Fracture casting remains a cornerstone of non-operative orthopedic management. The primary goal of casting is to provide semirigid immobilization while minimizing the risk of pressure-related and skin complications. Proper technique is essential, particularly in the acute setting where swelling and soft tissue injury may increase the risk of adverse outcomes.
General Principles of Casting
Fracture Casting must balance stability with safety. While immobilization supports fracture healing, excessive pressure or poor technique can lead to serious complications.
Key Objectives
- Maintain fracture alignment
- Provide adequate immobilization
- Avoid pressure injury and neurovascular compromise
- Accommodate swelling in acute injuries
Caution: Fracture Casting should be used carefully in acute fractures due to the risk of swelling and soft tissue complications.
Padding Technique
Proper padding is critical to prevent pressure necrosis and improve patient comfort.
- Apply padding from distal to proximal
- Maintain 50% overlap
- Use a minimum of two layers
- Add extra padding over bony prominences:
- Fibular head
- Malleoli
- Patella
- Femoral condyles
- Olecranon
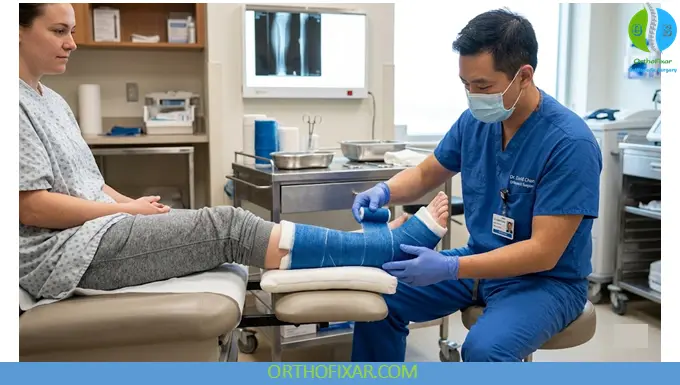
Plaster Application
Plaster remains widely used due to its excellent molding characteristics.
Best Practices
- Use room temperature water for optimal handling
- Cold water increases molding time
- Avoid hot water, as it may cause thermal skin injury
Recommended Widths
- Thigh: 5-inch
- Leg: 4–5 inch
- Arm: 3–4 inch
- Forearm: 2–4 inch
Fiberglass Casting
Fiberglass is increasingly preferred in many settings.
Advantages
- More resistant to moisture and breakdown
- 2–3 times stronger than plaster for the same thickness
- Lighter and more durable
Limitations
- More difficult to mold precisely
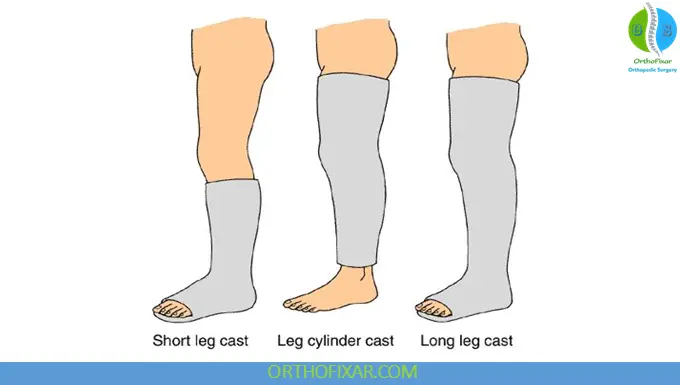
Below-Knee (Short Leg) Cast
Short Leg Cast is used for distal tibia, ankle, and foot injuries.
Technique
- Support the metatarsal heads
- Position the ankle in neutral
- Apply with the knee flexed
- Ensure toe mobility
- Build up the plantar surface for walking casts
Key Considerations
- Pad the fibular head and plantar foot
- Fiberglass is preferred for durability
Above-Knee (Long Leg) Cast
Long Leg Cast provides immobilization for tibial shaft and knee-related injuries.
Technique
- Begin with below-knee application
- Maintain knee flexion at 5–20 degrees
- Mold the supracondylar femur for rotational stability
- Add extra padding anterior to the patella
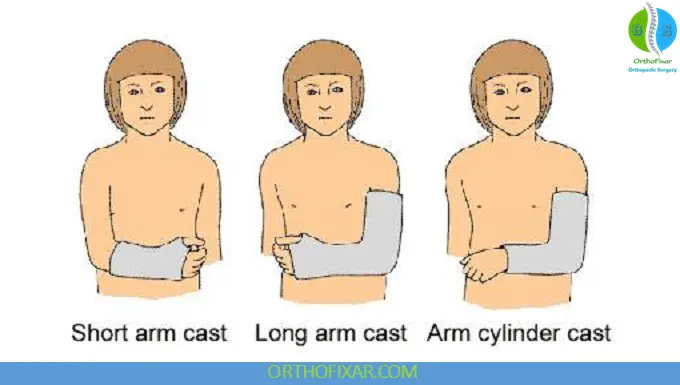
Short and Long Arm Casts
Used for fractures of the forearm, wrist, and elbow.
Positioning Guidelines
- Keep MCP joints free
- Do not extend beyond the proximal palmar crease
- Leave the thumb free to the base of the metacarpal
- Allow thumb opposition to the fifth digit
Technique Tips
- Apply even pressure for optimal molding
- Use only the heels of the palms to mold
- Avoid finger pressure to prevent pressure points
Complications of Fracture Casts and Splints
Despite proper technique, complications can occur and require vigilance.
Mechanical Complications
- Loss of fracture reduction
- Joint stiffness (minimize by leaving joints free when possible)
Pressure-Related Complications
- Pressure necrosis (can occur within 2 hours)
- Tight casts leading to compartment syndrome
Pressure Reduction Techniques
- Univalving: ~30% pressure reduction
- Bivalving: ~60% pressure reduction
- Cutting padding further reduces pressure
- Use of cast spreaders significantly lowers contact pressure
Thermal Injury
- Avoid plaster thicker than 10 ply
- Use water below 24°C
- Rare with fiberglass
Iatrogenic Injuries
- Cuts or burns during cast removal due to poor technique
Thromboembolic Risk
- Increased risk with lower extremity immobilization
- Pulmonary embolism and thrombophlebitis are concerns
- Upper extremity risk may be up to 0.7%
- Prophylaxis remains debated
Functional Positioning
When joints cannot be left free:
- Immobilize in a functional position
- Example: hand in intrinsic-plus position
Conclusion
Fracture casting is both an art and a science. Successful outcomes depend on meticulous technique, proper material selection, and careful monitoring for complications. Clinicians must remain vigilant, especially in the early phases after application, to ensure patient safety and optimal healing.
References & More
- Egol KA. Handbook of fractures. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2019.
- Liu DS, Bauer AS. Upper Extremity Cast Application. J Pediatr Soc North Am. 2025 Jul 3;12:100240. doi: 10.1016/j.jposna.2025.100240. PMID: 40799459; PMCID: PMC12341709. Pubmed
- Ramalingam W, Lamer S. Lower Extremity Cast Application. J Pediatr Soc North Am. 2025 Jul 3;12:100236. doi: 10.1016/j.jposna.2025.100236. PMID: 40809517; PMCID: PMC12345343. Pubmed
- McGraw-Heinrich JA, Wall JC, Rosenfeld SB. Common Cast Complications. J Pediatr Soc North Am. 2025 Jul 3;12:100244. doi: 10.1016/j.jposna.2025.100244. PMID: 40791972; PMCID: PMC12336002. Pubmed

I am back again and again
Tur Scripti