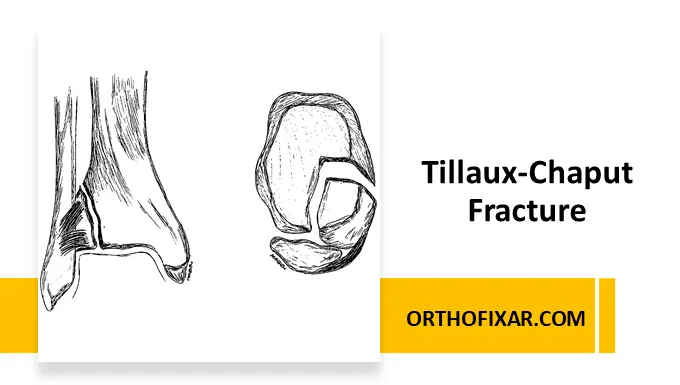
A Tillaux-Chaput fracture is an avulsion fracture involving the anterolateral distal tibia at the attachment of the anterior inferior tibiofibular ligament (AITFL). In adolescents, this injury is commonly referred to as a juvenile Tillaux fracture, a Salter-Harris type III physeal injury. In adults, the injury is rarer and usually associated with syndesmotic ankle trauma.
This fracture is clinically important because it is intra-articular and may lead to post-traumatic ankle arthritis if articular congruity is not restored.
What is a Tillaux-Chaput Fracture?
The Tillaux-Chaput fragment represents the anterolateral tibial tubercle (Chaput tubercle) where the AITFL inserts. An external rotational force applied to the ankle may avulse this fragment.
In adolescents, the fracture occurs during the transitional period of physeal closure when the distal tibial physis closes asymmetrically. Because the lateral physis closes last, rotational forces preferentially create a Salter-Harris III fracture through the anterolateral epiphysis.
See Also: Ankle Fractures: Classification, Diagnosis & Treatment
Epidemiology
- Represents approximately 2.9% of juvenile epiphyseal injuries
- Most common in adolescents nearing skeletal maturity
- More frequent in females because distal tibial physeal closure occurs earlier
- Often associated with sports injuries and twisting ankle trauma
- Adult Tillaux-Chaput fractures are uncommon but may accompany syndesmotic or malleolar injuries.
Relevant Anatomy
The injury involves:
- Distal tibial epiphysis
- Chaput tubercle
- Anterior inferior tibiofibular ligament (AITFL)
- Syndesmotic complex
The distal tibial physis closes in a predictable order:
- Central
- Medial
- Posteromedial
- Lateral (last)
This asymmetric closure explains the characteristic fracture pattern in adolescents.
See Also: Ankle Anatomy
Mechanism of Injury
The classic mechanism of Tillaux-Chaput Fracture is:
- Supination-external rotation injury
- External rotation of the foot relative to the leg
- AITFL traction avulses the anterolateral distal tibial fragment
Common causes include:
- Sports injuries
- Skateboarding accidents
- Falls
- Twisting ankle injuries
Because symptoms mimic ankle sprains, these fractures are frequently missed initially.
Classification
Juvenile Tillaux-Chaput Fracture:
This is classified as Salter-Harris Type III Fracture
Features:
- Fracture extends through the epiphysis into the ankle joint
- Involves partially closed distal tibial physis
- Usually isolated to the anterolateral distal tibia
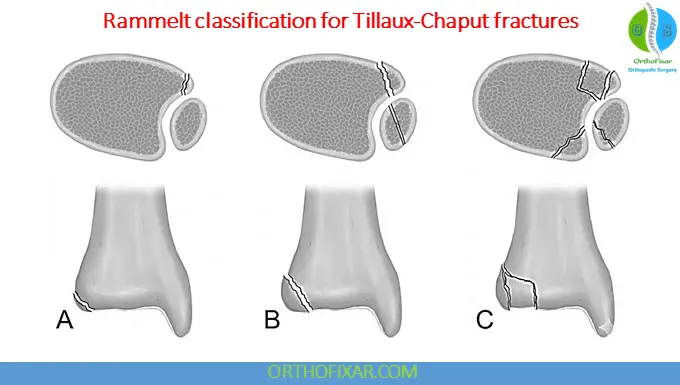
Rammelt classification for Tillaux-Chaput fractures
- Type 1: extra-articular avulsion.
- Type 2: fracture with involvement of the joint and incisura.
- Type 3: fracture with impaction of the anterolateral tibial plafond.
Clinical Presentation
Patients typically present with:
- Anterolateral ankle pain
- Swelling
- Difficulty weight-bearing
- Tenderness over the distal tibia
- Limited ankle motion
- Joint effusion or hemarthrosis
The presentation often resembles a severe ankle sprain.
Diagnosis
Plain Radiographs
Initial imaging includes:
- AP ankle view
- Lateral view
- Mortise view
Findings may include:
- Anterolateral epiphyseal fragment
- Physeal widening
- Intra-articular extension
However, small fragments are commonly missed on radiographs.
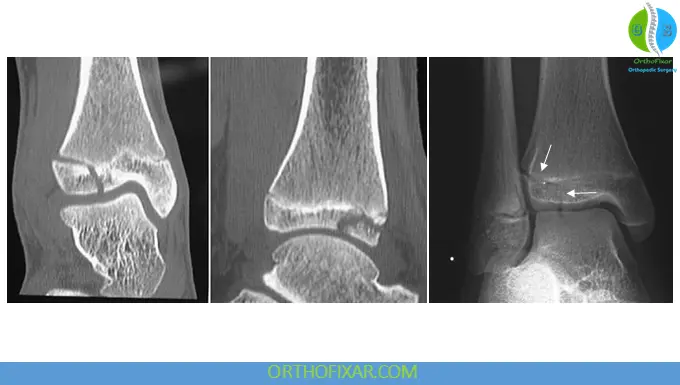
Role of CT Scan
CT is considered the best imaging modality for:
- Measuring displacement
- Assessing articular congruity
- Surgical planning
CT can detect displacement as small as: 2mm
Recent studies showed many adult Tillaux-Chaput fractures are not identified on standard radiographs alone.
Differential Diagnosis
Important differentials include:
- Lateral ankle sprain
- Triplane fracture
- Distal fibular fracture
- Syndesmotic injury
- Osteochondral talar lesion
Tillaux-Chaput Fracture Treatment
The primary treatment goal is anatomical reduction of the articular surface. Even minimal residual displacement may predispose patients to arthritis.
Nonoperative Management
Indications:
- Displacement less than: 2mm
Management includes:
- Closed reduction
- Short-leg cast
- Non-weight-bearing for approximately 4 weeks
- Transition to walking boot and rehabilitation
Reduction is often achieved using internal rotation maneuvers.
Operative Management
Indications:
- Displacement greater than:
Surgical options:
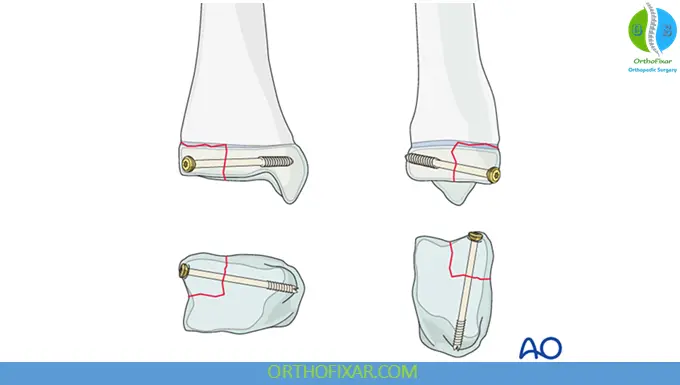
- Open reduction internal fixation (ORIF)
- Percutaneous screw fixation
- Arthroscopically assisted reduction
Fixation methods:
- Cannulated screws
- K-wires
ORIF allows direct visualization of the articular surface and restoration of ankle congruity.
Rehabilitation
Postoperative rehabilitation typically includes:
- Immobilization for 4–6 weeks
- Progressive range-of-motion exercises
- Gradual weight-bearing
- Strengthening and proprioceptive training
Return to sports generally occurs after radiographic healing and restoration of ankle function.
Complications
Potential complications include:
- Post-traumatic ankle arthritis
- Malunion
- Nonunion
- Chronic ankle pain
- Ankle stiffness
- Syndesmotic instability
- Premature physeal closure (rare)
Failure to restore joint congruity significantly increases the risk of degenerative arthritis.
Prognosis
The prognosis is generally excellent when:
- Diagnosis is early
- Anatomical reduction is achieved
- Articular congruity is restored
Most patients regain full ankle function and return to previous activity levels.
Key Clinical Pearls
- Tillaux-Chaput fractures are often mistaken for ankle sprains
- CT imaging is highly valuable for evaluating displacement
- Displacement greater than 2 mm usually requires surgery
- Anatomical reduction is critical to prevent arthritis
- Juvenile Tillaux fractures are Salter-Harris III injuries
Frequently Asked Questions (FAQ)
Is a Tillaux-Chaput fracture the same as a Tillaux fracture?
Yes. In adolescents, the term “Tillaux fracture” commonly refers to avulsion of the Chaput tubercle caused by AITFL traction.
Why are Tillaux-Chaput fractures common in adolescents?
Because the distal tibial physis closes asymmetrically, leaving the anterolateral portion vulnerable to rotational injury.
When is surgery needed?
Surgery is generally recommended when displacement exceeds 2 mm or when articular congruity cannot be restored by closed reduction.
Can Tillaux-Chaput fractures cause arthritis?
Yes. Poor reduction of the articular surface can lead to early post-traumatic ankle arthritis.
Conclusion
The Tillaux-Chaput fracture is an important transitional ankle injury involving the anterolateral distal tibia and syndesmotic attachment. Although uncommon, especially in adults, it carries significant implications because of its intra-articular nature. Early recognition, advanced imaging with CT, and restoration of anatomical alignment are essential for optimal outcomes and prevention of long-term ankle degeneration.
References
- Habusta SF, Ponnarasu S, Mabrouk A, Griffin EE. Tillaux Fracture. StatPearls Publishing. PMID: 29493957. (NCBI)
- Stefanich RJ, Lozman J. The juvenile fracture of Tillaux. Clin Orthop Relat Res. 1986. PMID: 3757367. (PubMed)
- Dongmo Mayopa C, et al. Predictive Factors for Tillaux-Chaput Tubercle Fracture: A Case-Control Study. Foot Ankle Orthop. 2025. PMID: 40322590. (PubMed)
- Kose O, et al. Isolated Adult Tillaux Fracture Associated With Volkmann Fracture. J Foot Ankle Surg. 2016. PMID: 26711834. (PubMed)
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.