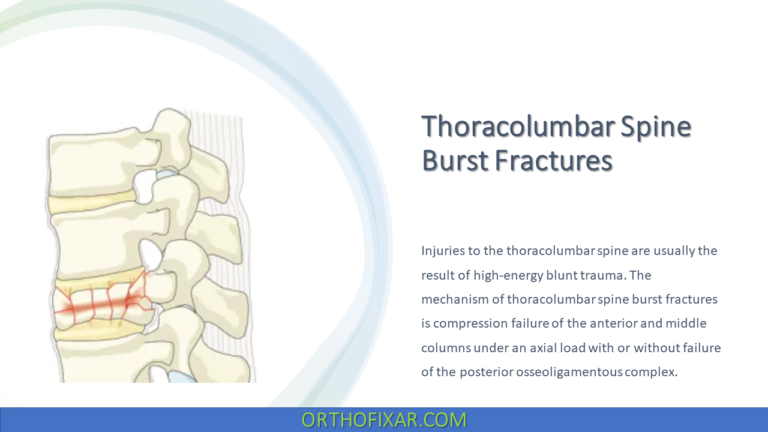
Spinal Spondylolysis is a defect in the pars interarticularis, the area of the vertebral arch between the inferior and superior articular facets, usually brought on by repetitive stress.
Bony disorders of the posterior elements of the spinal column, Spondylolysis and spondylopathies, are a common cause of persistent low back pain in young athletes and tend to be more prevalent in those who repeatedly hyperextend and rotate, or rotate their torso against resistance during activity.
The development of spondylolysis is general attributed to repetitive microtrauma and/or a genetic predisposition to thinner, weakened, or elongated pars interarticularis. Lumbar spondylytic defects are rarely caused by acute trauma. These defects are caused by repetitive forced hyperextension such as that experienced by football linemen, gymnasts, divers, and cheerleaders.
| Term | Description |
|---|---|
| Spondylalgia | Pain arising from the vertebrae |
| Spondylitis | Inflammation of the vertebrae |
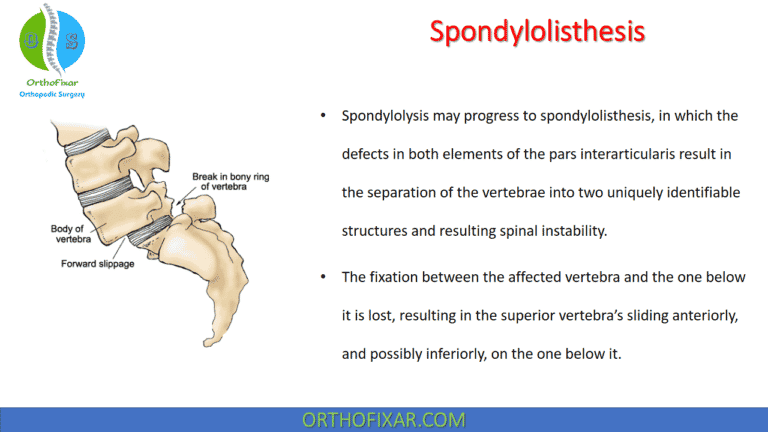
| Spondylolisthesis | Forward slippage of a vertebra on the one below it (may occur secondary to spondylolysis, in which the fracture of the pars interarticularis results in the anterior displacement of the vertebral body) |
| Spondylolysis | Degeneration of a vertebral structure secondary to repetitive stress, most commonly affecting the pars interarticularis but with no displacement of the vertebral body |
| Spondylopathy | Any disorder of the vertebrae |
| Spondylosis | Arthritis or osteoarthritis of the vertebrae; results in pressure being placed on the vertebral nerve roots |
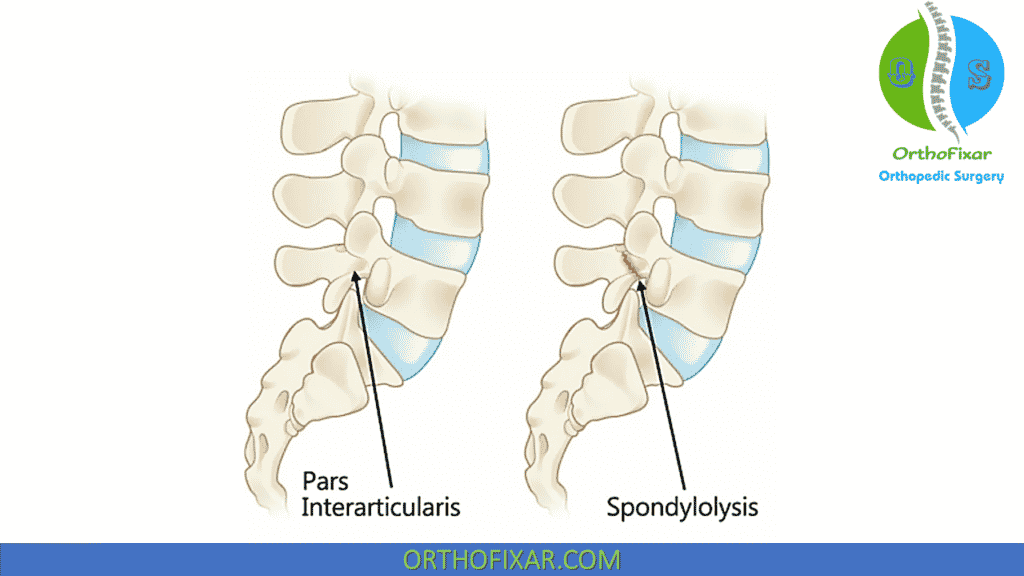
Spondylolysis can occur bilaterally or unilaterally. Bilateral Spondylolysis defects in the pars interarticularis result in listhesis. The anterosuperior segment, consisting of the vertebral body, pedicles, and transverse processes, separates from the posteroinferior segment, consisting of the laminae, inferior articular processes, and spinous processes.
The exact cause of spinal spondylolysis is unknown, but it is likely related to congenital, acquired (repeated microtrauma), or developmental causes.
Radiology
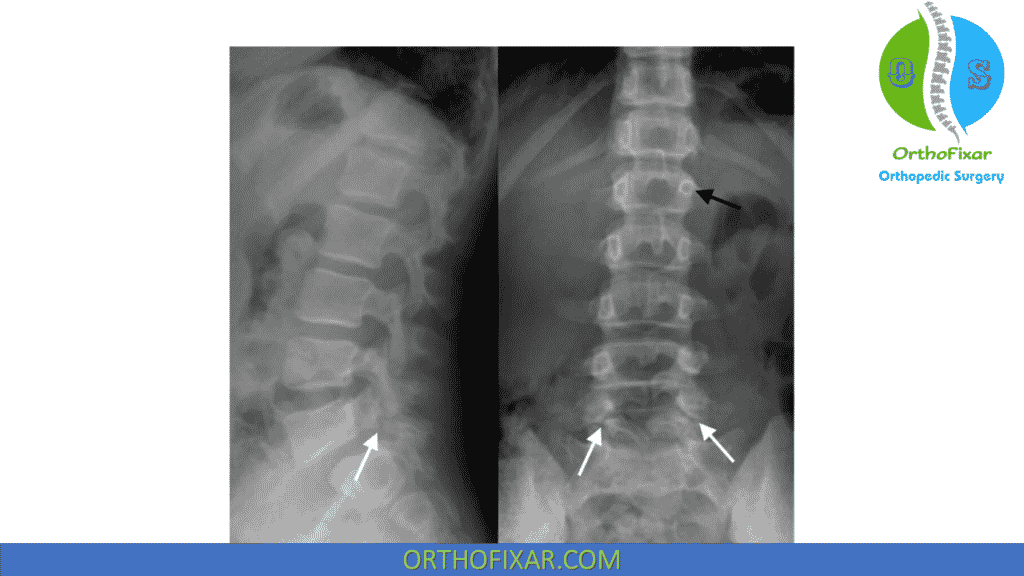
Patients with suspected spinal spondylolysis should be evaluated initially with plain radiography, consisting of anteroposterior, lateral, and oblique views of the lumbar spine. The lateral views are most sensitive for detection of pars fractures, and the oblique views are the most specific.
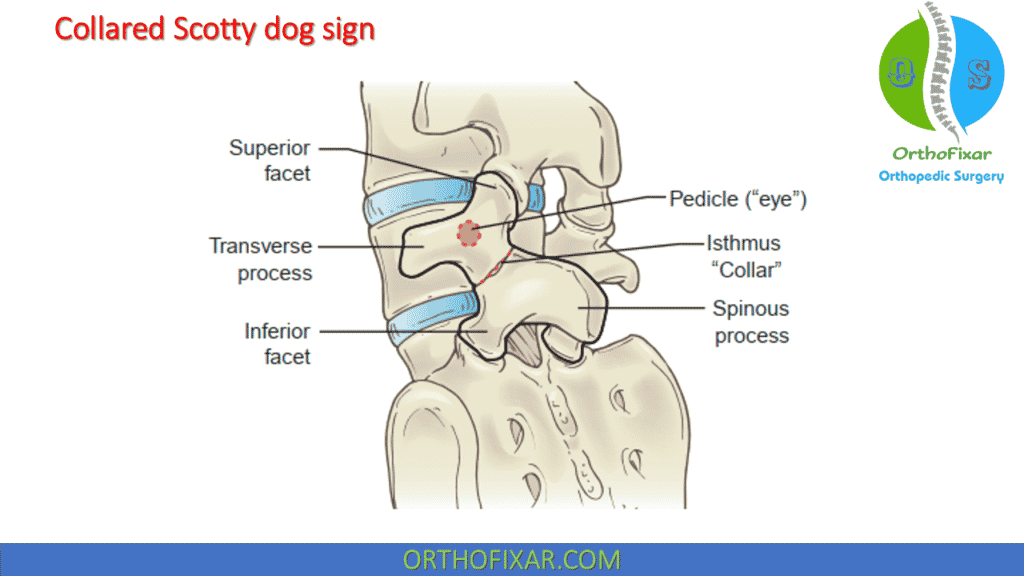
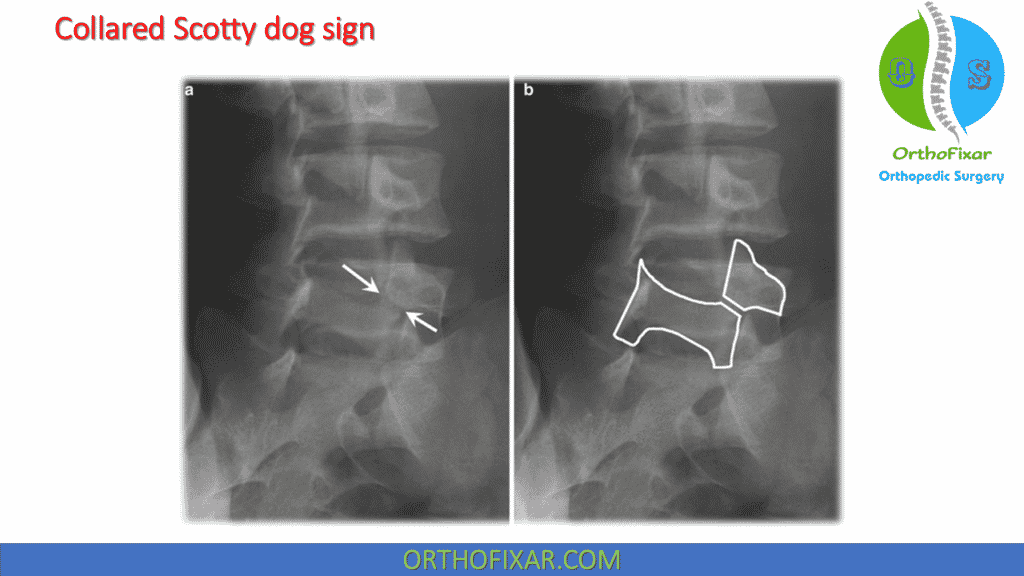
This defect, when seen on an oblique radiographic view, appears as a “collared Scotty dog” deformity, with the area of the stress fracture representing the dog’s collar.
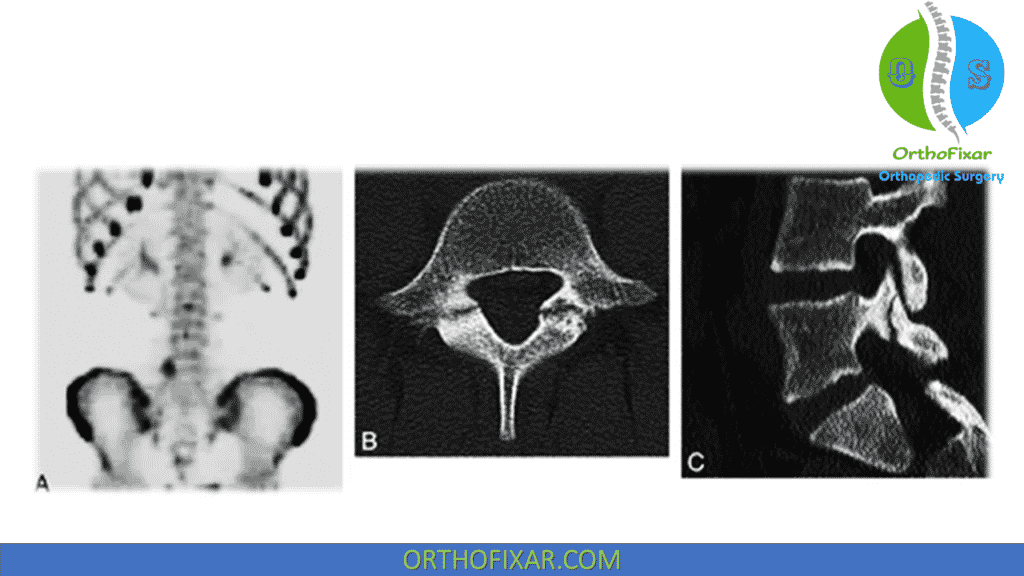
Defects in the pars are a common radiological finding in individuals with no symptoms, so CT scans are used to determine whether or not the fracture site is metabolically active. Radiographs may show a flattening of the inferior facet on the vertebra above the affected site.
CT scans have slightly higher sensitivity than bone scans with less radiation exposure.
MRI may be helpful to detect early cases that is not detectable on standard radiographs.
See Also: Spondylolisthesis: Causes, Symptoms and Treatment
Spinal Spondylosis Symptoms
The patient with lumbar spondylolysis presents with localized low back pain that is increased during and after activity but decreases with rest.
During observation, spinal alignment is usually normal. Those with spondylotic defects typically describe a pattern where extension (e.g., standing and walking) is aggravating and symptoms are alleviated with postures or activities that incorporate more flexion (e.g., sitting).
Active ROM is normal for flexion, but pain restricts extension. Results of selective tissue tests and neurological tests are normal. The evaluative findings of advanced spondylolysis resemble those of spondylolisthesis.
Spondylolysis Treatment
The initial Spondylolysis Treatment is conservative. In a meta-analysis performed by McNeely et al, the efficacy of physical therapist intervention in the treatment of spondylolysis and spondylolisthesis was systematically reviewed. Of the 71 potential studies, only two of the studies met the relevance criteria of the critical appraisal.
Spratt et al. examined the efficacy of trunk extension and flexion treatment programs on 56 patients with radiographic instability (retrodisplacement or spondylolisthesis). Subjects were randomly assigned to one of three groups: a flexion, an extension, or a control group. The flexion and extension groups performed exercises biased into flexion or extension, respectively. At the 1-month follow-up, no treatments were shown to alter ROM or trunk strength. However, patients in the extension group reported less pain, as compared with patients in the flexion and control groups.
In a study by O’Sullivan et al., 45 subjects with spondylolysis or spondylolisthesis were divided into two groups: a group that underwent 10 weeks of rehabilitation, with a focus on training of the deep abdominal muscles, and a control group that underwent treatment as directed by their treating practitioner. The group that underwent specific abdominal exercise training had a reduction in pain and disability levels, which was maintained at a 30-month follow-up. The control group showed no significant change throughout the study.
Based on these studies, the physical therapy intervention should strive to correct any muscle imbalances (adaptively shortened hip flexors), increase trunk muscle strength, and educate the patient to avoid activities involving excessive impact and activities involving lumbar hyperextension. Bracing may also be advocated.
Spondylolysis surgery is indicated only after patients have failed conservative management.
References
- Thein-Nissenbaum J, Boissonnault WG. Differential diagnosis of spondylolysis in a patient with chronic low back pain. J Orthop Sports Phys Ther. 2005 May;35(5):319-26. doi: 10.2519/jospt.2005.35.5.319. PMID: 15966543.
- Sairyo K, Katoh S, Takata Y, et al: MRI signal changes of the pedicle as an indicator for early diagnosis of spondylolysis in children and adolescents: A clinical and biomechanical study. Spine 31:206–211, 2006.
- Cassidy RC, Shaffer WO, Johnson DL: Spondylolysis and spondylolisthesis in the athlete. Orthopedics 28:1331–1333, 2005.
- Hicks, GE, et al: Preliminary development of a clinical prediction rule for determining which patients with low back pain will respond to a stabilization exercise program. Arch Phys Med Rehabil, 86:1753, 2005.
- Congeni, J, McCulloch, J, and Swanson, K: Lumbar spondylolysis: a study of natural progression in athletes. Am J Sports Med, 25:248, 1997.
- Soler, T, and Calderón, C: The prevalence of spondylolysis in the Spanish elite athlete. Am J Sports Med, 28:57, 2000.
- Moore, KL: The perineum and pelvis. In Moore, KL (ed): Clinically Oriented Anatomy, ed 5. Baltimore, MD: Williams & Wilkins, 2005, p 389.
- O’Sullivan P, Twomey L, Allison G: Evaluation of specific stabilizing exercise in the treatment of chronic low back pain with radiologic diagnosis of spondylolysis or spondylolisthesis. Spine 22:2959–2967, 1997.
- McNeely ML, Torrance G, Magee DJ: A systematic review of physiotherapy for spondylolysis and spondylolisthesis. Man Ther 8:80–91, 2003.
- Spratt KF, Weinstein JN, Lehmann TR, et al: Efficacy of flexion and extension treatments incorporating braces for low-back pain patients with retrodisplacement, spondylolisthesis, or normal sagittal translation.