Subtrochanteric femur fractures account for 10–30% of all hip fractures and can occur across all age groups. The injury demonstrates a bimodal distribution, affecting younger adults aged 20–40 years (often from high-energy trauma) and older adults over 60 years (typically due to low-energy falls through osteoporotic bone).
Anatomy
The subtrochanteric region is defined as the femoral segment between the lesser trochanter and a point 5 cm distal. This area experiences high biomechanical stress:
- Medial and posteromedial cortices: high compressive forces
- Lateral cortex: high tensile forces
The subtrochanteric region is composed mainly of cortical bone, resulting in reduced vascularity and a slower healing potential compared with intertrochanteric fractures.
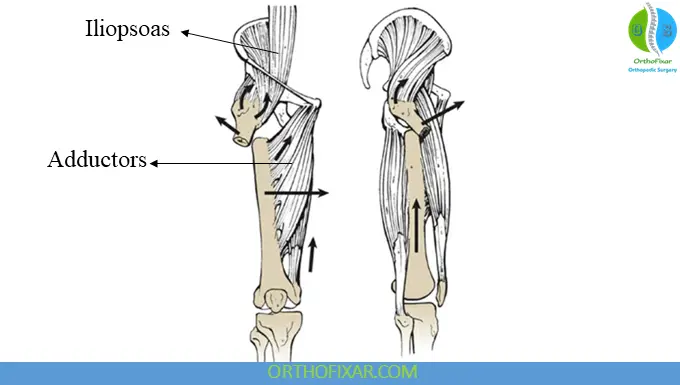
Deforming Muscle Forces
- Proximal fragment: abducted by gluteus, externally rotated by short rotators, flexed by psoas
- Distal fragment: pulled proximally and into varus by adductors
These forces often result in malalignment if untreated.
See Also: Hip Joint Anatomy
Mechanism of Injury
Subtrochanteric fractures may result from:
- Low-energy trauma – Minor falls in elderly patients with osteoporotic bones
- High-energy trauma – Motor vehicle accidents, falls from height, gunshot wounds (10% of cases)
- Pathologic fractures – Tumors or metabolic bone disease (17–35% of cases)
- Atypical fractures – Minimal trauma fractures, often associated with bisphosphonates, glucocorticoids, or PPIs
Clinical Evaluation
Patients typically present with:
- Inability to bear weight
- Gross deformity of the lower extremity
- Painful hip motion, swelling, and tenderness of the proximal thigh
Important considerations:
- Evaluate for associated injuries in high-energy trauma
- Neurovascular compromise is rare but should be assessed
- Monitor for hemorrhagic shock, as the thigh can conceal significant blood loss
See Also: Hip Intertrochanteric Fractures
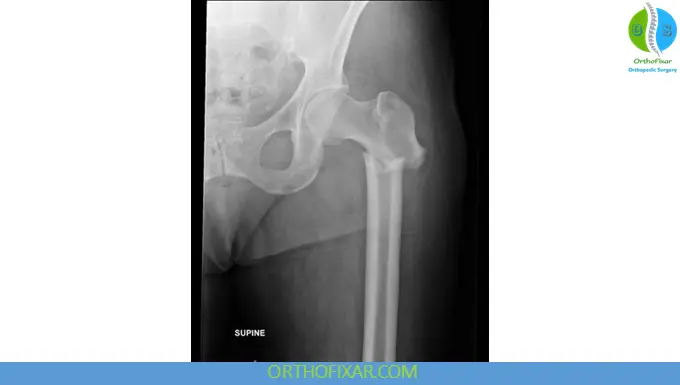
Radiographic Evaluation
- AP pelvis and AP/lateral hip and femur
- Assess the entire femur including the knee
- Contralateral femur radiograph may help determine length in comminuted fractures
See Also: Hip Joint X-Ray Imaging
Subtrochanteric Femur Fractures Classification
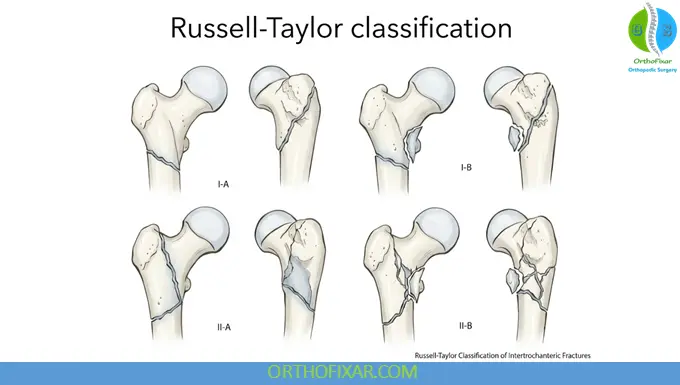
Russell-Taylor Classification (historical)
- Type I: Fractures with intact piriformis fossa
- A: Lesser trochanter attached
- B: Lesser trochanter detached
- Type II: Fractures extending into piriformis fossa
- A: Stable medial construct
- B: Comminuted piriformis fossa and lesser trochanter
Subtrochanteric Fracture Treatment
Nonoperative (Historical)
- Skeletal traction followed by spica casting or cast bracing
- Reserved for nonoperative candidates (elderly or children)
- Increased risk of nonunion, malunion, varus angulation, and rotational deformity
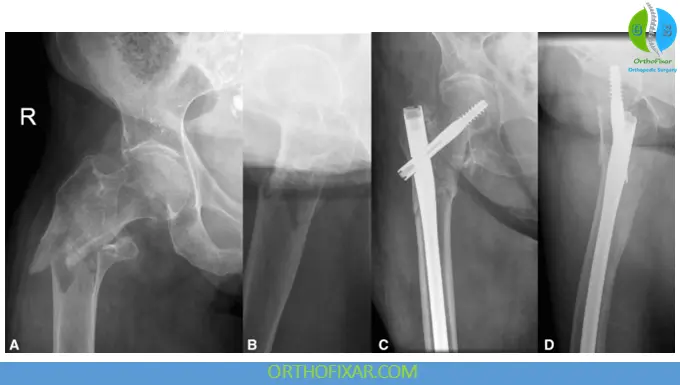
Operative (Preferred)
- Interlocking Nails (Intramedullary nails)
- First-generation: trochanteric entry, both trochanters intact
- Second-generation cephalomedullary nails: for fractures with posteromedial cortex loss
- 95-degree Fixed Angle Plate
- Suitable for fractures involving both trochanters
- Accessory screw may increase proximal fixation
- Proximal femur precontoured locking plates: newer alternative
Important Notes:
- Sliding hip screws are not recommended for subtrochanteric fractures
- Bone grafting is used only if indirect reduction fails
- Open fractures require immediate debridement and stabilization
Complications
- Loss of Fixation
- Implant failure due to screw cutout, plate breakage, or nail fatigue
- Nonunion
- Inability to bear weight after 4–6 months
- Associated with inadequate reduction
- Malunion
- Coxa vara, leg length discrepancy, malrotation
- Corrected with valgus osteotomy and revision fixation
Key Takeaways
- Subtrochanteric fractures are biomechanically challenging due to high cortical stress
- Operative fixation with intramedullary nails or fixed-angle plates is standard
- Complications like nonunion and malunion are common if alignment and reduction are not optimal
- Careful clinical and radiographic evaluation is critical, especially in high-energy trauma
References & More
- Medda S, Reeves RA, Pilson H. Subtrochanteric Femur Fractures. [Updated 2023 Jul 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Gösling T. Subtrochantäre Frakturen [Subtrochanteric fractures]. Unfallchirurg. 2022 May;125(5):389-403. German. doi: 10.1007/s00113-022-01175-y. Epub 2022 Apr 8. PMID: 35394157. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.