Scapulothoracic dissociation is a rare but devastating traumatic injury characterized by disruption of the scapula from the posterior chest wall. It represents one of the most severe forms of shoulder girdle trauma and is often described as a “subcutaneous forequarter amputation” due to the extent of soft tissue, vascular, and neurologic damage.
Epidemiology & Mechanism of Injury
This condition is uncommon but carries high morbidity and mortality. It typically occurs in high-energy trauma, most frequently:
- Motor vehicle collisions
- Motorcycle accidents
- Industrial or crush injuries
Mechanism
The injury results from:
- Violent traction forces
- Combined rotation and lateral displacement of the shoulder girdle
These forces lead to separation of the scapula from the thoracic cage, often with severe damage to surrounding neurovascular structures.
Pathophysiology
Scapulothoracic dissociation involves disruption of multiple anatomical components:
- Muscles anchoring the scapula to the thorax
- Ligamentous stabilizers of the shoulder girdle
- Neurovascular bundle (brachial plexus and subclavian/axillary vessels)
This results in a functionally nonviable upper extremity in severe cases.
Associated Neurovascular Injuries
Neurovascular compromise is extremely common and a major determinant of outcome:
- Complete brachial plexopathy: ~80%
- Partial brachial plexopathy: ~15%
- Subclavian or axillary artery injury: ~88%
These injuries often dictate both limb viability and long-term function.
See Also: Scapular Dyskinesis
Clinical Presentation
Patients are typically polytraumatized and may present with:
- Massive swelling of the shoulder region
- A pulseless upper limb (vascular compromise)
- Complete or partial neurologic deficit
- Flail or nonfunctional extremity
High clinical suspicion is essential in high-energy trauma settings.
Diagnosis
Clinical Clues
- Severe shoulder swelling
- Absent distal pulses
- Neurologic impairment
Imaging
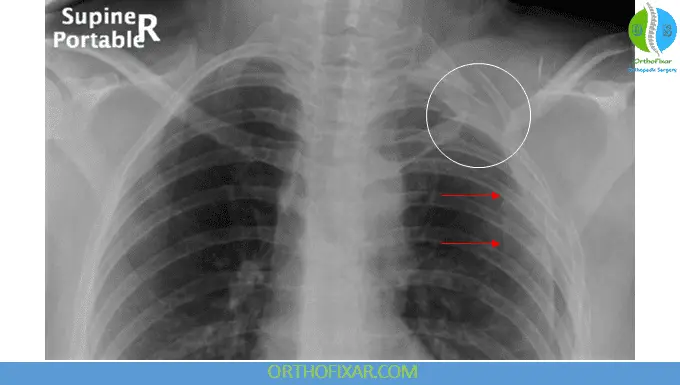
Chest radiograph (nonrotated) is key:
- Shows lateral displacement of the scapula compared to the contralateral side
- This finding is considered diagnostic
Additional imaging:
- CT angiography → evaluate vascular injury
- MRI → assess brachial plexus injury
MRI finding:
- “Empty sleeve sign” → indicates nerve root avulsion
Classification
Scapulothoracic dissociation is classified based on associated injuries:
| Type | Description |
|---|---|
| Type I | Musculoskeletal injury only |
| Type IIA | Musculoskeletal + vascular injury |
| Type IIB | Musculoskeletal + neurologic injury |
| Type III | Musculoskeletal + both neurologic and vascular injury |
Initial Treatment
Treatment of Scapulothoracic Dissociation follows Advanced Trauma Life Support (ATLS) principles:
Primary Priorities
- Airway, breathing, circulation stabilization
- Control of hemorrhage
- Rapid assessment of associated injuries
Limb-Specific Treatment
- Angiography for suspected vascular injury
- Urgent vascular repair when indicated
- Brachial plexus exploration in select cases
- Stabilization of fractures or dislocations
Secondary (Definitive) Treatment
Neurologic Evaluation
- 3 weeks: Electromyography (EMG)
- 6 weeks: MRI or cervical myelography
Prognostic Indicators
Poor prognosis associated with:
- Complete brachial plexus injury
- Nerve root avulsions
- ≥3 pseudomeningoceles on imaging
Surgical Options
- Shoulder arthrodesis for stability
- Above-elbow amputation in nonfunctional (flail) limbs
- Early amputation may be considered in severe cases
Outcomes & Prognosis
Scapulothoracic dissociation has a poor overall prognosis:
- Flail extremity: ~52%
- Early amputation: ~21%
- Mortality: ~10%
Recovery Potential
- Partial brachial plexus injuries → better prognosis, possible functional recovery
- Complete plexus injuries → typically poor functional outcomes
Key Takeaways
- Scapulothoracic dissociation is a high-energy, life-threatening injury.
- Strongly associated with severe neurovascular damage.
- Lateral scapular displacement on chest X-ray is diagnostic.
- Management requires multidisciplinary trauma care.
- Prognosis depends largely on the extent of brachial plexus injury.
References & More
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Kani KK, Chew FS. Scapulothoracic dissociation. Br J Radiol. 2019;92(1101):20190090. doi:10.1259/bjr.20190090. Pubmed
- Kani KK, Chew FS. Scapulothoracic dissociation. Br J Radiol. 2019 Sep;92(1101):20190090. doi: 10.1259/bjr.20190090. Epub 2019 Jun 5. PMID: 31046412; PMCID: PMC6732935. Pubmed
- Brucker PU, Gruen GS, Kaufmann RA. Scapulothoracic dissociation: evaluation and management. Injury. 2005 Oct;36(10):1147-55. doi: 10.1016/j.injury.2004.12.053. Epub 2005 Feb 23. PMID: 16214460. Pubmed