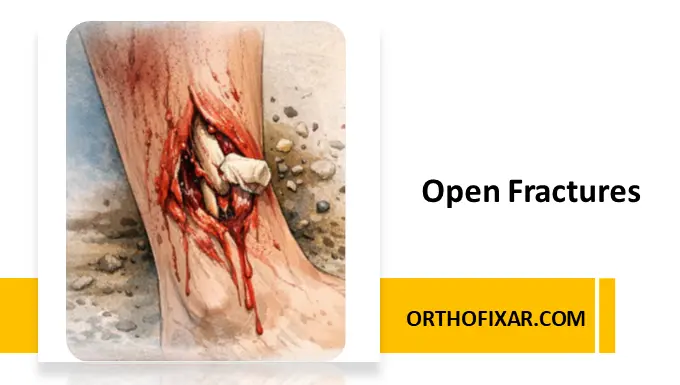
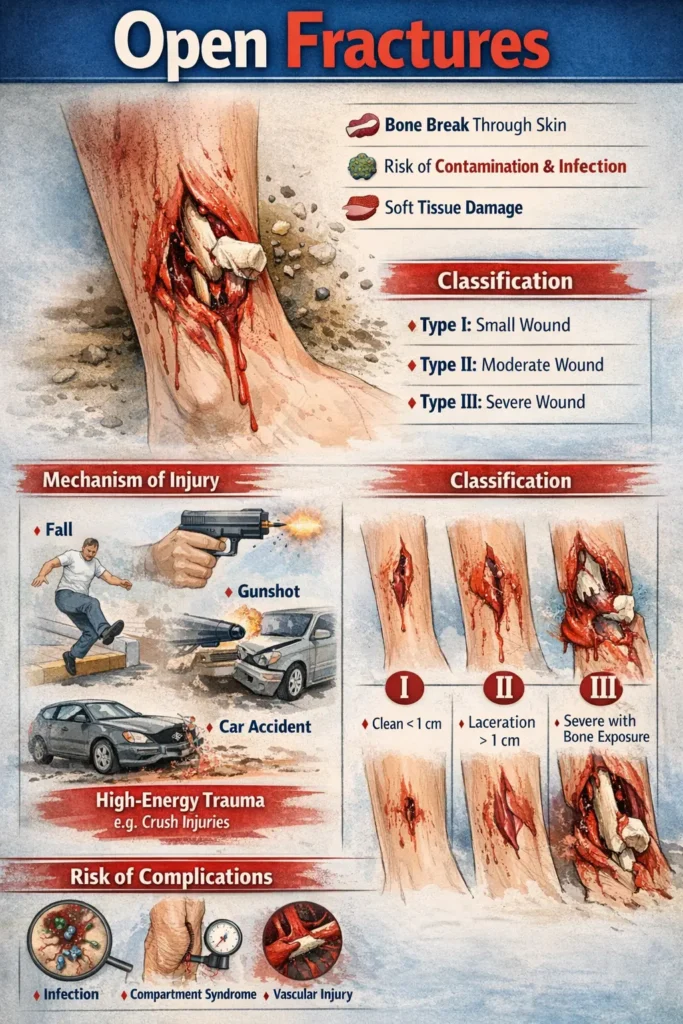
An open fracture is an osseous injury in which a break in the skin and underlying soft tissue communicates directly with the fracture and its hematoma. The term compound fracture is synonymous but considered outdated.
Clinically, any wound overlying a fractured limb segment must be treated as an open fracture until proven otherwise.
Approximately one-third of patients with open fractures have polytrauma, making systematic trauma assessment essential.
Pathophysiology & Clinical Significance
Open fractures are not simply bone injuries—they represent a combined bone and soft tissue insult with three major consequences:
- Contamination
- Direct exposure introduces bacteria → risk of infection and osteomyelitis
- Soft Tissue Damage
- Crushing, devascularization → impaired healing and increased infection susceptibility
- Loss of Soft Tissue Envelope
- Affects:
- Fracture stabilization
- Biological healing (loss of osteoprogenitor contribution)
- Limb function (muscle, nerve, vascular damage)
- Affects:
Mechanism of Injury
Open fractures result from high-energy trauma, where kinetic energy is transferred to bone and soft tissues.
Examples of Energy Transfer
| Injury Mechanism | Energy (ft-lb) |
|---|---|
| Fall from curb | ~100 |
| Skiing injury | 300–500 |
| Gunshot (high velocity) | ~2,000 |
| 20 mph bumper impact | ~100,000 |
👉 Greater energy → more comminution + worse soft tissue injury
Clinical Evaluation
1. Trauma Assessment (ATLS Protocol)
Follow Advanced Trauma Life Support:
- Primary survey (ABCDE)
- Secondary survey (full exam + imaging)
- Tertiary survey (serial reassessment)
2. Key Steps
- Resuscitate and treat life-threatening injuries first
- Evaluate:
- Head, chest, abdomen, pelvis, spine
- Assess:
- Neurovascular status
- Soft tissue damage
- All extremities
3. Wound Handling Principles
- ❌ Do NOT probe or aggressively explore in ER if surgery planned
- ✅ Remove only obvious superficial foreign bodies
- ✅ Irrigate if surgical delay is expected
4. Imaging
- X-rays: ≥2 orthogonal views
- Include joint above and below
- CT scan:
- Useful for intra-articular fractures
- Detects traumatic arthrotomy (air in joint)
Compartment Syndrome
⚠️ Open fractures do NOT exclude compartment syndrome
Key Signs
- Severe pain (especially with passive stretch)
- Paresthesia
- Tense compartment
- Reduced sensation
Diagnostic Threshold
- Compartment pressure >30 mmHg
- Or within 30 mmHg of diastolic BP (ΔP)
👉 Requires urgent fasciotomy
Vascular Injury Assessment
- Measure Ankle-Brachial Index (ABI): Normal: >0.9
Indications for Angiography
- ABI <0.9
- Knee dislocation
- Pale/cool limb with poor perfusion
- High-energy injuries near major vessels
Classification Systems
1. Gustilo-Anderson Classification
Most widely used system:
| Type | Characteristics |
|---|---|
| I | <1 cm, clean, minimal damage |
| II | >1 cm, moderate soft tissue injury |
| IIIA | Severe injury but adequate bone coverage |
| IIIB | Bone exposed, requires flap coverage |
| IIIC | Associated vascular injury requiring repair |
⚠️ Final classification is made after surgical debridement
2. Tscherne Classification (Open Fractures)
| Grade | Description |
|---|---|
| I | Small wound, low contamination |
| II | Moderate soft tissue injury |
| III | Extensive damage + contamination |
| IV | Partial/complete amputation |
Emergency Management
Initial Steps
- Control bleeding (direct pressure)
- Sterile dressing
- Splinting / provisional reduction
- Start IV antibiotics early (critical step)
Antibiotic Protocol
| Fracture Type | Antibiotic |
|---|---|
| Type I & II | 1st-gen cephalosporin |
| Type III | Add aminoglycoside |
| Farm injuries | Add penicillin |
Tetanus Prophylaxis
- Toxoid ± immunoglobulin depending on vaccination history
Operative Management
1. Irrigation & Debridement (MOST IMPORTANT)
Principles:
- Extend wound to assess injury zone
- Remove:
- Necrotic tissue
- contaminants
- Preserve:
- viable muscle, tendons
Muscle Viability Criteria
- Color (red)
- Consistency (firm)
- Bleeding
- Contractility
Irrigation Strategy
- High-volume saline lavage
- Low-pressure preferred (less tissue damage)
2. Wound Management
Options:
- Primary closure (selected cases)
- Delayed closure
- VAC (vacuum-assisted closure)
- Skin grafts or flaps
3. Fracture Stabilization
Options:
- External fixation
- Internal fixation
- Intramedullary nailing
Goals:
- Protect soft tissue
- Enable early mobilization
- Improve healing
4. Soft Tissue Coverage & Bone Grafting
- Performed after wound is clean
- Options:
- Skin grafts
- Rotational flaps
- Free flaps
5. Limb Salvage vs Amputation
Indications for Amputation
- Irreparable vascular injury
- Warm ischemia >8 hours
- Severe crush injury
- Life-threatening systemic risk
👉 Decision is individualized; scoring systems (e.g., MESS) are not fully reliable
Complications
1. Infection
- Cellulitis
- Osteomyelitis
Risk factors:
- Severe contamination
- Delayed treatment
- Poor soft tissue coverage
2. Compartment Syndrome
- May lead to permanent disability
- Requires early detection + fasciotomy
3. Nonunion & Delayed Healing
- Due to:
- Soft tissue loss
- infection
- poor vascularity
Key Clinical Pearls
- 🚨 Treat all suspicious wounds near fractures as open fractures
- 💉 Early IV antibiotics = most effective infection prevention
- 🔪 Surgical debridement is the cornerstone of treatment
- ⚠️ Open fracture ≠ protection from compartment syndrome
- 🦴 Soft tissue condition is more important than wound size
References & More
- Rockwood & Green’s Fractures in Adults, 9th Edition
- Advanced Trauma Life Support (ATLS) guidelines
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Sop JL, Sop A. Open Fracture Management. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Dheenadhayalan J, Nagashree V, Devendra A, Velmurugesan PS, Rajasekaran S. Management of open fractures: A narrative review. J Clin Orthop Trauma. 2023 Sep 1;44:102246. doi: 10.1016/j.jcot.2023.102246. PMID: 37720489; PMCID: PMC10502353. Pubmed
- Whiting PS, Obremskey W, Johal H, Shearer D, Volgas D, Balogh ZJ. Open fractures: evidence-based best practices. OTA Int. 2024 May 3;7(3 Suppl):e313. doi: 10.1097/OI9.0000000000000313. PMID: 38708043; PMCID: PMC11064778. Pubmed