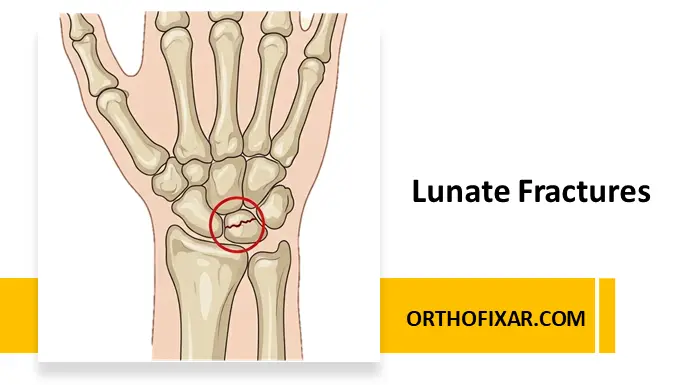
Lunate fractures are uncommon but clinically significant wrist injuries that require a high index of suspicion for accurate diagnosis and management. Despite being relatively rare, the lunate is recognized as the fourth most frequently fractured carpal bone, following the scaphoid, triquetrum, and trapezium. Due to its central role in carpal stability and motion, injury to this bone can result in substantial functional impairment if not properly treated.
Anatomy and Biomechanical
The lunate occupies a pivotal position within the proximal carpal row and is often described as the “carpal keystone.” It sits securely within the lunate fossa of the distal radius, forming a stable articulation proximally. Laterally and medially, it is anchored by strong interosseous ligaments to the scaphoid and triquetrum, respectively. Distally, it articulates with the convex head of the capitate, contributing to smooth wrist motion.
The vascular supply of the lunate is derived from both dorsal and volar branches of the proximal carpal arcade. These vessels form variable intraosseous anastomoses, which are critical for maintaining bone viability. Disruption of this delicate blood supply significantly increases the risk of osteonecrosis.
Mechanism of Injury
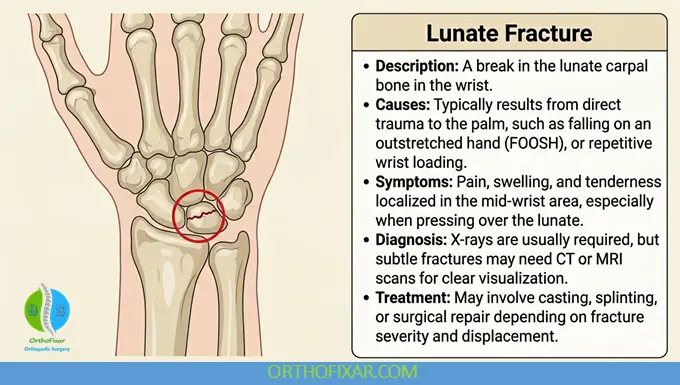
Lunate fractures most commonly occur due to high-energy loading of the wrist. The typical mechanisms include:
- A fall onto an outstretched hand (FOOSH) with the wrist in hyperextension
- Forceful axial loading or pushing with the wrist extended
These mechanisms generate compressive and shear forces across the lunate, leading to fracture.
Clinical Presentation
Patients with a lunate fracture often present with:
- Localized tenderness over the dorsal wrist, particularly over the lunate and distal radius
- Painful and restricted range of motion
- Swelling and decreased grip strength in some cases
Due to the nonspecific nature of these symptoms, diagnosis may be delayed or overlooked.
Imaging and Diagnosis
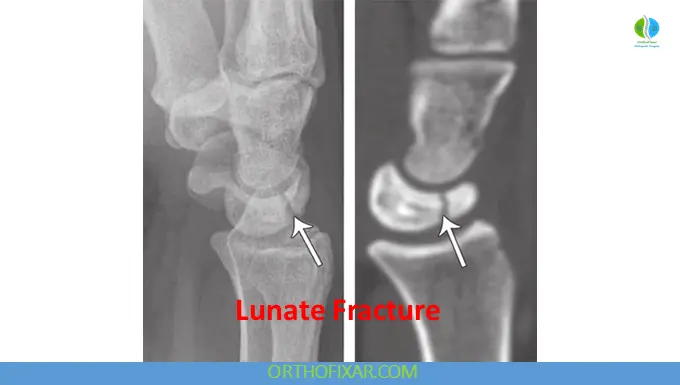
Standard radiographic evaluation includes posteroanterior (PA) and lateral wrist views. However, these are frequently insufficient due to overlapping carpal structures obscuring the lunate.
Advanced imaging plays a crucial role:
- Oblique radiographs may improve visualization
- CT scans provide superior detail and are considered the gold standard for detecting fractures
- MRI is essential for assessing vascular integrity and is particularly valuable when evaluating for osteonecrosis or Kienböck disease
Classification of Lunate Fractures
Acute lunate fractures are classified into five distinct types based on fracture pattern and vascular involvement:
- Frontal fractures of the palmar pole involving nutrient arteries
- Osteochondral fractures of the proximal articular surface without major vascular disruption
- Frontal fractures of the dorsal pole
- Transverse fractures through the body
- Transarticular frontal fractures involving the lunate body
This classification assists clinicians in predicting prognosis and selecting appropriate treatment strategies.
Lunate Fractures Treatment
Conservative Management
Nondisplaced Lunate fractures are typically managed nonoperatively:
- Immobilization using a short or long arm cast or splint
- Close follow-up with serial imaging to monitor healing
This approach is supported by clinical evidence showing favorable outcomes when vascular supply remains intact.
Surgical Intervention
Surgery is indicated in cases of:
- Displaced or angulated Lunate fractures
- Instability or subluxation involving adjacent carpal bones
Procedures may include:
- Open reduction and internal fixation (ORIF)
- Restoration of anatomical alignment to promote revascularization
In particular, palmar lip fractures with volar subluxation of the capitate require surgical stabilization to prevent long-term dysfunction.
Complications
Kienböck Disease (Osteonecrosis of the Lunate)
One of the most serious complications is osteonecrosis, known as Kienböck disease. This condition arises from compromised blood supply and may occur following trauma or idiopathically.
Clinical consequences include:
- Progressive collapse of the lunate
- Chronic wrist pain
- Radiocarpal joint degeneration
MRI is the diagnostic modality of choice for early detection.
See Also: Wrist Pain Causes
Advanced Management Options
In advanced cases, surgical interventions may be required for pain relief and functional restoration:
- Radial shortening osteotomy
- Radial wedge osteotomy
- Ulnar lengthening procedures
- Salvage procedures such as proximal row carpectomy
- Wrist denervation
Conclusion
Lunate fractures, although rare, present significant diagnostic and therapeutic challenges. Their central role in wrist biomechanics and vulnerability to vascular compromise necessitate early recognition and appropriate management. Advanced imaging techniques, particularly CT and MRI, are essential for accurate diagnosis and prevention of complications such as Kienböck disease. Evidence-based treatment—ranging from immobilization to surgical intervention—ensures optimal outcomes and preservation of wrist function.
References & More
- Tagliero LE, Munaretto N, Lenartowicz K, Shin A, Bishop A, Moran SL, Kakar S. Treatment Options for Coronal Plane Fractures of the Lunate in Kienböck Disease. Hand (N Y). 2026 Jan;21(1):151-158. doi: 10.1177/15589447241298722. Epub 2024 Nov 26. PMID: 39588834; PMCID: PMC11590080. Pubmed
- MacLean SBM, Bain GI. Lunate Fracture Morphology in Kienbock’s Disease-A Computed Tomography Study. J Wrist Surg. 2022 Oct 6;12(2):128-134. doi: 10.1055/s-0042-1756497. PMID: 36926207; PMCID: PMC10010897. Pubmed
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.