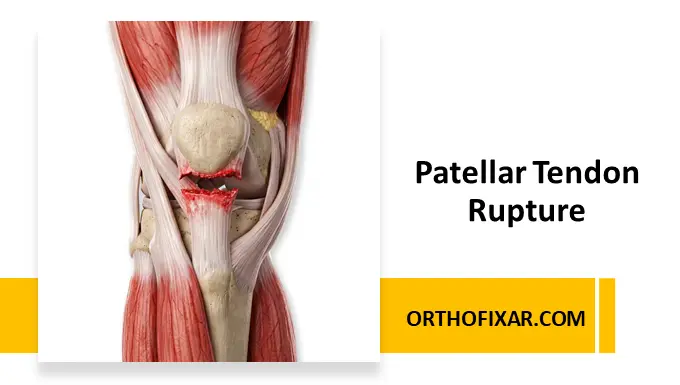
Patellar tendon rupture is a disabling injury that disrupts the knee’s extensor mechanism, resulting in loss of active knee extension. Although less common than quadriceps tendon rupture, it predominantly affects younger, active individuals and requires prompt recognition and treatment to restore function.
Epidemiology
- Patellar Tendon Rupture is less common than quadriceps tendon rupture
- Most frequently occurs in patients under 40 years old
- Often associated with pre-existing degenerative tendon changes
- Calcification may be visible on radiographs
- Most Patellar Tendon Ruptures occur at the inferior pole of the patella
Risk Factors
Systemic and local factors contribute to tendon degeneration:
- Rheumatoid arthritis
- Systemic lupus erythematosus
- Diabetes mellitus
- Chronic kidney disease
- Chronic systemic corticosteroid use
- Local steroid injections
- Chronic patellar tendinitis
Anatomy
Patellar Tendon Structure
- Average thickness: ~4 mm, widening to 5–6 mm at the tibial tubercle
- Composed of ~90% type I collagen
- Continuity with medial and lateral retinacula
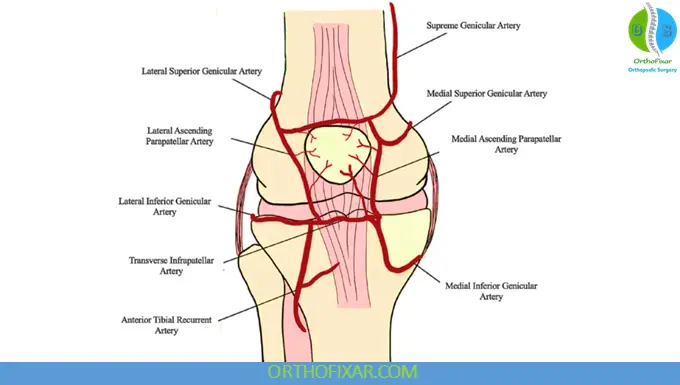
Blood Supply
- Posterior supply: infrapatellar fat pad vessels via inferior geniculate arteries
- Anterior supply: retinacular vessels via recurrent tibial and geniculate arteries
- Relatively avascular zones at proximal and distal insertions → common rupture sites
See Also: Knee Muscles Anatomy
Biomechanics
- Peak stress occurs at approximately 60° of knee flexion
- Forces across the tendon can reach 3.2× body weight during stair climbing
Clinical Evaluation
History
Patients with Patellar Tendon Rupture typically report:
- Sudden, forceful quadriceps contraction against a flexed knee
- Audible “pop”
- Immediate functional deficit
- Inability to bear weight or actively extend the knee
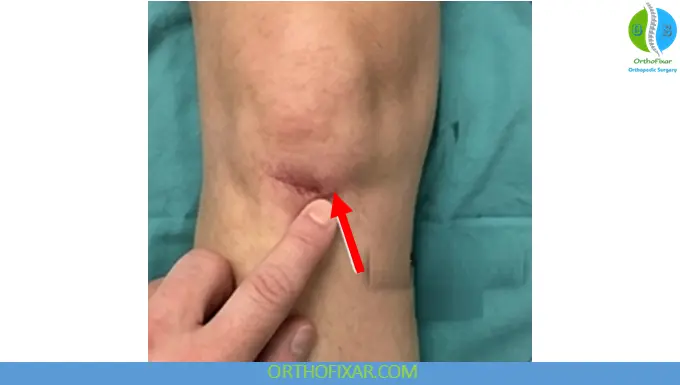
Physical Examination
- Palpable infrapatellar defect
- Hemarthrosis
- Pain with passive knee flexion
- Partial or complete loss of active extension
- Quadriceps atrophy in chronic cases
Radiographic Evaluation
X-ray (AP and Lateral)
- Patella alta (high-riding patella)
- Patella positioned superior to Blumensaat’s line
Ultrasound
- Useful for assessing patellar tendon continuity
- Operator-dependent
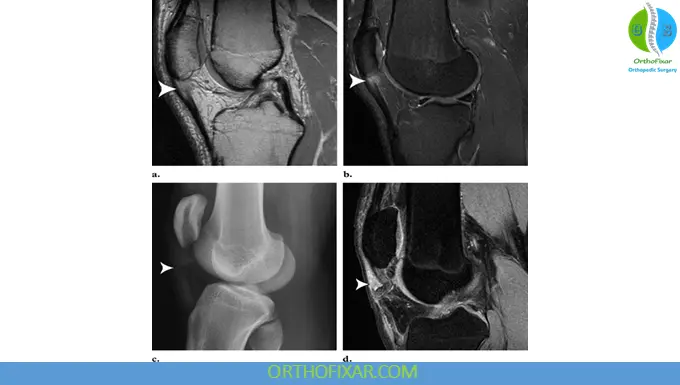
MRI
- Gold standard when Patellar Tendon Rupture diagnosis is unclear
- Accurately evaluates the patellar tendon integrity and associated injuries
Classification
There is no universally accepted classification system, but patellar tendon tears are commonly categorized by location:
- Proximal (most common)
- Mid-substance
- Distal (tibial tubercle insertion)
Patellar Tendon Rupture Treatment
Nonoperative Management
Indicated for partial tears with preserved active extension:
- Immobilization in full extension for 3–6 weeks
- Gradual rehabilitation
Operative Management
Indication: Complete rupture requiring restoration of extensor mechanism
Timing
- Acute repair (<2 weeks) → best outcomes
- Delayed repair (>6 weeks) → technically challenging, poorer prognosis
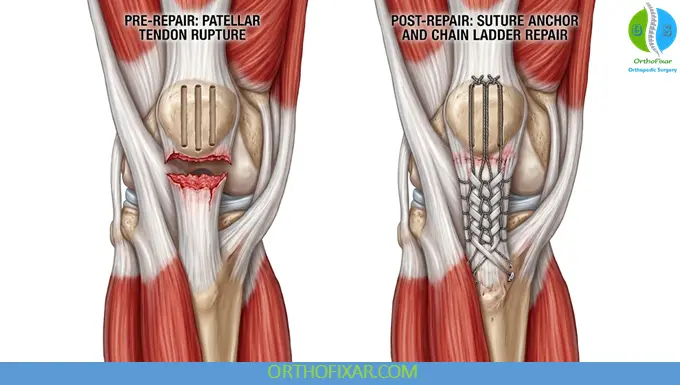
Early Surgical Repair
- Midline anterior incision
- Debridement of tendon edges
- Repair with nonabsorbable sutures
- Fixation methods:
- Transosseous bone tunnels
- Suture anchors (distal pole of patella)
- Repair of associated retinacular tears
- Optional augmentation:
- Cerclage wire, cable, or synthetic tape
Postoperative Recovery Protocol
- Knee immobilized in extension
- Immediate isometric quadriceps exercises
- Gradual ROM:
- 0–45° at 2 weeks
- Increase ~30° weekly
- Active extension at ~6 weeks
- Full weight-bearing in extension for 6 weeks
- Return to full activity at 4–6 months once:
- Full ROM achieved
- ≥90% quadriceps strength restored
Delayed Repair
Challenges include:
- Quadriceps retraction
- Patellar migration
- Adhesions
Surgical Options
- Primary repair with augmentation
- Autografts:
- Hamstring tendon
- Fascia lata
- Allograft:
- Achilles tendon
Rehabilitation
- More conservative than acute repair
- Immobilization (often casting) for ~6 weeks
- Delayed initiation of ROM
Complications
- Knee stiffness
- Persistent quadriceps weakness
- Rerupture
- Infection
- Patella baja (inferior patellar positioning)
Prognosis
- Strongly dependent on timing of surgical intervention
- Early patella rupture repair yields superior functional outcomes
- Delayed cases often require reconstruction and have reduced strength recovery
Key Takeaways
- Patellar tendon rupture is a surgical emergency in active individuals
- Diagnosis is primarily clinical, supported by imaging
- Early repair (<2 weeks) is the most critical prognostic factor
- Structured rehabilitation is essential for optimal recovery
References & More
- Mabrouk A, Siwiec RM. Patellar Tendon Rupture. [Updated 2026 Feb 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Brinkman JC, Reeson E, Chhabra A. Acute Patellar Tendon Ruptures: An Update on Management. J Am Acad Orthop Surg Glob Res Rev. 2024 Apr 3;8(4):e24.00060. doi: 10.5435/JAAOSGlobal-D-24-00060. PMID: 38569093; PMCID: PMC10994452. Pubmed
- Patellar Tendon Tear – Orthoinfo
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.