Hand Flexor tendon injury is among the most common cases represent to the Emergency Room, and it’s usually due to volar lacerations.
Flexor Tendon Anatomy
Muscles
Flexor digitorum profundus muscle (FDP):
- Flex the DIP joint and assists with PIP and MCP flexion.
- Its tendons insert on the base of the distal phalanx.
Flexor digitorum superficialis muscle (FDS):
- Flex the PIP joint and assists in MCP flexion.
- Its tendons insert on the base of the middle phalanx.
Flexor pollicis longus muscle (FPL):
- Flex the IP joint of the thumb.
- Its tendon insert on the base of the distal phalanx of the thumb.
Flexor carpi radialis muscle (FCR):
- It’s the primary wrist flexor.
- Inserts on the base of the second metacarpal.
Flexor carpi ulnaris muscle (FCU):
- It’s the primary wrist flexor.
- Inserts on the pisiform, hook of hamate, and the base of the 5th metacarpal.
See Also: Extensor compartments of the wrist
Blood supply
Tendon nutrition is believed to derive from two basic sources:
- The synovial fluid produced within the tenosynovial sheath.
- The blood supply provided through longitudinal vessels in the paratenon, intraosseous vessels at the tendon insertion, and vincular circulation.
Two zones of ischemia are present in the flexor digitorum profundus beneath the A2 pulley and beneath the A4 pulley.
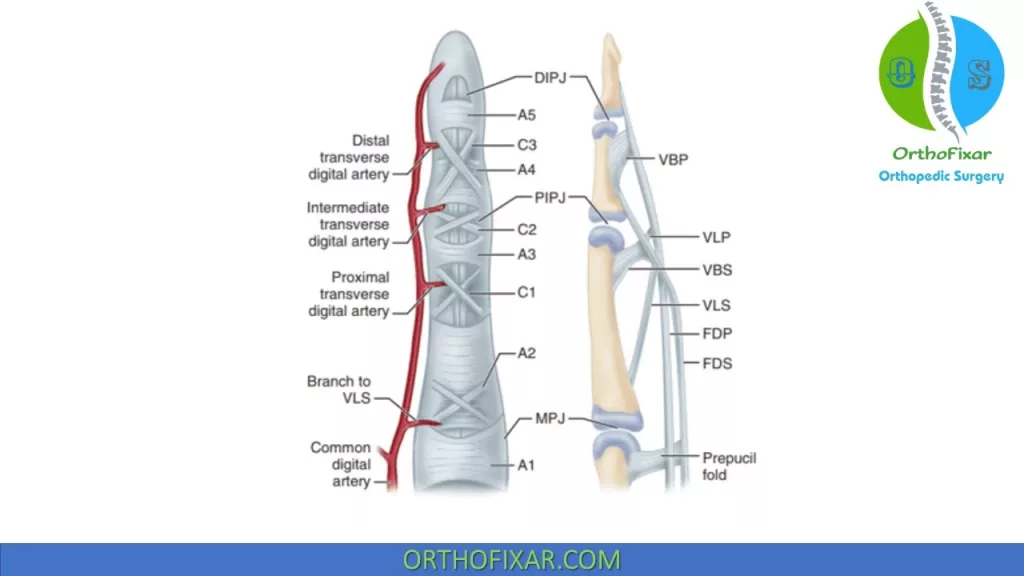
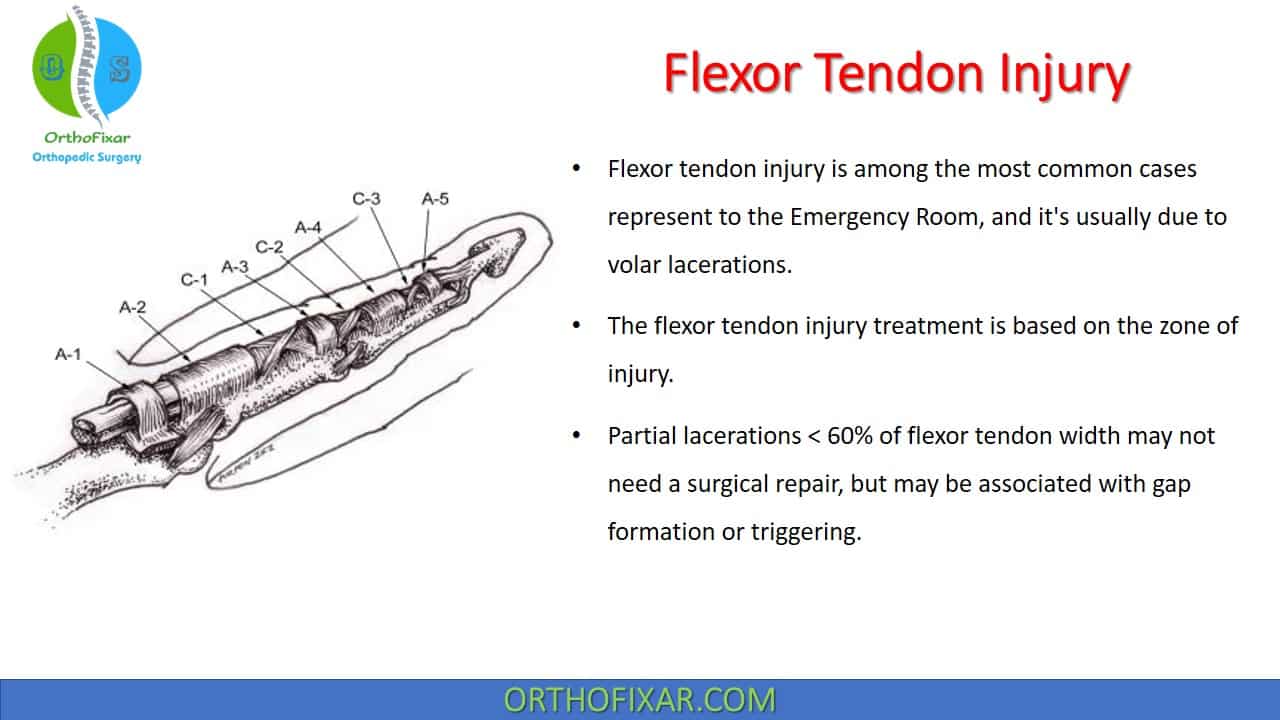
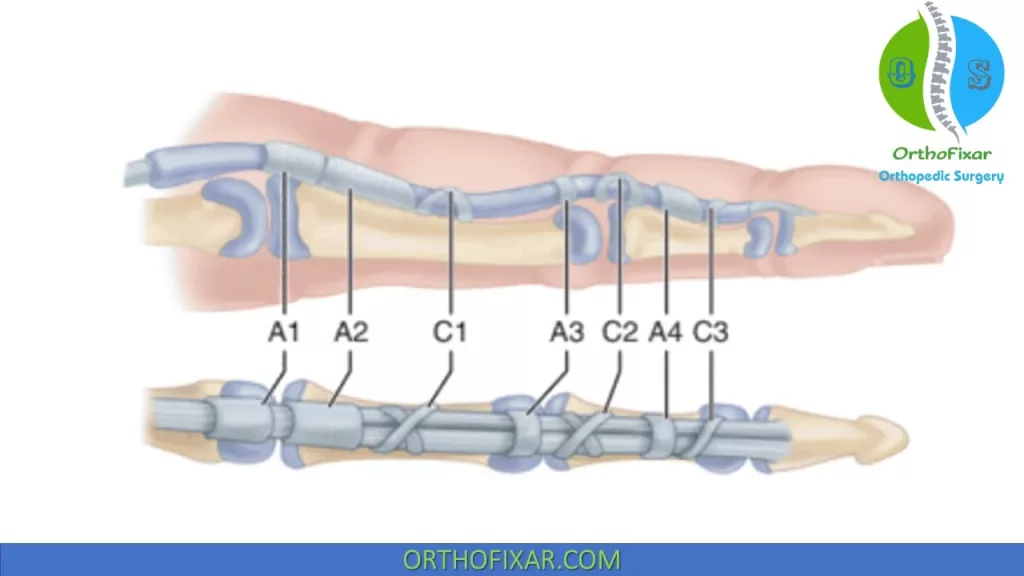
Pulley system
Every digit (except the thumb) has:
- 5 annular pulleys (A1 to A5).
- 3 cruciate pulleys (C1 to C3).
Thumb finger has:
- 2 annular pulley.
- Oblique pulley .
A2 and A4 are the most important pulleys to prevent flexor tendon bow-stringing.
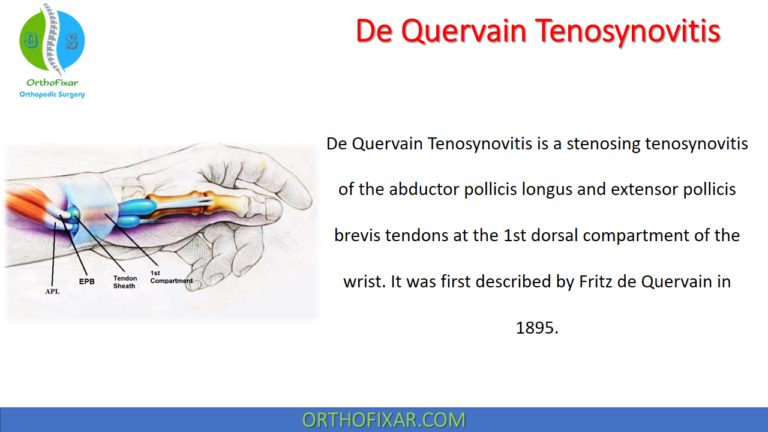
See Also: Trigger Finger (Stenosing tenosynovitis)
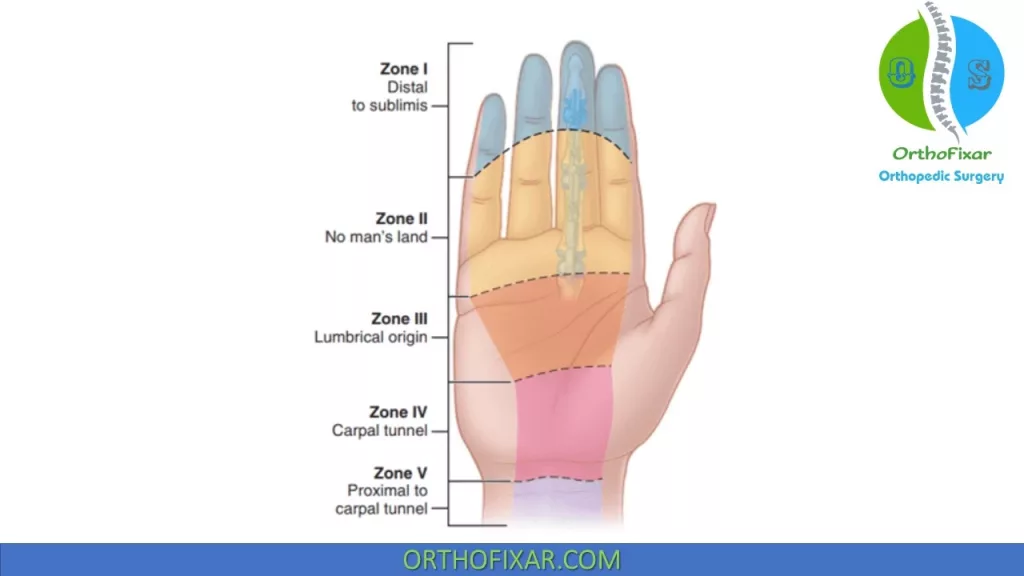
Flexor Tendon Zones (Verdan zones):
| Zone | Definition | Comments |
|---|---|---|
| I | Distal to FDS insertion | It’s injury called Jersey finger |
| II | From FDS insertion to distal palmar crease. | – FDP and FDS are in same tendon sheath. – historically had very poor results but results have improved due to advances in postoperative motion protocols |
| III | Palm | Often associated with neurovascular injury which carries a worse prognosis |
| IV | Carpal tunnel | Often complicated by postoperative adhesions |
| V | From Wrist to forearm | Often associated with neurovascular injury which carries a worse prognosis |
| Thumb | TI, TII, TIII | – Oblique pulley is more important than the A1 pulley. – Outcomes different than fingers. |
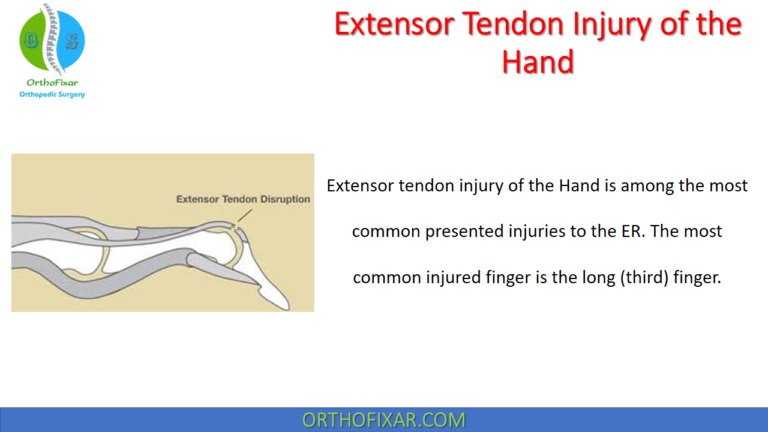
See Also: Extensor Tendon Injury of the Hand

Tendon Healing
Tendon healing after flexor tendon injury occurs through the activity of extrinsic and intrinsic mechanisms, occurring in three phases:
- Inflammatory: (48 to 72 hours) – Cellular proliferation.
- fibroblastic: (5 days to 4 weeks) – Fibroblastic proliferation with disorganized collagen.
- Remodeling: (4 weeks to about 3.5 months) – Linear collagen organization.
The extrinsic mechanism occurs through the activity of peripheral fibroblasts and seems to be the dominant mechanism contributing to the formation of scar and adhesions. Intrinsic healing seems to occur through the activity of the fibroblasts derived from the tendon.
Clinical Evaluation
Attempting to probe wounds acutely and note the resting posture of the hand and check the tenodesis effect with passive wrist flexion and extension. When both flexor tendons of a finger are severed, the finger lies in an unnatural position of hyperextension. Also assess the digital cascade.
Each digit is tested in isolation for active DIP and PIP flexion, especially in setting of multiple digit trauma.
Careful examination of the neurovascular status of the hand.
Gentle compression of the forearm muscle mass at times shows concomitant flexion of the joints of the uninvolved fingers, whereas the injured finger does not show this flexion.
If the wound is distal to the wrist, the injured finger should be stabilized to obtain specific joint movements. With the proximal interphalangeal joint stabilized, the flexor digitorum profundus is presumed injured if the distal interphalangeal joint cannot be actively flexed. If neither the proximal nor the distal interphalangeal joint can be actively flexed with the metacarpophalangeal joint stabilized, both flexor tendons probably are injured.
In the thumb flexor tendon injury, to check the integrity of the flexor pollicis longus tendon, the metacarpophalangeal joint of the thumb is stabilized: If the flexor pollicis longus tendon is divided, flexion at the interphalangeal joint is absent.
If a wound is located at the level of the wrist, the joints of a finger can be actively flexed even though the tendons to that finger are severed: This is the result of intercommunication of the flexor profundus tendons at the wrist, particularly in the little and ring fingers.
These maneuvers do not detect partially flexor tendon injury because a partially divided tendon usually is functional.
Treatment of Flexor Tendon Injury
The flexor tendon injury treatment is based on the zone of injury.
Partial lacerations < 60% of flexor tendon width may not need a surgical repair, but may be associated with gap formation or triggering.
Strickland stressed six characteristics of an ideal flexor tendon repair:
- Easy placement of sutures in the tendon,
- Secure suture knots,
- Smooth juncture of tendon ends,
- Minimal gapping at the repair site,
- Minimal interference with tendon vascularity,
- Sufficient strength throughout healing to permit application of early motion stress to the tendon.
In general, studies have shown that four-strand core suture with epidermis repair best accomplishes these objectives.
Suture Material
Most surgeons find that the braided polyester sutures (Ticron, Fiberwire, Mersilene)in the treatment of flexor tendon injury provide:
- Sufficient resistance to disrupting forces and gap formation.
- Handle easily.
- Have satisfactory knot characteristics: These sutures are widely used.
4-0 suture is estimated to be 66% stronger than 5-0 suture, and 3-0 suture 52% stronger than 4-0 suture.
3-0 suture may be useful to repair tendons in the forearm, palm, and larger digits, whereas a 4-0 suture may handle better in smaller digits.
Epitendinous repair usually is done with 5-0 or 6-0 monofilament suture (Prolene).
Suture Configurations
Flexor Tendon repair types:
Simple sutures:
- The suture pull is parallel to the tendon collagen bundles, transmitting the stress of the repair directly to the opposing tendon ends.
- The weakest and unsuitable in most tendon repairs.
Bunnell suture:
- Stress is transmitted directly across the juncture by the suture material and depends on the strength of the suture itself.
Pulvertaft technique (fish-mouth weave):
- Sutures are placed perpendicular to the tendon collagen bundles and the applied stress.
- The strongest type.
- Most suitable for tendon graft and tendon transfer junctures in the distal forearm and palm areas.
Four-strand, six-strand, and eight-strand core sutures:
- Create stronger repairs
- Reduce the possibility of gap formation.
- Permit greater forces to be applied to the repaired tendons.
- Allow earlier active motion than the traditional two-strand core sutures.
Continuous epitendinous sutures, placed circumferentially around the repair site, decrease the bulk of the repair site, minimizing the risk of triggering, enhances the strength of the core suture repair, and resists gap formation.
Peripheral sutures placed 2 mm from the repair site provide a stronger repair than placement of the sutures 1 mm from the repair site.
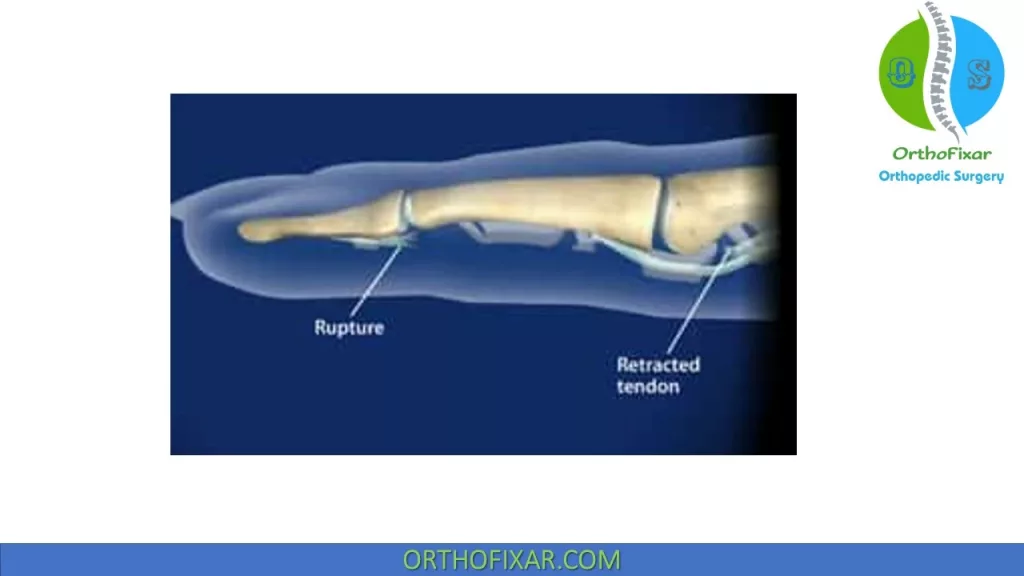
Zone I injury:
This zone injuries called “rugger jersey” finger, which is a closed FDP avulsion occurring distal to the FDS insertion. The ring finger is involved in 75% of cases.
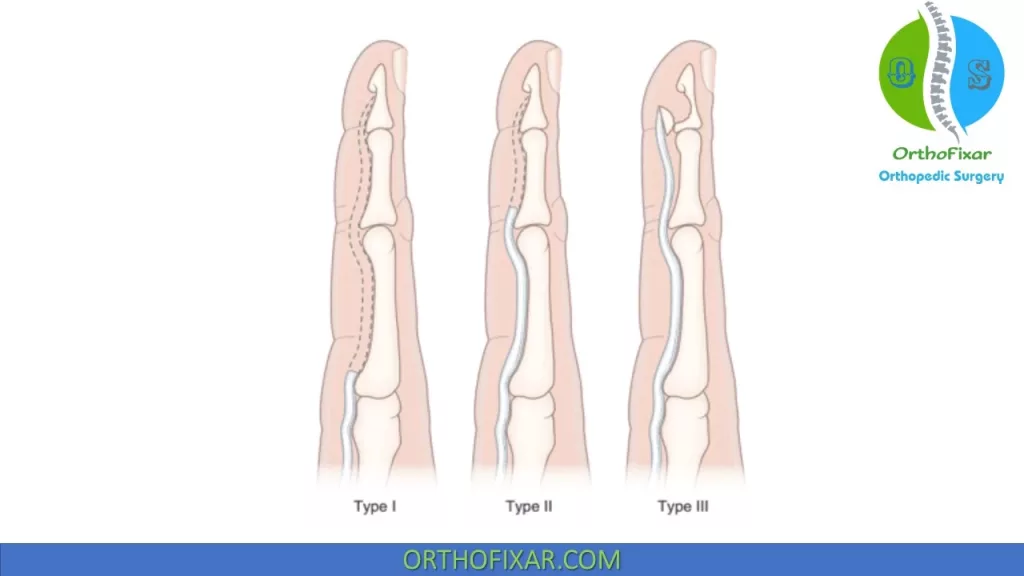
Leddy and Packer classification for zone I flexor tendon injury:
| Type | Description | Treatment |
|---|---|---|
| I | The FDP is retracted to the palm | This type require direct repair within 7 to 10 days. |
| II | FDP retracts proximal to the PIP joint. | May be directly repaired up to 6 weeks later because the intact vincula prevent FDP retraction proximal to the PIP joint. |
| III | Associated with small bony avulsion fragments with little retraction | May be successfully repaired up to 6 weeks after injury |
Quadrigia effect or DIP joint flexion contracture occurs when profundus advancement of 1 cm or more.
A pull-out wire technique can be used to attach the proximal tendon end to its distal stump, or directly to the bone after advancement.

Zone II injury:
It’s called “No man’s land” historically because of the poor results of treatment in this zone historically, and attribution to the high rate of adhesion formation at the pulleys and associated digital neurovascular injuries.
Nowadays, advances in postoperative rehabilitation have improved the clinical outcomes:
- Both the FDS and FDP may be injured in this zone.
- Tendon lacerations may be at a different level than the skin laceration, depending on the position of the finger when the laceration occurred.
- Direct repair of both tendons with a core and epitendinous suture technique followed by an early mobilization protocol is typically advocated.
- The A2 and A4 pulleys, should be preserved.
Technical concerns during the repair procedure of zone II flexor tendon injury include:
- The management of lacerations of the profundus and sublimis tendons.
- The appropriate orientation of the profundus with the sublimis slips.
- The attachment of the sublimis slips in the thin flat area.
- The management of the flexor sheath, including the annular pulleys (A2 – A4).
- The postoperative management.
- The timing and technique for tenolysis.

Zone III injury
- The results of direct repair in this zone are much better compared with zone II injuries..
- Lumbrical muscles originate from the radial aspect of FDP tendons in zone III.
- Lumbrical muscle bellies usually are not sutured because this can increase the tension of these muscles and result in a lumbrical plus finger.
Zone IV injury
Transverse carpal ligament should be repaired in a lengthened fashion to prevent bowstringing and allow for immobilization of wrist in flexion.
Zone V injury
- Direct repair of flexor tendon injury in this zone has a favorable prognosis.
- Results may be compromised by coexisting nerve injury.
Postoperative Rehabilitation
Rehabilitation and Physical Therapy for flexor tendon injury is very important to
- Prevent tendon adhesion.
- Increased tendon excursion.
- Accelerate healing of the tendon.
- Keep the strength of the muscles.
The most common rehabilitation protocols are Kleinert and Duran protocols, both programs restrict active flexion for approximately 6 weeks.
A dorsal splint holds the wrist in 20 to 30 degrees of flexion and the metacarpophalangeal joints at 40 to 60 degrees.
Kleinert protocol:
Dynamic splinting, which allows for active digit extension and passive digit flexion:
- Can use a rubber band attached to the fingernail and at the wrist.
- Rubber band should allow full extension of the proximal interphalangeal joint against the traction of the rubber band.
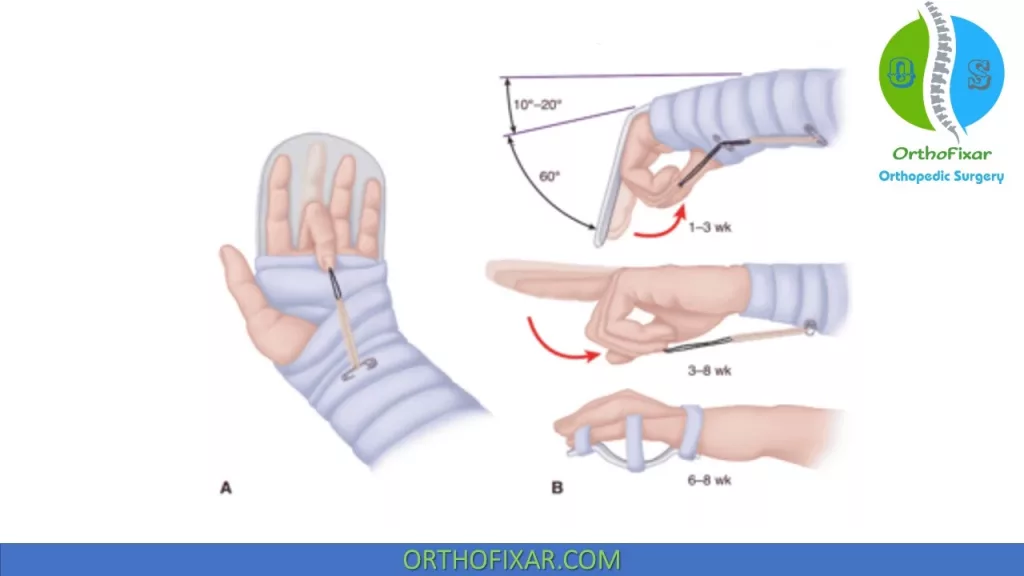
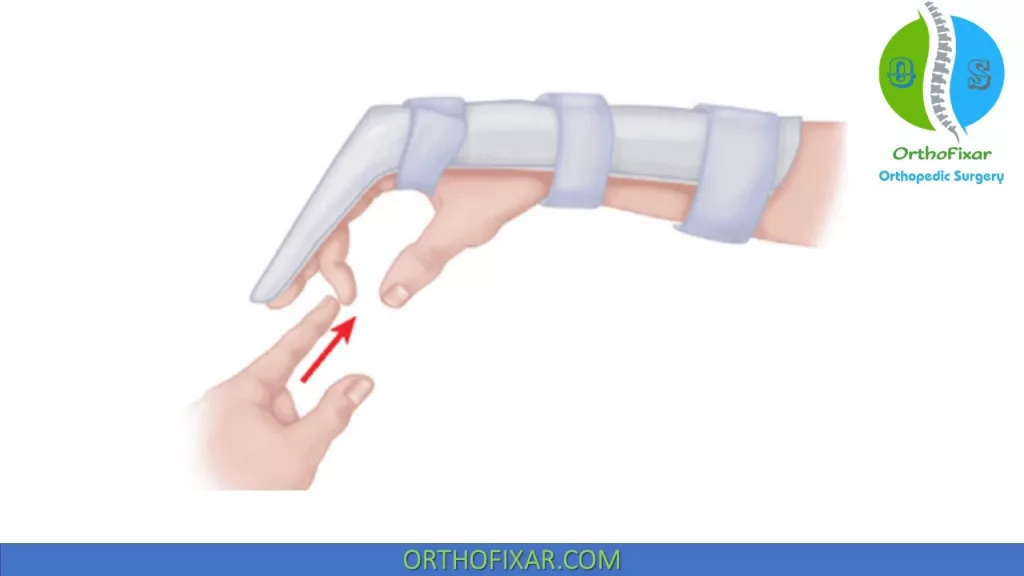
Duran protocol:
Requires strict patient compliance because other hand is used to perform passive digital flexion exercises.
- After 3 weeks, the dorsal splint is removed and a wrist band with a hook for the rubber band is used for an additional 3 weeks.
- The patient actively extends the digit against the resistance of the rubber band.
- The wrist band splint is discontinued at 6 to 8 weeks, and dynamic extension splinting is used to prevent contractures of the proximal interphalangeal joint.
- At 8 to 10 weeks, strengthening exercises are permitted, and the patient progresses to using the hand normally at 10 to 12 weeks after the repair.
Complications of Flexor Tendon Injury
1. Tendon adhesions:
- The most common complication following flexor tendon repair.
2. Rerupture of repaired tendon:
- If the scar is <1cm: Excise the scar and do a primary repair.
- If the scar is >1cm: Excise the scar and proceed a tendon graft.
3. Lumbrical plus finger:
- The “lumbrical plus” finger develops when the pull of the profundus musculotendinous unit is applied through the lumbrical muscle, rather than through a flexor tendon injury repairing distal to the lumbrical muscle origin.
- The long finger seems to be most commonly involved.
- The treatment of Lumbrical plus finger consists of transection of the involved lumbrical tendon.
4. Quadrigia effect:
- Quadrigia or DIP joint flexion contracture occurs when profundus advancement of 1 cm or more.
- Occurs because the FDP tendons (middle, ring, small) share a common muscle belly, and distal advancement of one tendon will compromise flexion of the adjacent digits, resulting in forearm pain.
5. Swan-neck deformity
6. Trigger finger
7. Joint contracture
Download Files
Hand Flexor Tendon Injury PDF File: Slideshare | Issuu
References
- Venkatramani H, Varadharajan V, Bhardwaj P, Vallurupalli A, Sabapathy SR. Flexor tendon injuries. J Clin Orthop Trauma. 2019 Sep-Oct;10(5):853-861. doi: 10.1016/j.jcot.2019.08.005. Epub 2019 Aug 19. PMID: 31528057; PMCID: PMC6739511.
- Campbel’s Operative Orthopaedics 12th edition Book.
- Millers Review of Orthopaedics -7th Edition Book.