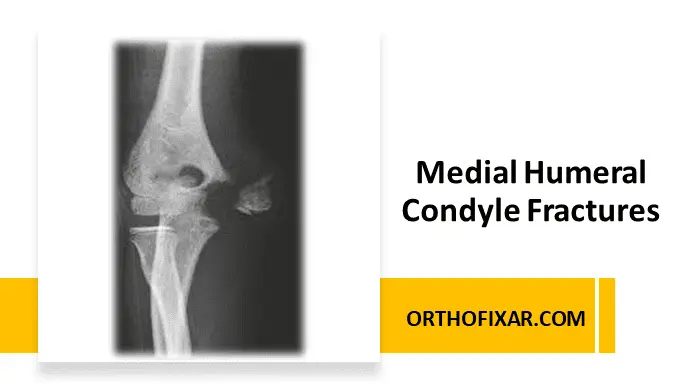
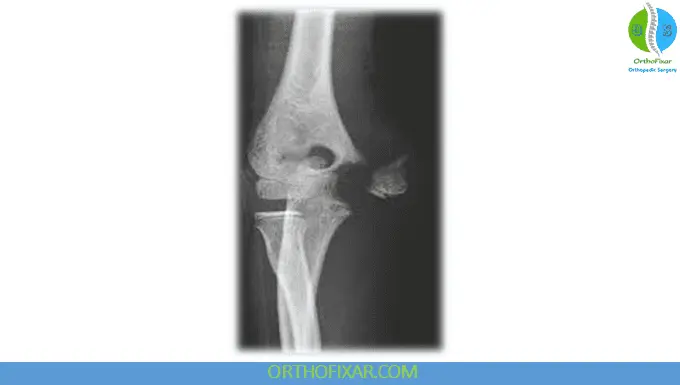
A medial humeral condyle fractures is a rare pediatric intra-articular injury involving the medial portion of the distal humerus. Unlike isolated medial epicondylar injuries, these fractures extend into the trochlea and the articular surface, making early recognition essential.
The medial condyle fractures are typically Salter-Harris type IV injuries, involving:
- The trochlea
- The medial metaphysis
- The medial epicondyle (common flexor origin)
Because the fracture crosses the physis and articular cartilage, delayed diagnosis may lead to deformity, stiffness, nonunion, or osteonecrosis.
Epidemiology
Medial humeral condyle fractures are uncommon injuries in children.
Key epidemiologic facts:
- Represent less than 1% of distal humerus fractures
- Peak incidence occurs between 8 and 14 years of age
- More common after high-energy falls or sports trauma
- Frequently missed during initial evaluation due to incomplete ossification of the trochlea in younger children
Recent reviews report a peak incidence between ages 8–12 years.
Surgical Anatomy
Ossification
The medial condylar ossification center develops relatively late, which makes radiographic diagnosis challenging in younger children.
Only the medial crista is initially ossified.
Vascular Supply
The blood supply of the medial condyle is clinically important:
- Medial epicondyle and metaphysis receive blood from the flexor muscle mass
- Trochlear vascularity traverses the medial physis
Physeal disruption may compromise blood flow and lead to:
- Trochlear osteonecrosis
- Growth disturbance
- “Fishtail deformity”
See Also: Elbow Anatomy
Mechanism of Injury
Medial humeral condyle fractures occur through either direct or indirect trauma.
Direct Mechanism
A fall onto a flexed elbow may cause:
- Olecranon impaction into the trochlea
- Splitting of the trochlea
- Proximal propagation into the metaphysis
Indirect Mechanism
A fall onto an outstretched hand with valgus stress may cause:
- Avulsion by the flexor-pronator mass
- Fracture beginning in the metaphysis and extending into the joint
These injuries are considered the mirror image of lateral condyle fractures. Powerful forearm flexors often produce anterior rotation of the fragment.
See Also: Pediatric Elbow – Lateral Condyle Fractures
Clinical Evaluation
Children with a medial humeral condyle fracture typically present with:
- Medial elbow pain
- Swelling
- Tenderness over the distal humerus
- Painful elbow motion
- Pain with resisted wrist flexion
A careful neurologic examination is mandatory because the ulnar nerve is vulnerable.
A common diagnostic error is mislabeling the injury as an isolated medial epicondyle fracture.
Important clues suggesting medial condyle fracture:
- Positive posterior fat pad sign
- Posteromedial elbow subluxation
- Intra-articular swelling
- Ulnar nerve symptoms
Radiographic Evaluation
Standard Imaging
Obtain:
- AP view
- Lateral view
- Oblique views
Arthrogram
Useful to:
- Delineate the cartilaginous fracture line
- Confirm intra-articular extension
MRI
Useful to:
- Identify fracture orientation
- Assess cartilage involvement
- Differentiate epicondylar versus condylar injuries
MRI and advanced imaging may improve diagnostic accuracy in occult pediatric elbow injuries.
See Also: Elbow X-Ray Views
Classification
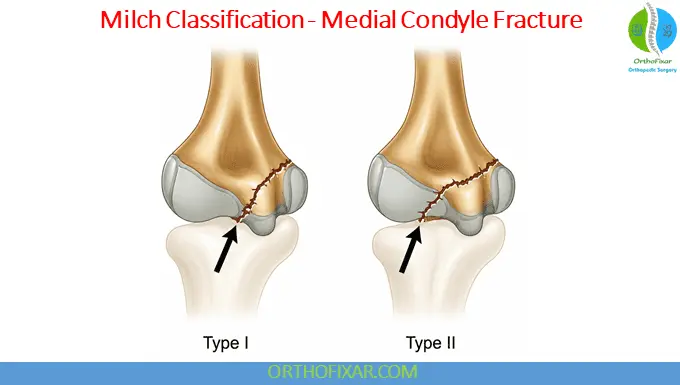
Milch Classification
Originally described by Harold Milch.
Type I
Fracture line traverses the apex of the trochlea.
Type II
Fracture line extends through the capitulotrochlear groove.
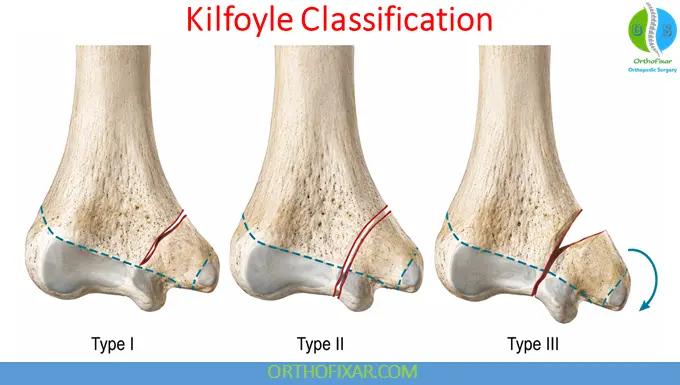
Kilfoyle Classification
Stage I
- Nondisplaced
- Articular surface intact
Stage II
- Complete fracture
- Minimal displacement
Stage III
- Complete displacement
- Fragment rotation caused by flexor pull
Kilfoyle classification remains the most widely used classification system.
See Also: Pediatric Supracondylar Humerus Fractures
Treatment of Medial Humeral Condyle Fractures
Nonoperative Treatment
Indications:
- Kilfoyle stage I
- Minimal displacement
- Stable fracture pattern
Treatment protocol:
- Long-arm cast or posterior splint
- Forearm in neutral rotation
- Elbow flexed to 90°
- Immobilization for 3–4 weeks
Followed by:
- Range-of-motion exercises
- Progressive strengthening
Closed Reduction and Percutaneous Pinning
May be considered when:
- Reduction is possible
- Fragment stability is acceptable
Technique:
- Elbow extended
- Forearm pronated to reduce flexor tension
- Two parallel K-wires across metaphysis
Open Reduction Internal Fixation (ORIF)
Indications:
- Kilfoyle stage II or III
- Irreducible fracture
- Fragment rotation
- Unstable reduction
Surgical principles:
- Medial approach
- Identification and protection of ulnar nerve
- Preserve posterior trochlear blood supply
- Fixation with smooth K-wires or cannulated screws in adolescents
Recent surgical series show excellent outcomes with stable fixation of displaced fractures.
Delayed Presentation
If diagnosis is delayed beyond 3–6 weeks:
Open reduction may increase risk of:
- Osteonecrosis
- Severe stiffness
- Soft tissue injury
In many delayed cases, nonoperative management may be preferred.
Complications
Missed Diagnosis
Most common complication.
Often confused with medial epicondyle fracture.
Nonunion
Usually occurs in:
- Untreated displaced fractures
- Rotated fragments
Angular Deformity
Includes:
- Cubitus varus
- Cubitus valgus
Osteonecrosis
May produce:
- Trochlear collapse
- “Fishtail deformity”
Ulnar Neuropathy
May occur:
- Early after trauma
- Late from deformity or scar tissue
Persistent symptoms may require surgical decompression.
Prognosis
Early diagnosis and anatomic reduction generally produce excellent outcomes.
Poor prognostic factors include:
- Missed diagnosis
- Delayed treatment
- Fragment rotation
- Vascular compromise
Key Clinical Pearls
✅ Rare injury (<1% of distal humerus fractures)
✅ Usually affects children aged 8–14 years
✅ Frequently mistaken for medial epicondyle fracture
✅ Positive fat pad sign strongly suggests intra-articular injury
✅ Kilfoyle classification guides treatment
✅ Protect the ulnar nerve during surgery
✅ Late surgery increases osteonecrosis risk
Frequently Asked Questions
Are medial humeral condyle fractures common?
No. They account for less than 1% of pediatric distal humerus fractures.
Why are these fractures frequently missed?
Because the trochlear ossification center develops late, making radiographs difficult to interpret in younger children.
When is surgery indicated?
Surgery is typically required for displaced or rotated fractures (Kilfoyle II–III).
References & More
- Orellana KJ, Baghdadi S, Buttrick E, Värk PR, Baldwin K, Shah AS. Pediatric Medial Humeral Condyle Fractures: Classification, Treatment, and Outcomes. J Pediatr Orthop. 2025 Mar 1;45(3):113-119. doi: 10.1097/BPO.0000000000002879. Epub 2024 Dec 2. PMID: 39618147. Pubmed
- Fernandez FF, Vatlach S, Wirth T, Eberhardt O. Medial humeral condyle fracture in childhood: a rare but often overlooked injury. Eur J Trauma Emerg Surg. 2019 Aug;45(4):757-761. doi: 10.1007/s00068-018-0930-y. Epub 2018 Feb 26. PMID: 29484463. Pubmed
- Sonohata M, Nakashima T, Suetsugi H, Kitajima M, Ueno M, Mawatari M. Medial Condyle Fracture (Kilfoyle Type III) of the Distal Humerus with Transient Fishtail Deformity after Surgery. Case Rep Orthop. 2017;2017:9053949. doi: 10.1155/2017/9053949. Epub 2017 Dec 14. PMID: 29527370; PMCID: PMC5745729. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.