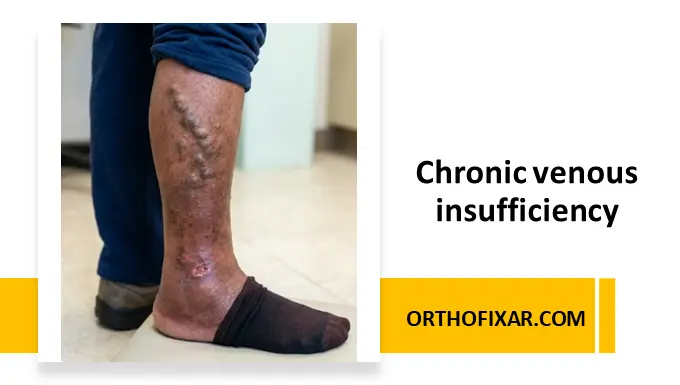
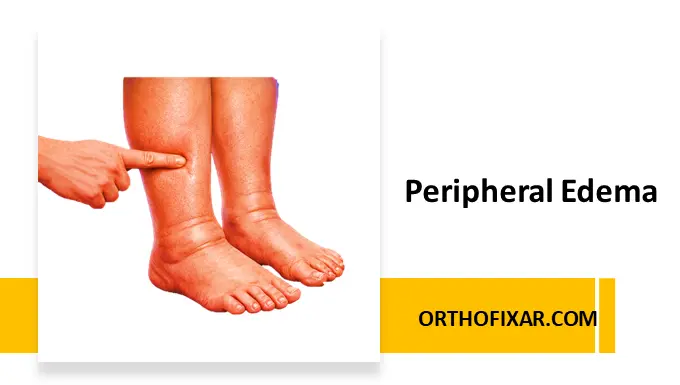
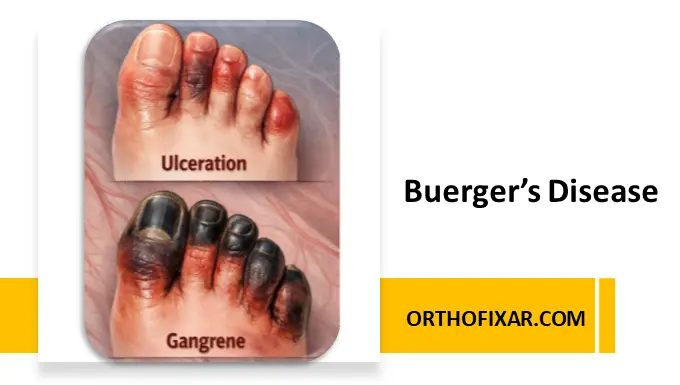
Chronic venous insufficiency (CVI) is a progressive vascular disorder characterized by impaired venous return, most commonly due to valvular incompetence, leading to venous hypertension and a spectrum of clinical manifestations ranging from mild edema to venous ulceration.
Introduction
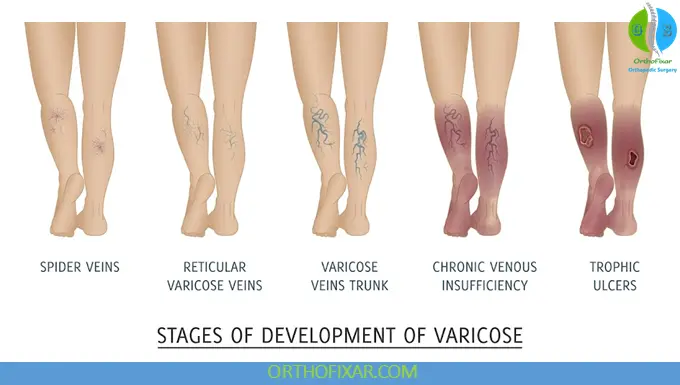
Chronic venous insufficiency represents a major global health burden, significantly affecting quality of life, productivity, and healthcare costs. It is part of the broader spectrum of chronic venous disease (CVD), with clinical severity ranging from telangiectasia to advanced ulcerative disease.
Venous Anatomy & Physiology
The venous system of the lower limbs consists of:
Venous return depends on:
- One-way venous valves
- Calf muscle pump
- Pressure gradients
Failure of these mechanisms leads to retrograde flow (reflux) and venous stasis.
See Also: Veins Anatomy
Pathophysiology of Chronic venous insufficiency
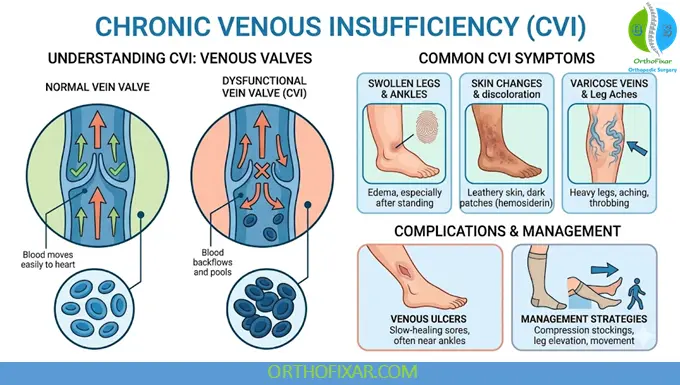
The hallmark of CVI is ambulatory venous hypertension, primarily due to valve incompetence or venous obstruction.
Key mechanisms:
- Venous reflux and obstruction
- Increased venous pressure
- Endothelial dysfunction and inflammation
- Leukocyte activation and microcirculatory damage
- Tissue hypoxia and fibrosis
These processes result in:
Chronic inflammation and vascular remodeling further perpetuate disease progression.
Risk Factors
Major risk factors include:
- Increasing age
- Female sex
- Pregnancy
- Obesity
- Prolonged standing or sedentary lifestyle
- History of deep vein thrombosis (DVT)
These factors contribute to venous valve damage or increased venous pressure.
Clinical Presentation
Early symptoms:
- Leg heaviness
- Aching pain
- Mild edema
- Nocturnal cramps
Progressive signs:
- Varicose veins
- Hyperpigmentation (hemosiderin deposition)
- Stasis dermatitis
- Lipodermatosclerosis
Advanced disease:
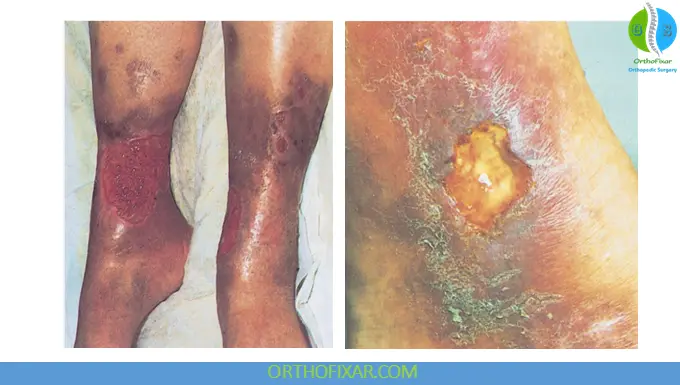
- Venous leg ulcers (typically medial malleolus)
CVI is often progressive if untreated, leading to chronic morbidity.
Classification: CEAP System
The CEAP classification of Chronic venous insufficiency is widely used:
- C: Clinical (C0–C6; from no signs to active ulcer)
- E: Etiology (congenital, primary, secondary)
- A: Anatomy (superficial, deep, perforator)
- P: Pathophysiology (reflux, obstruction)
This system guides both diagnosis and management.
Diagnosis
1. Clinical Assessment
2. Gold Standard Investigation
- Duplex ultrasonography
- Evaluates reflux and obstruction
- First-line imaging modality
3. Additional Tests (selected cases)
- Air plethysmography
- Venography (rare)
Chronic Venous Insufficiency Treatment
Treatment of Chronic venous insufficiency is multimodal, tailored to disease severity.
1. Conservative Therapy (First-line)
Compression Therapy
- Cornerstone of treatment
- Reduces venous hypertension and edema
- Improves venous return
Compression stockings and bandages are strongly evidence-based.
Lifestyle Modifications
- Leg elevation
- Regular exercise (calf muscle activation)
- Weight reduction
2. Pharmacological Therapy
Used as adjunctive treatment:
- Venoactive drugs (e.g., flavonoids such as diosmin/hesperidin)
- Hydroxyethylrutoside, Pycnogenol (emerging options)
These agents:
- Reduce edema
- Improve microcirculation
- Decrease inflammation
However, evidence varies, and they are not definitive therapy.
3. Interventional & Surgical Management
Indicated in refractory or advanced disease:
Minimally Invasive Techniques
- Endovenous laser ablation (EVLA)
- Radiofrequency ablation (RFA)
- Ultrasound-guided foam sclerotherapy
Surgical Options
- Vein stripping
- Ligation procedures
Modern practice favors endovenous techniques due to lower morbidity and faster recovery.
4. Management of Venous Ulcers
- Compression therapy (essential)
- Wound care
- Infection control
- Adjunctive pharmacotherapy
Venous ulcers are associated with high recurrence rates and require long-term follow-up.
Complications
Untreated Chronic venous insufficiency may lead to:
- Chronic pain and disability
- Recurrent infections
- Venous leg ulcers
- Post-thrombotic syndrome
These complications significantly impair quality of life.
Prognosis
Chronic venous insufficiency is:
- Chronic and progressive
- Not fully reversible
- Manageable with early and appropriate treatment
Early intervention is critical to prevent advanced complications.
Key Takeaways
- Chronic venous insufficiency is driven by venous hypertension due to valvular incompetence
- Duplex ultrasound is the diagnostic gold standard
- Compression therapy remains the cornerstone of management
- Advanced cases benefit from endovenous interventions
- Early treatment prevents ulceration and long-term morbidity
References & More
- Azar J, Rao A, Oropallo A. Chronic venous insufficiency: a comprehensive review of management. J Wound Care. 2022 Jun 2;31(6):510-519. doi: 10.12968/jowc.2022.31.6.510. PMID: 35678787. Pubmed
- Peschen M, Petter O, Vanscheidt W. Chronisch venöse Insuffizienz–von der Pathophysiologie zur Therapie. Folge 1: Pathophysiologie–Kompressionsbehandlung–systemische Pharmakotherapie [Chronic venous insufficiency–from pathophysiology to therapy. 1: Pathophysiology–compression treatment–systemic pharmacotherapy]. Fortschr Med. 1996 Sep 20;114(26):315-8. German. PMID: 8999001. Pubmed
- Miguel CB, Andrade RS, Mazurek L, Martins-de-Abreu MC, Miguel-Neto J, Barbosa AM, Silva GP, Góes-Neto A, Soares SC, Lazo-Chica JE, Rodrigues WF. Emerging Pharmacological Interventions for Chronic Venous Insufficiency: A Comprehensive Systematic Review and Meta-Analysis of Efficacy, Safety, and Therapeutic Advances. Pharmaceutics. 2025 Jan 3;17(1):59. doi: 10.3390/pharmaceutics17010059. PMID: 39861707; PMCID: PMC11768779. Pubmed
- Patel SK, Manea C, Surowiec SM. Venous Insufficiency. [Updated 2026 Jan 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed