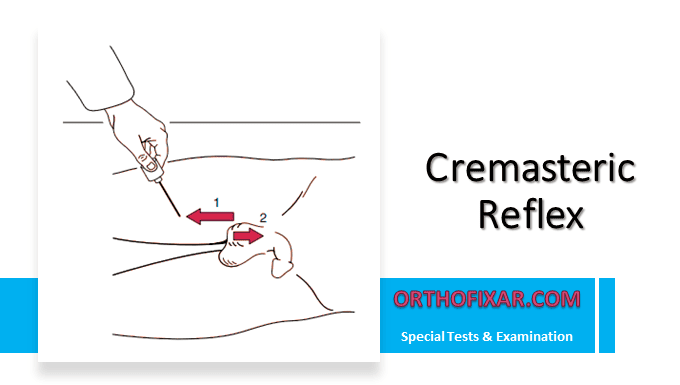
The cremasteric reflex is a superficial cutaneous‑muscular reflex that causes elevation of the testis when the inner thigh (or the superior scrotal skin) is gently stroked. In men, it is one of the three “genital reflexes” (the other two are the bulbocavernosus and the anal wink) that are routinely examined in a neurological bedside exam.
Although simple, the cremasteric reflex provides a quick, non‑invasive window into the integrity of the L1‑L2 spinal cord segments, the genitofemoral nerve, and the peripheral motor pathways that innervate the cremaster muscle.
The cremasteric reflex is particularly useful in assessing neurological function:
- Absent or reduced bilaterally: may indicate an upper motor neuron lesion.
- Absent unilaterally: suggests a lower motor neuron lesion affecting the L1–L2 spinal segments or the genitofemoral nerve on that side.
- The absence of this reflex gains additional significance if associated with increased deep tendon reflexes, further supporting the presence of an upper motor neuron lesion.
Related Anatomy
The cremaster muscle is a paired structure made of thin layers of striated and smooth muscle. The muscle has 2 parts, a lateral and medial cremaster muscle. The lateral muscle originates from the internal oblique muscle and inguinal ligament, and the medial cremaster muscle usually originates from the pubic tubercle but sometimes from the lateral pubic crest. The muscles that are covered by a fascia loop over the spermatic cord and testicles and insert into the testicle tunica vaginalis. In the female, the cremaster muscle is found on the round ligament.
The innervation for the cremasteric reflex is provided by the sensory and motor fibers of the genitofemoral nerve that originates from the L1 and L2 spinal nerve nuclei.
See Also: Lumbar Plexus Anatomy
| Component | Pathway | Clinical relevance |
|---|---|---|
| Afferent limb | Sensory fibers of the genital branch of the genitofemoral nerve (L1‑L2) travel from the skin of the upper inner thigh/scrotum to the dorsal root ganglion. | Damage to this branch (e.g., inguinal hernia repair) abolishes the reflex on the affected side. |
| Central integration | Synapse at the L1–L2 spinal cord gray matter; the interneuronal circuit is short and spinal‑mediated. | A lesion of the spinal cord at or above L1 (e.g., traumatic spinal cord injury) leads to a bilateral loss. |
| Efferent limb | Motor fibers of the genital branch of the genitofemoral nerve travel back to the cremaster muscle surrounding the spermatic cord. | Peripheral neuropathies (e.g., diabetic polyneuropathy) may attenuate the reflex. |
How to Perform the Cremasteric Reflex?
- The patient lies supine and relaxed, with the thighs slightly abducted; the penis is gently retracted to expose the scrotum.
- Using a warm cotton‑tip applicator (or the examiner’s fingertip), lightly stroke the superior medial thigh (inner thigh) from lateral to medial, or directly rub the superior scrotal skin. Avoid pinching or deep pressure.
- Within 1–2 seconds, the ipsilateral testis should rise (cremasteric contraction).
- Test each side separately; note latency, symmetry, and quality (full rise vs. subtle twitch).
See Also: Deep Tendon Reflex Testing
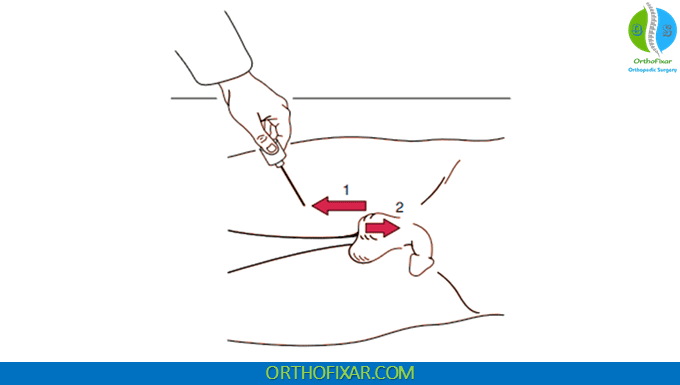
What is the Positive Cremasteric Reflex?
A normal or positive response is a contraction of the cremaster muscle, which causes the scrotal sac on the tested side to elevate. This reaction occurs because of a reflex arc involving:
- Afferent limb: the femoral branch of the genitofemoral nerve (L1)
- Efferent limb: the genital branch of the genitofemoral nerve (L2)
Bilateral absence or reduction of the cremasteric reflex may suggest:
- An upper motor neuron (UMN) lesion, which could indicate damage to the brain or spinal cord above the reflex arc
Unilateral absence (missing on only one side) may suggest:
- A lower motor neuron (LMN) lesion affecting the nerve roots between L1 and L2 (first and second lumbar vertebrae)
- This could indicate damage to the peripheral nerves, nerve roots, or anterior horn cells at this level.
Clinical Significance
Neurological Examination
- ISNCSCI (International Standards for Neurological Classification of Spinal Cord Injury) lists the cremasteric reflex as a key motor test for L1‑L2 integrity in males.
- Absent bilateral reflex → suggests an incomplete spinal cord injury above L1 or severe central nervous system disease.
- Unilateral loss → points to a localized peripheral lesion (e.g., postoperative genitofemoral nerve injury).
Acute Scrotum & Testicular Torsion
- The reflex is absent in 70‑80 % of surgically confirmed testicular torsion while preserved in most cases of epididymitis or hydrocele.
- Sensitivity ranges from 70–85 % and specificity ≈ 92 % when combined with other signs (e.g., high‑driving test, absent Prehn’s sign).
- Clinical tip: In an equivocal acute scrotum, a present cremasteric reflex does not rule out torsion, but a absent reflex raises the index of suspicion and should expedite scrotal ultrasound.
Inguinal Hernia & Post‑operative Nerve Damage
- Iatrogenic transection or stretch of the genital branch of the genitofemoral nerve during open or laparoscopic hernia repair can lead to a persistent unilateral loss of the reflex.
- Documenting the reflex pre‑ and post‑operatively helps differentiate surgical neuropathy from other causes of testicular pain.
Multiple Sclerosis (MS) & Demyelinating Disease
- Studies correlating MRI‑confirmed spinal cord plaques (L1‑L2) with genital reflex testing report a significant association between absent/diminished cremasteric reflexes and cervical‑to‑thoracic cord lesions.
- Reflex testing can therefore complement standard disability scales (e.g., EDSS) when evaluating lower‑thoracic involvement.
Peripheral Neuropathy (Diabetes, Alcoholic Neuropathy)
- In diabetic men, the cremasteric reflex may be reduced or delayed in proportion to the severity of symmetrical peripheral neuropathy.
- This reflex is a quick bedside adjunct to formal nerve conduction studies, especially in resource‑limited settings.
Geriatric & Age‑Related Changes
- Age‑related decline in peripheral nerve conduction velocity can blunt the reflex in older adults, but a new loss should still prompt evaluation for lumbar spinal stenosis, degenerative spondylolisthesis, or new peripheral nerve injury.
References & More
- Hoppenfeld S. Physical Examination of the Spine and Extremities. New York: Appleton-Century-Crofts; 1976.
- Orthopedic Physical Assessment by David J. Magee, 7th Edition.
- Mellick LB, Mowery ML, Al-Dhahir MA. Cremasteric Reflex. [Updated 2023 Apr 19]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: PubMed