at the end of activity Pain decreasing with rest | Unremitting pain most likely prohibiting activity | Pain increasing with activity Pain decreasing with rest |
| Positive Findings | Localized pain with palpation | Pain with palpation over the posteromedial tibia Pain during toe raises Pain during resisted plantarflexion, inversion, dorsiflexion, or toe flexion. | Pain with active or resisted motion of the compartment’s muscles Pain with passive stretching of the compartment’s muscles | Pain after or during exercise |
| Negative Test Results | AROM MMT PROM | AROM PROM | Most test results negative if the individual has not been exercising recently | |
| Definitive Diagnosis | Bone scan Radiograph MRI | Bone scan may show periosteal irritation | Intracompartmental pressure minus diastolic BP ≥30 mm Hg Pain that does not subside with rest | Increased intracompartmental pressure after activity Pain that subsides with rest |
Medial Tibial Stress Syndrome Treatment
Medial Tibial Stress Syndrome is treated non-operatively, consisting of:
- Rest from the offending activities is typically effective.
- Activity modification, followed by a gradual return to sports
- Controlling excessive pronation through adequate footwear or orthotics also provides relief.
- An examination of lower extremity biomechanics and posture accompanied by appropriate strengthening and ROM exercises may be necessary.
FAQ
Is Medial Tibial Stress Syndrome the same as shin splints?
Yes. MTSS is the medical term for shin splints, a common overuse injury in runners.
How long does MTSS take to heal?
Most cases resolve in 1–3 months with rest and rehabilitation.
Can MTSS turn into a stress fracture?
Yes. Untreated MTSS can progress into a tibial stress fracture.
How to prevent MTSS?
Gradual training increases, supportive footwear, orthotics, and strengthening exercises help prevent recurrence.
References
- Andrish JT: Leg pain. In: DeLee JC, Drez D, eds. Orthopedic Sports Medicine. Philadelphia, PA: WB Saunders, 1994:1603–1607.
- Bennett JE, Reinking MF, Pluemer B, Pentel A, Seaton M, Killian C. Factors contributing to the development of medial tibial stress syndrome in high school runners. J Orthop Sports Phys Ther. 2001 Sep;31(9):504-10. doi: 10.2519/jospt.2001.31.9.504. PMID: 11570734.
- Yates, B, and White, S: The incidence and risk factors in the development of medial tibial stress syndrome among naval recruits. Amer J Sports Med, 32:772, 2004.
- Willems, TM, et al: Gait-related risk factors for exercise-related lowerleg pain during shod running. Med Sci Sports Exer, 39:330, 2007.
- Edwards, PH, Wright, ML, and Hartman, JF: A practical approach for the differential diagnosis of chronic leg pain in the athlete. Am J Sports Med, 33:1241, 2005.