Elbow dislocation accounts for 25% of elbow injuries, mostly occurs in adolescent population as a result of a direct injury by a fall on the outstretched arm. In uncomplicated dislocations, conservative treatment is usually successful.
The more common type is posterior elbow dislocation which occurs as a result of a fall on the outstretched arm when the olecranon is driven back out of the trochlear fossa. The less common is anterior elbow dislocation which occurs as a result of a direct blow on the olecranon when the elbow is in a partially flexed position.

Related Anatomy
The elbow is a complex of three joints, the ulnohumeral, radiohumeral and proximal radioulnar joints, which together provide a flexion range of 0–150° and a pronation– supination arc of 85° from the neutral. The stability of the joint is provided by the congruity of bony structures, surrounding muscles and ligamentous constraints.
The medial collateral ligament (MCL) is the main medial stabilizer resisting a valgus stress, whereas the lateral stability is provided by the lateral ulnar collateral ligament and the anconeus muscle along with the radial head.
See Also: Elbow Anatomy
Clinical Features and Signs of a Dislocated Elbow
Recognizing the signs of a dislocated elbow is crucial for rapid diagnosis and appropriate management:
Pain and Visible Deformity
- Severe acute pain localized to the elbow, often aggravated by movement
- Noticeable deformity or irregular joint contour with inability to actively move the elbow
Functional Loss
- Complete loss of normal range of motion
- Difficulty in flexion and extension of the elbow joint
Swelling, Bruising, and Instability
- Rapid onset of swelling due to soft tissue disruption
- Ecchymosis and warmth around the joint
- Sensation of instability or “looseness” when attempting motion
Neurological and Vascular Signs
- Paresthesia (numbness, tingling) in the forearm or hand
- In rare cases, signs of vascular compromise
A thorough neurovascular assessment is mandatory both before and after reduction to avoid missed injury to adjacent nerves or vessels.
Prominent Bony Landmarks
In elbow posterior dislocations, the olecranon often appears unusually prominent and displaced posteriorly relative to the distal humerus—a physical finding characteristic of this injury.
A thorough examination is essential to check for neurovascular injury, including damage to nearby nerves or blood vessels. This assessment should be performed both before and after reduction of the elbow dislocation. Clinicians must also carefully evaluate for associated fractures, particularly involving the olecranon, radial head, or coronoid process of the ulna, which can accompany elbow dislocations and affect management.
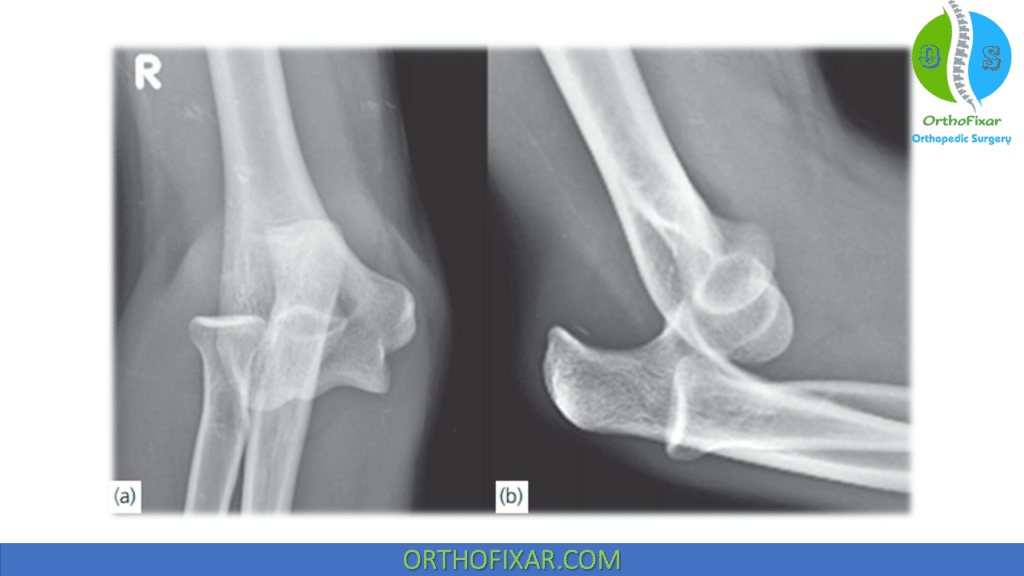
Radiology
The standard anteroposterior and lateral radiographs of the elbow will reveal the type of dislocation and should be scrutinized for other associated fractures.
Based on the direction of the displacement of the ulna relative to the humerus, the dislocation is termed posterior, anterior, lateral, medial and divergent.
Patients with suspected intraarticular fractures, persistent instability and incongruous reduction need to be further evaluated with a CT scan.

Fracture dislocations of the elbow joint
Elbow dislocations can be associated with fractures around the joint. The radial head is fractured in 10% of patients, and the medial or lateral epicondyle can be avulsed in 15–20% of patients.
In children, the medial epicondyle can become trapped in the joint space during the process of reduction and result in an incongruent reduction. The coronoid process can be fractured by avulsion of the brachial muscle or, rarely, by a direct injury of the coronoid over the trochlear notch.
Elbow dislocations that are associated with one or more intra-articular fractures are at a greater risk for recurrent or chronic instability.
Patients in whom excision of the radial head is performed in the acute stage have a risk of re-dislocation. They must be stabilized in such cases either by cross-pinning the joint or by an external fixator.
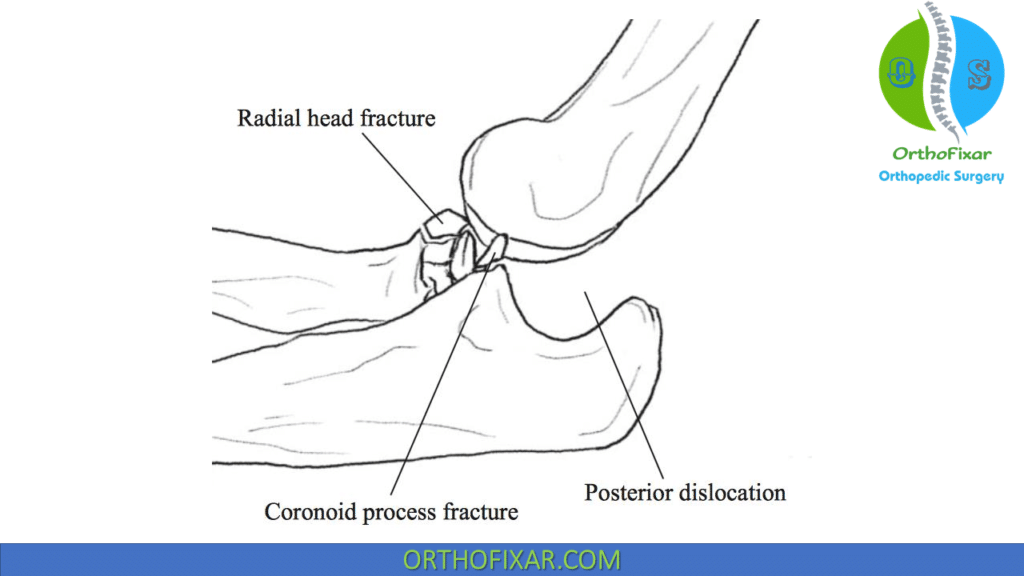
Elbow posterior dislocation with fractures of the radial head and coronoid process and disruption of the MCL is called the ‘terrible triad injury’ and such patients have very unstable elbows. This condition is managed surgically with fixation of the coronoid, repair or replacement of the radial head, and medial collateral ligament repair.
Elbow Dislocation Management
Dislocations without associated fractures are usually treated by reducing the joint under a regional block or a short intravenous regional anesthesia. The neurovascular status should be reassessed, followed by evaluation of stability.
The elbow is splinted for 2–3 weeks, then physical therapy for dislocated elbow is started. The associated ligamentous injuries will heal spontaneously, restoring the stability of the joint.
Post-reduction instability or an incongruent reduction must raise suspicion of associated fractures, loose bodies and severe ligamentous injuries.
Elbow dislocation surgery is indicated in complex fracture dislocations and when the elbow cannot be held in a concentrically reduced position, when it re-dislocates or when the dislocation is deemed unstable. Here stability is achieved by open reduction and internal fixation and repair of soft tissues.
Complications
The complications that may occur after elbow joint dislocation include:
- Loss of a few degrees of extension can occur, especially in dislocations associated with soft-tissue injuries.
- In severe cases and in patients with associated head injuries, formation of heterotopic bone leading to myositis ossificans is a potential complication.
- Owing to the close proximity of vital neurovascular structures, acute dislocations can be associated with injuries to the brachial artery and the median nerve.
References & More
- Layson J, Best BJ. Elbow Dislocation. [Updated 2022 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK549817/
- Waymack JR, An J. Posterior Elbow Dislocation. [Updated 2022 Oct 30]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470574/
- Layson J, Best BJ. Elbow Dislocation. 2022 Aug 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 31747224.
- Mercer’s Textbook of Orthopaedics and Trauma, Tenth edition.
- Terrible Triad Injury of Elbow – Orthobullets