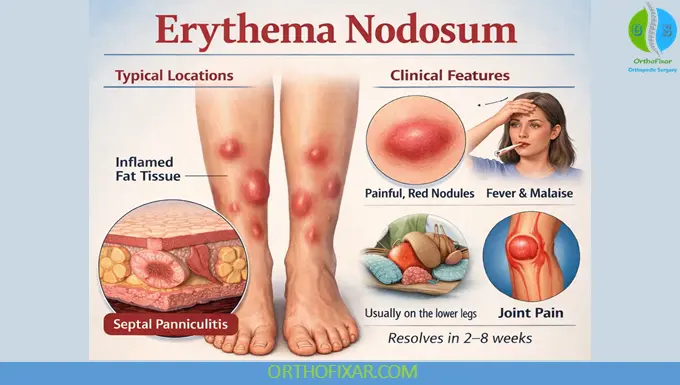
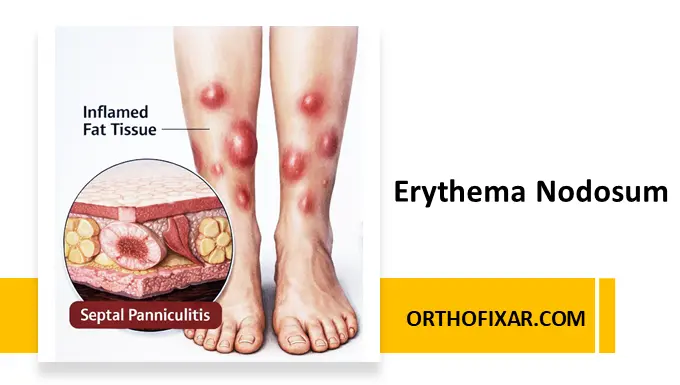
Erythema nodosum (EN) is the most common form of panniculitis, characterized by inflammation of subcutaneous fat tissue. It presents as painful, erythematous nodules, typically located on the anterior aspects of the lower legs. EN is not a disease itself but rather a reactive process, often indicating an underlying systemic condition.
Epidemiology
Erythema nodosum occurs worldwide and shows a clear female predominance, affecting women approximately 3–5 times more often than men. It is most commonly seen in young adults.
Pathophysiology
EN is considered a delayed hypersensitivity reaction to various antigenic stimuli. The inflammatory process involves:
- Septal panniculitis (inflammation of fat septa)
- Immune complex deposition
- Neutrophilic infiltration in early stages
Unlike other panniculitides, EN does not cause necrosis or ulceration, and lesions typically resolve without scarring.
See Also: Skin Anatomy
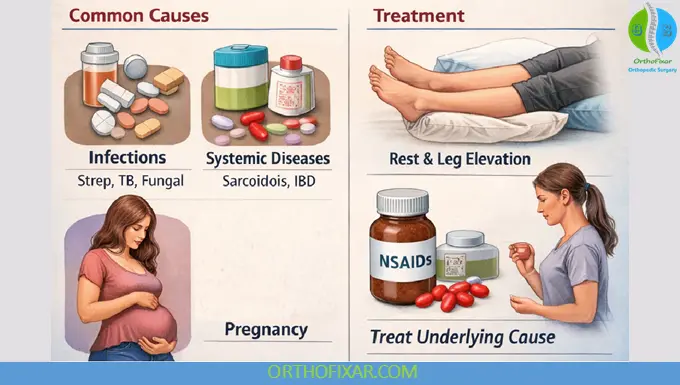
Causes of Erythema Nodosum
In approximately 50% of cases, EN is idiopathic, but many identifiable causes exist.
1. Infectious Causes
- Streptococcal infections (most common identifiable cause)
- Tuberculosis
- Yersinia, Histoplasmosis, Coccidioidomycosis
2. Systemic Diseases
- Sarcoidosis
- Inflammatory bowel disease (Crohn’s disease, ulcerative colitis)
- Behçet disease
3. Drugs
- Oral contraceptives
- Sulfonamides
- Antibiotics
4. Other Causes
- Pregnancy
- Malignancy (rare, but important consideration)
EN may represent the first manifestation of systemic disease, making evaluation essential.
See Also: Peripheral Edema: Causes, Diagnosis, and Management
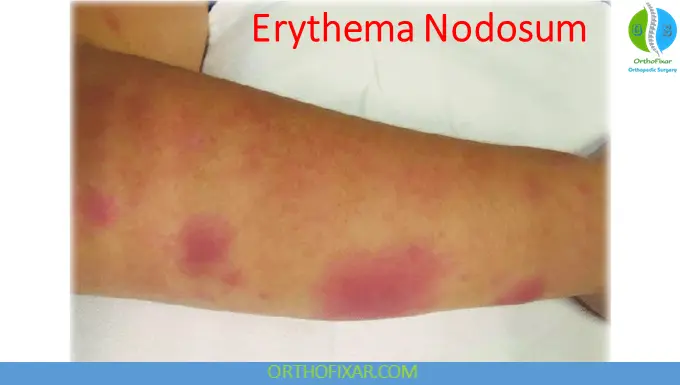
Clinical Features
Skin Findings
- Tender, erythematous nodules (1–6 cm)
- Bilateral and symmetrical distribution
- Commonly located on the pretibial region
Systemic Symptoms
- Fever
- Malaise
- Arthralgia or arthritis
Lesions evolve similarly to bruises and typically resolve within 2–8 weeks without scarring.
Diagnosis
Clinical Diagnosis
Erythema Nodosum is primarily a clinical diagnosis, based on characteristic lesions and distribution.
Laboratory Evaluation
Workup should focus on identifying the underlying cause:
- CBC, ESR, CRP
- Throat culture and ASO titers
- Chest X-ray (for sarcoidosis or tuberculosis)
Biopsy
- Rarely required
- Shows septal panniculitis without vasculitis
A systematic diagnostic approach is crucial, as Erythema Nodosum may signal serious systemic disease.
Differential Diagnosis
- Cellulitis
- Vasculitis
- Other panniculitides
- Lipodermatosclerosis
See Also: Cellulitis: Causes, Symptoms, Diagnosis & Treatment
Management
1. Treat the Underlying Cause
- Infection → antibiotics
- Systemic disease → targeted therapy
2. Supportive Treatment
- Bed rest
- Leg elevation
- Compression (in selected cases)
3. Pharmacologic Therapy
- NSAIDs (first-line for pain relief)
- Potassium iodide (historical use)
- Corticosteroids (reserved for severe cases after excluding infection)
Most cases are self-limiting, resolving spontaneously.
Prognosis
- Excellent in most patients
- Resolves without scarring
- Recurrence may occur, especially if the underlying cause persists
Key Clinical Pearls
- Erythema Nodosum is the most common panniculitis
- Often a marker of systemic disease
- Always investigate for underlying etiology
- Usually self-limited with supportive care
References & More
- Chowaniec M, Starba A, Wiland P. Erythema nodosum – review of the literature. Reumatologia. 2016;54(2):79-82. doi: 10.5114/reum.2016.60217. Epub 2016 Jun 3. PMID: 27407284; PMCID: PMC4918048. Pubmed
- Hafsi W, Badri T. Erythema Nodosum. [Updated 2022 Nov 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Pérez-Garza DM, Chavez-Alvarez S, Ocampo-Candiani J, Gomez-Flores M. Erythema Nodosum: A Practical Approach and Diagnostic Algorithm. Am J Clin Dermatol. 2021 May;22(3):367-378. doi: 10.1007/s40257-021-00592-w. Epub 2021 Mar 8. PMID: 33683567; PMCID: PMC7938036. Pubmed
- Pérez-Garza DM, Chavez-Alvarez S, Ocampo-Candiani J, Gomez-Flores M. Erythema Nodosum: A Practical Approach and Diagnostic Algorithm. Am J Clin Dermatol. 2021 May;22(3):367-378. doi: 10.1007/s40257-021-00592-w. Epub 2021 Mar 8. PMID: 33683567; PMCID: PMC7938036. Pubmed
- Leung AKC, Leong KF, Lam JM. Erythema nodosum. World J Pediatr. 2018 Dec;14(6):548-554. doi: 10.1007/s12519-018-0191-1. Epub 2018 Sep 29. PMID: 30269303. Pubmed
- Diernaes, Jon & Bygum, Anette & Poulsen, Per. (2014). Unmasking sarcoidosis following surgery for Cushing disease. Dermato-Endocrinology. 8. e29855. 10.4161/derm.29855.
This article is very clear.