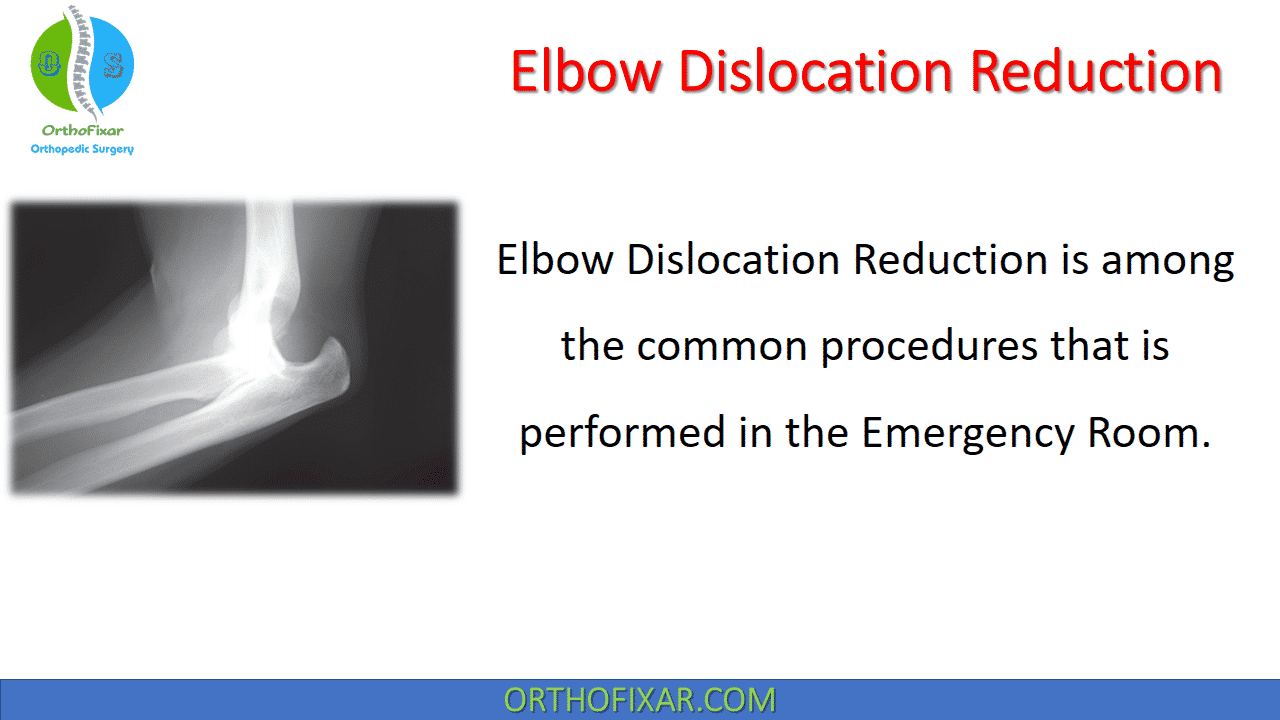
Elbow dislocation reduction procedure is among the most common procedures that is performed in the emergency room.
Elbow dislocations accounts for 20 percent of all traumatic dislocations. The elbow most commonly dislocates in the posterior or posterolateral direction. Posterior elbow dislocations are the most common dislocations in children less than ten years of age.
Elbow dislocations most commonly occur after a twisting injury or fall onto an outstretched arm and result in a ruptured capsule.
See Also: Elbow Anatomy
Elbow Dislocation Evaluation
When taking the history of the patient with a suspected elbow dislocation, it is important to note the following:
- mechanism of injury,
- the type and location of pain,
- the presence of any sensory,
- motor or vascular deficits,
- the time of injury,
- whether or not the patient has a history of a prior elbow injury.
When performing the physical examination, it is important to note the presence of gross deformity and the condition of the overlying soft tissue. The elbow should be evaluated for the presence of an effusion, put through a range of motion and undergo stability testing if possible. These findings should be compared to the uninjured contralateral side.
In an uninjured elbow, the medial and lateral epicondyles form an isosceles triangle with the olecranon. This anatomical triangle will not be present if the patient has a simple elbow dislocation (no fracture present) as the relationship between the olecranon and the epicondyles will be altered, and the olecranon process will become more prominent. There may also be an empty area medially.
Neurovascular injury is uncommon but a thorough evaluation is warranted and the evaluator should be alert for the development of compartment syndrome. Median nerve injury is rare and is characterized by severe pain that does not improve with the reduction. The patient will have difficulty in abducting the thumb and/or loss of sensation of the palmar aspect of the skin from the wrist to the tips of the lateral three and a half digits and dorsal aspect of the distal two-third of these same digits.
See Also: Lateral Pivot Shift Test of the Elbow
Elbow Dislocation Reduction Technique
After ruling out any associated elbow fractures, elbow dislocation reduction is necessary.
Steps for Elbow Reduction
- Ensure the patient has an adequate pain control. This may be done with an intra-articular anesthetic and/or pain medications. If these measures are ineffective, the patient may be put under conscious sedation.
- Remove clothing and jewelry from the affected limb.
- Place the patient in the supine position.
- Align the olecranon and distal humerus in the medial-lateral plane.
- Supinate the forearm.
- Apply upward traction across elbow while flexing the elbow to 90°.
- Have assistant apply counter traction and stabilize the humeral shaft.
- Place thumb on top of the patient’s olecranon process and lever the olecranon over the distal humerus with direct pressure. The force from the thumb should be directed upward and posterior while the arm is flexed up to 90°. A palpable “clunk” should be felt.
- Check stability by taking the elbow through a complete arc of motion.
- Confirm successful elbow reduction by checking for smooth and unrestricted arc of motion and realignment of the olecranon, medial and lateral epicondyles into the isosceles triangle.
- After confirming a stable and successful elbow reduction, apply a padded posterior splint to immobilize the elbow in approximately 90° flexion and forearm in neutral rotation.
- Post-reduction radiographs must confirm concentric ulnohumeral and radiocapitellar reductions.
- The splint can be discarded within 1 to 2 weeks. Make sure the splint extends far enough to support the wrist and keep the elbow above the heart to help reduce swelling.
- Patient should be re-evaluated by an orthopedic surgeon 7 to 10 days following the injury for re-evaluation of elbow stability and referral for physical therapy.


Posterior Long Arm Splint Application
After a successfully Elbow Dislocation Reduction, a Posterior Long Arm Splint should be applied.
Materials required are:
- plaster rolls of 8 to 10 sheets of 3 or 4 inches, depending on the patient’s size,
- 1 inch plaster roll,
- cotton undercast padding,
- a basin of lukewarm water,
- elastic bandages 3 to 4 inches wide,
- chux pads,
- trauma shears,
- bedsheet and stockinette.

Steps to apply the Posterior Long Arm Splint:
- Make sure the patient is comfortably positioned.
- Remove clothing and jewellery from the affected limb.
- Cover the patient with a sheet to protect him/her from splatter from the plaster.
- Flex the affected elbow to 90°, extend the wrist to 10 to 20° and keep the forearm in neutral position with the thumb up.
- Wrap the arm in cotton padding, starting distally and moving proximally, and overlapping each layer by half a width .
- The cotton padding should extend 2 to 3 cm beyond the plaster.
- Smooth out creases and wrinkles, as these can cause pressure and damage underlying soft tissue. Make sure to add extra padding to bony prominences of the elbow and wrist, epicondyles of the elbow, metacarpophalangeal joints and the base of the thumb. Remove excessive padding from cubital fossa.
- Measure the plaster by placing one end of a dry roll of plaster on the ulnar side of the affected arm, extending from the palmar crease to the proximal humerus. Add about 5 mm of extra plaster on either end, as plaster shrinks when it is wet. Pinch off this desired length and fold over the plaster. Unroll the rest of the plaster and fold over until there are total 8 to 10 layers. A supporting side slab is also measured out.
- Immerse the plaster in the room temperature water and squeeze out the excess water. Lay the plaster flat and smooth out the wrinkles and folds.
- Apply the wet plaster over the padding, starting on the ulnar side at the mid-metacarpals and continuing to the proximal humerus.
- Have the patient use the opposite hand to hold the distal end of the wet plaster. If the patient cannot do it, an assistant must be called in to do so.
- Smooth out the excess plaster at the elbow and mold it against the outside splint.
- Reinforce the splint with the supporting side slab extending from the mid-humerus to mid-forearm.
- Apply the elastic wrap over the wet plaster, starting distally and moving proximally. Do not wrap too tightly and ensure an adequate hole for the thumb.
- Mold the splint into the desired shape while the plaster is still wet and tell the patient to keep his or her hand, forearm, wrist and elbow immobile until the plaster dries.
- Inform the patient that he or she may feel some warmth as the splint dries. However, if the heat becomes too intense, remove the splint as thermal burns can occur.
- Check neurovascular function after the splint dries.

References
- Carter Sadie J, Carl A Germann, Angelo A Dacus, et al. “Orthopedic pitfalls in the ED: neurovascular injury associated with posterior elbow dislocations.” Am J Emerg Med. 2010;28(8):960-5. Epub 2010 Mar 12.
- De Haan J, Schep NW, Tuinebreijer WE, et al. Simple elbow dislocations: a systematic review of the literature. Arch Orthop Trauma Surg. 2010;130(2):241-9. Epub 2009 Apr 2.
- McGuire DT, Bain GI. Management of dislocations of the elbow in the athlete. Sports Med Arthrosc Rev. 2014 Sep;22(3):188-93. doi: 10.1097/JSA.0000000000000016. PMID: 25077749.