What is Cellulitis?
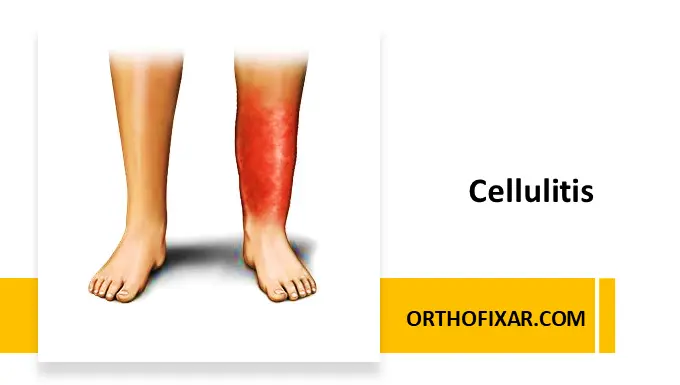
Cellulitis is an acute bacterial infection of the skin and subcutaneous tissues, primarily affecting the deep dermis. It is characterized by erythema, warmth, swelling, and tenderness of the affected area.
This condition is common worldwide and can range from mild to severe, potentially leading to complications if untreated.
Cellulitis Causes
Cellulitis occurs when bacteria enter the skin through breaks in the protective barrier, such as cuts, abrasions, insect bites, or surgical wounds.
Common causative organisms
- β-hemolytic Streptococcus (especially Streptococcus pyogenes)
- Staphylococcus aureus (including MRSA in some cases)
In certain populations (e.g., immunocompromised patients), gram-negative bacteria or anaerobes may also be involved.
See Also: Skin Anatomy
Risk Factors
Several factors increase susceptibility to cellulitis:
- Skin trauma or wounds
- Chronic skin conditions (e.g., eczema, fungal infections)
- Diabetes mellitus
- Peripheral vascular disease
- Lymphedema
- Immunosuppression
Cellulitis Symptoms
Cellulitis typically presents with:
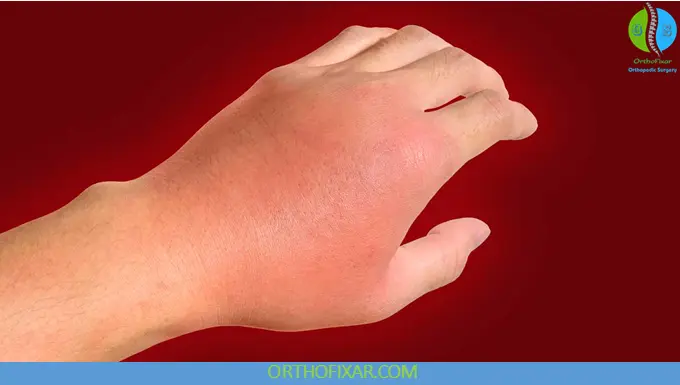
- Redness (erythema)
- Warmth over the affected area
- Swelling (edema)
- Pain or tenderness
- Poorly defined borders of infection
Systemic symptoms may include:
- Fever
- Malaise
- Fatigue
The lower extremities are most commonly affected, but cellulitis can occur anywhere on the body.
See Also: Peripheral Edema: Causes, Diagnosis, and Management
Diagnosis
Cellulitis is primarily a clinical diagnosis, based on patient history and physical examination.
There is no definitive laboratory test, and diagnosis depends on identifying key features such as spreading erythema, warmth, and tenderness.
Clinicians must also differentiate cellulitis from similar conditions like:
- Deep vein thrombosis
- Contact dermatitis
- Necrotizing soft tissue infections
Cellulitis Treatment
1. Antibiotic Therapy
The cornerstone of Cellulitis treatment is empiric antibiotic therapy targeting:
- Streptococcus species
- Staphylococcus aureus
- Mild cases: Oral antibiotics
- Severe cases: Intravenous antibiotics
A typical course is around 5 days, extended if symptoms persist.
2. Supportive Measures
- Elevation of the affected limb
- Pain management
- Hydration
3. Management of Risk Factors
Addressing underlying conditions (e.g., diabetes, edema) reduces recurrence risk.
Complications
If untreated or severe, cellulitis can lead to:
- Abscess formation
- Sepsis
- Lymphangitis
- Necrotizing fasciitis (life-threatening)
Prevention
Preventive strategies include:
- Proper wound care and hygiene
- Treating fungal infections (e.g., tinea pedis)
- Managing chronic conditions
- Avoiding skin injuries
When to Seek Medical Attention
Immediate medical care is required if:
- Rapidly spreading redness
- High fever or systemic symptoms
- Severe pain
- Immunocompromised state
Conclusion
Cellulitis is a common but potentially serious bacterial skin infection that requires early recognition and appropriate treatment. Prompt antibiotic therapy and management of underlying risk factors are essential to prevent complications and recurrence.
References & More
- Raff AB, Kroshinsky D. Cellulitis: A Review. JAMA. 2016 Jul 19;316(3):325-37. doi: 10.1001/jama.2016.8825. PMID: 27434444. Pubmed
- Brown BD, Syed HA, Hood Watson KL. Cellulitis. [Updated 2025 Dec 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2026 Jan-. Available from: Pubmed
- Featherstone P, Brindle R, Williams OM. Acute management of cellulitis: A review. Acute Med. 2019;18(2):112-119. PMID: 31127800. Pubmed
- Gunderson CG. Cellulitis: definition, etiology, and clinical features. Am J Med. 2011 Dec;124(12):1113-22. doi: 10.1016/j.amjmed.2011.06.028. Epub 2011 Oct 18. PMID: 22014791. Pubmed