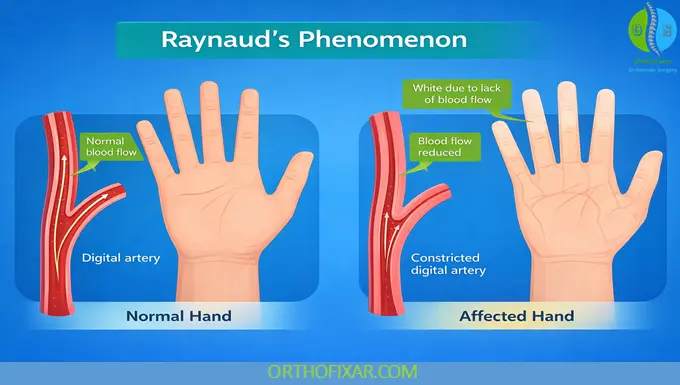
What is Raynaud’s Phenomenon?
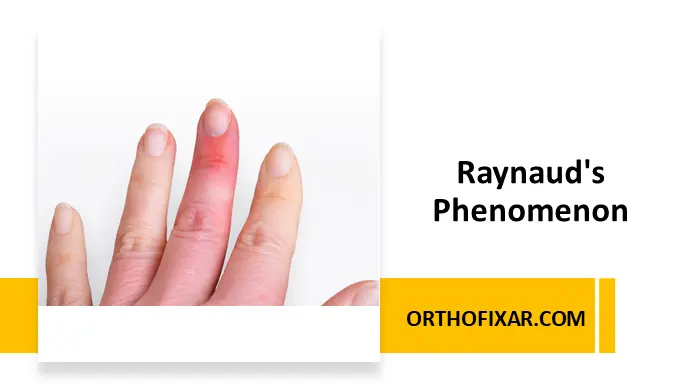
Raynaud’s phenomenon is a vascular condition characterized by episodic narrowing of small blood vessels (vasospasm) in the extremities, most commonly the fingers and toes. This reduced blood flow leads to color changes, numbness, and discomfort, usually triggered by cold exposure or emotional stress.
During an attack, the skin typically turns white (ischemia), then blue (deoxygenation), and finally red (reperfusion) as blood flow returns.
Although often mild, Raynaud’s can sometimes indicate an underlying systemic disease and should not be ignored in clinical practice.
Types of Raynaud’s Phenomenon
Primary Raynaud’s (Raynaud’s disease)
- Most common form
- No identifiable underlying disease
- Usually begins in young adults
- Typically mild and non-destructive
Primary Raynaud’s represents an exaggerated vascular response to cold or stress without structural vessel disease.
Secondary Raynaud’s (Raynaud’s syndrome)
- Associated with systemic disorders
- More severe and progressive
- Can lead to ulcers or tissue loss
Common causes include connective tissue diseases such as lupus, systemic sclerosis, and rheumatoid arthritis.
Secondary Raynaud’s may be the first manifestation of autoimmune disease in up to 20% of patients.
Causes and Risk Factors
Raynaud’s occurs when vascular control mechanisms malfunction, causing excessive vasoconstriction in response to stimuli.
Major triggers
- Cold exposure or rapid temperature change
- Emotional stress or anxiety
- Smoking or nicotine use
- Vibration injury or repetitive hand trauma
Cold remains the most common trigger because the body normally restricts blood flow to conserve heat; in Raynaud’s, this response is exaggerated and prolonged.
See Also: Arteries Anatomy: Layers, Function & Clinical Insight
Risk factors
- Female sex
- Younger age (primary type)
- Family history
- Living in cold climates
- Autoimmune disease
Women and people with a genetic predisposition are more frequently affected.
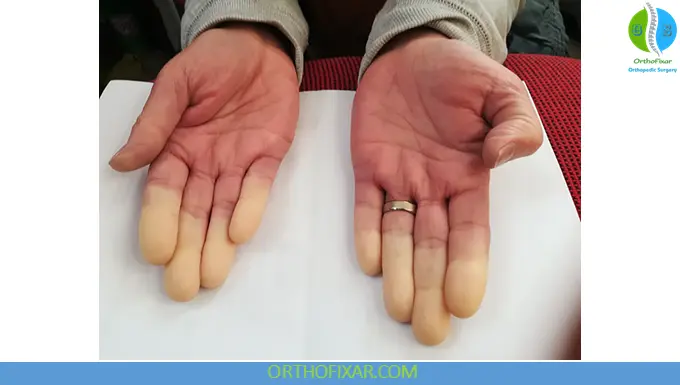
Clinical Symptoms
Raynaud’s attacks may last minutes to hours and present with:
- Cold, pale fingers or toes
- Blue discoloration from reduced oxygen
- Numbness or tingling
- Pain during reperfusion
- Swelling or throbbing after warming
In severe cases, recurrent ischemia can lead to digital ulcers or gangrene.
See Also: Peripheral Edema: Causes, Diagnosis, and Management
Diagnosis
Diagnosis is primarily clinical, based on the classic episodic color change pattern.
Investigations may include:
- Detailed history and physical examination
- Blood tests for autoimmune markers
- Nailfold capillaroscopy to distinguish primary from secondary disease
Capillaroscopy helps identify structural vascular abnormalities suggestive of connective tissue disease.
See Also: Allen Test Steps
Treatment and Management
1. Lifestyle and Conservative Management (First-line)
Most patients improve with behavioral measures:
- Keep hands, feet, and body warm
- Avoid smoking and nicotine exposure
- Manage stress levels
- Avoid sudden temperature shifts
These strategies are often sufficient for mild primary Raynaud’s.
2. Pharmacologic Treatment
For persistent or severe symptoms:
- Calcium channel blockers (e.g., nifedipine) are first-line drugs to reduce attack frequency and severity.
- Vasodilators or PDE-5 inhibitors may be considered in refractory cases.
Secondary Raynaud’s requires treatment of the underlying disease as well.
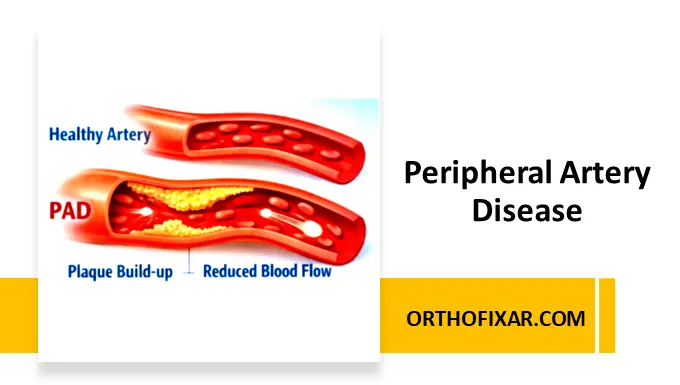
See Also: Peripheral Artery Disease (PAD): Symptoms, Causes & Treatment
3. Management During an Acute Attack
- Move to a warm environment
- Gently warm affected areas
- Wiggle fingers or toes
- Use warm (not hot) water
These steps help restore circulation and shorten the episode.
Complications
Although primary Raynaud’s is usually benign, secondary disease may lead to:
- Digital ulcers
- Infection
- Tissue necrosis
- Rarely, gangrene
Early recognition of secondary causes is crucial to prevent permanent damage.
When to Refer
Patients should be referred to rheumatology if they have:
- Late onset of symptoms
- Severe pain or ulcers
- Asymmetric attacks
- Signs of connective tissue disease
These features suggest secondary Raynaud’s and warrant further evaluation.
Prognosis
Primary Raynaud’s often remains stable or improves with age, while secondary Raynaud’s prognosis depends on the underlying disorder. Early diagnosis and treatment significantly reduce complications and improve quality of life.
References & More
- Musa R, Qurie A. Raynaud Disease. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: Pubmed
- Nawaz I, Nawaz Y, Nawaz E, Manan MR, Mahmood A. Raynaud’s Phenomenon: Reviewing the Pathophysiology and Management Strategies. Cureus. 2022 Jan 28;14(1):e21681. doi: 10.7759/cureus.21681. PMID: 35242466; PMCID: PMC8884459. Pubmed
- Nawaz I, Nawaz Y, Nawaz E, Manan MR, Mahmood A. Raynaud’s Phenomenon: Reviewing the Pathophysiology and Management Strategies. Cureus. 2022 Jan 28;14(1):e21681. doi: 10.7759/cureus.21681. PMID: 35242466; PMCID: PMC8884459. Pubmed
- Herrick AL. Raynaud’s phenomenon. J Scleroderma Relat Disord. 2019 Jun;4(2):89-101. doi: 10.1177/2397198319826467. Epub 2019 Feb 13. PMID: 35382391; PMCID: PMC8922643. Pubmed
- Bickley, L. S., Szilagyi, P. G., Hoffman, R. M., & Soriano, R. P. (2021). Bates’ guide to physical examination and history taking, 12e.