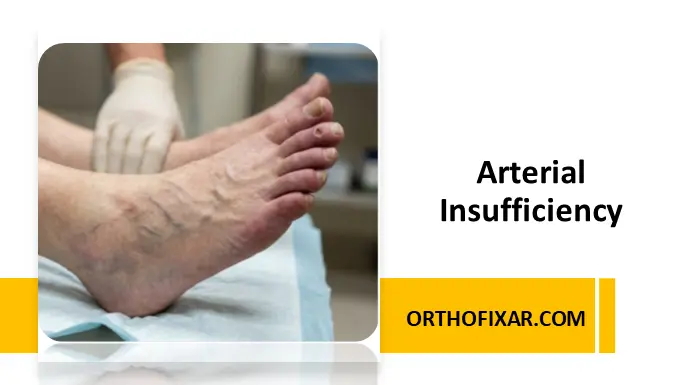
Arterial insufficiency is a vascular disorder characterized by reduced or obstructed blood flow through the arterial system, resulting in inadequate delivery of oxygen and nutrients to tissues. It is a major component of peripheral arterial disease (PAD) and is associated with significant morbidity if left untreated. Early recognition and management are essential to prevent complications such as tissue ischemia, ulceration, and limb loss.
Definition
Arterial insufficiency refers to any condition that impairs arterial blood flow, leading to tissue hypoxia and ischemia. It most commonly affects the lower extremities but may involve coronary, cerebral, or mesenteric arteries.
See Also: Peripheral Artery Disease (PAD): Symptoms, Causes & Treatment
Etiology and Risk Factors
1. Atherosclerosis (Primary Cause)
The most common cause is atherosclerosis, characterized by plaque accumulation within arterial walls, leading to narrowing (stenosis) and reduced perfusion.
2. Thrombosis and Embolism
- Thrombosis: Local clot formation on atherosclerotic plaques
- Embolism: Clots traveling from distant sites (e.g., heart)
Both can acutely occlude arterial flow.
3. Contributing Risk Factors
- Smoking
- Diabetes mellitus
- Hypertension
- Hyperlipidemia
- Sedentary lifestyle
These factors accelerate endothelial damage and plaque formation.
Pathophysiology
Arterial insufficiency results from reduced arterial lumen diameter, which limits blood flow. During increased metabolic demand (e.g., exercise), tissues cannot receive adequate oxygen, leading to ischemia and pain (claudication). Chronic ischemia may result in tissue necrosis and ulceration.
See Also: Arteries Anatomy: Layers, Function & Clinical Insight
Clinical Features
Symptoms vary depending on the affected vascular territory:
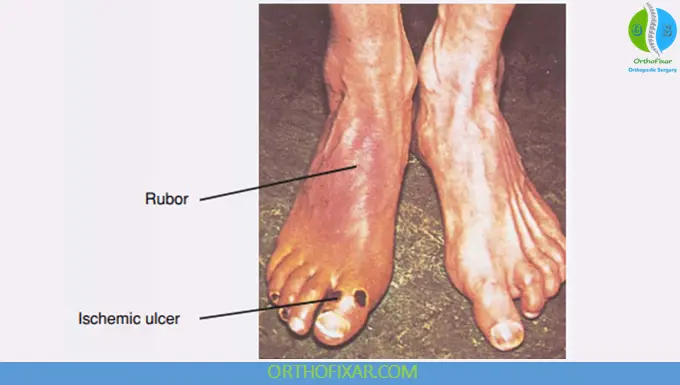
1. Peripheral Arterial Insufficiency (Lower Limbs)
- Intermittent claudication (pain during walking, relieved by rest)
- Rest pain (advanced disease)
- Cold, pale extremities
- Hair loss and shiny skin
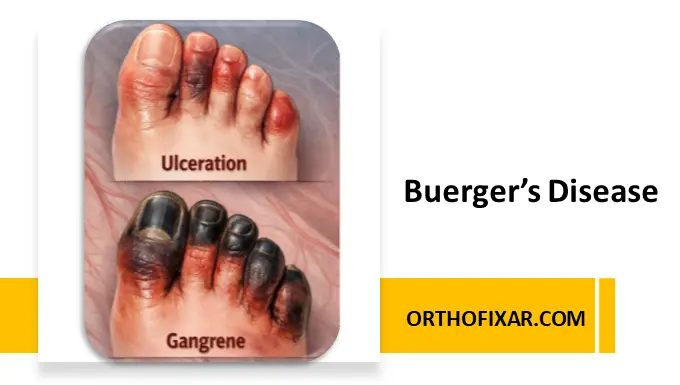
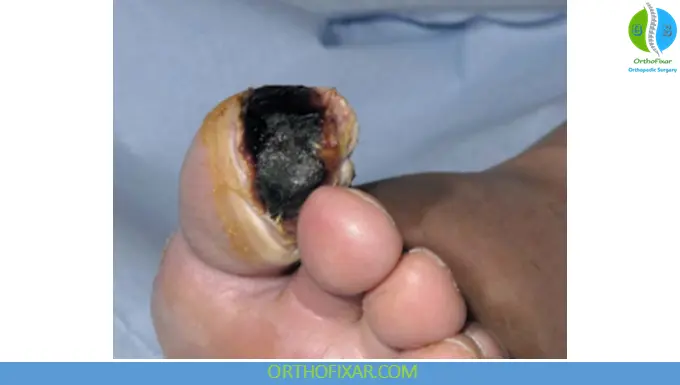
- Non-healing ulcers or gangrene
2. Coronary Artery Involvement
- Angina pectoris
- Myocardial infarction
3. Cerebral Circulation
- Transient ischemic attack (TIA)
- Stroke
4. Mesenteric Ischemia
- Postprandial abdominal pain (“abdominal angina”)
Diagnostic Evaluation
1. Clinical Assessment
- Detailed history (claudication, rest pain)
- Pulse examination (diminished or absent pulses)
- Skin and ulcer evaluation
2. Non-Invasive Tests
- Ankle-Brachial Index (ABI): Key diagnostic tool
- Doppler ultrasound
- Pulse volume recordings
3. Imaging
- CT angiography (CTA)
- MR angiography
- Conventional angiography (gold standard in some cases)
Complications
- Critical limb ischemia
- Chronic non-healing ulcers
- Gangrene
- Limb amputation
- Increased cardiovascular mortality
Arterial Insufficiency VS Venous Insufficiency
| Feature | Chronic Arterial Insufficiency (Advanced) | Chronic Venous Insufficiency (Advanced) |
|---|---|---|
| Pain | Intermittent claudication, progressing to pain at rest | Often painful |
| Mechanism | Tissue ischemia | Venous stasis and hypertension |
| Pulses | Decreased or absent | Normal, though may be difficult to feel through edema |
| Color | Pale (especially on elevation); dusky red on dependency | Normal, or cyanotic on dependency; petechiae then brown pigmentation with chronicity |
| Temperature | Cool | Normal |
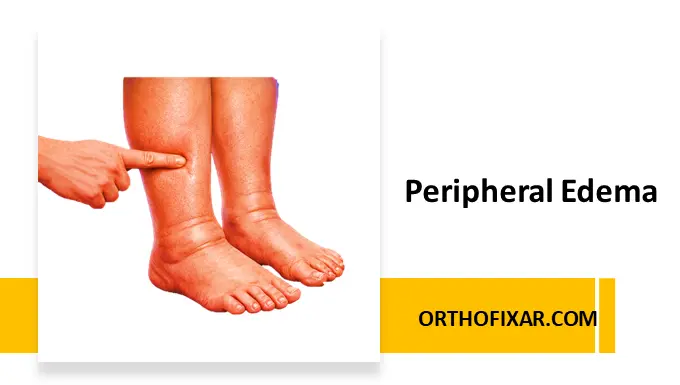
| Edema | Absent or mild; may develop as the patient tries to relieve rest pain by lowering the leg | Present, often marked |
| Skin Changes | Trophic changes: thin, shiny, atrophic skin; loss of hair over foot and toes; nails thickened and ridged | Brown pigmentation around the ankle, stasis dermatitis, thickening of the skin, narrowing of the leg as scarring develops |
| Ulceration | If present, involves toes or points of trauma on feet | If present, develops at sides of ankle, especially medially |
| Gangrene | May develop | Does not develop |
Arterial Insufficiency Treatment
1. Lifestyle Modification
- Smoking cessation
- Regular exercise (supervised walking programs)
- Dietary changes
2. Pharmacological Treatment
- Antiplatelet agents (e.g., aspirin)
- Statins (lipid control)
- Antihypertensive therapy
- Glycemic control in diabetics
3. Interventional Procedures
- Angioplasty with or without stenting
- Atherectomy
- Endarterectomy
4. Surgical Treatment
- Bypass grafting (e.g., CABG or peripheral bypass)
Prognosis and Prevention
Early-stage arterial insufficiency can be effectively managed with lifestyle and medical therapy. However, advanced disease significantly increases the risk of cardiovascular events and limb-threatening complications. Preventive strategies focus on risk factor modification and early detection.
Key Clinical Pearls
- Intermittent claudication is the hallmark symptom.
- Atherosclerosis is the leading cause.
- ABI is a simple and effective diagnostic tool.
- Management requires both systemic cardiovascular risk control and local vascular intervention.
Conclusion
Arterial insufficiency is a progressive vascular condition with systemic implications. Understanding its pathophysiology, recognizing early clinical signs, and implementing evidence-based management strategies are critical to improving patient outcomes and preventing severe complications.
References & More
- Sieggreen MY, Kline RA. Arterial insufficiency and ulceration: diagnosis and treatment options. Adv Skin Wound Care. 2004 Jun;17(5 Pt 1):242-51; quiz 252-3. doi: 10.1097/00129334-200406000-00013. PMID: 15192492. Pubmed
- Schorr EN, Treat-Jacobson D. Methods of symptom evaluation and their impact on peripheral artery disease (PAD) symptom prevalence: a review. Vasc Med. 2013 Apr;18(2):95-111. doi: 10.1177/1358863X13480001. Epub 2013 Mar 18. PMID: 23509087; PMCID: PMC3654822. Pubmed
- Swedish Council on Health Technology Assessment. Peripheral Arterial Disease – Diagnosis and Treatment: A Systematic Review (Summary and conclusions) [Internet]. Stockholm: Swedish Council on Health Technology Assessment (SBU); 2008 Nov. SBU Yellow Report No. 187. Available from: Pubmed
- Swedish Council on Health Technology Assessment. Peripheral Arterial Disease – Diagnosis and Treatment: A Systematic Review [Internet]. Stockholm: Swedish Council on Health Technology Assessment (SBU); 2008 Nov. SBU Yellow Report No. 187. PMID: 28876730. Pubmed