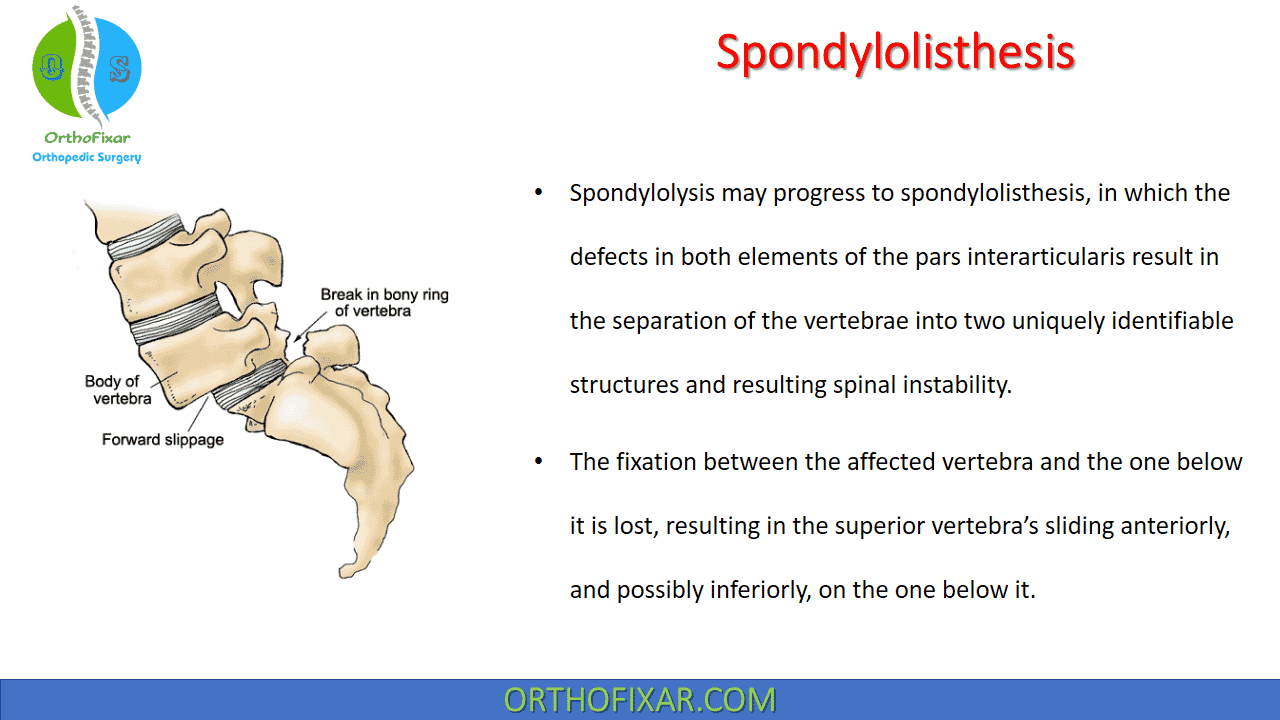
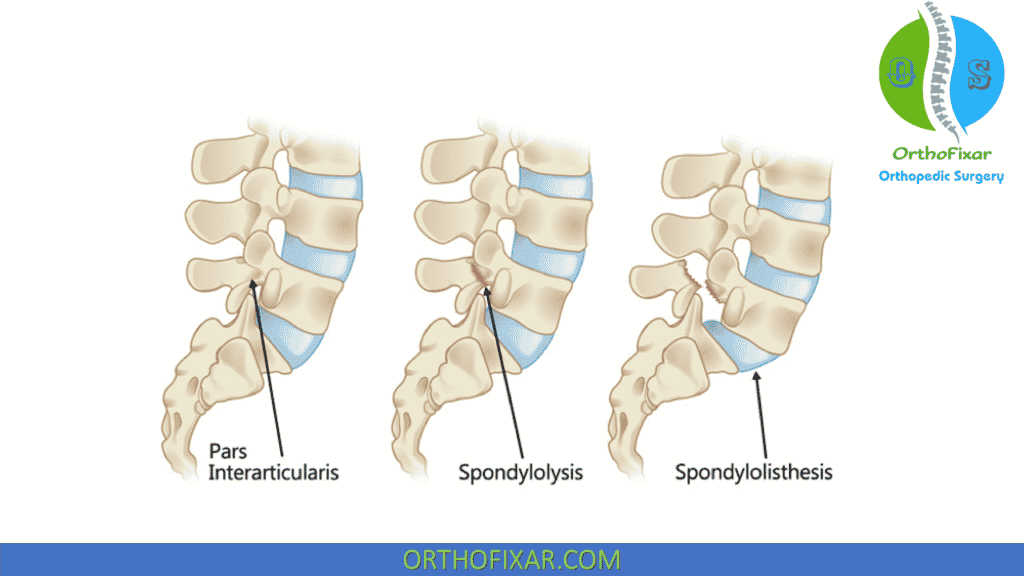
Spondylolisthesis is a pathological condition that can develop as a progression of spondylolysis. It is characterized by defects in both elements of the pars interarticularis, leading to the separation of the vertebrae into distinct structures and subsequent instability of the spine.
The loss of fixation between the affected vertebra and the one below it causes anterior slippage, and potentially inferior slippage, of the superior vertebrae on the adjacent vertebra. This condition is identifiable through distinct anatomical changes and can result in various clinical manifestations.
It’s most prevalent in adolescents under the age of 16 and in women. Also, young gymnasts have an incidence of pars interarticularis defects four times higher than that of the average population.
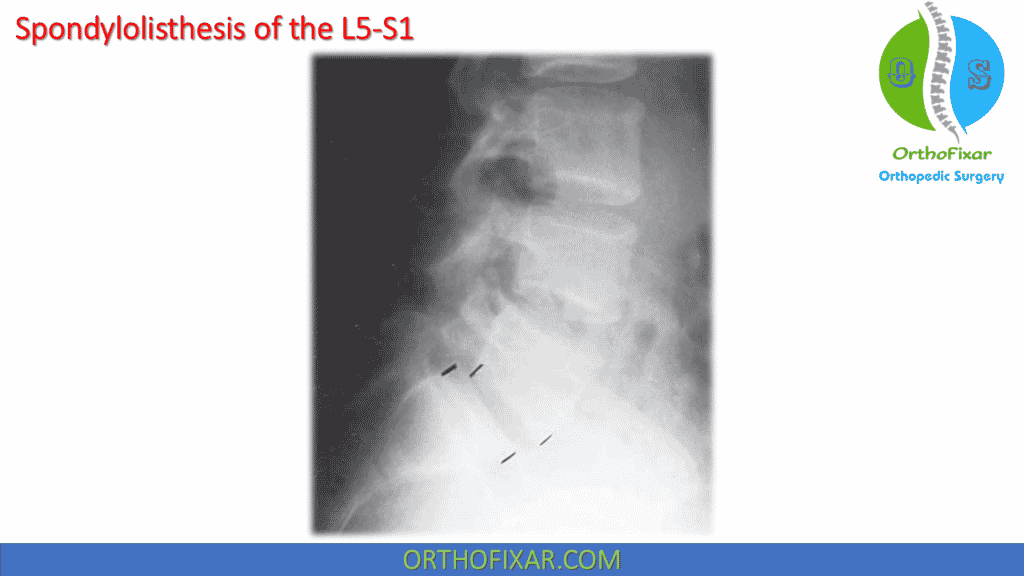
The most common site for spondylolysis and spondylolisthesis L5 S1.
Age appears to be an important factor in the natural history of spondylolisthesis. Children younger than 5 years of age rarely present with spondylolysis, and severe spondylolisthesis is equally rare.
The period of most rapid slipping is between the ages of 10 and 15 years, with no more slipping occurring after the age of 20. In the adolescent spine, the zygapophyseal joints are more horizontal than in the adult’s allowing more side flexion and rotation, and causing the lumbar disk and posterior column structures to sustain a greater responsibility for mobility control. Higher grade spondylolisthesis is twice as common in girls as in boys, and is approximately four times more common in women than men.
Causes
The causes of spondylolisthesis has been discussed extensively in the literature. Newman described five groups represented by this deformity, based on etiology:
- Congenital spondylolisthesis: This type results from dysplasia of the fifth lumbar and sacral arches and zygapophyseal joints.
- Isthmic spondylolisthesis: This type is caused by a defect in the pars interarticularis, which can include a fracture or elongation of the pars.
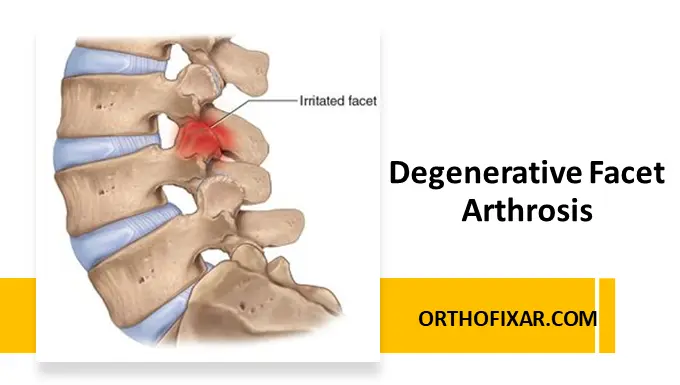
- Degenerative spondylolisthesis: This type usually affects older people and occurs most commonly at the L4–5 level. This type is perhaps the most commonly encountered by the orthopaedic surgeons.
- Traumatic spondylolisthesis: This type occurs with a fracture or acute dislocation of the zygapophyseal joint and is fairly rare.
- Pathologic spondylolisthesis: This type can result from a pathologic process causing a weakening of the pars, pedicle, or zygapophyseal joint.
- Acquired Spondylolisthesis: a sixth etiologic category, was added to represent the slip caused by the surgical disruption of ligaments, bone, and disk.
There are two prevailing theories as to the etiology of degenerative spondylolisthesis:
- Dysfunction of the inter-vertebral disc: The inter-vertebral disc at the level of the spondylolisthesis is subjected to considerable anteriorly directed shear forces and is the main structure that opposes these shear forces, functioning to prevent against further slippage and keeping the spinal motion segment in a stable equilibrium. It is postulated that slip progression after skeletal maturity is almost always related to inter-vertebral disc degeneration at the slip level. As the biochemical integrity of the inter-vertebral disc is lost, the lumbosacral slip becomes unstable and progresses. Disk degeneration at the slip level and adult slip progression are likely to develop during the fourth and fifth decades of life. This unstable mechanical situation leads to symptoms of low back and sciatic pain and may necessitate spinal instrumentation and fusion.
- Horizontalization of the lamina and the facets or sacrum morphology: A more trapezoidal shape of the vertebral body, or a dome-shaped contour of the top of the sacrum, or both, are found in individuals with slipping. There is also a greater anterior flexion of the lumbar spine than in A sagittal 500 individuals of comparable age. Normal orientation of the facet joints also could predispose the vertebra to slip.
Other factors such as the lumbosacral angle, ligamentous laxity, previous pregnancy, and hormonal factors impose an increased stress on the L4–5 facet joints, and, as most of the stress is placed anteriorly on the inferior facet of L4, the wear pattern is concentrated at this point, creating a more sagittally orientated joint by way of remodeling.
Grading
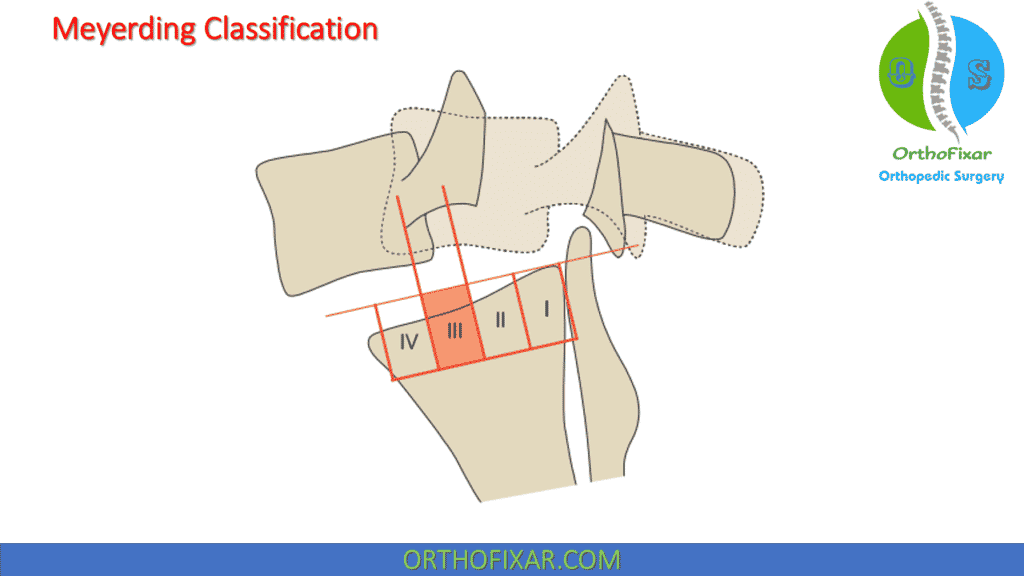
Spondylolisthesis is graded according to the percentage of slip. Slip percentage is the distance from a line extended along the posterior cortex of the S1 body to the posteroinferior corner of the L5 vertebra, divided by the anteroposterior diameter of the sacrum. Grading is then performed using the Meyerding classification as follows:
- Grade I: 1–25%;
- Grade II: 26–50%;
- Grade III: 51–75%;
- Grade IV: 76–100%;
- Grade V (spondyloptosis): more than 100%.
Radiology
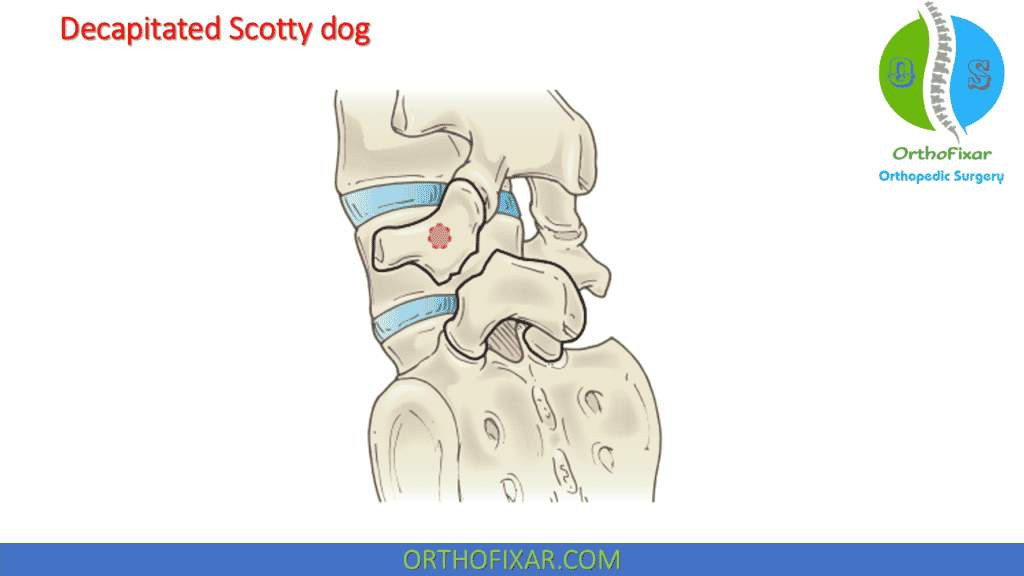
Radiographic examination of this condition reveals a “decapitated Scotty dog” deformity, in which the head of the dog, the anterior element of the vertebra, has become detached from the body, the posterior element . The severity of the spondylolisthesis is determined by the relative amount of anterior displacement of the vertebra.
After the fracture occurs, the displacement of the vertebra usually does not progress under the normal daily stresses. However, the stresses of sports and other exertive activities may increase the amount of anterior displacement. True healing of the fracture site rarely occurs.
Symptoms
There is often no correlation with the degree of slip and the level of symptoms, This is because the anterior slippage of the vertebral body usually results in intervertebral foramen enlargement initially.
Patients with spondylolisthesis have a history and physical presentation that is very similar to that of spondylolysis, with increased symptoms in postures that emphasize trunk extension. During AROM, the patient may reveal a “catch” when returning to upright from a flexed position. The pain may be more intense and is likely to be more constant.
The spectrum of neurologic involvement runs from rare to more common in the higher grade slips, with the majority of neurologic deficits being an L5 radiculopathy with a spondylolisthesis L5 S1, but cauda equina impairments can occur in grade III or IV slips.
On observation and with palpation of the spinous processes, an actual step-off deformity may be identified, as the normal continuity of the lumbar spine is lost when the vertebra shifts forward. Detecting anterior slippage via palpation has poor interrater reliability.
More severe cases result in a flattening of the buttocks when viewed laterally and more severe limitations in ROM. As with intervertebral disc pathologies, pain may be described in the lumbar region when the patient returns to a standing posture.
Results of selective tissue tests and neurological tests may become positive if the slippage of the vertebra is great enough to impinge on the neurological structures. Pain associated with spondylolysis and early stages of spondylolisthesis tends not to radiate. Although its diagnostic utility is questionable, the single-leg stance test may reinforce a suspicion of spondylolysis or spondylolisthesis.
Questions regarding bicycle use versus walking can help the clinician to differentiate neurogenic from vascular claudication. Both cycling and walking increase symptoms in vascular claudication due to the increased demand for blood supply. However, patients with neurogenic claudication worsen with walking but are unaffected by cycling due to the differing positions of the lumbar spine adopted in each of these activities. Patients with neurogenic claudication are far more comfortable leaning forward or sitting, which flexes the spine, than walking. The position of forward flexion increases the anteroposterior diameter of the canal, which allows a greater volume of the neural elements and improves the microcirculation. A check of distal pulses is important to rule out any coexisting vascular insufficiency.
See Also: Lasegue Test
Spondylolisthesis Treatment
The treatment for spondylolisthesis depends on the presenting symptoms, rather than the degree of slip, and ranges from conservative to surgical. Conservative treatment is more likely to be successful in the case of a limited slip and sparse clinical findings. Such an approach includes pelvic positioning initially to provide symptomatic relief, followed by physical therapy for spondylolisthesis with an active lumbar stabilization program, and stretching of the rectus femoris and iliopsoas muscles to decrease the degree of anterior pelvic tilting.
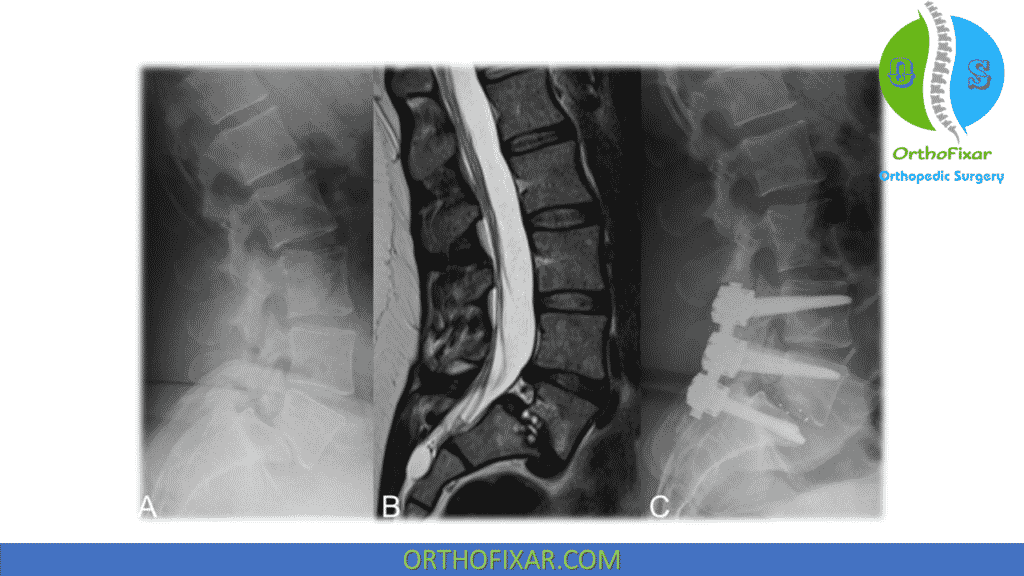
In those cases where conservative measures do not provide adequate relief, or the neurological signs and symptoms appear to be progressing, spondylolisthesis surgery may be required. During the past decade, numerous patients with lumbar degenerative spondylolisthesis have been treated with spinal decompression and fusion with or without instrumentation. A high fusion rate and satisfactory clinical outcome have been reported.
However, a few patients present with recurrent back pain and sciatica after surgery. The possible causes of postoperative pain include inadequate decompression, fibrosis, recurrent IVD herniation, adjacent stenosis. Ironically, another cause of postoperative pain is instability of those segments above and below the fusion site.
References
- Tallarico RA, Madom IA, Palumbo MA. Spondylolysis and spondylolisthesis in the athlete. Sports Med Arthrosc Rev. 2008 Mar;16(1):32-8. doi: 10.1097/JSA.0b013e318163be50. PMID: 18277260.
- Alfieri, A, et al: The current management of lumbar spondylolisthesis. J Neurosurg Sci, 57:103, 2013.
- Tertti, M, et al: Disc degeneration in young gymnasts: a magnetic resonance imaging study. Am J Sports Med, 18:206, 1990.
- Hicks, GE, et al: Preliminary development of a clinical prediction rule for determining which patients with low back pain will respond to a stabilization exercise program. Arch Phys Med Rehabil, 86:1753, 2005.
- McNeely ML, Torrance G, Magee DJ: A systematic review of physiotherapy for spondylolysis and spondylolisthesis. Man Ther 8:80–91, 2003.
- Spratt KF, Weinstein JN, Lehmann TR, et al: Efficacy of flexion and extension treatments incorporating braces for low-back pain patients with retrodisplacement, spondylolisthesis, or normal sagittal translation. Spine 18:1839–1849, 1993.
- Assendelft WJ, Morton SC, Yu EI, et al: Spinal manipulative therapy for low back pain. Cochrane Database Syst Rev 138:871–881, 2004.
- O’Sullivan P, Twomey L, Allison G: Evaluation of specific stabilizing exercise in the treatment of chronic low back pain with radiologic diagnosis of spondylolysis or spondylolisthesis. Spine 22:2959–2967, 1997.
- Seitsalo S, Osterman K, Hyvarinen H, et al: Progression of the spondylolisthesis in children and adolescents. Spine 16:417–421, 1991
- Friberg S: Studies on spondylolisthesis. Acta Chir Orthop 60:1, 1939.
- Bradford DS, Hu SS: Spondylolysis and spondylolisthesis. In: Weinstein SL, ed. The Pediatric Spine. Philadelphia, PA: Raven Press, 1994.
- Dandy DJ, Shannon MJ: Lumbosacral subluxation. J Bone Joint Surg 53B:578, 1971.
- Edelman B: Conservative treatment considered best course for spondylolisthesis. Orthop Today 9:6–8, 1989.
- Grobler LJ, Robertson PA, Novotny JE, et al: Etiology of spondylolisthesis: Assessment of the role played by lumbar facet joint morphology. Spine 18:80–91, 1993.
- Laus M, Tigani D, Alfonso C, et al: Degenerative spondylolisthesis: Lumbar stenosis and instability. Chir Organi Mov 77:39–49, 1992.
- Love TW, Fagan AB, Fraser RD: Degenerative spondylolisthesis: Developmental or acquired? J Bone Joint Surg 81B:670–674, 1999.
- Matsunaga S, Sakou T, Morizonon Y, et al: Natural history of degenerative spondylolisthesis: Pathogenesis and natural course of slippage. Spine 15:1204–1210, 1990.
- Newman PH: The etiology of spondylolisthesis. J Bone Joint Surg 45B:39–59, 1963.
- Postacchinia F, Perugia D: Degenerative lumbar spondylolisthesis. Part I: Etology, pathogenesis, pathomorphology, and clinical features. Ital J Orthop Traumatol 17:165–173, 1991.
- Rosenberg NJ: Degenerative spondylolisthesis. J Bone Joint Surg 57A:467–474, 1975.
- Meyerding HW: Spondylolisthesis. Surg Gynecol Obstet 54:371–377, 1932.
- Chen WJ, Lai PL, Niu CC, et al: Surgical treatment of adjacent instability after lumbar spine fusion. Spine 26:E519–E524, 2001.
- Cook C, Cook A, Fleming R: Rehabilitation for clinical lumbar instability in a female adolescent competitive diver with spondylolisthesis. J Man Manip Ther 12:91–99, 2004.