Pronator Teres Syndrome (PTS) is a compression of the median nerve in the arm/ forearm. It’s more common in women in the fifth decade of life.
Pronator syndrome differentiated from Carapal Tunnel Syndrome CTS by proximal volar forearm pain and sensory disturbances in distribution of palmar cutaneous branch of the median nerve.
See Also: Carapal Tunnel Syndrome
Related Anatomy
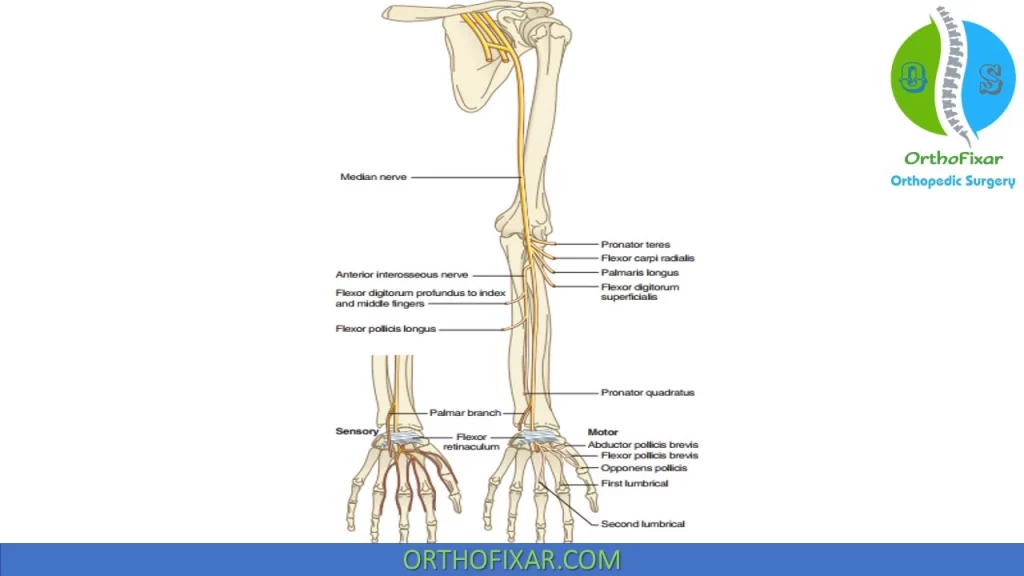
Median Nerve
The median nerve arises from the medial and lateral cords, (C5-T1). It accompanies brachial artery in the arm, crossing it during its course (lateral to medial) approximately 15 cm from the medial epicondyle.
It Supplies some branches to the elbow joint but has no branches in the arm itself.
In forearm, the median nerve splits the two heads of the pronator teres and then runs between the FDS and FDP. Supplies all the superficial flexor muscles of the forearm except the FCU.
Anterior interosseous nerve branches 4 cm distal to elbow and runs between the FPL and FDP, supplies all the deep flexors except the ulnar half of the FDP. Terminates in the pronator quadratus (PQ).
Palmar cutaneous branch arises approximately 6 cm proximal to radial styloid and passes superficial to the flexor retinaculum to innervate the thenar skin.
Median nerve passes through the carpal tunnel between FDS and flexor carpi radialis (FCR) to supply the radial lumbricals, thenar musculature via a deep recurrent branch, and sensation to the volar aspect of thumb, index, long, and radial half of the ring fingers.
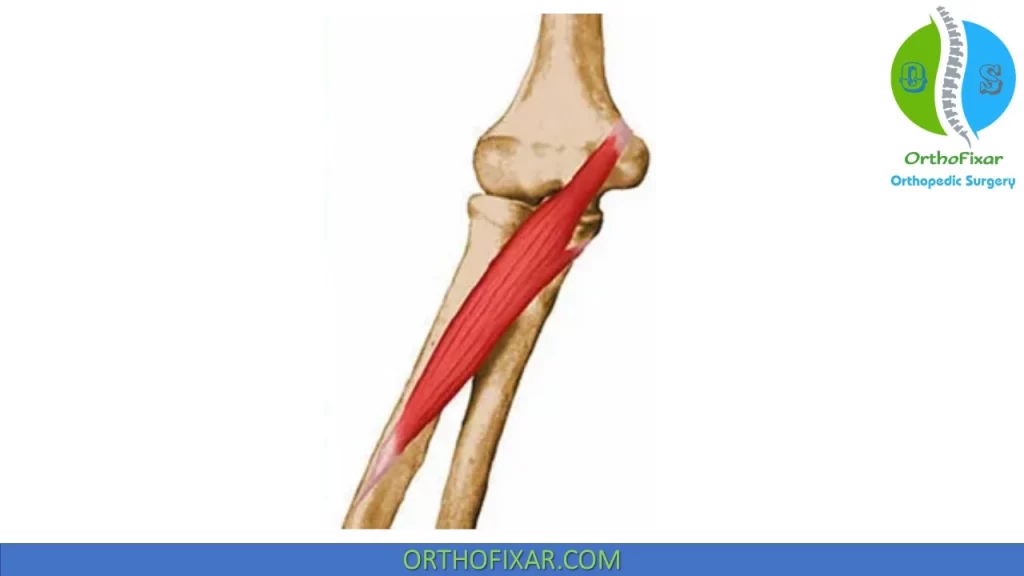
Pronator Teres Muscle
Pronator Teres Muscle is one of the superficial flexors of the forearm.
It’s origin is from the medial epicondyle and coronoid, and inserts onto the midlateral radius.
Its action includes Pronating and flexing theforearm.
It’s innervated by the Median nerve.
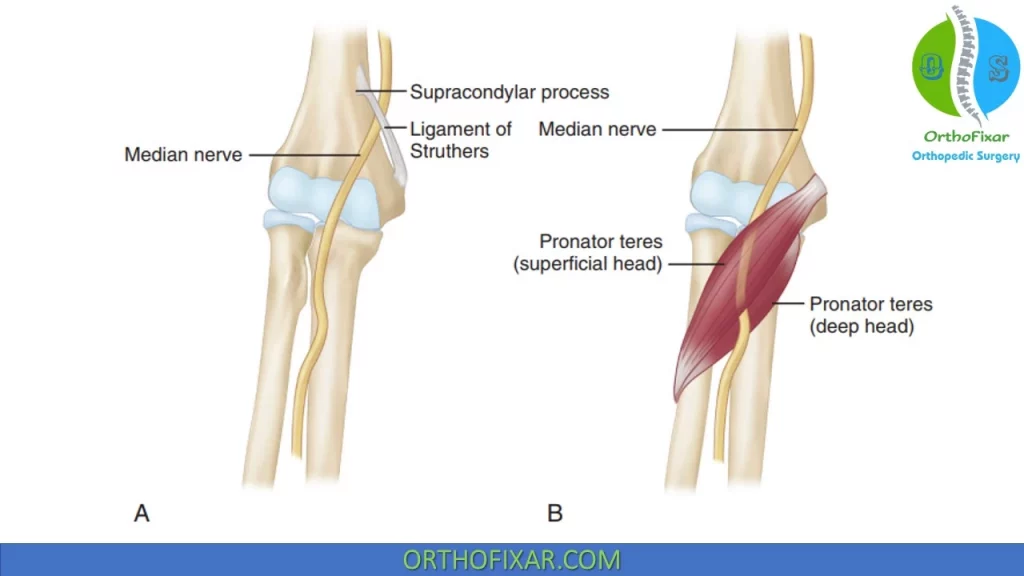
Sites of Compression
Potential site of compression of median nerve in case of pronator teres syndrome include:
- Supracondylar process (anterior distal humerus seen on lateral radiograph), occurs in approximately 1% of the population.
- Ligament of Struthers (courses between the supracondylar process and medial epicondyle).
- Bicipital aponeurosis (lacertus fibrosis).
- Between the two heads of pronator teres muscle.
- FDS aponeurotic arch.
The lacertus fibrosis is an aponeurosis layer of the distal biceps, coursing obliquely in a distal and medial orientation.
The most proximal site at which the median nerve can be compressed is in the distal arm by the ligament of Struthers, an anatomic variant present in 0.7–2.7% of the population.

Symptoms & Signs
The patient typically complains of an insidious onset of pain that is usually felt on the anterior aspect of the elbow, radial side of the palm, and the palmar side of the first, second, third, and half of the fourth digits.
There is often associated “heaviness” of the forearm.
Unlike CTS, there is no Tinel’s sign at the wrist, and there are no nocturnal symptoms.
Pain can be reproduced with:
- Pressure applied over the pronator teres 4 cm distal to the cubital crease with concurrent resistance against pronation,
elbow flexion, and wrist flexion; - Resisted supination (due to compression of the lacertus fibrosus);
- Resistance of the long finger flexors (due to compression by the FDS arch).
See Also: Durkan Test
Diagnosis of Pronator Syndrome is confirmed electromyographically with EMG.

Pronator Syndrome Treatment
Pronator Teres Syndrome typically responds well to conservative treatment:
- Activity modification (removing the causative activity),
- Rest,
- NSAIDs,
- Ice application,
- The restoration of proper flexibility and strength of the wrist flexors and forearm pronators.
Rehabilitation will most benefit those cases in which compression is related to medial elbow tendinosis. In these cases, gentle massage along the fibers may aid in the breaking of adhesions.
When nonoperative management fails, surgery must address all potential sites of compression, success rate approximately 80% in most series.
References
- Vennix MJ, Wertsch JJ. Entrapment Neuropathies about the Elbow. J Back Musculoskelet Rehabil. 1994 Jan 1;4(1):31-43. doi: 10.3233/BMR-1994-4108. PMID: 24571994.
- Lubahn JD, Cermak MB. Uncommon nerve compression syndromes of the upper extremity. J Am Acad Orthop Surg. 1998 Nov-Dec;6(6):378-86. doi: 10.5435/00124635-199811000-00006. PMID: 9826421.
- Werner CO, Rosén I, Thorngren KG. Clinical and neurophysiologic characteristics of the pronator syndrome. Clin Orthop Relat Res. 1985 Jul-Aug;(197):231-6. PMID: 4017339.
- Gainor BJ. The pronator compression test revisited. A forgotten physical sign. Orthop Rev. 1990 Oct;19(10):888-92. PMID: 2250993.
- Spinner M, Linscheid RL: Nerve entrapment syndromes. In: Morrey BF, ed. The Elbow and Its Disorders. Philadelphia, PA: Saunders, 1985:691– 712.
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.
- Millers Review of Orthopaedics -7th Edition Book.