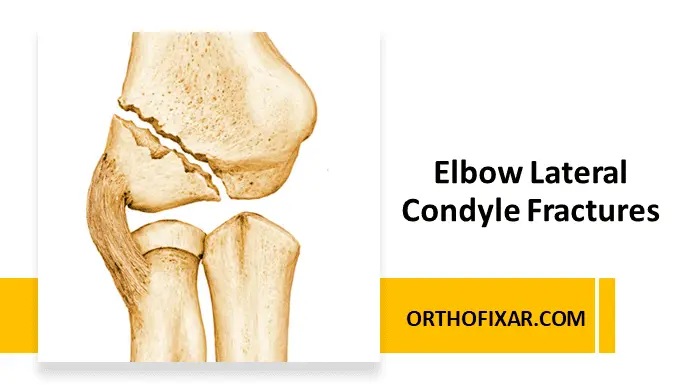
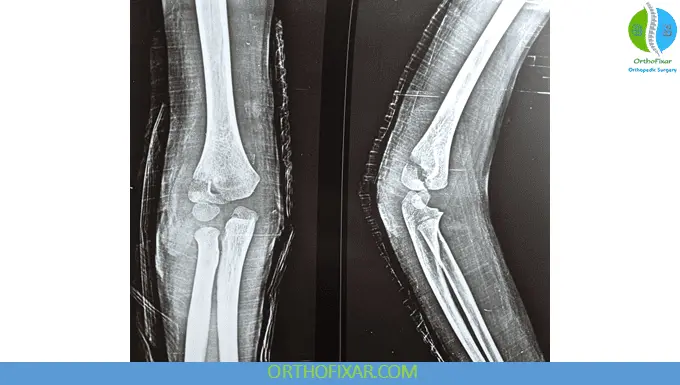
Pediatric lateral condyle fractures of the distal humerus are among the most clinically important elbow injuries in children because they involve the articular surface and growth plate. Delayed diagnosis or inadequate treatment may lead to long-term complications including nonunion, cubitus valgus deformity, stiffness, and tardy ulnar nerve palsy.
These fractures often appear deceptively subtle on examination and radiographs, making careful evaluation essential.
What Are Pediatric Lateral Condyle Fractures?
A lateral condyle fracture is a physeal injury involving the lateral distal humerus, usually extending into the capitellum and trochlea. These fractures are intra-articular and frequently unstable because of muscular pull from the common extensor origin.
They are distinct from supracondylar fractures and generally have a higher risk of growth disturbance and poorer functional outcomes if not appropriately managed.
Epidemiology
- Represent approximately 17% of all distal humerus fractures in children
- Peak incidence occurs around 6 years of age
- Less satisfactory outcomes compared with supracondylar fractures because:
- Diagnosis may be subtle and easily missed
- Intra-articular involvement causes greater motion loss
- Higher incidence of growth disturbance and nonunion
Why These Fractures Are Important
Even minimally displaced fractures may later displace because the extensor musculature remains attached to the distal fragment. Missed injuries can progress to chronic instability, deformity, and permanent elbow dysfunction.
Anatomy of the Lateral Condyle
The lateral condyle ossification center extends to the lateral crista of the trochlea. The fracture often disrupts the cartilaginous articular surface and adjacent soft tissues.
Important anatomic considerations include:
- The origins of the:
- Extensor carpi radialis longus
- Brachioradialis: remain attached to the distal fragment
- This muscular attachment contributes to:
- Initial displacement
- Progressive late displacement
- Risk of nonunion
- Disruption of the lateral trochlear crista (Milch type II) may produce:
- Posterolateral subluxation of the radius and ulna
- Cubitus valgus deformity
- Confusion with elbow dislocation on imaging
See Also: Elbow Anatomy
Mechanism of Injury
Two classic theories explain the mechanism of injury of the Lateral Condyle Fractures in children.
1. “Pull-Off” Theory
A varus stress on the extended elbow creates avulsion by the common extensor origin.
2. “Push-Off” Theory
An axial load through the forearm during a fall onto an outstretched hand causes the radial head to impact the lateral condyle.
Both mechanisms commonly occur during falls while playing or sports activities.
Clinical Presentation
Unlike supracondylar fractures, lateral condyle fractures usually produce minimal gross deformity.
Common Findings
- Mild lateral elbow swelling
- Localized tenderness over the lateral distal humerus
- Painful elbow motion
- Pain with resisted wrist extension
- Decreased range of motion
- Possible crepitus during pronation-supination
Crepitus should not be intentionally elicited because manipulation may worsen displacement.
See Also: Pediatric Supracondylar Humerus Fractures
Radiographic Evaluation
Proper imaging is critical because Lateral Condyle Fractures are frequently underestimated on initial radiographs.
Recommended Views
- AP view
- Lateral view
- Internal oblique view
The oblique view is especially useful for detecting subtle displacement.
Additional Imaging
Varus Stress Views
Can accentuate fracture displacement.
Arthrogram
Helpful in young children with unossified cartilage when distinguishing between:
- Lateral condyle physeal fracture
- Distal humeral physeal separation
MRI
May better define:
- Fracture orientation
- Cartilage involvement
- Articular disruption
Classification of Pediatric Lateral Condyle Fractures
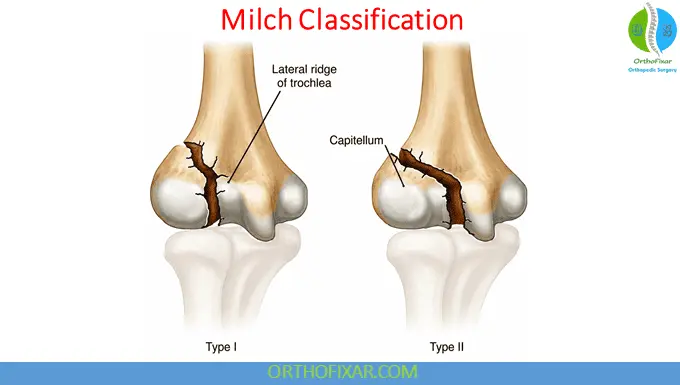
Milch Classification
Milch Type I
- Fracture line passes lateral to the trochlea
- Equivalent to Salter-Harris type IV
Characteristics:
- Trochlea remains intact
- Elbow is relatively stable
- Less common
Milch Type II
- Fracture extends through the trochlea apex
- Equivalent to Salter-Harris type II
Characteristics:
- Trochlear disruption present
- Elbow instability common
- Most common fracture type
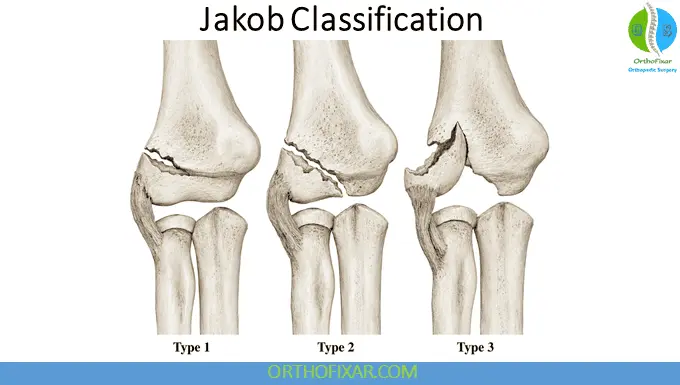
Jakob Classification
Stage I
- Nondisplaced fracture
- Intact articular surface
Stage II
- Moderate displacement
- Partial articular disruption
Stage III
- Complete displacement with rotation
- Elbow instability present
The Jakob classification is clinically useful because it directly guides treatment decisions.
Treatment of Pediatric Lateral Condyle Fractures
Nonoperative Treatment
Indicated for:
- Jakob stage I fractures
- Displacement less than 2 mm
Approximately 40% of fractures can be managed conservatively.
Immobilization Technique
- Posterior splint or long-arm cast
- Elbow flexed to 90°
- Forearm in neutral rotation
Immobilization typically continues for approximately 3 weeks followed by progressive range-of-motion exercises.
Important Considerations
Serial radiographs are essential because initially nondisplaced fractures may later displace.
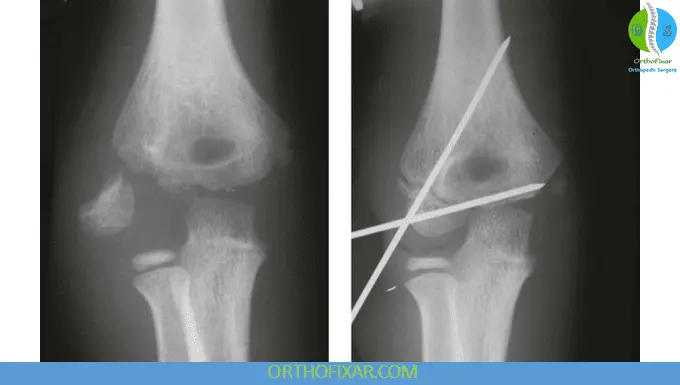
Closed Reduction and Percutaneous Pinning
May be attempted in selected Jakob stage II fractures.
Reduction maneuvers include:
- Varus force
- Supination
- Elbow extension
If reduction is satisfactory:
- Percutaneous Kirschner wires are inserted
- Arthrogram may confirm articular congruity
Operative Management
Indications
Open reduction is usually required for:
- Unstable Jakob stage II fractures
- All Jakob stage III fractures
Approximately 60% of patients require surgery.
Surgical Technique
The fracture fragment is commonly fixed using:
- Two smooth divergent Kirschner wires
Important principles:
- Preserve posterior soft tissues
- Avoid disrupting vascular supply
- Minimize periosteal stripping
Smooth pins crossing the physis generally do not produce growth arrest.
Postoperative Care
- Long-arm cast
- Elbow flexed 60–90°
- Neutral forearm rotation
Pins and cast are usually removed after 3–6 weeks, followed by active rehabilitation.
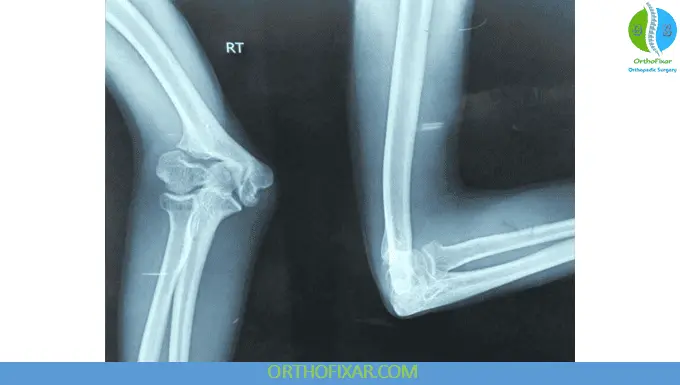
Delayed Presentation
When diagnosis is delayed beyond 3–6 weeks:
- Closed treatment is often preferred
- Late open reduction carries increased risk of:
- Osteonecrosis
- Joint stiffness
- Poor outcomes
Management decisions become significantly more complex in chronic injuries.
Complications
Lateral Condylar Overgrowth
Occurs from ossified periosteal elevation.
May create:
- Cosmetic lateral prominence
- Cubitus pseudovarus appearance
Usually not functionally limiting.
Delayed Union and Nonunion
Nonunion risk is relatively high because of:
- Extensor muscle pull
- Limited metaphyseal circulation
Potential consequences:
- Cubitus valgus
- Chronic instability
- Tardy ulnar nerve palsy
Treatment options include:
- Observation
- Corrective osteotomy
- Compression fixation
Angular Deformity
Cubitus Valgus
Most common deformity.
Caused by:
- Lateral physeal arrest
- Nonunion
May lead to tardy ulnar nerve palsy requiring nerve transposition.
Cubitus Varus
Less common than valgus deformity.
Neurologic Complications
Acute nerve injury is uncommon.
However, chronic cubitus valgus may produce:
- Progressive ulnar neuropathy
- Hand weakness
- Sensory changes
This delayed neuropathy is known as tardy ulnar nerve palsy.
Osteonecrosis
Iatrogenic osteonecrosis may occur after delayed or aggressive surgery.
Possible findings include:
- “Fishtail” deformity
- Persistent physeal gap
Although radiographically striking, long-term functional impairment is often limited.
Prognosis
Outcomes are generally excellent when fractures are:
- Diagnosed early
- Anatomically reduced
- Properly stabilized
Poor outcomes are usually associated with:
- Missed fractures
- Delayed treatment
- Inadequate fixation
- Nonunion
Key Clinical Pearls
- Always obtain oblique radiographs in pediatric elbow trauma
- Mild swelling does not exclude significant injury
- Fractures displaced less than 2 mm still require close follow-up
- Nonunion risk is substantially higher than in supracondylar fractures
- Preservation of posterior blood supply is critical during surgery
Frequently Asked Questions (FAQ)
What is the most common type of pediatric lateral condyle fracture?
Milch type II fractures are the most common and are associated with elbow instability.
Why are lateral condyle fractures easily missed?
Children often present with only mild swelling and minimal deformity despite significant intra-articular injury.
When is surgery required?
Surgery is generally indicated for fractures displaced more than 2 mm or fractures with articular incongruity or instability.
What is the most serious long-term complication?
Nonunion with cubitus valgus and tardy ulnar nerve palsy is among the most clinically significant complications.
Conclusion
Pediatric lateral condyle fractures are common intra-articular elbow injuries with substantial potential for long-term morbidity if missed or undertreated. Accurate diagnosis, careful radiographic assessment, and appropriate stabilization are essential to prevent complications such as nonunion, deformity, stiffness, and growth disturbance.
Because subtle injuries may later displace, vigilant follow-up is critical even in minimally displaced fractures.
References & More
- Martins T, Tiwari V, Marappa-Ganeshan R. Pediatric Lateral Humeral Condyle Fractures. [Updated 2024 Feb 9]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Tan SHS, Dartnell J, Lim AKS, Hui JH. Paediatric lateral condyle fractures: a systematic review. Arch Orthop Trauma Surg. 2018 Jun;138(6):809-817. doi: 10.1007/s00402-018-2920-2. Epub 2018 Mar 24. PMID: 29574555. Pubmed
- Masci G, Basiglini L, Giusti C, Aulisa AG, Falciglia F. Lateral Humeral Condyle Fracture in Childhood: Results of a New Surgical Technique. J Clin Med. 2024 May 11;13(10):2830. doi: 10.3390/jcm13102830. PMID: 38792372; PMCID: PMC11122216. Pubmed