Brown-Séquard syndrome (BSS) is a rare but classic incomplete spinal cord injury caused by hemisection (damage to one side) of the spinal cord. It produces a distinctive neurological pattern that is highly testable and clinically important.
Despite its textbook clarity, pure Brown-Séquard syndrome is uncommon—most real cases present with mixed or incomplete features.
Pathophysiology
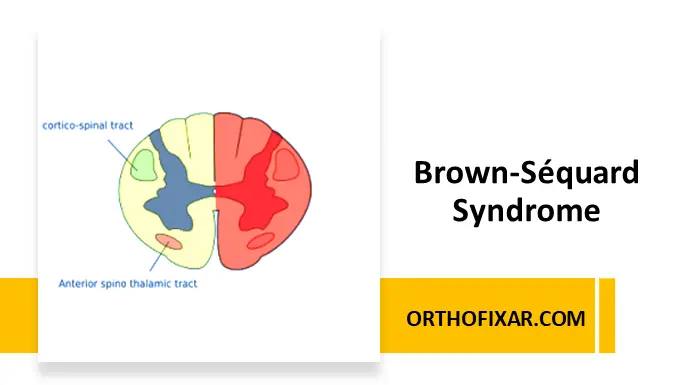
The syndrome results from damage to one half of the spinal cord, disrupting major neural pathways:
- Corticospinal tract → motor function
- Dorsal columns → proprioception & vibration
- Spinothalamic tract → pain & temperature
Because these tracts cross at different levels, the neurological deficits are asymmetrical.
Classic Neurological Pattern
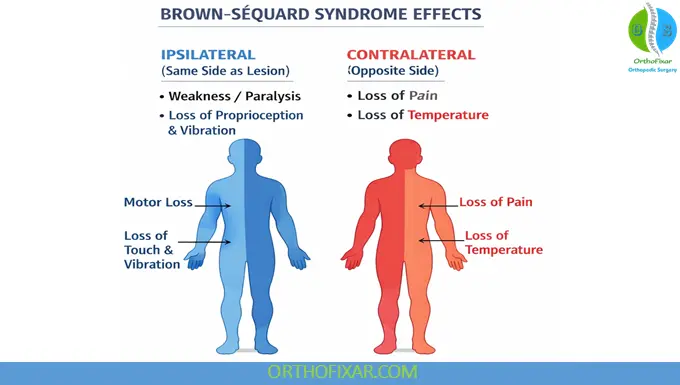
- Ipsilateral (same side as lesion):
- Weakness or paralysis
- Loss of proprioception and vibration
- Contralateral (opposite side):
- Loss of pain and temperature sensation
This unique dissociation is the hallmark of Brown-Séquard Syndrome.
Etiology
1. Traumatic Causes (Most Common)
- Penetrating injuries (stab wounds, gunshots)
- Blunt trauma (motor vehicle accidents, falls)
- Vertebral fractures
2. Non-Traumatic Causes
- Intervertebral disc herniation
- Spinal tumors or cysts
- Degenerative conditions (e.g., cervical spondylosis)
- Demyelinating diseases (e.g., multiple sclerosis)
- Vascular causes (ischemia, hemorrhage)
- Infections (e.g., tuberculosis, herpes zoster)
Trauma accounts for the majority of Brown-Séquard Syndrome cases.
See Also: Neurogenic Shock: Causes, Symptoms & Treatment
Clinical Features
Motor Findings
- Ipsilateral upper motor neuron weakness below the lesion
- Possible lower motor neuron signs at the level of injury
Sensory Findings
- Ipsilateral loss of:
- Proprioception
- Fine touch
- Vibration
- Contralateral loss of:
- Pain
- Temperature
Symptoms typically begin below the level of injury and vary depending on lesion location.
See Also: Dermatome Distribution for Upper & Lower Limbs
Diagnosis
Clinical Diagnosis
Primarily based on the classic neurological pattern.
Imaging
- MRI (gold standard)
- Identifies cord hemisection
- Detects underlying causes (tumor, disc, hemorrhage)
Additional Tests
- CT scan (trauma cases)
- Laboratory tests (infection/inflammation suspected)
Treatment
Acute Treatment
- Stabilization of spine
- High-dose corticosteroids (selected cases)
- Surgical intervention (if compression present)
Definitive Treatment
Depends on underlying cause:
- Tumor → surgical resection
- Infection → antibiotics/antivirals
- MS → immunotherapy
Rehabilitation
- Early physiotherapy is critical
- Multidisciplinary care improves outcomes
Prognosis
Brown-Séquard syndrome has one of the best prognoses among spinal cord injuries:
- Up to 90% of patients regain the ability to walk
- Recovery depends on:
- Cause of injury
- Severity
- Timing of treatment
Early intervention significantly improves outcomes.
Complications
If the Brown-Séquard Syndrome is untreated or severe:
- Spinal shock
- Deep vein thrombosis
- Pulmonary embolism
- Pressure ulcers
- Respiratory complications (high-level lesions)
Key Clinical Pearls
- Think “motor + proprioception same side, pain opposite side”
- Most cases are trauma-related
- MRI is essential for diagnosis
- Prognosis is better than most spinal cord syndromes
Conclusion
Brown-Séquard syndrome remains one of the most elegant neuroanatomical syndromes in clinical medicine. Its distinct presentation reflects the anatomical organization of spinal tracts and provides a powerful diagnostic clue.
Early recognition and targeted management are crucial, as functional recovery is often excellent compared to other spinal cord injuries.
References & More
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Shams S, Davidson CL, Arain A. Brown-Séquard Syndrome. [Updated 2024 Feb 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Shams S, Davidson CL, Arain A. Brown-Séquard Syndrome. 2024 Feb 27. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan–. PMID: 30844162. Pubmed