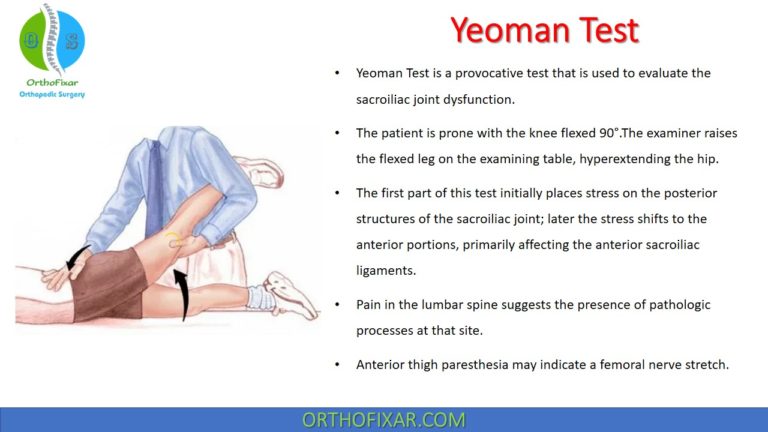
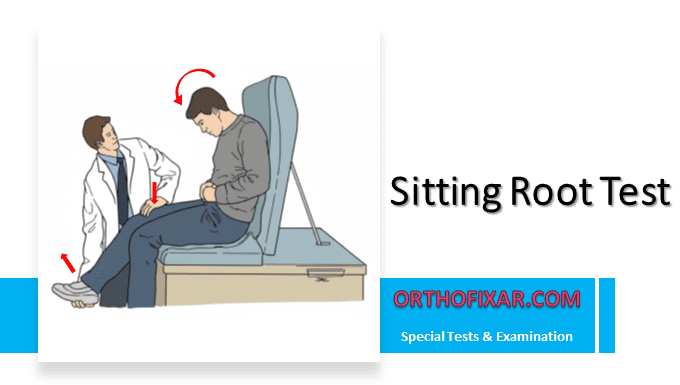
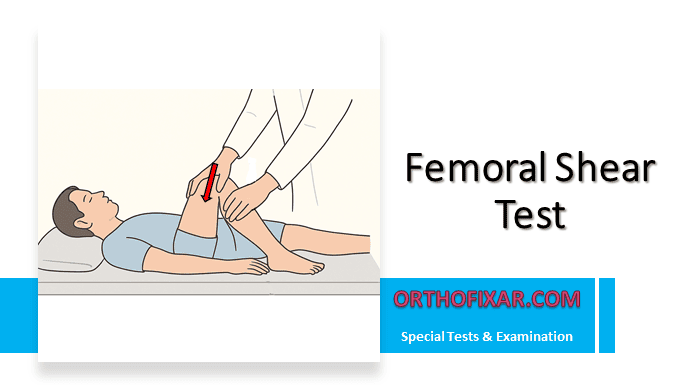
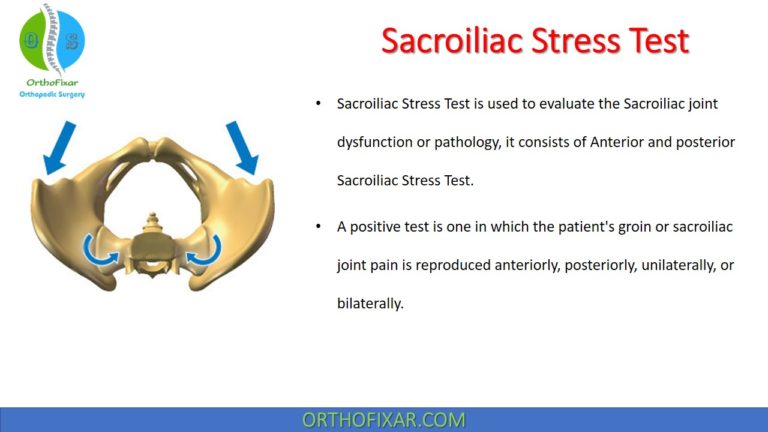
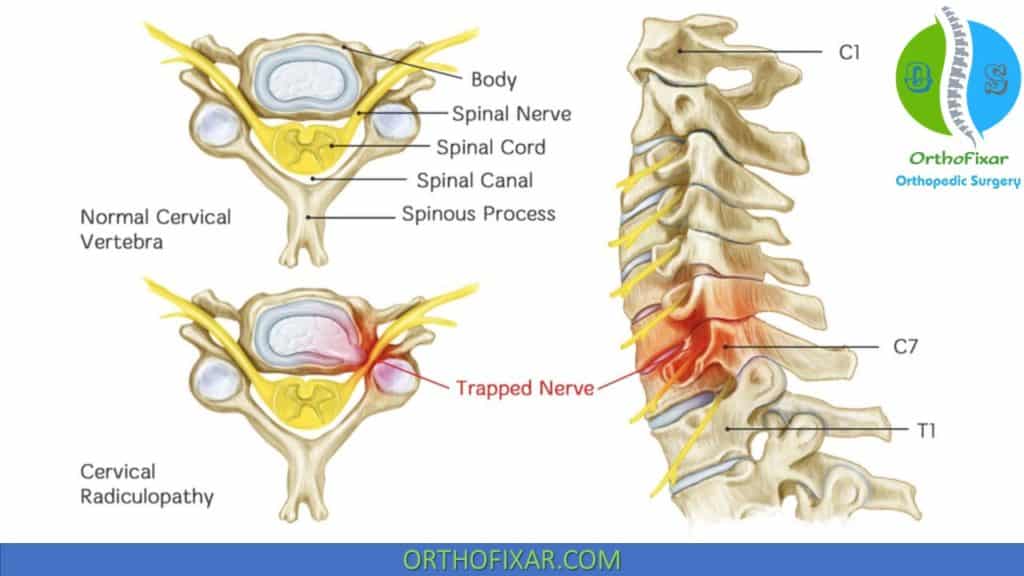
The Spurling Test, also called the Foraminal Compression Test or Neck Compression Test, is a clinical examination used to detect cervical radiculopathy caused by nerve root compression.
Spurling’s Test was originally named as Spurling’s neck compression test in 1944 by Roy Glenwood Spurling (1894 – 1968) and William Beecher Scoville (1906 – 1984) who were American neurosurgeons. The test has also been referred to as the Foraminal Compression Test, Neck Compression Test, or Quadrant Test.
It is a cervical special test designed to exacerbate encroachment of a cervical nerve root at the neural foramen by extension and rotation of the neck toward the involved side.
Purpose of the test
The Spurling’s test helps clinicians reproduce symptoms of cervical nerve root irritation by narrowing the neural foramen. It is particularly useful in patients with suspected:
- Cervical stenosis
- Cervical spondylosis
- Osteophytes
- Herniated cervical discs
- Facet joint pathology
How do you perform the Spurling’s test?
Spurling’s test is performed in seated position. The patient flexes the head and tilts it laterally, first to the unaffected side and then to the affected side. The examiner stands behind the patient with one hand on the patient’s head. With the other hand, the examiner lightly taps (compresses) the hand resting on the patient’s head applying a downward axial force (classically ~7 kg), thus narrowing the space for cervical nerve roots to exit the spinal cord.
If the patient tolerates this initial step of the test, Spurling Test is then repeated with the cervical spine extended as well.
See Also: Shoulder Abduction Test (Bakody Test)

What is a positive Spurling test?
The Spurling test is considered positive if pain radiates into the limb ipsilateral to the side at which the head is rotated.
- Simultaneous extension of the cervical spine narrows the intervertebral foramina by 20 to 30%.
- In conditions such as cervical stenosis, spondylosis, osteophytes, trophic facet joints, or herniated disks, the foramina may already be smaller than normal.
- The test is not considered to be positive if there is neck pain only, without radiation into the shoulder or arm. Only the pain that is radiating to the arm specific to a certain dermatome suggests nerve root irritation.
- Pain that is already present will be increased by this movement.
- Myalgia and whiplash syndrome can cause pain on the opposite side. This is called a reverse Spurling sign and suggests pain on the side of muscles that have been stretched from muscle strain or functional disturbance with muscle foreshortening.
If the pain is felt in the opposite side to which the head is taken, it is called a reverse Spurling sign and is indicative of muscle spasm in conditions such as tension myalgia and WADs.
Sensitivity & Specificity
The Spurling test sensitivity is low, but it has high specificity 1 for cervical radiculopathy diagnosed by electromyography:
- Sensitivity: 30 %
- Specificity: 93 %
Because it has low sensitivity, it is not useful as a screening test, but it is clinically useful in helping to confirm a cervical radiculopathy. It is best used combined with other specialized examination tests (some of which are mentioned below) to increase overall screening sensitivity, and should always be accompanied by thorough patient history
Shah and Rajshekhar studied the reliability of Spurling test in the diagnosis of cervical disc disease with the reference standard of magnetic resonance imaging (MRI) in 25 patients who were treated nonoperatively and direct visualization at surgery in 25 patients who were treated operatively. The test was performed by extending and laterally bending the neck and then applying an axial load to the top of the head. The investigators did not rotate the head prior to application of an axial load. The sensitivity and specificity of Spurling’s test was found to range between 0.90 and 1.00, depending on whether MRI or surgery was used as the reference standard.
In contrast, Wainner et al. performed the same test; however, they also rotated the head towards the ipsilateral side before applying an axial load. In that study, they used electromyography (EMG) as the reference standard. The investigators calculated a sensitivity of 0.50 and a specificity of 0.93 for this version of Spurling’s test.
In addition, Tong et al. calculated an even lower sensitivity (0.30) when rotating the neck towards the contralateral shoulder. Combining the results of these three studies, it appears that lateral rotation of the neck decreases the sensitivity of the Spurling test for the detection of cervical radiculopathy. This rationale is supported by Anekstein et al. who found the greatest sensitivity with the combination of lateral bending and extension without rotation. Thus, we prefer to perform the Spurling test in neutral rotation to improve diagnostic efficacy.
Modified Spurling Test
Modifications to Spurling Test have been advocated, which divide the test into three stages, each of which is more provocative. If symptoms are reproduced, the clinician does not progress to the next stage.
Modified Spurling Test stages:
- The first stage involves applying compression to the head in neutral.
- The second stage involves compression with the head in extension.
- The final stage involves compression with the head in extension and rotation to the uninvolved side, and then to the involved side.
No diagnostic accuracy studies have been performed to determine the sensitivity and specificity of these variations.
Notes
Pain on the concave side indicates nerve root irritation or facet joint pathology (Spurling sign), while pain on the convex side indicates muscle strain (reverse Spurling sign).
The patient may feel no discomfort, a sensation of heaviness, nonradicular or pseudoradicular pain, or radicular pain:
- Nonradicular or pseudoradicular pain includes pain that radiates to the occiput, the scapula, or the shoulders, or occasionally down the arm but not distal to the elbow. Such pseudoradicular pain may be the result of a mechanical or degenerative process in the cervical spine such as spondylolisthesis or degenerative disk disease without nerve root compression.
- Radicular pain radiates into the upper extremity, usually below the elbow, along the distribution of a specific dermatome.
Pain related to muscular strains or mild ligamentous sprains is not normally aggravated by these tests.
The test is an aggressive cervical compression test, and the patient should be prepared for each step of the examination.
The Spurling test should be avoided in patients suspected of having cervical instability, such as those with cervical spondylotic myelopathy, infectious process, or malignancy (most commonly metastatic). It should also not be performed in an acute trauma setting.
A very similar test is called the maximum cervical compression test . With this test, the patient side flexes the head and then rotates it to the same side. The test is repeated to the other side. A positive test is indicated if pain radiates into the arm. If the head is taken into extension (as well as side flexion and rotation) and compression is applied, the intervertebral foramina close maximally to the side of movement and symptoms are accentuated.
Pain on the concave side indicates nerve root or facet joint pathology, whereas pain on the convex side indicates muscle strain. This second position may also compress the vertebral artery. If one is testing the vertebral artery, the position should be held for 20 to 30 seconds to elicit symptoms (e.g., dizziness, nystagmus, feeling faint, nausea) that would indicate compression of the vertebral artery.
See Also: Myotomes of the Upper Limb
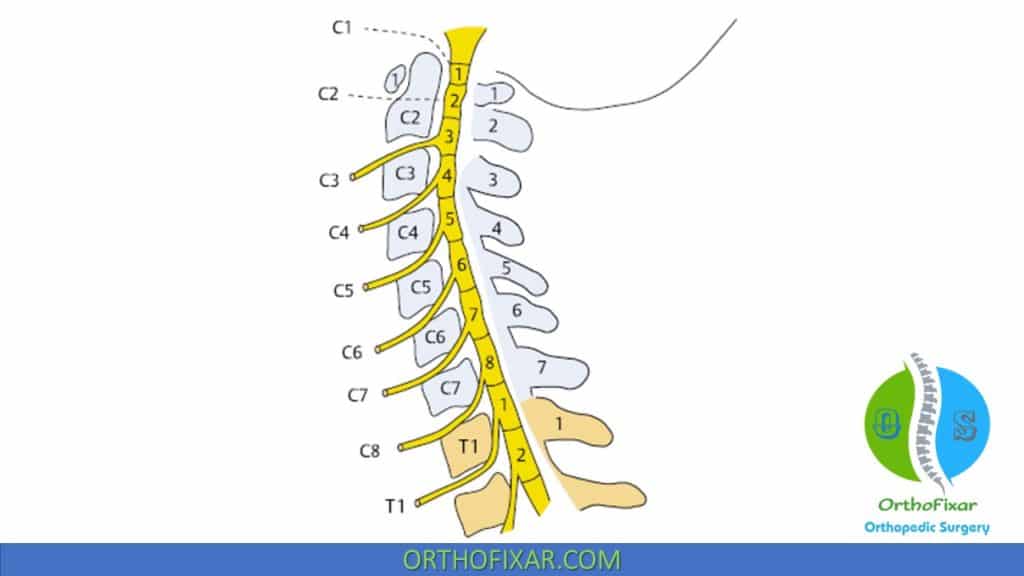
| Disk Level | Nerve Root | Motor Deficit | Sensory Deficit | Reflex Compromise |
|---|---|---|---|---|
| C4-C5 | C5 | Deltoid Muscle Biceps Muscle | Anterolateral shoulder and arm | Biceps Muscle |
| C5-C6 | C6 | Wrist extensors Biceps Muscle | Lateral forearm and hand Thumb | Brachoradialis Muscle Pronator teres Muscle |
| C6-C7 | C7 | Wrist flexors Muscle Triceps Muscle Finger extensors Muscle | Middle finger | Triceps Muscle |
| C7-T1 | C8 | Finger flexors Muscle Hand intrinsic Muscles | Medial forearm and hand and ring and little fingers | None |
| T1-T2 | T1 | Hand intrinsic Muscles | Medial forearm | None |
FAQ
What does a positive Spurling test indicate?
It suggests cervical nerve root compression due to stenosis, disc herniation, or osteophytes.
Is the Spurling test reliable?
Yes, it has high specificity (confirms radiculopathy), but low sensitivity (may miss some cases).
Can the Spurling test be harmful?
If performed incorrectly or in patients with instability or acute trauma, it can worsen symptoms.
What is the difference between Spurling and maximum cervical compression test?
Both involve compression, but the maximum cervical compression test adds rotation + extension, which can also test for vertebral artery compression.
Reference
- Tong HC, Haig AJ, Yamakawa K. The Spurling test and cervical radiculopathy. Spine (Phila Pa 1976). 2002 Jan 15;27(2):156-9. doi: 10.1097/00007632-200201150-00007. PMID: 11805661. Pubmed
- Shah KC, Rajshekhar V. Reliability of diagnosis of soft cervical disc prolapse using Spurling’s test. Br J Neurosurg 2004;18(5):480–483.
- Jones SJ, Miller JMM. Spurling Test. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: Pubmed
- Shabat, Shay; Leitner, Yossi; David, Rami; Folman, Yoram (September 2011). “The Correlation between Spurling Test and Imaging Studies in Detecting Cervical Radiculopathy”. Journal of Neuroimaging. 22: 375–378. doi:10.1111/j.1552-6569.2011.00644.x. PMID 21883627.
- Spurling RG, Scoville WB. Lateral rupture of the cervical intervertebral discs: a common cause of shoulder and arm pain. Surg Gynecol Obstet 1944;78:350–358.
- Anekstein Y, Blecher R, Smorgick Y, Mirovsky Y. What is the best way to apply the Spurling test for cervical radiculopathy? Clin Orthop Relat Res. 2012 Sep;470(9):2566-72. doi: 10.1007/s11999-012-2492-3. Epub 2012 Jul 18. PMID: 22806265; PMCID: PMC3830095. Pubmed
- Tong HC, Haig AJ, Yamakawa K. The Spurling test and cervical radiculopathy. Spine (Phila Pa 1976). 2002 Jan 15;27(2):156-9. doi: 10.1097/00007632-200201150-00007. PMID: 11805661. Pubmed
- Bradley JP, Tibone JE, Watkins RG: History, physical examination, and diagnostic tests for neck and upper extremity problems. In: Watkins RG, ed. The Spine in Sports. St. Louis, MO: Mosby-YearBook Inc., 1996.
- Jones SJ, Miller JMM. Spurling Test. 2021 Aug 11. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan–. PMID: 29630204.
- Jahnke RW, Hart BL. Cervical stenosis, spondylosis, and herniated disc disease. Radiol Clin North Am. 1991 Jul;29(4):777-91. PMID: 2063005.
- Wainner RS, Fritz JM, Irrgang JJ, Boninger ML, Delitto A, Allison S. Reliability and diagnostic accuracy of the clinical examination and patient selfreport measures for cervical radiculopathy. Spine (Phila Pa 1976). 2003;28(1):52–62.
- Clinical Tests for the Musculoskeletal System 3rd Edition.
- Dutton’s Orthopaedic Examination, Evaluation, And Intervention 3rd Edition.