What is Peripheral Edema?
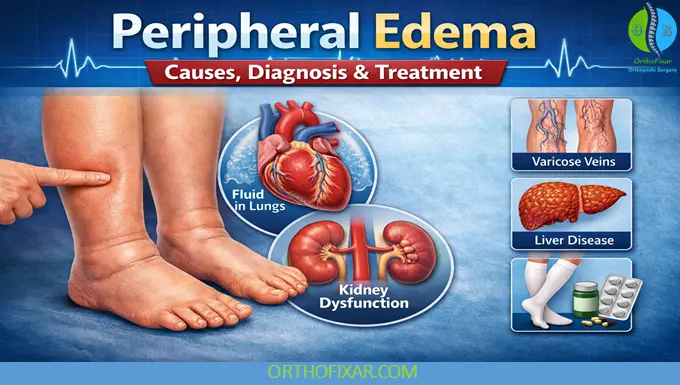
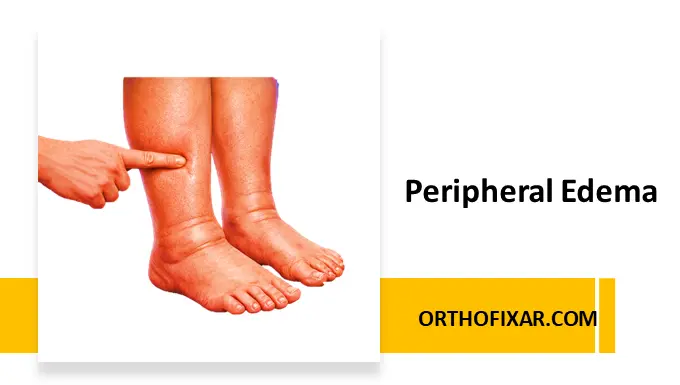
Peripheral edema refers to swelling caused by the accumulation of fluid in the tissues of the extremities, most commonly the legs, ankles, and feet. It results from disturbances in fluid balance between the vascular system and interstitial tissues. Peripheral edema can be benign and temporary, but it may also indicate serious systemic disease requiring urgent evaluation.
Pathophysiology of Peripheral Edema
Peripheral edema develops when fluid movement across capillary membranes becomes abnormal. The main mechanisms include:
- Increased capillary hydrostatic pressure (e.g., heart failure, venous obstruction)
- Reduced plasma oncotic pressure (e.g., nephrotic syndrome, liver disease)
- Increased capillary permeability (e.g., infection, burns, allergic reactions)
- Lymphatic obstruction (e.g., malignancy, filariasis)
These mechanisms disrupt Starling forces and allow fluid to accumulate in interstitial spaces.
See Also: Lymphatic System Anatomy
Causes of Peripheral Edema
1. Cardiovascular Causes
- Congestive heart failure
- Pulmonary hypertension
- Pericardial disease
Cardiac disorders lead to venous congestion and increased hydrostatic pressure, producing bilateral leg edema.
2. Renal Causes
- Chronic kidney disease
- Nephrotic syndrome
- Acute renal failure
Kidney dysfunction leads to sodium and fluid retention or protein loss, both of which promote edema formation.
3. Hepatic Causes
- Liver cirrhosis
- Liver failure
Reduced albumin synthesis decreases oncotic pressure and allows fluid to leak into tissues.
4. Venous and Lymphatic Disorders
- Chronic venous insufficiency
- Deep vein thrombosis
- Lymphedema
Venous obstruction or lymphatic drainage failure causes localized or unilateral swelling.
5. Medications and Hormonal Causes
Common drug-induced causes include:
- Calcium channel blockers
- NSAIDs
- Steroids
Pregnancy and hormonal shifts can also lead to fluid retention.
Clinical Assessment of Peripheral Edema
A structured clinical approach is essential.
Key History Points
- Onset: acute vs chronic
- Distribution: unilateral vs bilateral
- Associated symptoms: dyspnea, pain, fatigue
For example:
- Painful unilateral edema → suspect DVT
- Bilateral edema with dyspnea → consider heart failure
- Edema worse with standing → venous insufficiency
These features help narrow the differential diagnosis.
Diagnostic Workup
Initial investigations often include:
- Basic metabolic panel and renal function tests
- Liver function tests
- Thyroid function tests
- Urine protein measurement
- BNP if heart failure suspected
- Duplex ultrasound for venous disease
This systematic evaluation helps identify systemic vs localized causes of edema.
Management of Peripheral Edema
1. Treat the Underlying Cause
Management focuses primarily on correcting the underlying disease, such as heart failure, renal disease, or venous insufficiency.
2. General Supportive Measures
- Limb elevation above heart level
- Sodium restriction
- Regular ambulation or muscle activation
- Skin care to prevent infection
These measures reduce fluid accumulation and improve venous return.
3. Compression Therapy
Graduated compression stockings are first-line therapy for many chronic causes, especially venous insufficiency, after ruling out peripheral arterial disease.
4. Pharmacologic Therapy
- Diuretics such as furosemide are commonly used in systemic fluid overload (e.g., heart failure).
- Medication review is essential to discontinue drugs causing edema.
Treatment should be tailored to the etiology rather than applied uniformly.
When Peripheral Edema is a Red Flag
Peripheral edema may signal serious disease when accompanied by:
- Shortness of breath
- Chest pain
- Rapid weight gain
- Reduced urine output
- Signs of liver failure
In such cases, urgent evaluation is required to prevent complications.
Prognosis
The outcome depends largely on the underlying cause. Edema related to reversible conditions such as medication use or mild venous insufficiency often resolves with treatment, whereas edema from advanced heart, kidney, or liver disease may persist and require long-term management.
Pitting vs Non-Pitting Edema
| Feature | Pitting Edema | Non-Pitting Edema |
|---|---|---|
| Definition | Swelling that retains an indentation after finger pressure | Swelling that does not retain an indentation after pressure |
| Mechanism | Excess interstitial fluid that can be displaced by pressure | Fluid bound within tissues or due to fibrosis, inflammation, or lymphatic obstruction |
| Typical Causes | Heart failure, renal disease, liver cirrhosis, venous insufficiency, hypoalbuminemia | Lymphedema, hypothyroidism (myxedema), lipedema, chronic lymphatic obstruction |
| Consistency on palpation | Soft and compressible | Firm, thick, or “woody” texture |
| Skin appearance | Shiny, stretched skin; may improve with elevation | Thickened skin; may show peau d’orange changes in chronic cases |
| Response to elevation | Often improves with limb elevation | Usually minimal improvement with elevation |
| Distribution | Common in dependent areas (ankles, legs, sacrum in bedridden patients) | Often localized; may involve dorsum of foot, toes, or face (myxedema) |
| Associated symptoms | Dyspnea (HF), ascites, oliguria, fatigue depending on cause | Heaviness, tightness, skin thickening, reduced mobility |
| Clinical grading | Graded 1+ to 4+ based on depth and rebound time | No standard grading system |
| Management focus | Treat systemic fluid overload, diuretics, compression, sodium restriction | Treat lymphatic or endocrine cause, compression therapy, manual drainage, skin care |
References & More
- Goyal A, Singh B, Afzal M. Peripheral Edema. [Updated 2025 Apr 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: Pubmed
- Mayoclinic – Edema
- Patel H, Skok C, DeMarco A. Peripheral Edema: Evaluation and Management in Primary Care. Am Fam Physician. 2022 Nov;106(5):557-564. PMID: 36379502. Pubmed
Great information shared.. really enjoyed reading this post thank you author for sharing this post .. appreciated
バンコク ソープランド
[…] See Also: Peripheral Edema: Causes, Diagnosis, and Management […]
Gonna give 555p999 a try. The name is a little weird, but hey, you never know where your next big win will come from! 555p999
Alright folks, curious about vn666vn. Anybody got some experience with this site? Share your thoughts! vn666vn
Heard some buzz about 69jilicasino. Anyone playing there regularly? How are the payouts? Good luck everyone69jilicasino
555
555
555
555*1
555
Buy Alprazolam Online