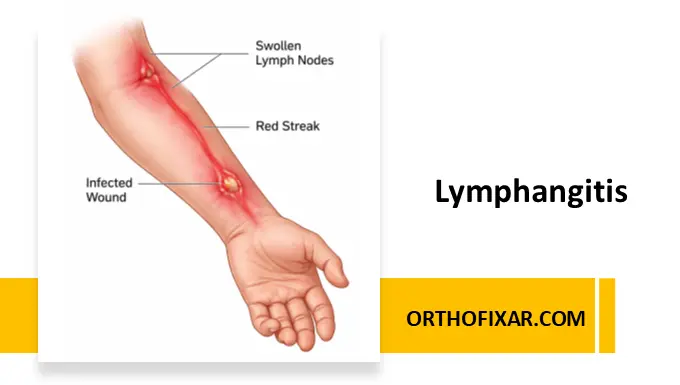
What is Lymphangitis?
Lymphangitis is an acute inflammation of the lymphatic vessels, most commonly caused by infection spreading from a skin wound into the lymphatic system. It is considered a medical emergency in some cases because of its rapid progression and potential to lead to sepsis.
The condition is characterized by linear red streaks extending proximally from the site of infection toward regional lymph nodes.
Causes of Lymphangitis
1. Bacterial Causes (Most Common)
The majority of cases are due to:
- Group A Streptococcus (Streptococcus pyogenes)
- Staphylococcus aureus
These organisms typically enter through:
- Skin wounds
- Surgical incisions
- Insect bites
- Ulcers or cellulitis
2. Other Infectious Causes
Less commonly, lymphangitis may be caused by:
- Fungal infections (e.g., Sporothrix schenckii)
- Mycobacteria (e.g., Mycobacterium marinum)
- Parasites or zoonotic organisms
Nodular lymphangitis (sporotrichoid pattern) is classically associated with:
- Sporotrichosis
- Nocardiosis
- Leishmaniasis
3. Non-Bacterial Causes
Although uncommon, lymphangitis may also result from:
- Viral infections (e.g., herpes simplex)
- Insect or spider bites
- Malignancy (neoplastic lymphangitis)
See Also: Phlebitis: Causes, Symptoms, Diagnosis & Treatment
Risk Factors
Patients at higher risk include those with:
- Diabetes mellitus
- Immunosuppression (HIV, steroid use)
- Chronic skin disease
- Poor wound care
- Recent trauma or surgery
Clinical Presentation
Lymphangitis Symptoms
- Red linear streaks along lymphatic vessels
- Local pain and tenderness
- Fever and chills
- Malaise
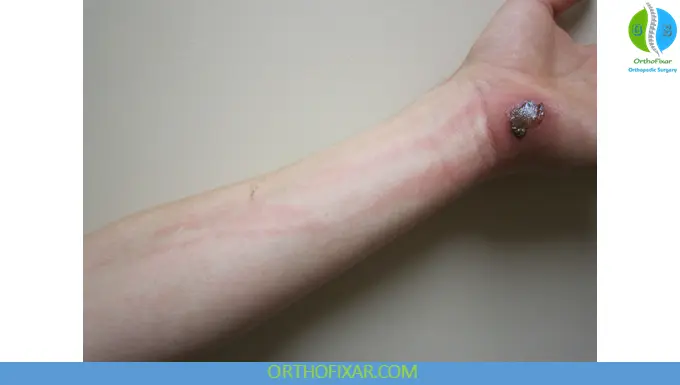
Physical Signs
- Enlarged regional lymph nodes (lymphadenopathy)
- Warm, erythematous skin
- Rapid proximal spread of infection (often within hours)
Complications
If untreated, lymphangitis can lead to:
- Cellulitis
- Abscess formation
- Bacteremia
- Sepsis (life-threatening)
This is why early recognition and treatment are critical.
Diagnosis
Diagnosis is mainly clinical, based on:
- Characteristic red streaking
- History of skin injury or infection
Additional investigations may include:
- Blood cultures (if systemic symptoms)
- Wound cultures
- Imaging in complicated cases
In atypical or chronic cases, biopsy and culture may be required (especially for nodular lymphangitis).
Lymphangitis Treatment
1. Antibiotic Therapy (Mainstay)
Empirical treatment should target:
- Streptococci
- Staphylococci
Common options:
- Oral antibiotics (mild cases)
- Intravenous antibiotics (severe cases)
Early antibiotic therapy usually leads to rapid improvement.
2. Supportive Care
- Limb elevation
- Analgesics
- Hydration
3. Surgical Management
Indicated if:
- Abscess formation
- Necrotic tissue
- Failure of medical therapy
4. Treatment of Atypical Causes
- Antifungal therapy (sporotrichosis)
- Antimycobacterial therapy
- Targeted therapy based on culture results
Differential Diagnosis
Conditions that may mimic lymphangitis include the following:
- Cellulitis
- Erysipelas
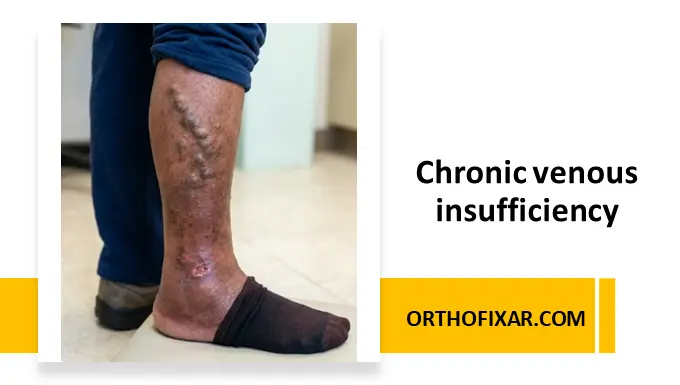
- Superficial thrombophlebitis
- Allergic reactions to insect bites
Prognosis
With early treatment, prognosis is excellent. However, delayed management increases the risk of:
- Rapid systemic spread
- Sepsis
- Hospitalization
Key Takeaways
- Lymphangitis is usually a bacterial infection of lymphatic vessels.
- Red streaking is the hallmark sign.
- It can progress rapidly within 24 hours.
- Prompt antibiotic treatment is essential to prevent complications.
References & More
- Kostman JR, DiNubile MJ. Nodular lymphangitis: a distinctive but often unrecognized syndrome. Ann Intern Med. 1993 Jun 1;118(11):883-8. doi: 10.7326/0003-4819-118-11-199306010-00009. PMID: 8480962. PubMed
- Tirado-Sánchez A, Bonifaz A. Nodular Lymphangitis (Sporotrichoid Lymphocutaneous Infections). Clues to Differential Diagnosis. J Fungi (Basel). 2018 May 9;4(2):56. doi: 10.3390/jof4020056. PMID: 29747448; PMCID: PMC6023502. PubMed
- Cohen BE, Nagler AR, Pomeranz MK. Nonbacterial Causes of Lymphangitis with Streaking. J Am Board Fam Med. 2016 Nov 12;29(6):808-812. doi: 10.3122/jabfm.2016.06.160015. PMID: 28076265. PubMed
- Bishara J, Cohen Y, Gabay B, Pavlov R, Samra Z, Pitlik S. Sporotrichoid lymphangitis due to group A Streptococcus. Clin Infect Dis. 2001 Jun 15;32(12):e154-7. doi: 10.1086/320753. Epub 2001 May 9. PMID: 11360227. PubMed