What is Neurogenic Shock?
Neurogenic shock is a life-threatening type of distributive shock characterized by loss of sympathetic vascular tone, leading to severe hypotension and inadequate tissue perfusion. It most commonly occurs following acute spinal cord injury, particularly at or above the T6 level.
Unlike other forms of shock, neurogenic shock is unique because it often presents with bradycardia instead of tachycardia, due to unopposed parasympathetic activity.
Causes of Neurogenic Shock
The primary cause is spinal cord injury, but other less common etiologies include:
- Cervical or upper thoracic spinal trauma (most common)
- Spinal anesthesia
- Transverse myelitis
- Guillain-Barré syndrome
- Central nervous system depressant toxins.
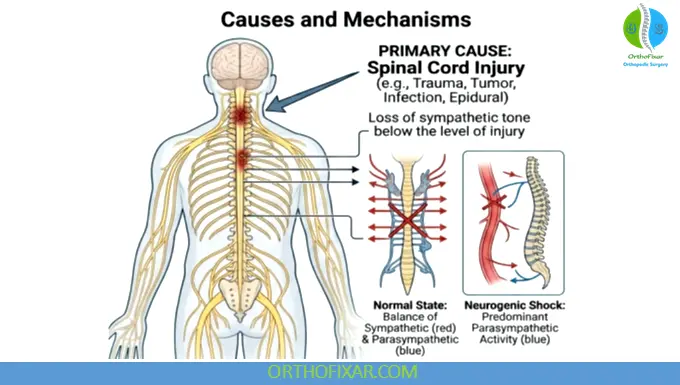
Pathophysiology
Neurogenic shock results from disruption of descending sympathetic pathways in the spinal cord.
Key Mechanisms:
- Loss of sympathetic tone → vasodilation
- Reduced systemic vascular resistance → hypotension
- Unopposed vagal tone → bradycardia
- Peripheral blood pooling → decreased venous return
This leads to organ hypoperfusion and cellular hypoxia, which can rapidly become fatal if untreated.
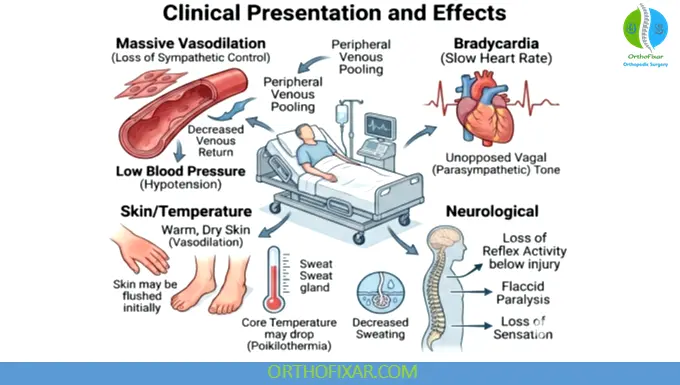
Clinical Features
Classic Triad:
- Hypotension
- Bradycardia
- Warm, dry skin (due to vasodilation)
Other Signs:
- Altered mental status
- Hypothermia (impaired thermoregulation)
- Reduced urine output
- Possible respiratory compromise (especially with cervical injury)
Neurogenic shock must be differentiated from spinal shock, which refers to temporary loss of reflexes and motor function, not hemodynamic instability.
Diagnosis
Diagnosis is primarily clinical, supported by:
- History of trauma or spinal injury
- Persistent hypotension without evidence of hypovolemia
- Bradycardia (key distinguishing feature)
Investigations:
- Imaging (CT/MRI of the spine)
- Hemodynamic monitoring
- Exclusion of other shock types (e.g., hemorrhagic shock)
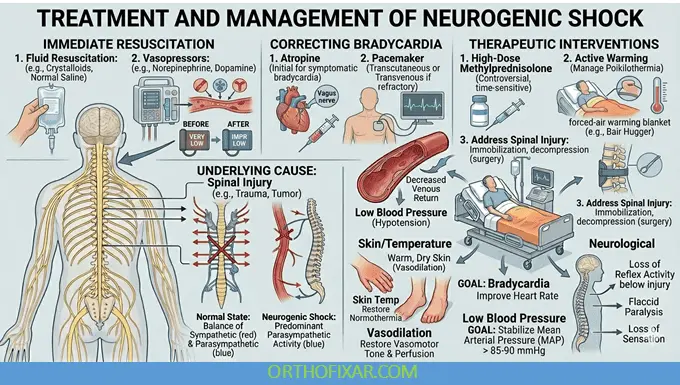
Neurogenic Shock Treatment
1. Initial Stabilization (ABCDE Approach)
- Airway protection
- Breathing support (oxygen/ventilation)
- Circulation management
- Disability: Evaluate neurological status with Glasgow Coma Scale (GCS).
- Exposure/Environment
- In addition to spinal immobilization.
See Also: Glasgow Coma Scale (GCS)
2. Fluid Resuscitation
- First-line of treatment
- Careful administration to avoid fluid overload.
3. Vasopressors
Used when hypotension persists:
- Phenylephrine (α1 agonist → vasoconstriction)
- Norepinephrine (commonly used in ICU)
Goal: restore vascular tone and maintain perfusion
4. Heart Rate Management
- Atropine for severe bradycardia
- Temporary pacing in refractory cases
5. Definitive Care
- Early spinal stabilization
- ICU monitoring
- Multidisciplinary management (trauma, neurosurgery, ICU)
Complications
- Persistent hypotension
- Organ failure
- Autonomic dysreflexia (late complication)
- Deep vein thrombosis (DVT).
Neurogenic Shock vs Other Types of Shock
| Feature | Neurogenic Shock | Hypovolemic Shock | Septic Shock |
|---|---|---|---|
| Heart Rate | ↓ Bradycardia | ↑ Tachycardia | ↑ Tachycardia |
| Skin | Warm, dry | Cold, clammy | Warm (early) |
| Cause | Spinal cord injury | Blood/fluid loss | Infection |
| SVR | ↓ | ↑ | ↓ |
Prognosis
Prognosis depends on:
- Level and severity of spinal injury
- Speed of recognition and treatment
- Associated trauma
Early aggressive management significantly improves outcomes.
Key Takeaways
- Neurogenic shock is a distributive shock caused by loss of sympathetic tone
- Classic signs: hypotension + bradycardia + warm skin
- Most commonly due to high spinal cord injury (above T6)
- Management focuses on hemodynamic stabilization and vasopressors
References & More
- Dave S, Dahlstrom JJ, Weisbrod LJ. Neurogenic Shock. 2023 Oct 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan–. PMID: 29083597. (PubMed)
- Dave S, Dahlstrom JJ, Weisbrod LJ. Neurogenic Shock. [Updated 2023 Oct 29]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: (PubMed)
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.

[…] See Also: Neurogenic Shock: Causes, Symptoms & Treatment […]