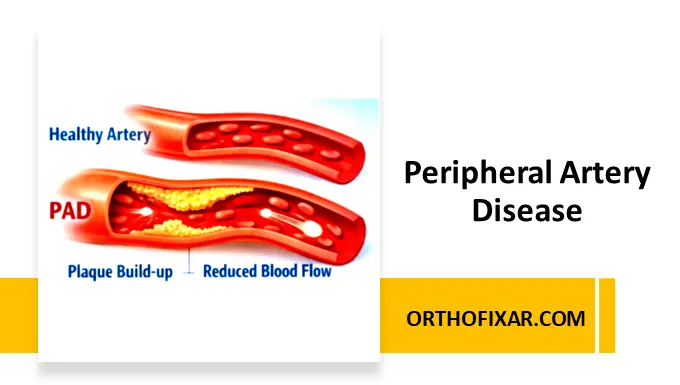
Peripheral Artery Disease (PAD), also known as peripheral arterial disease, is a common circulatory condition in which narrowed arteries reduce blood flow to the upper or lower limbs. It most often affects the lower extremities and is a marker for systemic atherosclerosis — the buildup of fatty plaque inside the arteries.
What Is Peripheral Artery Disease?
PAD occurs when plaque (fatty deposits, cholesterol, and cellular waste) accumulates in arterial walls, restricting oxygen-rich blood from reaching muscles and tissues—especially in the legs. This reduction in blood flow can lead to muscle pain, cramping, and impaired mobility.
According to the Centers for Disease Control and Prevention (CDC), the Peripheral Artery Disease is most common in the legs and can occur without noticeable symptoms in many people.
See Also: Arteries Anatomy: Layers, Function & Clinical Insight
Symptoms of PAD
Symptoms can vary depending on disease severity. Many people have no symptoms early on, but hallmark signs include:
- Claudication: Pain, cramping, or tiredness in the calves, thighs or buttocks during walking or exercise that improves with rest.
- Rest pain: A burning or aching pain in the feet or toes at rest, especially when lying flat.
- Weak or absent pulses in the legs or feet.
- Coldness or numbness in the lower limbs.
- Skin changes: Shiny skin, hair loss on the legs, slow-growing toenails.
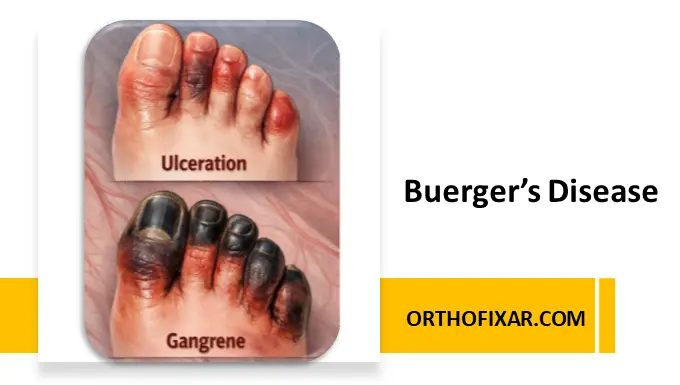
- Non-healing sores or ulcers on toes or feet.
In advanced disease, peripheral arterial disease can cause critical limb ischemia, where lack of blood flow leads to non-healing wounds and tissue loss.
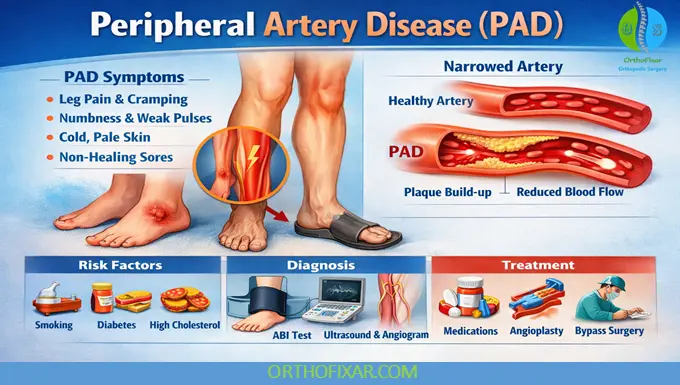
Causes and Risk Factors
Primary Cause
- Atherosclerosis: The most frequent cause of Peripheral Artery Disease is plaque buildup that narrows and stiffens arteries.
Key Risk Factors
- Smoking or tobacco use
- Diabetes mellitus
- High blood pressure (hypertension)
- High cholesterol levels
- Age (especially over 65)
- Family history of vascular disease
These factors increase the likelihood of arterial plaque accumulation and progressive blood flow restriction.
See Also: Raynaud’s Phenomenon: Causes, Symptoms, Diagnosis & Treatment
How PAD Is Diagnosed
Diagnosis begins with a medical history and physical exam. Healthcare providers commonly use the following tests:
Ankle-Brachial Index (ABI)
The ABI compares blood pressure in the ankles to the arms. A lower ankle pressure suggests peripheral arterial disease.
Doppler Ultrasound
This imaging assesses blood flow in leg arteries and can locate blockages.
Angiography
With contrast dye, this test visualizes blocked or narrowed arteries.
Blood Tests
Checks for diabetes, high cholesterol, and other conditions that influence peripheral arterial disease risk.
Peripheral Artery Disease Treatment
The goals of PAD treatment are to relieve symptoms, improve mobility, and reduce cardiovascular risk.
Lifestyle Modifications
- Quit smoking: Smoking accelerates plaque buildup and worsens blood flow.
- Regular exercise: Supervised programs can improve walking distance and reduce pain.
- Healthy diet: Emphasize fruits, vegetables, whole grains, and lean proteins.
Medications
- Statins to lower LDL cholesterol.
- Blood pressure control with antihypertensives.
- Antiplatelet agents (e.g., aspirin) to reduce clot risk.
- Cilostazol may help relieve claudication symptoms.
Procedures and Surgery
If conservative treatment isn’t sufficient:
- Angioplasty and stent placement to widen blocked arteries.
- Bypass surgery to reroute blood around blockages.
- Thrombolytic therapy to dissolve clots if present.
Prevention and Long-Term Management
PAD prevention focuses on controlling risk factors:
- Don’t smoke.
- Maintain a healthy weight.
- Manage blood glucose, blood pressure, and cholesterol.
- Stay physically active.
Early intervention can slow disease progression and lower risk of heart attack and stroke.
Conclusion
Peripheral Artery Disease is a serious but manageable vascular condition. Early recognition, targeted lifestyle changes, regular medical follow-up, and appropriate therapy can greatly improve quality of life and reduce complications. If you or a loved one experiences leg pain with walking or other peripheral arterial disease symptoms, consult a healthcare provider for evaluation and care.
What is Peripheral Artery Disease?
Peripheral Artery Disease is a condition caused by atherosclerosis that reduces blood flow to the legs, often leading to pain while walking
What are the first symptoms of PAD?
The most common early symptom is claudication, which is leg pain or cramping during walking that improves with rest.
How is PAD diagnosed?
PAD is commonly diagnosed using the ankle-brachial index (ABI), Doppler ultrasound, and imaging studies such as angiography.
References & More
- Zemaitis MR, Boll JM, Kato M, et al. Peripheral Arterial Disease. [Updated 2025 Dec 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: Pubmed
- Aboyans V, Canonico ME, Chastaingt L, Anand SS, Brodmann M, Couffinhal T, Criqui MH, Debus ES, Mazzolai L, McDermott MM, Bonaca MP. Peripheral artery disease. Nat Rev Dis Primers. 2025 Sep 18;11(1):68. doi: 10.1038/s41572-025-00651-0. PMID: 40968271. Pubmed
- Sunner SS, Welsh RC, Bainey KR. Medical Management of Peripheral Arterial Disease: Deciphering the Intricacies of Therapeutic Options. CJC Open. 2021 Mar 12;3(7):936-949. doi: 10.1016/j.cjco.2021.03.005. PMID: 34401701; PMCID: PMC8348339. Pubmed
- Minc SD, McGinigle KL. Peripheral Artery Disease: New Concepts, Treatments, and Disparities. Annu Rev Med. 2026 Jan;77(1):45-58. doi: 10.1146/annurev-med-050124-045433. Epub 2025 Dec 11. PMID: 41380712; PMCID: PMC12926866. Pubmed