Pediatric supracondylar humerus fractures are the most common elbow fractures in children and represent an orthopedic emergency because of the potential for neurovascular compromise and compartment syndrome. These injuries account for approximately 55% to 75% of all pediatric elbow fractures and occur most frequently in children between 5 and 8 years of age.
The injury typically follows a fall onto an outstretched hand (FOOSH), producing hyperextension at the elbow. Early recognition and appropriate management are essential to prevent long-term complications such as cubitus varus deformity, nerve injury, and Volkmann ischemic contracture.
Epidemiology
Pediatric supracondylar humerus fractures have several characteristic epidemiologic features:
- Represent 55%–75% of elbow fractures in children
- Male-to-female ratio: approximately 3:2
- Peak incidence: 5–8 years
- The left (nondominant) arm is injured more commonly
- Extension-type fractures account for nearly 98% of cases
- Flexion-type fractures comprise approximately 2%
These fractures become less common after 8 years of age as elbow dislocations become more frequent.
Relevant Anatomy
The distal humerus in children has unique anatomic characteristics that predispose it to supracondylar injury.
Important Anatomic Features
Decreased AP Diameter
During skeletal remodeling between ages 5 and 8 years, the supracondylar region develops a relatively thin anteroposterior (AP) diameter, making it structurally weak.
Ligamentous Laxity
Children in this age group demonstrate increased ligamentous laxity, which predisposes the elbow to hyperextension injuries.
Capsular Anatomy
- The anterior capsule is thicker and stronger than the posterior capsule.
- During forced hyperextension, the olecranon engages the olecranon fossa and acts as a fulcrum.
- Excessive force may cause failure through the supracondylar region.
Periosteal Hinge
The periosteum usually remains intact on the side opposite displacement:
- Posteromedial displacement → intact medial hinge
- Posterolateral displacement → intact lateral hinge
This principle is important during reduction maneuvers.
See Also: Elbow Joint Anatomy
Mechanism of Injury
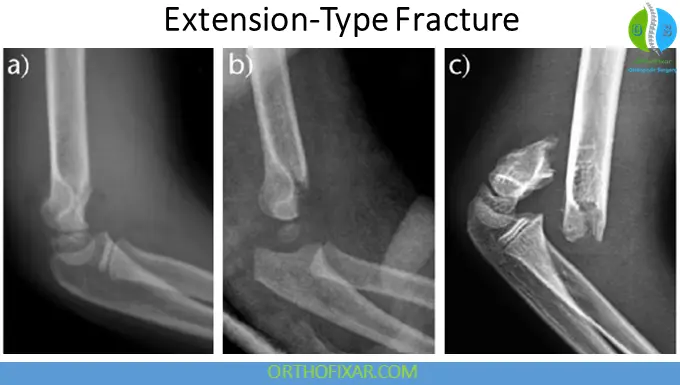
Extension-Type Fractures
These are the overwhelming majority of pediatric supracondylar fractures.
Mechanism
- Fall onto an outstretched hand
- Elbow hyperextension
- May occur with varus or valgus stress
Direction of Displacement
- Pronated hand → posteromedial displacement
- Supinated hand → posterolateral displacement
Posteromedial displacement is more common.
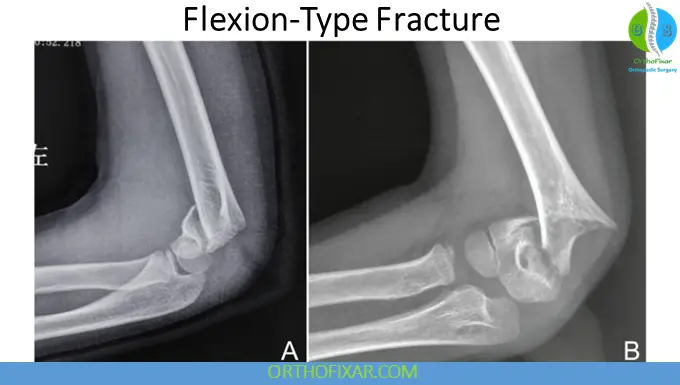
Flexion-Type Fractures
These are uncommon injuries.
Mechanism
- Direct trauma to the posterior elbow
- Fall onto a flexed elbow
Clinical Presentation
Common Symptoms and Signs
Children with Supracondylar Humerus Fractures usually present with:
- Severe elbow pain
- Swelling
- Tenderness
- Limited range of motion
- Refusal to use the arm
S-Shaped Deformity
Complete displaced fractures (Gartland III) may produce:
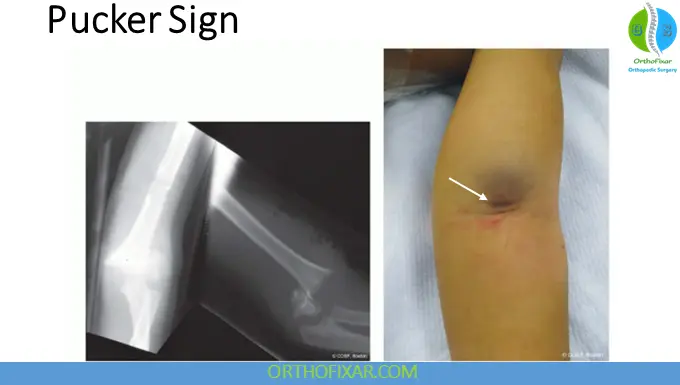
Pucker Sign
The pucker sign refers to anterior skin dimpling caused by penetration of the proximal fragment into the brachialis muscle.
This finding suggests:
- Significant displacement
- Difficult closed reduction
- Increased soft tissue interposition
Neurovascular Examination
A meticulous neurovascular assessment is mandatory both before and after reduction or splinting.
Nerves to Assess
Median Nerve / Anterior Interosseous Nerve (AIN)
Most commonly injured.
AIN testing:
- Ask child to make an “OK” sign
- Inability suggests AIN palsy
Radial Nerve
Assess:
- Wrist extension
- Thumb extension
Ulnar Nerve
Assess:
- Finger abduction
- Sensation over little finger
Vascular Examination
Document:
- Radial pulse
- Capillary refill
- Skin temperature
- Hand perfusion
A pulseless but well-perfused hand may be observed carefully after reduction.
Classification of Supracondylar Humerus Fractures
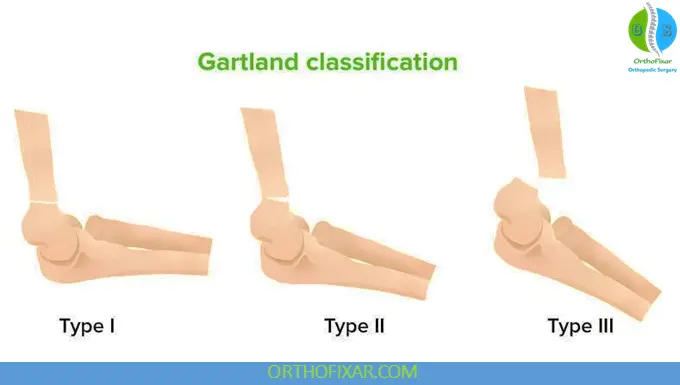
Gartland Classification
The Gartland system is based on degree of displacement.
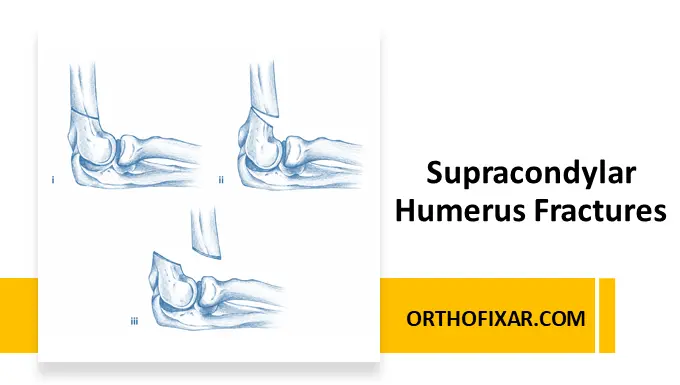
Extension-Type Classification
Type I
- Nondisplaced fracture
Type II
- Displaced fracture
- Posterior cortex intact
- May show angulation or rotation
Type III
- Completely displaced fracture
- Posteromedial or posterolateral displacement
Flexion-Type Classification
Type I
- Nondisplaced
Type II
- Displaced with intact anterior cortex
Type III
- Completely displaced
- Usually anterolateral displacement
Radiographic Evaluation
Standard Imaging
Radiographs should include:
- AP view
- Lateral view of the elbow
Important Radiographic Signs
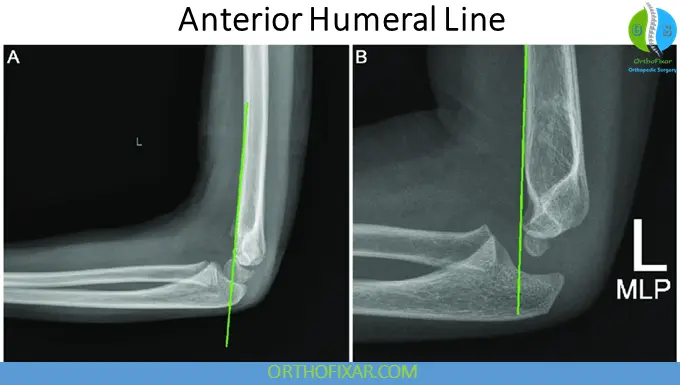
Anterior Humeral Line
Normally intersects the middle third of the capitellum on the lateral view.
Failure to intersect appropriately suggests displacement.
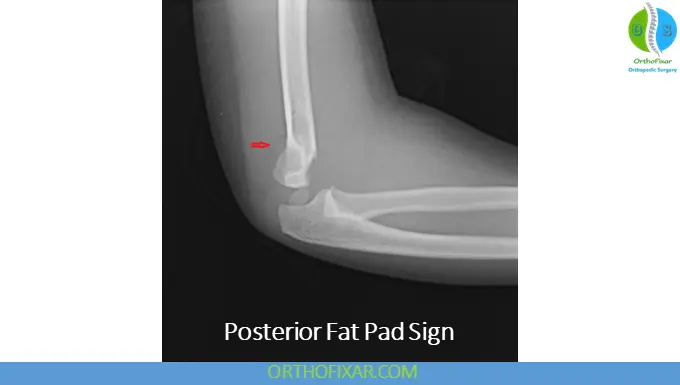
Fat Pad Sign
- Posterior fat pad visibility is abnormal
- Indicates elbow effusion and occult fracture
Baumann Angle
Used to evaluate coronal alignment after reduction.
See Also: Elbow X-Ray Views
Treatment of Pediatric Supracondylar Humerus Fractures
General Principles
Goals of Supracondylar Humerus Fractures treatment include:
- Restoration of alignment
- Prevention of neurovascular injury
- Maintenance of elbow motion
- Prevention of deformity
Treatment of Extension-Type Fractures
Type I Fractures
- Long-arm cast or splint
- Elbow flexed 60–90 degrees
- Immobilization for 2–3 weeks
Prognosis
Excellent outcomes are typical.
Type II Fractures
Usually treated with:
- Closed reduction
- Casting
Percutaneous pinning may be needed if:
- Reduction is unstable
- Excessive elbow flexion is required to maintain reduction
- Neurovascular compromise is a concern
Type III Fractures
- Closed reduction
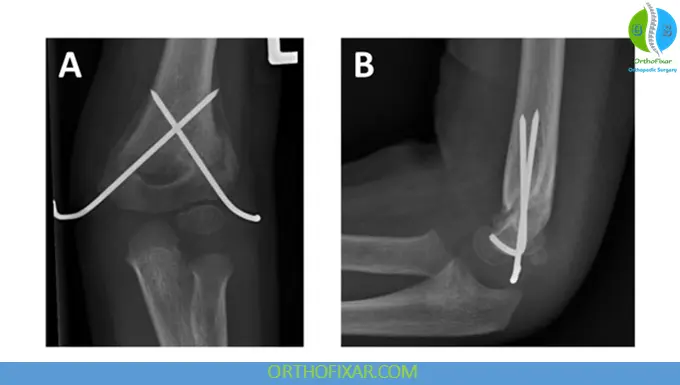
- Percutaneous pin fixation (CRPP)
Open Reduction Indications
- Open fractures
- Vascular injury
- Irreducible fractures
- Rotational instability
Rare Indications for Traction
- Severe comminution
- Significant soft tissue swelling
Reduction Technique Concepts
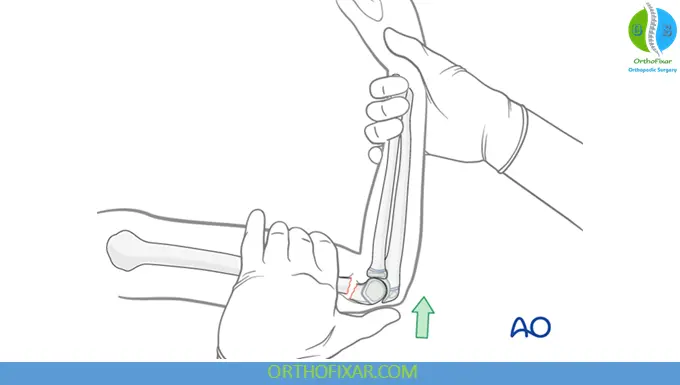
Step 1: Traction
Longitudinal traction restores length.
Step 2: Coronal and Rotational Correction
Displacement in coronal and horizontal planes corrected first.
Step 3: Sagittal Correction
Elbow flexion with posterior pressure on distal fragment.
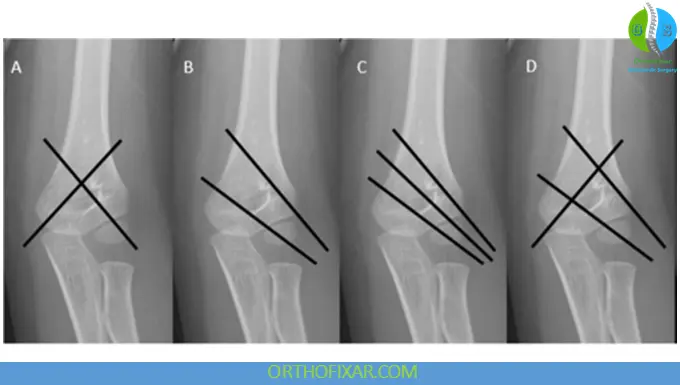
Step 4: Pin Stabilization
- Lateral pins placed first
- Medial pin added if necessary
- Elbow extension during medial pin placement reduces ulnar nerve risk
Treatment of Flexion-Type Fractures
Type I
- Long-arm cast
- Near extension
- 2–3 weeks
Type II
- Closed reduction
- Percutaneous fixation
Type III
- Frequently require open reduction
- Followed by pin fixation
Postoperative Care
Typical postoperative protocol includes:
- Long-arm cast or posterior splint
- Elbow flexion less than 90°
- Forearm neutral position
- Immobilization for approximately 3 weeks
After pin removal:
- Sling protection
- Active range-of-motion exercises
- Avoid sports for an additional 3 weeks
Complications
Neurologic Injury (7%–10%)
Most injuries are neurapraxias and recover spontaneously.
Most Common Nerve Injuries
Ulnar Nerve Injury
More common in:
- Flexion-type fractures
- Medial pin placement
Vascular Injury (0.5%)
May involve:
- Brachial artery injury
- Compression from swelling
A pulseless but perfused hand requires close observation.
Compartment Syndrome
Occurs in less than 1% of Supracondylar Humerus Fractures cases but is limb-threatening.
Risk factors:
- Excessive swelling
- Hyperflexion immobilization
Warning Signs
- Increasing pain
- Pain with passive stretch
- Anxiety or agitation in children
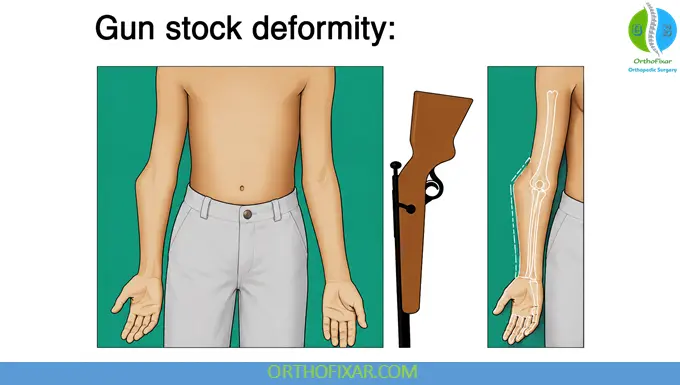
Cubitus Varus (“Gunstock Deformity”)
Most common angular deformity.
Usually caused by:
- Malreduction
- Coronal plane collapse
Risk reduced with percutaneous pinning.
Loss of Motion
Can result from:
- Poor reduction
- Soft tissue contracture
More than 5° motion loss occurs in approximately 5% of patients.
Myositis Ossificans
Rare complication associated with:
- Vigorous manipulation
- Repeated reduction attempts
Prognosis
Most children with Supracondylar Humerus Fractures achieve excellent functional outcomes with:
- Prompt diagnosis
- Proper reduction
- Stable fixation
- Appropriate rehabilitation
Neuropraxias generally recover completely within weeks to months.
Key Clinical Pearls
- Pediatric supracondylar humerus fractures are the most common pediatric elbow fractures.
- Extension-type injuries account for approximately 98% of cases.
- Always perform and document a detailed neurovascular examination.
- Gartland classification guides management.
- Type III fractures usually require urgent closed reduction and pinning.
- Watch carefully for compartment syndrome and vascular compromise.
- Cubitus varus is the most common late deformity.
Frequently Asked Questions (FAQs)
What is the most common complication of pediatric supracondylar humerus fractures?
Neurologic injury is the most common complication, particularly involving the median nerve or anterior interosseous nerve.
Which Gartland type usually requires surgery?
Gartland Type III fractures generally require closed reduction and percutaneous pin fixation.
What is the “pucker sign”?
It is anterior skin dimpling caused by soft tissue entrapment and severe displacement.
What causes cubitus varus deformity?
Malunion and coronal plane malalignment are the primary causes.
Conclusion
Pediatric supracondylar humerus fractures are common injuries with potentially serious neurovascular complications. Understanding the anatomy, injury mechanisms, Gartland classification, and evidence-based treatment principles is essential for optimal outcomes. Early recognition, meticulous neurovascular assessment, and appropriate stabilization significantly reduce the risk of long-term disability.
References & More
- Hope N, Varacallo MA. Supracondylar Humerus Fractures. [Updated 2023 Aug 4]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Li Y, Wei S, Canavese F, Liu Y, Li J, Liu Y, Xu H. Treatment and Outcome of Supracondylar Humeral Fractures in Children Over 10 Years of Age at the Time of Injury: A Review of 60 Cases. J Pediatr Orthop. 2024 Aug 1;44(7):e580-e587. doi: 10.1097/BPO.0000000000002710. Epub 2024 Apr 29. PMID: 38676464. Pubmed
- Hope N, Varacallo MA. Supracondylar Humerus Fractures. 2023 Aug 4. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan–. PMID: 32809768. Pubmed
- Li, WC., Meng, QX., Xu, RJ. et al. Biomechanical analysis between Orthofix® external fixator and different K-wire configurations for pediatric supracondylar humerus fractures. J Orthop Surg Res 13, 188 (2018). https://doi.org/10.1186/s13018-018-0893-z
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.